Abstract
Summary
We found social deprivation to be associated with higher mortality in the year following hip fracture among men and women aged 60 years and older in England. In those who did survive, deprivation was associated with longer hospital stays and greater risk of subsequent emergency readmission particularly for patients with dementia.
Introduction
Social deprivation predicts a range of adverse health outcomes; however, its impact on outcomes following hip fracture is not established. We examined the effect of area-level social deprivation on outcomes following hospital admission for hip fracture in England.
Methods
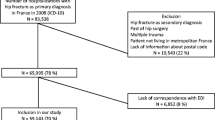
We used English Hospital Episodes Statistics linked to the National Hip Fracture Database (April 2011–March 2015) and Office for National Statistics mortality database, to identify patients aged 60+ years admitted with hip fracture. Deprivation was measured using Index of Multiple Deprivation quintiles; Q1-least deprived; Q5-most deprived, and outcomes by mortality over 1-year, length-of-stay in NHS acute and rehabilitation hospitals (‘superspell’), and emergency 30-day readmission.
Results
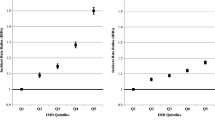
We identified 218,907 admissions with an index hip fracture (mean age 82.8 [standard deviation, SD 8.4] years; 72.6% female). Each quintile of deprivation was associated with greater mortality; age-adjusted 30-day mortality odds ratio, OR 1.30 [95% confidence interval, CI: 1.24, 1.37], p < 0.001, equating to on average 1038 fewer deaths/year among those who are least deprived (Q1 versus 2–5). Similarly, at 365 days, those most deprived had 24% higher mortality (age-sex-comorbidity-adjusted OR:1.24 [1.20, 1.28], p < 0.001; Q5 versus Q1). Among survivors, mean superspell was longer in the most versus least deprived (Q5:24.4 [SD 21.7] days, Q1:23.3 [SD 22.1], p < 0.001). Readmission was more common in those most versus least deprived (age-sex-comorbidity-adjusted OR 1.27 [1.22, 1.32], p < 0.001).
Conclusion
Greater deprivation is associated with reduced survival at all timepoints in the year following hip fracture. Among survivors, hospital stay is increased as is readmission risk. The extent to which configuration of English hospital services, rather than patient case-mix, explains these apparent health inequalities remains to be determined.


Similar content being viewed by others
References
Judge A, Javaid K, Cooper C, Arden N, Farmer A, Prieto-Alhambra D, et al (2016) Models of care for the delivery of secondary fracture prevention after hip fracture: a health service cost, clinical outcomes and cost-effectiveness study within the South Central Region. National Institute for Health Research (NIHR), Health Services and Delivery Research (HS&DR)
Griffin XL, Parsons N, Achten J, Fernandez M, Costa ML (2015) Recovery of health-related quality of life in a United Kingdom hip fracture population. The Warwick Hip Trauma Evaluation--a prospective cohort study. Bone Joint J 97–b(3):372–382. https://doi.org/10.1302/0301-620x.97b3.35738
Downey C, Kelly M, Quinlan JF (2019) Changing trends in the mortality rate at 1-year post hip fracture-a systematic review. World J Orthop 10(3):166–175
Bai J, Zhang P, Liang X, Wu Z, Wang J, Liang Y (2018) Association between dementia and mortality in the elderly patients undergoing hip fracture surgery: a meta-analysis. J Orthop Surg Res 13(1):298. https://doi.org/10.1186/s13018-018-0988-6
Royal College of Physicians (2016) National Hip Fracture Database annual report 2016. London: RCP
The NHS Information Centre (2013) Emergency readmissions 2010–11 summary. Department of Health, https://www.gov.uk/government/publications/emergency-readmissions-data
Ali AM, Gibbons CE (2017) Predictors of 30-day hospital readmission after hip fracture: a systematic review. Injury 48(2):243–252
Lang IA, Hubbard RE, Andrew MK, Llewellyn DJ, Melzer D, Rockwood K (2009) Neighborhood deprivation, individual socioeconomic status, and frailty in older adults. J Am Geriatr Soc 57(10):1776–1780
Pujades-Rodriguez M, Timmis A, Stogiannis D, Rapsomaniki E, Denaxas S, Shah A, Feder G, Kivimaki M, Hemingway H (2014) Socioeconomic deprivation and the incidence of 12 cardiovascular diseases in 1.9 million women and men: implications for risk prediction and prevention. PLoS One 9(8):e104671
Lee TC, Glynn RJ, Peña JM, Paynter NP, Conen D, Ridker PM, Pradhan AD, Buring JE, Albert MA (2011) Socioeconomic status and incident type 2 diabetes mellitus: data from the Women’s Health Study. PLoS One 6(12):e27670
