Abstract
Summary
To determine whether new national guidance on the specifications of a fracture liaison service are realistically deliverable, 1 year of data on the performance of such a service were audited. Audit targets were mostly met. This audit demonstrates that these standards are deliverable in a real world setting.
Introduction
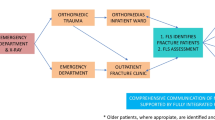
UK service specifications for a fracture liaison service (FLS) have been produced (National Osteoporosis Society, NOS) to promote effective commissioning and delivery of the highest quality care to patients with fragility fractures. How deliverable these standards are has not as yet been methodically reported. Our FLS was modelled on the ten NOS standards; performance was audited after 1 year to determine whether these standards could be delivered and to describe the lessons learnt.
Methods
Performance was audited against the NOS FLS Service Standards, with management based on the Fracture Risk Assessment Tool (FRAX®), the four-item Falls Risk Assessment Tool (FRAT), National Institute for Health and Care Excellence (NICE) and the National Osteoporosis Guideline Groups (NOGG) guidance. Data were recorded prospectively on a database. The FLS commenced in May 2014, was fully operational in August 2014 and data were captured from 1 September 2014 to 1 September 2015.
Results
The FLS detected 1773 patients and standards were largely achieved. Most, 94 %, patients were seen within 6 weeks, 533 DXA requests were generated, 804 outpatient FRAT assessments were recorded (134 required falls intervention) and 773 patients had bone treatments started. On follow-up at 3 months, between 78–79 % were still taking medication.
Conclusions
Preliminary evaluation of a FLS implemented according to UK NOS standards demonstrates that the model is practical to apply to a large teaching hospital population. Collection and review of outcome and cost effectiveness data is required to determine the performance of this model in comparison with existing models.


Similar content being viewed by others
References
van Staa TP, Dennison EM, Leufkens HG, Cooper C (2001) Epidemiology of fractures in England and Wales. Bone 29(6):517–522
National Osteoporosis Society (2015) Effective secondary prevention of fragility fractures: clinical standards for fracture liaison services. https://www.nos.org.uk/document.doc?id=1941. Accessed 26th September 2015
National Osteopororsis Society (2014) Life with osteoporosis: the untold story. National Osteoporosis Society, Bath
McLellan AR, Wolowacz SE, Zimovetz EA, Beard SM, Lock S, McCrink L, Adekunle F, Roberts D (2011) Fracture liaison services for the evaluation and management of patients with osteoporotic fracture: a cost-effectiveness evaluation based on data collected over 8 years of service provision. Osteoporos Int 22(7):2083–2098. doi:10.1007/s00198-011-1534-0
Nakayama A, Major G, Holliday E, Attia J, Bogduk N (2015) Evidence of effectiveness of a fracture liaison service to reduce the re-fracture rate. Osteoporos Int. doi:10.1007/s00198-015-3443-0
Huntjens KM, van Geel TA, van den Bergh JP, van Helden S, Willems P, Winkens B, Eisman JA, Geusens PP, Brink PR (2014) Fracture liaison service: impact on subsequent nonvertebral fracture incidence and mortality. J Bone Joint Surg Am 96(4):e29. doi:10.2106/JBJS.L.00223
Dell R (2011) Fracture prevention in Kaiser Permanente Southern California. Osteoporos Int 22(Suppl 3):457–460. doi:10.1007/s00198-011-1712-0
Yong JH, Masucci L, Hoch JS, Sujic R, Beaton D (2015) Cost-effectiveness of a fracture liaison service-a real-world evaluation after 6 years of service provision. Osteoporos Int 27(1):231–240. doi:10.1007/s00198-015-3280-1
IOF Fracture Working Group; EXCO, Javaid MK, Kyer C, Mitchell PJ, Chana J, Moss C, Edwards MH, McLellan AR, Stenmark J, Pierroz DD, Schneider MC, Kanis JA, Akesson K, Cooper C (2015) Effective secondary fracture prevention: implementation of a global benchmarking of clinical quality using the IOF Capture the Fracture® Best Practice Framework tool. Osteoporos Int 26(11):2573–2578. doi:10.1007/s00198-015-3192-0
Royal College of Physicians. Falls and Fragility Audit Programme, National Hip Fracture Database (NHFD) annual report 2015. Healthcare Quality Improvement Partnership 2015 http://www.nhfd.co.uk/20/hipfractureR.nsf/vwcontent/2014reportPDFs/$file/NHFD2014SummaryReport.pdf?OpenElement. Accessed 21 September 2015
FRAX®. WHO Fracture Risk Assessment Tool. https://www.shef.ac.uk/FRAX/. Accessed 30 September 2015
