Abstract
A deficiency of α-galactosidase A causes Fabry disease (FD) by disrupting lipid metabolism, especially trihexosylceramide (THC). Enzyme replacement therapy (ERT) is clinically offered to FD patients in an attempt to lower the accumulated lipids. Studies on specific types of lipids that are directly or indirectly altered by FD are very scarce, even though they are crucial in understanding the biological process linked to the pathogenesis of FD. We performed a comprehensive lipid profiling of plasma and urinary lipids from FD patients with nanoflow liquid chromatography electrospray-ionization tandem mass spectrometry (nLC-ESI-MS/MS) and identified 129 plasma and 111 urinary lipids. Among these, lipids that exhibited alternations (>twofold) in patients were selected as targets for selected reaction monitoring (SRM)-based high-speed quantitation using nanoflow ultra-performance LC-ESI-MS/MS (nUPLC-ESI-MS/MS) and 31 plasma and 26 urinary lipids showed significant elevation among FD patients. Higher percentages of sphingolipids (SLs; 48 % for plasma and 42 % for urine) were highly elevated in patients; whereas, a smaller percentage of phospholipids (PLs; 15 % for plasma and 13 % for urine) were significantly affected. Even though α-galactosidase A is reported to affect THC only, the results show that other classes of lipids (especially SLs) are changed as well, indicating that FD not only alters metabolism of THC but various classes of lipids too. Most lipids showing significant increases in relative amounts before ERT decreased after ERT, but overall, ERT influenced plasma lipids more than urinary lipids.

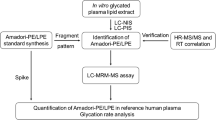
Brief overview of lipidomic analysis for Fabry disease using nLC-ESI-MS/MS and nUPLC-ESI-MS/MS.





Similar content being viewed by others
References
Branton MH, Schiffmann R, Sabnis SG, Murray GJ, Quirk JM, Altarescu G, et al. Natural history of Fabry renal disease: infleucne of α-galactosidase A activity and genetic mutations on clinical course. Medicine. 2002;81:122–38.
Meikle PJ, Hopwood JJ, Clague AE, Carrey WF. Prevalence of lysosomal storage disorders. JAMA. 1999;281:249–51.
Tse KC, Chan KW, Tin VP, Yip PS, Tang S, Li FK, et al. Clinical features and genetic analysis of a Chinese kindred with Fabry’s disease. Nephrol Dial Transplant. 2003;18:182–6.
Hauser AC, Lorenz M, Sunder-Plassmann G. The expanding clinical spectrum of Anderson–Fabry disease: a challenge to diagnosis in the novel era of enzyme replacement therapy. J Intern Med. 2004;255:629–36.
Mehta A, Beck M, Eyskens F, Feliciani C, Kantola I, Ramaswami U, et al. Fabry disease: a review of current management strategies. QJM. 2010;103:641–59.
Carubbi F, Bonilauri L. Fabry disease: raising awareness of the disease among physicians. Intern Emerg Med. 2012;7:227–31.
Weidemann F, Breunig F, Beer M, Sandstede J, Turschner O, Voelker W, et al. Improvement of cardiac function during enzyme replacement therapy in patients with Fabry disease. Circulation. 2003;108:1299–301.
Brouwers JFHM, Vernooji EAAM, Tielens AGM, van Golde LMG. Rapid separation and identification of phosphatidylethanolamine molecular species. J Lipid Res. 1999;40:164–9.
Wright MM, Howe AG, Zaremberg V. Cell membranes and apoptosis: role of cardiolipin, phosphatidylcholine, and anticancer lipid analogues. Biochem Cell Biol. 2004;82:18–26.
Isaac G, Bylund D, Månsson JE, Markides KE, Bergquist J. Analysis of phosphatidylcholine and sphingomyelin molecular species from brain extracts using capillary liquid chromatography electrospray ionization mass spectrometry. J Neurosci Methods. 2003;128:111–9.
Taguchi R, Hayakawa J, Takeuchi Y, Ishida M. Two-dimensional analysis of phospholipids by capillary liquid chromatography/electrospray ionization mass spectrometry. J Mass Spectrom. 2000;35:953–66.
