Abstract
Summary
We performed a cost-effectiveness analysis comparing 5 versus 10 years of alendronate treatment prior to 5-year drug holiday for US postmenopausal women with hip BMD T-scores between − 2.5 and − 3.5. We found that for most postmenopausal women 5 years of treatment prior to drug holiday is the more effective and cost-effective option.
Introduction
We performed a cost-effectiveness analysis to compare 5 versus 10 years of alendronate treatment prior to 5-year drug holiday for postmenopausal osteoporotic women.
Methods
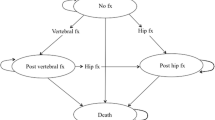
We created an individual-level state-transition microsimulation model to compare 3 treatment strategies for US postmenopausal women with osteoporosis and femoral neck BMD T-scores between − 2.5 and − 3.5 at baseline: recurrent periods of 5 years of alendronate followed by 5 years of drug holiday (alendronate 5/5), recurrent periods of 10 years of alendronate followed by 5 years of drug holiday (alendronate 10/5), and no alendronate treatment.
Results
Base-case analysis revealed for women initiating treatment at ages 50, 60, and 70, the alendronate 5/5 strategy dominated (was more effective and less costly than) the alendronate 10/5 strategy and no treatment. For women age 80, the alendronate 10/5 strategy dominated. When assuming a lower relative risk of nonvertebral fracture during years 6–10 of alendronate treatment than the base-case assumption, the alendronate 10/5 strategy became the most cost-effective strategy even at younger treatment initiation ages. Probabilistic sensitivity analysis results supported the base-case findings; for treatment initiation ages of 50, 60, and 70, the alendronate 5/5 strategy was favored, whereas for treatment initiation age of 80, the alendronate 10/5 strategy was favored; however, there was uncertainty in these findings.
Conclusions
After 5 years of alendronate treatment, younger postmenopausal women (ages 50–70) with osteoporosis would likely benefit from a drug holiday, whereas older women (age 80) are likely to benefit from treatment for 10 years before a drug holiday.


Similar content being viewed by others
References
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S, Dawson-Hughes B (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 29:2520–2526
US Department of Health and Human Services. Bone health and osteoporosis: a report of the surgeon general. Rockville, MD: US Department of Health and Human Services, Office of the Surgeon General, 2004
Osteoporosis prevention, diagnosis, and therapy. NIH Consens Statement. 2000;17(1):1–45
Lin JT, Lane JM (2004) Osteoporosis: a review. Clin Orthop Relat Res:126–134
Nguyen ND, Ahlborg HG, Center JR, Eisman JA, Nguyen TV (2007) Residual lifetime risk of fractures in women and men. J Bone Miner Res 22:781–788
Blume SW, Curtis JR (2011) Medical costs of osteoporosis in the elderly Medicare population. Osteoporos Int 22:1835–1844
Yang X, Sajjan S, Modi A (2016) High rate of non-treatment among osteoporotic women enrolled in a US Medicare plan. Curr Med Res Opin 32:1849–1856
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R, National Osteoporosis Foundation (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25:2359–2381
Adler RA, El-Hajj Fuleihan G, Bauer DC, Camacho PM, Clarke BL, Clines GA, Compston JE, Drake MT, Edwards BJ, Favus MJ, Greenspan SL, McKinney R Jr, Pignolo RJ, Sellmeyer DE (2016) Managing osteoporosis in patients on long-term bisphosphonate treatment: report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 31:16–35