Stapleton C, Hough P, Bull K, Hill K, Greenwood K, Oldmeadow L (2009) A 4-item falls-risk screening tool for sub-acute and residential care: the first step in falls prevention. Australas J Ageing 28(3):139–143. doi:10.1111/j.1741-6612.2009.00375.x
National Institute for Health and Care Excellence (2011) The management of hip fracture in adults. Clinical guideline (CG124). London: NICE. www.nice.org.uk/guidance/cg124. Accessed 29 September 2015
National Institute for Health and Care Excellence (2013) Falls: assessment and prevention of falls in older people. NICE guidelines [CG161]. London: NICE. https://www.nice.org.uk/Guidance/CG161. Accessed 29 September 2015
National Institute for Health and Care Excellence (2012) Hip fracture quality standard (QS16). NICE, London, www.nice.org.uk/guidance/qs16. Accessed 29 September 2015
National Institute for Health and Clinical Excellence (2008) Alendronate, etidronate, risedronate, raloxifene, strontium ranelate and teriparatide for the secondary prevention of osteoporotic fragility fractures in postmenopausal women (amended): NICE technology appraisal guidance 161 [TA161]. NICE, London, https://www.nice.org.uk/Guidance/TA161. Accessed 29 September 2015
National Osteoporosis Guideline Group (NOGG) http://www.shef.ac.uk/NOGG/index.html. Accessed 30 September 2015
Department of Health (2011) Whole system demonstrator programme; headline findings—December 2011. Gateway Ref: 16972. Available https://www.gov.uk/government/publications/whole-system-demonstrator-programme-headline-findings-december-2011. Accessed 17 November 2015
Cooper C, Mitchell P, Kanis JA (2011) Breaking the fragility fracture cycle. Osteoporos Int 22(7):2049–2050. doi:10.1007/s00198-011-1643-9
Dell R, Greene D, Schelkun SR, Williams K (2008) Osteoporosis disease management: the role of the orthopaedic surgeon. J Bone Joint Surg Am 90:188–194. doi:10.2106/JBJS.H.00628
IOF CSA Fracture Working Group, Marsh D, Åkesson K, Beaton DE, Bogoch ER, Boonen S, Brandi ML, McLellan AR, Mitchell PJ, Sale JE, Wahl DA (2011) Coordinator-based systems for secondary prevention in fragility fracture patients. Osteoporos Int 22(7):2051–2065. doi:10.1007/s00198-011-1642-x
Mitchell PJ (2013) Fracture liaison services in the United Kingdom. Curr Osteoporos Rep 11(4):377–384. doi:10.1007/s11914-013-0166-z
Edwards BJ, Bunta AD, Simonelli C, Bolander M, Fitzpatrick LA (2007) Prior fractures are common in patients with subsequent hip fractures. Clin Orthop Relat Res 461:226–230
Skelton D, Neil F (2009) NHS Greater Glasgow and Clyde Strategy for Osteoporosis and Falls Prevention 2006-2010: An evaluation 2007-2009. http://library.nhsggc.org.uk/mediaAssets/OFPS/NHSGGC%20Strategy%20for%20Osteoporosis%20and%20Falls%20Prevention%202006-2010_An%20Evaluation_Skelton%20and%20Neil%202009.pdf. Accessed 29 September 2015
Department of Health (2009) Fracture prevention services: an economic evaluation. DH, London
Department of Health (2001) National Service Framework for Older People. https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/198033/National_Service_Framework_for_Older_People.pdf. Accessed 29 September 2015
National Institute for Health and Clinical Excellence (2010) Denosumab for the prevention of osteoporotic fractures in postmenopausal women. NICE technology appraisal guidance 204. London: NICE. http://www.nice.org.uk/guidance/ta204/resources/guidance-denosumab-for-the-prevention-of-osteoporotic-fractures-in-postmenopausal-women-pdf. Accessed 29 September 2015
Scottish Intercollegiate Guidelines Network (SIGN) (2015) Management of osteoporosis and the prevention of fragility fractures. (SIGN publication no. 142). Edinburgh: SIGN; 2015. http://www.sign.ac.uk. Accessed 29 September 2015
Acknowledgments
The authors would like to thank the members of the FLS for their hard work, excellent data keeping and assistance with any enquiries regarding the audit. The authors would also like to thank Chris Boivin and the DXA department for all their hard work in both providing the service and data for the audit.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards in regards to audit and data protection were adhered to.
Conflicts of interest
NG chaired the NOS Service Standards document and is a Trustee of the NOS and Chair of the Clinical and Scientific Committee of the NOS.
Rights and permissions
About this article
Cite this article
Shipman, K.E., Stammers, J., Doyle, A. et al. Delivering a quality-assured fracture liaison service in a UK teaching hospital—is it achievable?. Osteoporos Int 27, 3049–3056 (2016). https://doi.org/10.1007/s00198-016-3639-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3639-y