Abstract
The endocannabinoid system (ECS) is a complex cell-signaling system. To address the growing need of analytics capturing endocannabinoid levels to investigate the ECS, we developed and validated an assay for the quantitative analysis of 14 endocannabinoids and congeners. A simple extraction using protein precipitation with acetonitrile followed by online-trapping high-performance liquid chromatography–tandem mass spectrometry (LC/LC-MS/MS) was used to monitor the levels of 14 endocannabinoids in plasma. The assay was validated and intra-run and inter-run accuracies and imprecisions as well as matrix effects, recoveries, and sample stabilities were determined. As a proof of concept, a subset of study samples after naturalistic administration of Cannabis flower and concentrate was analyzed. With the exception of N-oleoyl dopamine and oleamide, all endocannabinoids fulfilled the predefined acceptance criteria. Reproducible recoveries and no significant matrix effects were observed. Sample stability was an issue. Analysis of the proof-of-concept study samples revealed a significantly (p = 0.006) higher concentration of docosatetraenoyl ethanolamide in concentrate users (300 ± 13 pg/mL) compared to flower users (252 ± 11 pg/mL). A robust, sensitive high-throughput assay for the quantitation of 14 endocannabinoids and congeners was successfully validated. Our study showed that it is mandatory to (A) appropriately stabilize samples and (B) separate and separately quantify 1-AG and 2-AG; otherwise, study results are unreliable. The analysis of study samples from Cannabis flower users versus Cannabis concentrate users revealed higher levels of docosatetraenoyl ethanolamide and anandamide (n.s.) in high THC concentrate users in accordance with the existing literature, supporting the validity of the assay measurements.

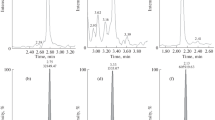
Graphical abstract



Similar content being viewed by others
References
Di Marzo V, Piscitelli F. The endocannabinoid system and its modulation by phytocannabinoids. Neurotherapeutics. 2015;12(4):692–8.
Zamberletti E, Gabaglio M, Parolaro D. The endocannabinoid system and autism spectrum disorders: insights from animal models. Int J Mol Sci. 2017;18(9).
Witkamp R. Fatty acids, endocannabinoids and inflammation. Eur J Pharmacol. 2016;785:96–107.
Alger BE. Endocannabinoids and their implications for epilepsy. Epilepsy Curr. 2004;4(5):169–73.
Lovinger DM. Presynaptic modulation by endocannabinoids. Handb Exp Pharmacol. 2008;184:435–77.
Di Marzo V, et al. Anandamide receptors. Prostaglandins Leukot Essent Fatty Acids. 2002;66(2–3):377–91.
Woodhams SG, et al. The cannabinoid system and pain. Neuropharmacology. 2017;124:105–20.
Woodhams SG, et al. The role of the endocannabinoid system in pain. Handb Exp Pharmacol. 2015;227:119–43.
Pistis M, Melis M. From surface to nuclear receptors: the endocannabinoid family extends its assets. Curr Med Chem. 2010;17(14):1450–67.
Moriconi A, et al. GPR55: current knowledge and future perspectives of a purported “Type-3” cannabinoid receptor. Curr Med Chem. 2010;17(14):1411–29.
Alexander SP, Kendall DA. The complications of promiscuity: endocannabinoid action and metabolism. Br J Pharmacol. 2007;152(5):602–23.
Pertwee RG, et al. International Union of Basic and Clinical Pharmacology. LXXIX. Cannabinoid receptors and their ligands: beyond CB(1) and CB(2). Pharmacol Rev. 2010;62(4):588–631.
Woodward DF, Liang Y, Krauss AH. Prostamides (prostaglandin-ethanolamides) and their pharmacology. Br J Pharmacol. 2008;153(3):410–9.
Maione S, Costa B, Di Marzo V. Endocannabinoids: a unique opportunity to develop multitarget analgesics. Pain. 2013;154(Suppl 1):S87–93.
Marchioni C, et al. A column switching ultrahigh-performance liquid chromatography-tandem mass spectrometry method to determine anandamide and 2-arachidonoylglycerol in plasma samples. Anal Bioanal Chem. 2017;409(14):3587–96.