Nayak S, Greenspan SL (2019) A systematic review and meta-analysis of the effect of bisphosphonate drug holidays on bone mineral density and osteoporotic fracture risk. Osteoporos Int 30:705–720
Black DM, Schwartz AV, Ensrud KE, Cauley JA, Levis S, Quandt SA, Satterfield S, Wallace RB, Bauer DC, Palermo L, Wehren LE, Lombardi A, Santora AC, Cummings SR, FLEX Research Group (2006) Effects of continuing or stopping alendronate after 5 years of treatment: the fracture intervention Trial long-term extension (FLEX): a randomized trial. JAMA 296:2927–2938
Jackson SA, Tenenhouse A, Robertson L (2000) Vertebral fracture definition from population-based data: preliminary results from the Canadian multicenter osteoporosis study (CaMos). Osteoporos Int 11:680–687
Looker AC, Borrud LG, Hughes JP, Fan B, Shepherd JA, Melton LJ 3rd (2012) Lumbar spine and proximal femur bone mineral density, bone mineral content, and bone area: United States, 2005-2008. Vital Health Stat 11(251):1–132
Black DM, Thompson DE, Bauer DC, Ensrud K, Musliner T, Hochberg MC, Nevitt MC, Suryawanshi S, Cummings SR, Trial FI (2000) Fracture risk reduction with alendronate in women with osteoporosis: the Fracture Intervention Trial. FIT Research Group. J Clin Endocrinol Metab 85:4118–4124
Krege JH, Wan X, Lentle BC, Berger C, Langsetmo L, Adachi JD, Prior JC, Tenenhouse A, Brown JP, Kreiger N, Olszynski WP, Josse RG, Goltzman D, CaMos Research Group (2013) Fracture risk prediction: importance of age, BMD and spine fracture status. Bonekey Rep 2:404
Fink HA, Milavetz DL, Palermo L, Nevitt MC, Cauley JA, Genant HK, Black DM, Ensrud KE (2005) What proportion of incident radiographic vertebral deformities is clinically diagnosed and vice versa? J Bone Miner Res 20:1216–1222
PharmacyChecker.com. Available at: http://pharmacychecker.com
Kilgore ML, Curtis JR, Delzell E, Becker DJ, Arora T, Saag KG, Morrisey MA (2013) A close examination of healthcare expenditures related to fractures. J Bone Miner Res 28:816–820
Genworth 2018 Cost of Care Survey. Available at https://www.genworth.com/aging-and-you/finances/cost-of-care.html
Boston Scientific 2018 GI Procedural Reimbursement Guide. Available at: https://www.bostonscientific.com
Centers for Medicare and Medicaid Services. National Physician Fee Schedule. Available at: https://www.cms.gov/apps/physician-fee-schedule/overview.aspx
Fryback DG, Dunham NC, Palta M, Hanmer J, Buechner J, Cherepanov D, Herrington SA, Hays RD, Kaplan RM, Ganiats TG, Feeny D, Kind P (2007) US norms for six generic health-related quality-of-life indexes from the National Health Measurement study. Med Care 45:1162–1170
Hiligsmann M, Ethgen O, Richy F, Reginster JY (2008) Utility values associated with osteoporotic fracture: a systematic review of the literature. Calcif Tissue Int 82:288–292
Brazier JE, Green C, Kanis JA (2002) A systematic review of health state utility values for osteoporosis-related conditions. Osteoporos Int 13:768–776
Solomon DH, Patrick AR, Schousboe J, Losina E (2014) The potential economic benefits of improved postfracture care: a cost-effectiveness analysis of a fracture liaison service in the US health-care system. J Bone Miner Res 29:1667–1674
Tajeu GS, Delzell E, Smith W, Arora T, Curtis JR, Saag KG, Morrisey MA, Yun H, Kilgore ML (2014) Death, debility, and destitution following hip fracture. J Gerontol A Biol Sci Med Sci 69:346–353
Orces CH (2013) In-hospital hip fracture mortality trends in older adults: the National Hospital Discharge Survey, 1988-2007. J Am Geriatr Soc 61:2248–2249
LeBlanc ES, Hillier TA, Pedula KL, Rizzo JH, Cawthon PM, Fink HA, Cauley JA, Bauer DC, Black DM, Cummings SR, Browner WS (2011) Hip fracture and increased short-term but not long-term mortality in healthy older women. Arch Intern Med 171:1831–1837
