Abstract
Summary
Vitamin D (VD) plays an important role in bone mineralization. The present study investigates the effect of VD supplementation alone on bone turnover markers in younger postmenopausal women. It has been shown that VD supplementation in postmenopausal women with hypovitaminosis D is associated with a reduction in bone turnover markers.
Purpose
The purpose of this study is to evaluate the effect of VD supplementation alone on bone turnover markers in younger postmenopausal women.
Methods
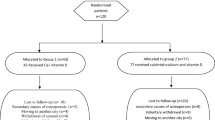
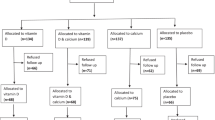
In this double-blind, placebo-controlled trial, 160 women were randomized into the VD group (supplementation with 1000 IU of vitamin D3/day, orally; n = 80) or placebo group (n = 80). Women aged 50–65 years with amenorrhea ≥ 12 months and normal bone mineral density were included. The intervention lasted 9 months, and the participants were assessed at the beginning and end of treatment. Serum levels of total calcium, parathormone (PTH), alkaline phosphatase (AP), and 24-h urine calcium were determined. Serum C-terminal telopeptide of type I collagen (s-CTX) and procollagen type 1 N-terminal propeptide (P1NP) were measured by immunoassay as markers of bone resorption and formation, respectively. Plasma 25-hydroxyvitamin-D [25(OH)D] concentrations were measured by HPLC. Intention-to-treat analysis was performed using ANOVA, Student’s t test, Tukey’s test, and gamma distribution.
Results
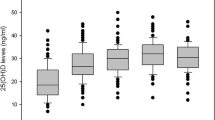
Over the period of 9 months, 25(OH)D concentrations increased from 15.0 ± 7.5 to 27.5 ± 10.4 ng/mL (+ 45.4%) in the VD group and decreased from 16.9 ± 6.7 to 13.8 ± 6.0 ng/mL (− 18.5%) in the placebo group (p < 0.001). There was a decrease (− 21.3%) of PTH levels in the VD group with a significant difference between groups at the end of the study (p < 0.001). No significant differences were observed in the other laboratory parameters (total calcium, AP, and calciuria) in either group (p > 0.05). A comparison of bone turnover markers showed a significant reduction in of s-CTX (− 24.2%, p < .0001) and P1NP (− 13.4%, p = 0.003) levels in the VD group. No significant variations in bone turnover markers were observed in the placebo group (s-CTX, − 6.9%, p = 0.092 and P1NP, − 0.6%, p = 0.918).
Conclusion
In younger postmenopausal women with VD deficiency, isolated supplementation with 1000 IU of vitamin D3 for 9 months is associated with a reduction in bone turnover markers. However, any between-group differences was not observed in bone turnover markers.

Similar content being viewed by others
References
Cavalier E, Bergmann P, Bruyère O, Delanaye P, Durnez A, Devogelaer JP, Ferrari SL, Gielen E, Goemaere S, Kaufman JM, Toukap AN, Reginster JY, Rousseau AF, Rozenberg S, Scheen AJ, Body JJ (2016) The role of biochemical of bone turnover markers in osteoporosis and metabolic bone disease: a consensus paper of the Belgian Bone Club. Osteoporos Int 27:2181–2195
Position Statement (2010) Management of osteoporosis in postmenopausal women: 2010 position statement of The North American Menopause Society. Menopause 17:25–54
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25:2359–2381
Ivaska KK, Lenora J, Gerdhem P, Akesson K, Väänänen HK, Obrant KJ (2008) Serial assessment of serum bone metabolism markers identifies women with highest rate of bone loss and osteoporosis risk. J Clin Endocrinol Metab 93:2622–2632
Bieglmayer C, Kudlacek S (2009) The bone marker plot: an innovative method to assess bone turnover in women. Eur J Clin Investig 39:230–238
Garnero P, Hausherr E, Chapuy MC, Marcelli C, Grandjean H, Muller C, Cormier C, Bréart G, Meunier PJ, Delmas PD (1996) Markers of bone resorption predict hip fracture in elderly women: the EPIDOS Prospective Study. J Bone Miner Res 11:1531–1538