Bang DY, Moon MH. On-line two-dimensional capillary strong anion exchange/reversed phase liquid chromatography-tandem mass spectrometry for comprehensive lipid analysis. J Chromatogr A. 2013;1310:82–90.
Lim S, Bang DY, Rha KH, Moon MH. Rapid screening of phospholipid biomarker candidates from prostate cancer urine samples by multiple reaction monitoring of UPLC-ESI-MS/MS and statistical approaches. Bull Korean Chem Soc. 2014;35:1133–8.
Kim JY, Kim S-K, Kang D, Moon MH. Dual lectin-based size sorting strategy to enrich targeted N-glycopeptides by asymmetrical flow field-flow fractionation: profiling lung cancer biomarkers. Anal Chem. 2012;84:5343–50.
Byeon SK, Lee JY, Lim S, Choi D, Moon MH. Discovery of candidate phospholipid biomarkers in human lipoproteins with coronary artery disease by flow field-flow fractionation and nanoflow liquid chromatography-tandem mass spectrometry. J Chromatogr A. 2012;1270:246–53.
Min HK, Lim S, Chung BC, Moon MH. Shotgun lipidomics for potential biomarkers of urinary phospholipids in prostate cancer. Anal Bioanal Chem. 2011;399:823–30.
Moon MH. Phospholipid analysis by nanoflow liquid chromatography-tandem mass spectrometry. Mass Spectrometry Letters. 2014;5:1–11.
Lee JY, Byeon SK, Moon MH. Profiling of oxidized phospholipids in lipoproteins from patients with coronary artery disease by hollow fiber flow field-flow fractionation and nanoflow liquid chromatography-tandem mass spectrometry. Anal Chem. 2015;87:1266–73.
Swartz ME. “UPLC: an introduction and review”. J Liq Chromatogr. 2005;28:1253–63.
Petrovic M, Gros M, Barcelo D. Multi-residue analysis of pharmaceuticals in wastewater by ultra-performance liquid chromatography-quadrupole-time-of-flight mass spectrometry. J Chromatogr A. 2006;1124:68–81.
Byeon SK, Lee JY, Moon MH. Optimized extraction of phospholipids and lysophospholipids for nanoflow liquid chromatography-electrospray ionization-tandem mass spectrometry. Analyst. 2012;137:451–8.
Bang DY, Lim S, Moon MH. Effect of ionization modifiers on the simultaneous analysis of all classes of phospholipids by nanoflow liquid chromatography/tandem mass spectrometry in negative ion mode. J Chromatogr A. 2012;1240:69–76.
Lim S, Byeon SK, Lee JY, Moon MH. Computational approach to the structural identification of phospholipids using raw mass spectra from nanoflow liquid chromatography-electrospray ionization-tandem mass spectrometry. J Mass Spectrom. 2012;47:1004–14.
Byeon SK, Lee JY, Lee J-S, Moon MH. Lipidomic profiling of plasma and urine from patients with Gaucher disease during enzyme replacement therapy by nanoflow liquid chromatography-tandem mass spectrometry. J Chromatogr A. 2015;1381:132–9.
Larson A, Uran S, Jacobsen PB, Skotland T. Collision-induced dissociation of glycerol phospholipids using electrospray ion-tran mass spectrometry. Rapid Commun Mass Sepctrom. 2001;15:2393–8.
Acknowledgments
This study was supported by a grant (HI12C-0022-030014) from the Korea Healthcare Technology R&D Project, Ministry for Health and Welfare Affairs and in part by a grant (NRF-2015R1A2A1A01004677) from the National Research Foundation of Korea.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 716 kb)
Rights and permissions
About this article
Cite this article
Byeon, S.K., Kim, J.Y., Lee, JS. et al. Variations in plasma and urinary lipids in response to enzyme replacement therapy for Fabry disease patients by nanoflow UPLC-ESI-MS/MS. Anal Bioanal Chem 408, 2265–2274 (2016). https://doi.org/10.1007/s00216-016-9318-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-016-9318-1