Abstract
Summary
DXA-measured lean mass is often used to assess muscle mass but has limitations. Thus, we compared DXA lean mass with two novel methods—bioelectric impedance spectroscopy and creatine (methyl-d3) dilution. The examined methodologies did not measure lean mass similarly and the correlation with muscle biomarkers/function varied.
Introduction
Muscle function tests predict adverse health outcomes better than lean mass measurement. This may reflect limitations of current mass measurement methods. Newer approaches, e.g., bioelectric impedance spectroscopy (BIS) and creatine (methyl-d3) dilution (D3-C), may more accurately assess muscle mass. We hypothesized that BIS and D3-C measured muscle mass would better correlate with function and bone/muscle biomarkers than DXA measured lean mass.
Methods
Evaluations of muscle/lean mass, function, and serum biomarkers were obtained in older community-dwelling adults. Mass was assessed by DXA, BIS, and orally administered D3-C. Grip strength, timed up and go, and jump power were examined. Potential muscle/bone serum biomarkers were measured. Mass measurements were compared with functional and serum data using regression analyses; differences between techniques were determined by paired t tests.
Results
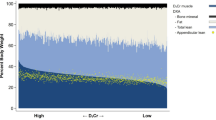
Mean (SD) age of the 112 (89F/23M) participants was 80.6 (6.0) years. The lean/muscle mass assessments were correlated (.57–.88) but differed (p < 0.0001) from one another with DXA total body less head being highest at 37.8 (7.3) kg, D3-C muscle mass at 21.1 (4.6) kg, and BIS total body intracellular water at 17.4 (3.5) kg. All mass assessment methods correlated with grip strength and jump power (R = 0.35–0.63, p < 0.0002), but not with gait speed or repeat chair rise. Lean mass measures were unrelated to the serum biomarkers measured.
Conclusions
These three methodologies do not similarly measure muscle/lean mass and should not be viewed as being equivalent. Functional tests assessing maximal muscle strength/power (grip strength and jump power) correlated with all mass measures whereas gait speed was not. None of the selected serum measures correlated with mass. Efforts to optimize muscle mass assessment and identify their relationships with health outcomes are needed.



Similar content being viewed by others
References
Clynes MA, Edwards MH, Buehring B, Dennison EM, Binkley N, Cooper C (2015) Definitions of sarcopenia: associations with previous falls and fracture in a population sample. Calcif Tissue Int 97(5):445–452
Landi F, Liperoti R, Russo A, Giovannini S, Tosato M, Capoluongo E, Bernabei R, Onder G (2012) Sarcopenia as a risk factor for falls in elderly individuals: results from the ilSIRENTE study. Clin Nutr 31(5):652–658
Cruz-Jentoft AJ, Landi F (2014) Sarcopenia. Clin Med 14(2):183–186
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, Martin FC, Michel JP, Rolland Y, Schneider SM, Topinkova E, Vandewoude M, Zamboni M (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European working group on sarcopenia in older people. Age Ageing 39(4):412–423
Studenski SA, Peters KW, Alley DE, Cawthon PM, McLean RR, Harris TB, Ferrucci L, Guralnik JM, Fragala MS, Kenny AM, Kiel DP, Kritchevsky SB, Shardell MD, Dam TT, Vassileva MT (2014) The FNIH sarcopenia project: rationale, study description, conference recommendations, and final estimates. J Gerontol Ser A-Biol Sci Med Sci 69(5):547–558
Fielding RA, Vellas B, Evans WJ, Bhasin S, Morley JE, Newman AB, Abellan van Kan G, Andrieu S, Bauer J, Breuille D, Cederholm T, Chandler J, De Meynard C, Donini L, Harris T, Kannt A, Keime Guibert F, Onder G, Papanicolaou D, Rolland Y, Rooks D, Sieber C, Souhami E, Verlaan S, Zamboni M (2011) Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 12(4):249–256
Dawson-Hughes B, Bischoff-Ferrari H (2016) Considerations concerning the definition of sarcopenia. Osteoporos Int 27(11):3139–3144
Ellis KJ (2000) Human body composition: in vivo methods. Physiol Rev 80(2):649–680
Guglielmi G, Ponti F, Agostini M, Amadori M, Battista G, Bazzocchi A 2016 The role of DXA in sarcopenia. Aging Clinical and Experimental Research
Cawthon PM, Fox KM, Gandra SR, Delmonico MJ, Chiou CF, Anthony MS, Sewall A, Goodpaster B, Satterfield S, Cummings SR, Harris TB (2009) Do muscle mass, muscle density, strength, and physical function similarly influence risk of hospitalization in older adults? J Am Geriatr Soc 57(8):1411–1419
