Abstract
Summary
Based on the prospective cohort of the Vietnam Osteoporosis Study, we show that bone loss occurred before menopause, and that the loss accelerated in the first 5 years post-menopause.
Purpose
To define the change in bone mineral density (BMD) among women during the menopausal transition.
Methods
The study involved 1062 women aged 40–59 who were participants of the population-based prospective Vietnam Osteoporosis Study. BMD at the femoral neck (FN), lumbar spine (LS), and whole body scan was measured by DXA. Each woman has had two BMD measurements separated by approximately 2 years, and the rate of BMD change was calculated for each woman. Multivariable linear regression models were used to quantify the association between body composition parameters and the rate of BMD change.
Results
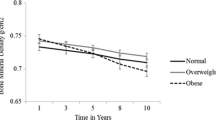
At FN, there were 3 phases of BMD change: a slight decline before the age of 45–49 (average loss of 0.51%/year); a substantial decline between the ages of 49 and 54 (average loss of 1.39%/year); and then slowed down between the ages of 54 and 59 (average loss of 0.31%/year). The same trend was also observed at LS: a slight decline (− 0.56%/year) among women aged 45–49; then a significant decline between the ages of 50 and 54 (− 1.33%/year); but then slowed down at − 0.31%/year after the age of 55. Changes in BMD were not significantly associated with changes in lean mass or fat mass.
Conclusions
Although bone loss occurred before menopause, the loss accelerated in the early perimenopausal transition (45–50 years of age). This finding suggests that screening for osteoporosis in women should be considered at the age of 45.


Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Rogers A et al (2002) Circulating estradiol and osteoprotegerin as determinants of bone turnover and bone density in postmenopausal women. J Clin Endocrinol Metab 87(10):4470–4475
Jones G et al (1994) Progressive loss of bone in the femoral neck in elderly people: longitudinal findings from the Dubbo osteoporosis epidemiology study. BMJ 309(6956):691
Finkelstein JS et al (2008) Bone mineral density changes during the menopause transition in a multiethnic cohort of women. J Clin Endocrinol Metab 93(3):861–868
Cheung E et al (2011) Bone loss during menopausal transition among southern Chinese women. Maturitas 69(1):50–56
Iqbal J, Zaidi M (2009) Understanding estrogen action during menopause. Endocrinology 150(8):3443–3445
Ho-Pham LT, Nguyen TV (2017) The Vietnam Osteoporosis Study: rationale and design. Osteoporos Sarcopenia 3(2):90–97
McKinlay SM (1996) The normal menopause transition: an overview. Maturitas 23(2):137–145
Sherman S (2005) Defining the menopausal transition. Am J Med 118(2):3–7
Harlow SD et al (2012) Executive summary of the Stages of Reproductive Aging Workshop + 10: addressing the unfinished agenda of staging reproductive aging. J Clin Endocrinol Metab 97(4):1159–1168
Davis SR et al (2015) Menopause. Nat Rev Dis Prim 1(1):15004
Morabia A et al (1998) International variability in ages at menarche, first livebirth, and menopause. Am J Epidemiol 148(12):1195–1205
McKinlay SM, Brambilla DJ, Posner JG (1992) The normal menopause transition. Maturitas 14(2):103–115
Gold EB (2011) The timing of the age at which natural menopause occurs. Obstet Gynecol Clin North Am 38(3):425–440
Greendale GA et al (2012) Bone mineral density loss in relation to the final menstrual period in a multiethnic cohort: results from the Study of Women’s Health Across the Nation (SWAN). J Bone Miner Res 27(1):111–118
Consultation WE (2004) Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet (London, England) 363(9403):157–163
Ho-Pham LT et al (2011) Reference ranges for bone mineral density and prevalence of osteoporosis in Vietnamese men and women. BMC Musculoskelet Disord 12(1):182
Kanis JA, Kanis JA (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. Osteoporos Int 4(6):368–381
Nguyen TV (2020) Common methodological issues and suggested solutions in bone research. Osteoporos Sarcopenia 6(4):161–167
Groemping U (2006) Relative importance for linear regression in R: the package relaimpo. J Stat Softw 17(1):1–27
Harrell FE (2001) Regression modeling strategies: with applications to linear models, logistic regression, and survival analysis. Springer-Verlag, New York. https://doi.org/10.1007/978-1-4757-3462-1
Crandall CJ et al (2013) Serum sex steroid levels and longitudinal changes in bone density in relation to the final menstrual period. J Clin Endocrinol Metab 98(4):E654–E663
Sowers MR et al (2010) Amount of bone loss in relation to time around the final menstrual period and follicle-stimulating hormone staging of the transmenopause. J Clin Endocrinol Metab 95(5):2155–2162
Guthrie J et al (1998) A prospective study of bone loss in menopausal Australian-born women. Osteoporos Int 8(3):282–290
Seifert-Klauss V et al (2012) Bone loss in premenopausal, perimenopausal and postmenopausal women: results of a prospective observational study over 9 years. Climacteric 15(5):433–440
Nguyen T et al (1994) Lifestyle factors and bone density in the elderly: implications for osteoporosis prevention. J Bone Miner Res 9(9):1339–1346
Harris S, Dallal GE, Dawson-Hughes B (1992) Influence of body weight on rates of change in bone density of the spine, hip, and radius in postmenopausal women. Calcif Tissue Int 50(1):19–23
Tsunenari T et al (1995) Menopause-related changes in bone mineral density in Japanese women: a longitudinal study on lumbar spine and proximal femur. Calcif Tissue Int 56(1):5–10
Eriksen EF et al (1999) Hormone replacement therapy prevents osteoclastic hyperactivity: a histomorphometric study in early postmenopausal women. J Bone Miner Res 14(7):1217–1221
Riggs BL, Khosla S, Melton LJ III (2002) Sex steroids and the construction and conservation of the adult skeleton. Endocr Rev 23(3):279–302
Butler L, Santoro N (2011) The reproductive endocrinology of the menopausal transition. Steroids 76(7):627–635
Schoenaker DA et al (2014) Socioeconomic position, lifestyle factors and age at natural menopause: a systematic review and meta-analyses of studies across six continents. Int J Epidemiol 43(5):1542–1562
Velez MP et al (2019) Age at natural menopause and physical functioning in postmenopausal women: the Canadian Longitudinal Study on Aging. Menopause (New York, NY) 26(9):958
Shieh A et al (2020) The association between fast increase in bone turnover during the menopause transition and subsequent fracture. J Clin Endocrinol Metab 105(4):e1440–e1448
Acknowledgements
We sincerely thank MS Tran Thi Ngoc Trang and Fr Pham Ba Lam for coordinating the recruitment of participants. We also thank doctors and medical students of the Pham Ngoc Thach University of Medicine for the data collection and clinical measurements.
Funding
This research is partly funded by the Foundation for Science and Technology Development of Ton Duc Thang University (FOSTECT, http://fostect.tdt.edu.vn), grant number FOSTECT.2014.BR.09, and a grant from the Department of Science and Technology of Ho Chi Minh City. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Ethics Committee of the People’s Hospital 115. The study was conducted according to the ethical principles of the Declaration of Helsinki, and all participants gave written informed consent.
Consent for publication
The manuscript does not contain any individual person’s data in any form.
Conflicts of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ho-Pham, L.T., Nguyen, H.G., Nguyen-Pham, S.Q. et al. Longitudinal changes in bone mineral density during perimenopausal transition: the Vietnam Osteoporosis Study. Osteoporos Int 34, 1381–1387 (2023). https://doi.org/10.1007/s00198-023-06757-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-023-06757-z