Reginster JY, Collette J, Neuprez A, Zegels B, Deroisy R, Bruyere O (2008) Role of biochemical markers of bone turnover as prognostic indicator of successful osteoporosis therapy. Bone 42:832–836
Vasikaran SD, Glendenning P, Morris HA (2006) The role of biochemical markers of bone turnover in osteoporosis management in clinical practice. Clin Biochem Rev 27:119–121
Rosen CJ (2011) Vitamin D insufficiency. N Engl J Med 364:248–254
Uitterlinden AG, Fang Y, Van Meurs JB, Pols HA, Van Leeuwen JP (2004) Genetics and biology of vitamin D receptor polymorphisms. Gene 338:143–156
Dawson-Hughes B, Heaney RP, Holick MF, Vieth R, Dawson-Hughes B, Heaney RP (2005) Estimated of optimal vitamin D status. Osteoporos Int 16:713–716
Holick MF (2010) The D-lemma: to screen or not to screen for 25-hydroxyvitamin D concentrations. Clin Chemistry 56:729–731
Holick MF (2007) Vitamin D deficiency. N Engl J Med 357:266–281
Wimalawansa SJ, Razzaque DMS, Al-Daghri NM (2017) Calcium and vitamin D in human health: hype or real? J Steroid Biochem Mol Biol. https://doi.org/10.1016/j.jsbmb.2017.12.009
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP (2011) Evaluation, treatment, and prevention of vitamin D deficiency: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 96:1911–1930
Rosen CJ, Abrams SA, Aloia JF, Brannon PM, Clinton SK, Durazo-Arvizu RA, Gallagher JC, Gallo RL, Jones G, Kovacs CS, Manson JE, Mayne ST, Ross AC, Shapses SA, Taylor CL (2012) IOM committee members respond to Endocrine Society vitamin D guideline. J Clin Endocrinol Metab 97:1146–1152
Macdonald HM, Wood AD, Aucott LS, Black AJ, Fraser WD, Mavroeidi A, Reid DM, Secombes KR, Simpson WG, Thies F (2013) Hip bone loss is attenuated with 1000 IU but not 400 IU daily vitamin D3: a 1-year double-blind RCT in postmenopausal women. J Bone Mineral Res 28:2202–2213
Schwetz V, Trummer C, Pandis M, Grübler MR, Verheyen N, Gaksch M, Zittermann A, März W, Aberer F, Lang A, Treiber G, Friedl C, Obermayer-Pietsch B, Pieber TR, Tomaschitz A, Pilz S (2017) Effects of vitamin D supplementation on bone turnover markers: a randomized controlled trial. Nutrients. https://doi.org/10.3390/nu9050432
Tang BM, Eslick GD, Nowson C, Smith C, Bensoussan A (2007) Use of calcium or calcium in combination with vitamin D supplementation to prevent fractures and bone loss in people aged 50 years and older: a meta-analysis. Lancet 370:657–666
Reid IR, Bolland MJ, Grey A (2014) Effects of vitamin D supplements on bone mineral density: a systematic review and meta-analysis. Lancet 383:146–155
EFSA Panel on Dietetic Products, Nutrition and Allergies (NDA) (2016) Scientific opinion on dietary reference values for vitamin D. EFSA J 14:4547
Madar AA, Knutsen KV, Stene LC, Brekke M, Lagerløv P, Meyer HE, Macdonald HM (2015) Effect of vitamin D3-supplementation on bone markers (serumP1NP and CTX): a randomized, double blinded, placebo controlled trial among healthy immigrants living in Norway. Bone Reports 2:82–88
Andersen R, Molgaard C, Skovgaard LT, Brot C, Cashman KD, Jakobsen J (2008) Effect of vitamin D supplementation on bone and vitamin D status among Pakistani immigrants in Denmark: a randomised double-blinded placebo-controlled intervention study. Br J Nutr 100:197–207
Viljakainen HT, Vaisanen M, Kemi V, Rikkonen T, Kröger H, Laitinen EK, Rita H, Lamberg-Allardt C (2009) Wintertime vitamin D supplementation inhibits seasonal variation of calcitropic hormones and maintains bone turnover in healthy men. J Bone Miner Res 24:346–352
Cangussu LM, Nahas-Neto J, Orsatti CL, Poloni PF, Schmitt EB, Almeida-Filho B, Nahas EAP (2016) Effect of isolated vitamin D supplementation on the rate of falls and postural balance in postmenopausal women fallers: a randomized, double-blind, placebo-controlled trial. Menopause 23:267–274
Cangussu LM, Nahas-Neto J, Orsatti CL, Bueloni-Dias F, Nahas EAP (2015) Effect of vitamin D supplementation alone on muscle function in postmenopausal women: a randomized, double-blind, placebo-controlled clinical trial. Osteoporos Int 26:2413–2421