Fanelli F, et al. Estimation of reference intervals of five endocannabinoids and endocannabinoid related compounds in human plasma by two dimensional-LC/MS/MS. J Lipid Res. 2012;53(3):481–93.
Bluher M, et al. Dysregulation of the peripheral and adipose tissue endocannabinoid system in human abdominal obesity. Diabetes. 2006;55(11):3053–60.
Fernandez-Rodriguez CM, et al. Circulating endogenous cannabinoid anandamide and portal, systemic and renal hemodynamics in cirrhosis. Liver Int. 2004;24(5):477–83.
Balvers MG, Verhoeckx KC, Witkamp RF. Development and validation of a quantitative method for the determination of 12 endocannabinoids and related compounds in human plasma using liquid chromatography-tandem mass spectrometry. J Chromatogr B Analyt Technol Biomed Life Sci. 2009;877(14–15):1583–90.
Di Marzo V, et al. Role of insulin as a negative regulator of plasma endocannabinoid levels in obese and nonobese subjects. Eur J Endocrinol. 2009;161(5):715–22.
Thomas A, et al. Quantitative and qualitative profiling of endocannabinoids in human plasma using a triple quadrupole linear ion trap mass spectrometer with liquid chromatography. Rapid Commun Mass Spectrom. 2009;23(5):629–38.
Acquaro Junior VR, et al. Analysis of endocannabinoids in plasma samples by biocompatible solid-phase microextraction devices coupled to mass spectrometry. Anal Chim Acta. 2019;1091:135–45.
Gurke R, et al. Determination of endocannabinoids and endocannabinoid-like substances in human K3EDTA plasma - LC-MS/MS method validation and pre-analytical characteristics. Talanta. 2019;204:386–94.
Souza ID, Hantao LW, Queiroz MEC. Polymeric ionic liquid open tubular capillary column for on-line in-tube SPME coupled with UHPLC-MS/MS to determine endocannabinoids in plasma samples. Anal Chim Acta. 2019;1045:108–16.
Matuszewski BK, Constanzer ML, Chavez-Eng CM. Strategies for the assessment of matrix effect in quantitative bioanalytical methods based on HPLC-MS/MS. Anal Chem. 2003;75(13):3019–30.
US Department of Health and Human Services, Guidance for Industry, Bioanalytical Method Validation. US FDA, Center for Drug Evaluation and Research, Center for Veterinary Medicine, MD, USA; 2018.
Bidwell LC, et al. Association of naturalistic administration of Cannabis flower and concentrates with intoxication and impairment. JAMA Psychiatry. 2020;77(8):787–96.
Fabritius M, et al. THCCOOH concentrations in whole blood: are they useful in discriminating occasional from heavy smokers? Drug Test Anal. 2014;6(1–2):155–63.
Lu HC, Mackie K. An introduction to the endogenous cannabinoid System. Biol Psychiatry. 2016;79(7):516–25.
Veilleux A, Di Marzo V, Silvestri C. The expanded endocannabinoid system/endocannabinoidome as a potential target for treating diabetes mellitus. Curr Diab Rep. 2019;19(11):117.
Chau CH, et al. Validation of analytic methods for biomarkers used in drug development. Clin Cancer Res. 2008;14(19):5967–76.
Klawitter J, et al. An atmospheric pressure chemical ionization MS/MS assay using online extraction for the analysis of 11 cannabinoids and metabolites in human plasma and urine. Ther Drug Monit. 2017;39(5):556–64.
Zoerner AA, et al. Quantification of endocannabinoids in biological systems by chromatography and mass spectrometry: a comprehensive review from an analytical and biological perspective. Biochim Biophys Acta. 2011;1811(11):706–23.
Rouzer CA, Ghebreselasie K, Marnett LJ. Chemical stability of 2-arachidonylglycerol under biological conditions. Chem Phys Lipids. 2002;119(1–2):69–82.
Engeli S, et al. Activation of the peripheral endocannabinoid system in human obesity. Diabetes. 2005;54(10):2838–43.