Riaz SP, Horton M, Kang J, Mak V, Lüchtenborg M, Møller H (2011) Lung cancer incidence and survival in England: an analysis by socioeconomic deprivation and urbanization. J Thorac Oncol 6(12):2005–2010
van de Vorst IE, Koek HL, Stein CE, Bots ML, Vaartjes I (2016) Socioeconomic disparities and mortality after a diagnosis of dementia: results from a nationwide registry linkage study. Am J Epidemiol 184(3):219–226. https://doi.org/10.1093/aje/kwv319
Bhimjiyani A, Neuburger J, Jones T, Ben-Shlomo Y, Gregson CL (2018) The effect of social deprivation on hip fracture incidence in England has not changed over 14 years: an analysis of the English Hospital Episodes Statistics (2001-2015). Osteoporos Int 29(1):115–124. https://doi.org/10.1007/s00198-017-4238-2
Valentin G, Pedersen SE, Christensen R, Friis K, Nielsen CP, Bhimjiyani A, Gregson CL, Langdahl BL (2020) Socio-economic inequalities in fragility fracture outcomes: a systematic review and meta-analysis of prognostic observational studies. Osteoporos Int 31(1):31–42. https://doi.org/10.1007/s00198-019-05143-y
Smith P, Ariti C, Bardsley M (2013) Focus on hip fracture: trends in emergency admissions for fractured neck of femur, 2001 to 2011. QualityWatch. The Health Foundation and Nuffield Trust, London
Kristensen PK, Thillemann TM, Pedersen AB, Soballe K, Johnsen SP (2017) Socioeconomic inequality in clinical outcome among hip fracture patients: a nationwide cohort study. Osteoporos Int 28(4):1233–1243
Gaughan J, Gravelle H, Santos R, Siciliani L (2017) Long-term care provision, hospital bed blocking, and discharge destination for hip fracture and stroke patients. International journal of health economics and management 17(3):311–331
Quah C, Boulton C, Moran C (2011) The influence of socioeconomic status on the incidence, outcome and mortality of fractures of the hip. J Bone Joint Surg Br 93(6):801–805
Castelli A, Daidone S, Jacobs R, Kasteridis P, Street AD (2015) The determinants of costs and length of stay for hip fracture patients. PLoS One 10(7):e0133545
Holder H, Kumpunen S, Castle-Clarke S, Lombardo S (2018) Managing the hospital and social care interface. Interventions targeting older adults. The Nuffield Trust
Bunning T, Dickinson R, Fagan E, Inman D, Johansen A, Judge A, Hannaford J, Liddicoat M, Wakeman R (2017) National Hip Fracture Database (NHFD) Annual Report 2018. Royal College of Physicians: London, UK
Bhimjiyani A (2019) Social and regional inequalities in the incidence of and outcomes after hip fracture in England. Dept Translational Health Sciences University of Bristol, Bristol Medical School Thesis Repository
Health and Social Care Information Centre (2017) HES Data Dictionary: Admitted Patient Care
NHS Digital (2018) Linked HES-ONS mortality data. https://digital.nhs.uk/data-and-information/data-tools-and-services/data-services/linked-hes-ons-mortality-data. Accessed 25/05/2018
Department for Communities and Local Government (2011) The English indices of deprivation 2010: Technical Report
McLennan D, Barnes H, Noble M, Davies J, Garratt E, Dibben C (2011) The english indices of deprivation 2010. Department for communities and local government. Her Majesty’s Stationery Office, London
Armitage JN, van der Meulen JH (2010) Identifying co-morbidity in surgical patients using administrative data with the Royal College of Surgeons Charlson score. Br J Surg 97(5):772–781. https://doi.org/10.1002/bjs.6930
Saklad M (1941) Grading of patients for surgical procedures. Anesthesiology: The Journal of the American Society of Anesthesiologists 2(3):281–284
Royal College of Physicians (2018) National Hip Fracture Database (NHFD) Website user guide V 11.0. London: RCP
Barone AP, Fusco D, Colais P, D'Ovidio M, Belleudi V, Agabiti N, Sorge C, Davoli M, Perucci CA (2009) Effects of socioeconomic position on 30-day mortality and wait for surgery after hip fracture. Int J Qual Health Care 21(6):379–386
Thorne K, Johansen A, Akbari A, Williams JG, Roberts SE (2016) The impact of social deprivation on mortality following hip fracture in England and Wales: a record linkage study. Osteoporos Int 27(9):2727–2737
Roberts SE, Goldacre MJ (2003) Time trends and demography of mortality after fractured neck of femur in an English population, 1968-98: database study. BMJ 327(7418):771–775
Bottle A, Aylin P (2006) Mortality associated with delay in operation after hip fracture: observational study. BMJ 332(7547):947–951
Wu TY, Jen MH, Bottle A, Liaw CK, Aylin P, Majeed A (2011) Admission rates and in-hospital mortality for hip fractures in England 1998 to 2009: time trends study. J Public Health 33(2):284–291