Schulz KF, Altman DG, Moher D, Group C (2010) CONSORT 2010 statement: updated guidelines for reporting parallel group randomized trials. Ann Intern Med 152(11):726–732
Executive Summary of the Third report of the National Cholesterol Education Program (NCEP) (2002) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation 106:3143–3421
Bischoff-Ferrari HA, Giovannucci E, Willett WC, Dietrich T, Dawson-Hughes B (2006) Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr 84:18–28
Paul Chubb SA (2012) Measurement of C-terminal telopeptide of type I collagen (CTX) in serum. Clin Biochem 45:928–935
Glover SJ, Gall M, Schoenborn-Kellenberger O, Wagener M, Garnero P, Boonen S, Cauley JA, Black DM, Delmas PD, Eastell R (2009) Establishing a reference interval for bone turnover markers in 637 healthy, young, premenopausal women from the United Kingdom, France, Belgium, and the United States. J Bone Miner Res 24:389–397
Grados F, Brazier M, Kamel S, Mathieu M, Hurtebize N, Maamer M, Garabédian M, Sebert JL, Fardellone P (2003) Prediction of bone mass density variation by bone remodeling markers in postmenopausal women with vitamin D insufficiency treated with calcium and vitamin D supplementation. J Clin Endocrinol Metab 88:5175–5179
Compstom J (2009) Monitoring osteoporosis treatment. Best Pract Res Clin Rheumatol 23:781–788
Garnero P, Munoz F, Sornay-Rendu E, Delmas PD (2007) Associations of vitamin D status with bone mineral density, bone turnover, bone loss and fracture risk in health postmenopausal women The OFELY study. Bone 40:716–722
Aloia JF, Dhaliwal R, Shieh A, Mikhail M, Islam S, Yeh JK (2013) Calcium and vitamin D supplementation in postmenopausal women. J Clin Endocrinol Metab 98:E1702–E1709
Rossini M, Adami S, Viapiana O, Fracassi E, Idolazzi L, Povino MR, Gatti D (2012) Dose-dependent short-term effects of single high doses of oral vitamin D3 on bone turnover markers. Calcif Tissue Int 91:365–369
Grimnes G, Joakimsen R, Figenschau Y, Torjesen PA, Almås B, Jorde R (2012) The effect of high-dose vitamin D on bone mineral density and bone turnover markers in postmenopausal women with low bone mass-a randomized controlled 1-year trial. Osteoporos Int 23:201–211
Garnero P, Vergnaud P, Hoyle N (2008) Evaluation of a fully automated serum assay for total N-terminal propeptide of type I collagen in postmenopausal osteoporosis. Clin Chem 54:188–196
Funck-Brentano T, Biver E, Chopin F, Bouvard B, Coiffier G, Souberbielle JC, Garnero P, Roux C (2011) Clinical utility of serum bone turnover markers in postmenopausal osteoporosis therapy monitoring: a systematic review. Semin Arthritis Rheum 41:157–169
Koivula MK, Risteli L, Risteli J (2012) Measurement of aminoterminal propeptide of type I procollagen (PINP) in serum. Clin Biochem 45:920–927
Vasikaran S, Eastell R, Bruyère O, Foldes AJ, Garnero P, Griesmacher A, McClung M, Morris HA, Silverman S, Trenti T, Wahl DA, Cooper C, Kanis JA, IOF-IFCC Bone Marker Standards Working Group (2011) Markers of bone turnover for the prediction of fracture risk and monitoring of osteoporosis treatment: a need for international reference standards. Osteoporos Int 22:391–420
Ford L (2013) Measurement of vitamin D. Methods Mol Biol 1065:245–257
Funding
This work was supported by grants from the São Paulo Research Foundation (FAPESP) process number 2014/00001-0.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent was obtained from all participants, and the study was approved by the Research Ethics Committee of the Botucatu Medical School, UNESP.
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Nahas-Neto, J., Cangussu, L.M., Orsatti, C.L... et al. Effect of isolated vitamin D supplementation on bone turnover markers in younger postmenopausal women: a randomized, double-blind, placebo-controlled trial. Osteoporos Int 29, 1125–1133 (2018). https://doi.org/10.1007/s00198-018-4395-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-018-4395-y