Sanders GD, Neumann PJ, Basu A, Brock DW, Feeny D, Krahn M, Kuntz KM, Meltzer DO, Owens DK, Prosser LA, Salomon JA, Sculpher MJ, Trikalinos TA, Russell LB, Siegel JE, Ganiats TG (2016) Recommendations for conduct, methodological practices, and reporting of cost-effectiveness analyses: second panel on cost-effectiveness in health and medicine. JAMA 316:1093–1103
Tosteson AN, Jonsson B, Grima DT, O’Brien BJ, Black DM, Adachi JD (2001) Challenges for model-based economic evaluations of postmenopausal osteoporosis interventions. Osteoporos Int 12:849–857
Ettinger B, Black DM, Dawson-Hughes B, Pressman AR, Melton LJ 3rd (2010) Updated fracture incidence rates for the US version of FRAX. Osteoporos Int 21:25–33
Johnell O, Kanis JA, Oden A, Johansson H, De Laet C, Delmas P, Elsman JA, Fujiwara S, Kroger H, Mellstrom D, Meunier PJ, Melton LJ III, O’Neill T, Pols H, Reeve J, Silman A, Tenenhouse A (2005) Predictive value of BMD for hip and other fractures. J Bone Miner Res 20:1185–1194
Cummings SR, Cawthon PM, Ensrud KE, Cauley JA, Fink HA, Orwoll ES (2006) BMD and risk of hip and nonvertebral fractures in older men: a prospective study and comparison with older women. J Bone Miner Res 21:1550–1556
Brown JP, Morin S, Leslie W, Papaioannou A, Cheung AM, Davison KS, Goltzman D, Hanley DA, Hodsman A, Josse R, Jovaisas A, Juby A, Kaiser S, Karaplis A, Kendler D, Khan A, Ngui D, Olszynski W, Ste-Marie LG, Adachi J (2014) Bisphosphonates for treatment of osteoporosis: expected benefits, potential harms, and drug holidays. Can Fam Physician 60:324–333
Black DM, Cummings SR, Karpf DB, Cauley JA, Thompson DE, Nevitt MC, Bauer DC, Genant HK, Haskell WL, Marcus R, Ott SM, Torner JC, Quandt SA, Reiss TF, Ensrud KE (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Fracture Intervention Trial Research Group. Lancet 348:1535–1541
Society of Actuaries Long-Term Care Experience Committee Intercompany Study Report 6 1984-2007. Available at: https://www.soa.org/globalassets/assets/files/research/exp-study/research-ltc-study-1984-report.pdf
Arias E, Xu J (2018) United States life tables, 2015. Natl Vital Stat Rep 67:1–64
Social Security Administration Actuarial Life Table. Available at: https://www.ssa.gov/oact/STATS/table4c6.html
Shiroiwa T, Sung YK, Fukuda T, Lang HC, Bae SC, Tsutani K (2010) International survey on willingness-to-pay (WTP) for one additional QALY gained: what is the threshold of cost effectiveness? Health Econ 19:422–437
Black DM, Cauley JA, Wagman R, Ensrud K, Fink HA, Hillier TA, Lui LY, Cummings SR, Schousboe JT, Napoli N (2018) The ability of a single BMD and fracture history assessment to predict fracture over 25 years in postmenopausal women: the study of osteoporotic fractures. J Bone Miner Res 33:389–395
Funding
Drs. Nayak and Greenspan were supported by grant no. R21AR072930 from the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Dr. Greenspan was also supported by NIH grants P30AG024827, K07AG052668, and R01AG050302 from the National Institute on Aging.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
Smita Nayak declares no conflict of interest. Susan L. Greenspan receives research funding from Amgen and Radius.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 36.2 kb)
Rights and permissions
About this article
Cite this article
Nayak, S., Greenspan, S.L. Cost-effectiveness of five versus ten years of alendronate treatment prior to drug holiday for women with osteoporosis. Osteoporos Int 31, 1273–1282 (2020). https://doi.org/10.1007/s00198-019-05258-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05258-2