Newman AB, Kupelian V, Visser M, Simonsick EM, Goodpaster BH, Kritchevsky SB, Tylavsky FA, Rubin SM, Harris TB (2006) Strength, but not muscle mass, is associated with mortality in the health, aging and body composition study cohort. J Gerontol Ser A-Biol Sci Med Sci 61(1):72–77
Visser M, Goodpaster BH, Kritchevsky SB, Newman AB, Nevitt M, Rubin SM, Simonsick EM, Harris TB (2005) Muscle mass, muscle strength, and muscle fat infiltration as predictors of incident mobility limitations in well-functioning older persons. J Gerontol Ser A-Biol Sci Med Sci 60(3):324–333
Yamada Y, Watanabe Y, Ikenaga M, Yokoyama K, Yoshida T, Morimoto T, Kimura M (2013) Comparison of single- or multifrequency bioelectrical impedance analysis and spectroscopy for assessment of appendicular skeletal muscle in the elderly. J Appl Physiol 115(6):812–818
Clark RV, Walker AC, O'Connor-Semmes RL, Leonard MS, Miller RR, Stimpson SA, Turner SM, Ravussin E, Cefalu WT, Hellerstein MK, Evans WJ (2014) Total body skeletal muscle mass: estimation by creatine (methyl-d3) dilution in humans. J Appl Physiol 116(12):1605–1613
Yamada Y, Schoeller DA, Nakamura E, Morimoto T, Kimura M, Oda S (2010) Extracellular water may mask actual muscle atrophy during aging. J Gerontol Ser A-Biol Sci Med Sci 65(5):510–516
Yamada Y, Buehring B, Krueger D, Binkley N, Schoeller DA (2014) Improving muscle mass measurement using bioelectrical impedance spectroscopy. J Clin Densitom 17:401–402
Yamada Y, Ikenaga M, Takeda N, Morimura K, Miyoshi N, Kiyonaga A, Kimura M, Higaki Y, Tanaka H 2013 Estimation of thigh muscle cross-sectional area by single- and multi-frequency segmental bioelectrical impedance analysis in the elderly. J Appl Physiol
Bartok C, Schoeller DA (2004) Estimation of segmental muscle volume by bioelectrical impedance spectroscopy. J Appl Physiol 96(1):161–166
Norman K, Stobaus N, Gonzalez MC, Schulzke JD, Pirlich M (2011) Hand grip strength: outcome predictor and marker of nutritional status. Clin Nutr 30(2):135–142
Studenski S, Perera S, Patel K, Rosano C, Faulkner K, Inzitari M, Brach J, Chandler J, Cawthon P, Connor EB, Nevitt M, Visser M, Kritchevsky S, Badinelli S, Harris T, Newman AB, Cauley J, Ferrucci L, Guralnik J (2011) Gait speed and survival in older adults. JAMA 305(1):50–58
Guralnik JM, Ferrucci L, Pieper CF, Leveille SG, Markides KS, Ostir GV, Studenski S, Berkman LF, Wallace RB (2000) Lower extremity function and subsequent disability: consistency across studies, predictive models, and value of gait speed alone compared with the short physical performance battery. Journals of gerontology series A-biological sciences and medical. Sciences 55(4):M221–M231
Bohannon RW (2008) Hand-grip dynamometry predicts future outcomes in aging adults. J Geriatr Phys Ther 31(1):3–10
Leong DP, Teo KK, Rangarajan S, Lopez-Jaramillo P, Avezum A Jr, Orlandini A, Seron P, Ahmed SH, Rosengren A, Kelishadi R, Rahman O, Swaminathan S, Iqbal R, Gupta R, Lear SA, Oguz A, Yusoff K, Zatonska K, Chifamba J, Igumbor E, Mohan V, Anjana RM, Gu H, Li W, Yusuf S (2015) Prognostic value of grip strength: findings from the prospective urban rural epidemiology (PURE) study. Lancet 386(9990):266–273
Cawthon PM, Fullman RL, Marshall L, Mackey DC, Fink HA, Cauley JA, Cummings SR, Orwoll ES, Ensrud KE (2008) Physical performance and risk of hip fractures in older men. J Bone Miner Res 23(7):1037–1044
Siglinsky E, Krueger D, Ward RE, Caserotti P, Strotmeyer ES, Harris TB, Binkley N, Buehring B (2015) Effect of age and sex on jumping mechanography and other measures of muscle mass and function. J Musculoskelet Neuronal Interact 15(4):301–308
Buehring B, Krueger D, Fidler E, Gangnon R, Heiderscheit B, Binkley N (2015) Reproducibility of jumping mechanography and traditional measures of physical and muscle function in older adults. Osteoporos Int 26(2):819–825
Hamrick MW (2011) A role for myokines in muscle-bone interactions. Exerc Sport Sci Rev 39(1):43–47
Pedersen BK, Febbraio MA (2012) Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nature reviews. Endocrinology 8(8):457–465
Lightfoot AP, Cooper RG (2016) The role of myokines in muscle health and disease. Curr Opin Rheumatol 28(6):661–666
Brotto M, Bonewald L (2015) Bone and muscle: interactions beyond mechanical. Bone 80:109–114
