Abstract
Purpose
This study aimed to investigate the clinical usefulness of the enhanced-T1WI-based deep learning radiomics model (DLRM) in differentiating low- and high-grade meningiomas.
Methods
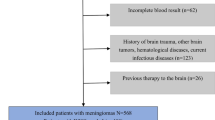
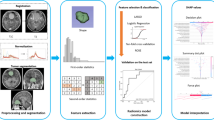
A total of 132 patients with pathologically confirmed meningiomas were consecutively enrolled (105 in the training cohort and 27 in the test cohort). Radiomics features and deep learning features were extracted from T1 weighted images (T1WI) (both axial and sagittal) and the maximum slice of the axial tumor lesion, respectively. Then, the synthetic minority oversampling technique (SMOTE) was utilized to balance the sample numbers. The optimal discriminative features were selected for model building. LightGBM algorithm was used to develop DLRM by a combination of radiomics features and deep learning features. For comparison, a radiomics model (RM) and a deep learning model (DLM) were constructed using a similar method as well. Differentiating efficacy was determined by using the receiver operating characteristic (ROC) analysis.
Results
A total of 15 features were selected to construct the DLRM with SMOTE, which showed good discrimination performance in both the training and test cohorts. The DLRM outperformed RM and DLM for differentiating low- and high-grade meningiomas (training AUC: 0.988 vs. 0.980 vs. 0.892; test AUC: 0.935 vs. 0.918 vs. 0.718). The accuracy, sensitivity, and specificity of the DLRM with SMOTE were 0.926, 0.900, and 0.924 in the test cohort, respectively.
Conclusion
The DLRM with SMOTE based on enhanced T1WI images has favorable performance for noninvasively individualized prediction of meningioma grades, which exhibited favorable clinical usefulness superior over the radiomics features.





Similar content being viewed by others
Availability of data and material
Research data are not available for public access due to patient privacy concerns but can be obtained from the corresponding author on reasonable request approved by the institutional review boards of all participating institutions.
Code availability
Not applicable.
References
Wiemels J, Wrensch M, Claus EB (2010) Epidemiology and etiology of meningioma. J Neuro-Oncol 99:307–314
Alexandru D, Glantz MJ, Kim L et al (2011) Pulmonary metastases in patients with recurrent, treatment-resistant meningioma: prognosis and identification by Indium-octreotide imaging. Cancer 117:4506–4511
Spille D, Adeli A, Sporns P et al (2021) Predicting the risk of postoperative recurrence and high-grade histology in patients with intracranial meningiomas using routine preoperative MRI. Neurosurg Rev 44:1109–1117
Lam Shin Cheung V, Kim A, Sahgal A et al (2018) Meningioma recurrence rates following treatment: a systematic analysis. J Neuro-Oncol 136:351–361
Biczok A, Jungk C, Egensperger R et al (2019) Microscopic brain invasion in meningiomas previously classified as WHO grade I is not associated with patient outcome. J Neuro-Oncol 145:469–477
Goldbrunner R, Minniti G, Preusser M et al (2016) EANO guidelines for the diagnosis and treatment of meningiomas. Lancet Oncol 17:e383–e391
Willis J, Smith C, Ironside JW et al (2005) The accuracy of meningioma grading: a 10-year retrospective audit. Neuropathol Appl Neurobiol 31:141–149
Bertero L, Dalla Dea G, Osella-Abate S et al (2019) Prognostic characterization of higher-grade meningiomas: a histopathological score to predict progression and outcome. J Neuropathol Exp Neurol 78:248–256
Ly KI, Hamilton SR, Rostomily RC et al (2015) Improvement in visual fields after treatment of intracranial meningioma with bevacizumab. J Neuroophthalmol 35:382–386
Buerki RA, Horbinski CM, Kruser T et al (2018) An overview of meningiomas. Future Oncol 14:2161–2177
Zhu Y, Man C, Gong L et al (2019) A deep learning radiomics model for preoperative grading in meningioma. Eur J Radiol 116:128–134
Huang RY, Bi WL, Griffith B et al (2019) Imaging and diagnostic advances for intracranial meningiomas. Neuro-Oncology 21:i44–i61
Spille D, Sporns P, Heß K et al (2019) Prediction of high-grade histology and recurrence in meningiomas using routine preoperative magnetic resonance imaging: a systematic review. World Neurosurg 128:174–181
Ke C, Chen H, Lv X et al (2020) Differentiation between benign and nonbenign meningiomas by using texture analysis from multiparametric MRI. J Magn Reson Imaging 51:1810–1820
Radakovich N, Nagy M, Nazha A (2020) Machine learning in haematological malignancies. Lancet Haematol 7:e541–e550
Martin Noguerol T, Paulano-Godino F, Martin-Valdivia MT et al (2019) Strengths, weaknesses, opportunities, and threats analysis of artificial intelligence and machine learning applications in radiology. J Am Coll Radiol 16:1239–1247
Ugga L, Perillo T, Cuocolo R et al (2021) Meningioma MRI radiomics and machine learning: systematic review, quality score assessment, and meta-analysis. Neuroradiology 63:1293–1304