Bisogno T, et al. Brain regional distribution of endocannabinoids: implications for their biosynthesis and biological function. Biochem Biophys Res Commun. 1999;256(2):377–80.
Richardson D, et al. Quantitative profiling of endocannabinoids and related compounds in rat brain using liquid chromatography-tandem electrospray ionization mass spectrometry. Anal Biochem. 2007;360(2):216–26.
Valenti M, et al. The endocannabinoid system in the brain of Carassius auratus and its possible role in the control of food intake. J Neurochem. 2005;95(3):662–72.
Gonzalez S, et al. Changes in endocannabinoid contents in the brain of rats chronically exposed to nicotine, ethanol or cocaine. Brain Res. 2002;954(1):73–81.
Kondo S, et al. 2-Arachidonoylglycerol, an endogenous cannabinoid receptor agonist: identification as one of the major species of monoacylglycerols in various rat tissues, and evidence for its generation through CA2+-dependent and -independent mechanisms. FEBS Lett. 1998;429(2):152–6.
Rohrig W, et al. Quantification of 24 circulating endocannabinoids, endocannabinoid-related compounds, and their phospholipid precursors in human plasma by UHPLC-MS/MS. J Lipid Res. 2019;60(8):1475–88.
Solinas M, et al. Dopaminergic augmentation of delta-9-tetrahydrocannabinol (THC) discrimination: possible involvement of D(2)-induced formation of anandamide. Psychopharmacology. 2010;209(2):191–202.
Leweke FM, et al. Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia. Transl Psychiatry. 2012;2:e94.
Morgan CJ, et al. Cerebrospinal fluid anandamide levels, cannabis use and psychotic-like symptoms. Br J Psychiatry. 2013;202(5):381–2.
Hall W, Degenhardt L. Adverse health effects of non-medical cannabis use. Lancet. 2009;374(9698):1383–91.
Bisogno T, et al. Molecular targets for cannabidiol and its synthetic analogues: effect on vanilloid VR1 receptors and on the cellular uptake and enzymatic hydrolysis of anandamide. Br J Pharmacol. 2001;134(4):845–52.
Gaston TE, Szaflarski JP. Cannabis for the treatment of epilepsy: an update. Curr Neurol Neurosci Rep. 2018;18(11):73.
Muhl D, et al. Increased CB2 mRNA and anandamide in human blood after cessation of cannabis abuse. Naunyn Schmiedeberg's Arch Pharmacol. 2014;387(7):691–5.
Felder CC, et al. Anandamide, an endogenous cannabimimetic eicosanoid, binds to the cloned human cannabinoid receptor and stimulates receptor-mediated signal transduction. Proc Natl Acad Sci U S A. 1993;90(16):7656–60.
Hanus L, et al. Two new unsaturated fatty acid ethanolamides in brain that bind to the cannabinoid receptor. J Med Chem. 1993;36(20):3032–4.
Kelly P, Jones RT. Metabolism of tetrahydrocannabinol in frequent and infrequent marijuana users. J Anal Toxicol. 1992;16(4):228–35.
Funding
Funding for this study was provided by grants from the National Institutes of Health (DA039707 to Dr. Hutchison) and Colorado Department of Public Health and Environment (96947 to Dr. Bidwell). The funding organizations had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Clinical samples
The clinical study was approved by the University of Colorado Boulder Institutional Review Board and the primary outcomes have been published previously [27]. The study was registered as an observational study in ClinicalTrials.gov (NCT03522103).
Source of biological material
Blank human K2EDTA plasma was received from Bioreclamation IVT (Westbury, NY, USA) and charcoal-stripped human plasma was received from BioCheMed (Winchester, VA, USA).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 1.94 mb)
Rights and permissions
About this article
Cite this article
Sempio, C., Klawitter, J., Jackson, M. et al. Analysis of 14 endocannabinoids and endocannabinoid congeners in human plasma using column switching high-performance atmospheric pressure chemical ionization liquid chromatography–mass spectrometry. Anal Bioanal Chem 413, 3381–3392 (2021). https://doi.org/10.1007/s00216-021-03280-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-021-03280-0