Abreu EL, Cheng AL, Kelly PJ, Chertoff K, Brotto L, Griffith E, Kinder G, Uridge T, Zachow R, Brotto M (2014) Skeletal muscle troponin as a novel biomarker to enhance assessment of the impact of strength training on fall prevention in the older adults. Nurs Res 63(2):75–82
Ilich JZ, Kelly OJ, Inglis JE, Panton LB, Duque G, Ormsbee MJ (2014) Interrelationship among muscle, fat, and bone: connecting the dots on cellular, hormonal, and whole body levels. Ageing Res Rev 15:51–60
Tagliaferri C, Wittrant Y, Davicco MJ, Walrand S, Coxam V (2015) Muscle and bone, two interconnected tissues. Ageing Res Rev 21:55–70
Buehring B, Binkley N (2013) Myostatin--the holy grail for muscle, bone, and fat? Current Osteoporosis Reports 11(4):407–414
Krueger D, Siglinsky E, Buehring B, Binkley N 2016 Total body less head measurement is most appropriate for lean mass assessment in adults. J Clin Densitom
Yamada Y, Buehring B, Krueger D, Anderson RM, Schoeller DA, Binkley N 2016 Electrical properties assessed by bioelectrical impedance spectroscopy as biomarkers of age-related loss of skeletal muscle quantity and quality. J Gerontol Ser A Biol Sci Med Sci
Wadsworth CT, Krishnan R, Sear M, Harrold J, Nielsen DH (1987) Intrarater reliability of manual muscle testing and hand-held dynametric muscle testing. Phys Ther 67(9):1342–1347
Guralnik JM, Simonsick EM, Ferrucci L, Glynn RJ, Berkman LF, Blazer DG, Scherr PA, Wallace RB (1994) A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 49(2):M85–M94
Dobson F (2015) Timed up and go test in musculoskeletal conditions. J Phys 61(1):47
Zeng P, Han Y, Pang J, Wu S, Gong H, Zhu J, Li J, Zhang T (2016) Sarcopenia-related features and factors associated with lower muscle strength and physical performance in older Chinese: a cross sectional study. BMC Geriatr 16:45
Falsarella GR, Gasparotto LP, Barcelos CC, Coimbra IB, Moretto MC, Pascoa MA, Ferreira TC, Coimbra AM (2015) Body composition as a frailty marker for the elderly community. Clin Interv Aging 10:1661–1666
Dodds RM, Syddall HE, Cooper R, Benzeval M, Deary IJ, Dennison EM, Der G, Gale CR, Inskip HM, Jagger C, Kirkwood TB, Lawlor DA, Robinson SM, Starr JM, Steptoe A, Tilling K, Kuh D, Cooper C, Sayer AA (2014) Grip strength across the life course: normative data from twelve British studies. PLoS One 9(12):e113637
Rantanen T, Guralnik JM, Foley D, Masaki K, Leveille S, Curb JD, White L (1999) Midlife hand grip strength as a predictor of old age disability. J Am Med Assoc 281(6):558–560
Cooper R, Kuh D, Cooper C, Gale CR, Lawlor DA, Matthews F, Hardy R, Falcon THAS (2011) Objective measures of physical capability and subsequent health: a systematic review. Age Ageing 40(1):14–23
Hofmann M, Halper B, Oesen S, Franzke B, Stuparits P, Tschan H, Bachl N, Strasser EM, Quittan M, Ploder M, Wagner KH, Wessner B (2015) Serum concentrations of insulin-like growth factor-1, members of the TGF-beta superfamily and follistatin do not reflect different stages of dynapenia and sarcopenia in elderly women. Exp Gerontol 64:35–45
Kawao N, Kaji H (2015) Interactions between muscle tissues and bone metabolism. J Cell Biochem 116(5):687–695
Coletti D, Daou N, Hassani M, Li Z, Parlakian A (2016) Serum response factor in muscle tissues: from development to ageing. Eur J Transl Myol 26(2):6008
Acknowledgements
The authors want to thank Helen Werner for her statistical analysis expertise and assistance with this project as well as Scott Turner, Shubha Shankaran, and Gregg Czerwieniec at Kinemed for their help with D3-creatine data analysis and interpretation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Buehring has received a grant from the UW Department of Medicine to conduct the study; additionally, he received grants from Extendicare Foundation, personal fees from Clinical Care Options, GE/Lunar, Janssen outside of the submitted work. Ms. Siglinsky, Ms. Krueger and Dr. Yamada does not have any conflict of interest. Drs. Hellerstein and Evans were KineMed, Inc. at the time the study was conducted. Dr. Binkley NB has received consultancy fees from Amgen and Radius and research grants from Amgen, GE Healthcare, Lilly, Merck, Novartis, and Viking outside of the submitted work.
Rights and permissions
About this article
Cite this article
Buehring, B., Siglinsky, E., Krueger, D. et al. Comparison of muscle/lean mass measurement methods: correlation with functional and biochemical testing. Osteoporos Int 29, 675–683 (2018). https://doi.org/10.1007/s00198-017-4315-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-017-4315-6