Wen PY, Huse JT (2017) 2016 World Health Organization classification of central nervous system tumors. Continuum (Minneap Minn) 23:1531–1547
Tustison NJ, Avants BB, Cook PA et al (2010) N4ITK: improved N3 bias correction. IEEE Trans Med Imaging 29:1310–1320
van Griethuysen JJM, Fedorov A, Parmar C et al (2017) Computational radiomics system to decode the radiographic phenotype. Cancer Res 77:e104–e107
Pedregosa F, Varoquaux G, Gramfort A et al (2012) Scikit-learn: machine learning in Python
Nakamura M, Kajiwara Y, Otsuka A et al (2013) LVQ-SMOTE - Learning Vector Quantization based Synthetic Minority Over-sampling Technique for biomedical data. BioData Min 6:16
Nie P, Wang N, Pang J et al (2021) CT-based radiomics nomogram: a potential tool for differentiating hepatocellular adenoma from hepatocellular carcinoma in the noncirrhotic liver. Acad Radiol 28:799–807
Meng Q (2018) LightGBM: a highly efficient gradient boosting decision tree
Kawahara Y, Nakada M, Hayashi Y et al (2012) Prediction of high-grade meningioma by preoperative MRI assessment. J Neuro-Oncol 108:147–152
Apra C, Peyre M, Kalamarides M (2018) Current treatment options for meningioma. Expert Rev Neurother 18:241–249
Hu J, Zhao Y, Li M et al (2020) Machine learning-based radiomics analysis in predicting the meningioma grade using multiparametric MRI. Eur J Radiol 131:109251
Bohara M, Nakajo M, Kamimura K et al (2020) Histological grade of meningioma: prediction by intravoxel incoherent motion histogram parameters. Acad Radiol 27:342–353
Zhang J, Mucs D, Norinder U et al (2019) LightGBM: an effective and scalable algorithm for prediction of chemical toxicity-application to the Tox21 and mutagenicity data sets. J Chem Inf Model 2019
Vranes V, Vujasinovic T, Rajkovic N et al (2020) Analysis of spatial distribution and prognostic value of different pan cytokeratin immunostaining intensities in breast tumor tissue sections. Int J Mol Sci 21
Laukamp KR, Shakirin G, Baessler B et al (2019) Accuracy of radiomics-based feature analysis on multiparametric magnetic resonance images for noninvasive meningioma grading. World Neurosurg 132:e366–e390
Hamerla G, Meyer HJ, Schob S et al (2019) Comparison of machine learning classifiers for differentiation of grade 1 from higher gradings in meningioma: a multicenter radiomics study. Magn Reson Imaging 63:244–249
Han Y, Wang T, Wu P et al (2021) Meningiomas: preoperative predictive histopathological grading based on radiomics of MRI. Magn Reson Imaging 77:36–43
Agarwalla S, Sarma KK (2016) Machine learning based sample extraction for automatic speech recognition using dialectal Assamese speech. Neural Netw 78:97–111
Jing Y, Bian Y, Hu Z et al (2018) Deep learning for drug design: an artificial intelligence paradigm for drug discovery in the Big Data Era. AAPS J 20:58
Zhang H, Mo J, Jiang H et al (2021) Deep learning model for the automated detection and histopathological prediction of meningioma. Neuroinformatics 19:393–402
Banzato T, Causin F, Della Puppa A et al (2019) Accuracy of deep learning to differentiate the histopathological grading of meningiomas on MR images: a preliminary study. J Magn Reson Imaging 50:1152–1159
Mlynarski P, Delingette H, Criminisi A, et al (2018) 3D convolutional neural networks for tumor segmentation using long-range 2D context.
Acknowledgments
The authors would like to especially thank Professor Thelma R. Gower for her assistance with the preparation of this manuscript.
Funding
This paper is supported by the Haiyan Funding [grant number JJQN2019-23 to LY]. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Substantial contributions to the conception of the work: Liping Yang, Panpan Xu, Ying Zhang, and Tianzuo Wang. Substantial contributions to the acquisition of data: all authors. Substantial contributions to the analysis of data: Liping Yang, Panpan Xu, Ying Zhang, Nan Cui, Menglu Wang, Mengye Peng, Chao Gao, and Tianzuo Wang. Substantial contributions to interpretation of data for the work: Liping Yang, Panpan Xu, Ying Zhang, Nan Cui, Menglu Wang, Mengye Peng, Chao Gao, and Tianzuo Wang. Drafting the work or revising it critically for important intellectual content: all authors. Final approval of the version to be published: all authors.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee of the Harbin Medical University Cancer Hospital.
Consent to participate
For this type of retrospective study, formal consent is not required.
Consent for publication
All authors agree to the publication of this paper.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, L., Xu, P., Zhang, Y. et al. A deep learning radiomics model may help to improve the prediction performance of preoperative grading in meningioma. Neuroradiology 64, 1373–1382 (2022). https://doi.org/10.1007/s00234-022-02894-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-022-02894-0