Cookson R, Propper C, Asaria M, Raine R (2016) Socio-economic inequalities in health care in England. Fisc Stud 37(3–4):371–403. https://doi.org/10.1111/j.1475-5890.2016.12109
Prince M, Knapp M, Guerchet M, McCrone P, Prina M, Comas-Herrera A, Wittenberg R, Adelaja B, Hu B, King D, Rehill A, Salimkumar D (2014) Dementia UK: update. Alzheimer’s Society
Smith P, Sherlaw-Johnson C, Ariti C, Bardsley M (2015) Focus on: hospital admissions from care homes. The Health Foundation and Nuffield Trust, London
Office for National Statistics (2015) 2011 Census analysis: what does the 2011 census tell us about people living in communal establishments? https://www.ons.gov.uk/peoplepopulationandcommunity/housing/articles/2011censusanalysiswhatdoesthe2011censustellusaboutpeoplelivingincommunalestablishments/2015-02-11 (30/04/2019)
Department for Communities and Local Government (2015) The English Indices of Deprivation 2015 Statistical Release
Mudrazija S, Thomeer MB, Angel JL (2015) Gender differences in institutional long-term care transitions. Womens Health Issues 25(5):441–449. https://doi.org/10.1016/j.whi.2015.04.010
Kristensen PK, Johnsen SP, Mor A, Thillemann TM, Pedersen AB (2017) Is the higher mortality among men with hip fracture explained by sex-related differences in quality of in-hospital care? A population-based cohort study. Age Ageing 46(2):193–199
Health and Social Care Information Centre (2013) Hospital episode statistics, emergency readmissions to hospital within 28 days of discharge - Financial year 2011/12
French DD, Bass E, Bradham DD, Campbell RR, Rubenstein LZ (2008) Rehospitalization after hip fracture: predictors and prognosis from a national veterans study. J Am Geriatr Soc 56(4):705–710
Basques BA, Bohl DD, Golinvaux NS, Leslie MP, Baumgaertner MR, Grauer JN (2015) Postoperative length of stay and 30-day readmission after geriatric hip fracture: an analysis of 8434 patients. J Orthop Trauma 29(3):e115–e120
Kates SL, Shields E, Behrend C, Noyes KK (2015) Financial implications of hospital readmission after hip fracture. Geriatr Orthop Surg Rehabil 6(3):140–146
Schrøder H, Petersen KK, Erlandsen M (1993) Occurrence and incidence of the second hip fracture. Clin Orthop Relat Res 289:166–169
Ryg J, Rejnmark L, Overgaard S, Brixen K, Vestergaard P (2009) Hip fracture patients at risk of second hip fracture: a nationwide population-based cohort study of 169,145 cases during 1977-2001. J Bone Miner Res Off J Am Soc Bone Miner Res 24(7):1299–1307. https://doi.org/10.1359/jbmr.090207
Marmot M, Allen J, Goldblatt P, Boyce T, McNeish D, Grady M, Geddes I (2010) Fair society, healthy lives: strategic review of health inequalities in England post-2010. The Marmot Review 2010 February;Available from: http://www.marmotreview.org/
Acknowledgments
The authors acknowledge Jenny Neuburger for her considered comments to the manuscript. Susan Charman for access to the Stata code that she developed for calculating the Royal College of Surgeons Charlson score. We are grateful to NHS Digital, the Royal Collage of Physician’s Falls and Fragility Fracture Audit Programme, and the Office of National Statistics for providing the data used in this study and to Crown for extracting and supplying the data. The views expressed in this publication are those of the authors and do not necessarily reflect those of the NHS, the National Institute for Health Research or the Department of Health and Social Care. This publication is based on data collected by or on behalf of the Healthcare Quality Improvement Partnership, who have no responsibility or liability for the accuracy, currency, reliability and/or correctness of this publication.
Funding
RP and CLG are supported by Versus Arthritis (ref. 22086). CLG was funded by Versus Arthritis (ref. 20000). AB was supported by the Linda Edwards Memorial PhD studentship funded by the Royal Osteoporosis Society. YBS’s time is supported by the National Institute for Health Research (NIHR) Applied Research Collaboration West (ARC West) at University Hospitals Bristol NHS Foundation Trust.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
CLG chairs the Royal College of Physicians Falls and Fragility Fracture Audit Programme (FFFAP) Scientific and Publications committee (a voluntary position). RP, AB, and YBS declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 69.7 kb).
Rights and permissions
About this article
Cite this article
Patel, R., Bhimjiyani, A., Ben-Shlomo, Y. et al. Social deprivation predicts adverse health outcomes after hospital admission with hip fracture in England. Osteoporos Int 32, 1129–1141 (2021). https://doi.org/10.1007/s00198-020-05768-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05768-4