Abstract
Introduction and hypothesis
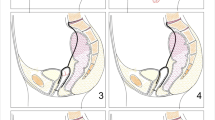
We evaluated the anatomical and functional outcomes following modified laparoscopic sacrocolpopexy (LSC) utilizing deep dissection of the vaginal walls and distal mesh fixation at the anterior and posterior compartments. We hypothesized that anatomical and functional outcomes improve after this modified LSC technique.
Methods
This was a retrospective study of all women (n = 240) who underwent LSC for pelvic organ prolapse (POP) from January to December 2017 in a tertiary center. POP-Q staging, validated questionnaires (International Consultation on Incontinence Questionnaire-Short Form [ICIQ-SF] and Pelvic Floor Distress Inventory Questionnaire-Short Form), and uroflowmetry were used to evaluate the anatomical and functional outcomes. Statistical analyses were performed using McNemar test and repeated measures analysis of variance with Fisher’s least significant difference post hoc (p < 0.05).
Results
The anatomical success rate is 96%, with a prolapse recurrence rate of 3.8% at 3-year follow-up. Bulge symptoms and anatomical compartments were significantly improved after LSC. Clinically, there were significant improvements after LSC in voiding dysfunction and bowel symptoms. Also, there was a significant increase in stress urinary incontinence and non-significant decrease in mixed urinary incontinence and urge urinary incontinence. ICIQ-SF and Colorectal-Anal Distress Inventory 8 scores were significantly lower after LSC, signifying improvement in incontinence and bowel symptoms.
Conclusion
Our modified LSC technique is safe and effective in restoring level 1 and level 2 supports, without adverse effects on urinary and bowel function. Bladder and bowel symptoms have also been found to keep improving over time.



Similar content being viewed by others
Abbreviations
- CRADI-8:
-
Colorectal-Anal Distress Inventory 8
- ICIQ-SF:
-
International Consultation on Incontinence Questionnaire-Short Form
- LSC:
-
Laparoscopic sacrocolpopexy
- MUI:
-
Mixed urinary incontinence
- PFDI-20:
-
Pelvic Floor Distress Inventory Questionnaire-Short Form
- POP:
-
Pelvic organ prolapse
- SUI:
-
Stress urinary incontinence
- UUI:
-
Urge urinary incontinence
- VD:
-
Voiding dysfunction
- VVP:
-
Vaginal vault prolapse
References
Ganatra AM, Rozet F, Sanchez-Salas R, Barret E, Galiano M, Cathelineau X, Vallancien G. The current status of laparoscopic sacrocolpopexy: a review. Eur Urol. 2009;55(5):1089-103. https://doi.org/10.1016/j.eururo.2009.01.048.
Matthews CA. Minimally invasive sacrocolpopexy: How to avoid short- and long-term complications. Current Urology Reports. 2016;17(11):81. https://doi.org/10.1007/s11934-016-0638-7.
Gluck O, Blaganje M, Veit-Rubin N, Phillips C, Deprest J, O'reilly B, But I, Moore R, Jeffery S, Haddad JM, Deval B. Laparoscopic sacrocolpopexy: A comprehensive literature review on current practice. Eur J Obstet Gynecol Reprod Biol. 2020;245:94–101. https://doi.org/10.1016/j.ejogrb.2019.12.029.
Myers EM, Siff L, Osmundsen B, Geller E, Matthews CA. Differences in recurrent prolapse at 1 year after total vs supracervical hysterectomy and robotic sacrocolpopexy. Int Urogynecol J. 2015;26(4):585–9. https://doi.org/10.1007/s00192-014-2551-2.
Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J. Surgery for women with apical vaginal prolapse. Cochrane Database Syst Rev 2016;(10):Art. No.: CD012376. https://doi.org/10.1002/14651858.CD012376.
Marzi L, Vincenzo, Serati M. Management of Pelvic Organ Prolapse. Current Controversies. 2018. https://doi.org/10.1007/978-3-319-59195-7.
Maher C, Feiner B, Baessler K, Schmid C. Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 2013(4):Art. No.: CD004014. https://doi.org/10.1002/14651858.CD004014.pub5. Accessed 01 May 2021.
Weber AM, Abrams P, Brubaker L, Cundiff G, Davis G, Dmochowski RR, Fischer J, Hull T, Nygaard I, Weidner AC. The standardization of terminology for researchers in female pelvic floor disorders. Int Urogynecol J Pelvic Floor Dysfunct. 2001;12(3):178-86. https://doi.org/10.1007/pl00004033.
Gustilo-Ashby AM, Paraiso MF, Jelovsek JE, Walters MD, Barber MD. Bowel symptoms 1 year after surgery for prolapse: further analysis of a randomized trial of rectocele repair. Am J Obstet Gynecol. 2007;197(1):76.e1–5. https://doi.org/10.1016/j.ajog.2007.02.045.
Sung VW, Rardin CR, Raker CA, LaSala CA, Myers DL. Changes in bowel symptoms 1 year after rectocele repair. Am J Obstet Gynecol. 2012;207(5):423.e1–423.e4235. https://doi.org/10.1016/j.ajog.2012.06.054.
Bradley CS, Nygaard IE, Brown MB, Gutman RE, Kenton KS, Whitehead WE, Goode PS, Wren PA, Ghetti C, Weber AM. Pelvic Floor Disorders Network. Bowel symptoms in women 1 year after sacrocolpopexy. Am J Obstet Gynecol. 2007;197(6):642.e1–8. https://doi.org/10.1016/j.ajog.2007.08.023.
Antosh DD, Kim-Fine S, Meriwether KV, Kanter G, Dieter AA, Mamik MM, Good M, Singh R, Alas A, Foda MA, Balk EM, Rahn DD, Rogers RG. Changes in Sexual Activity and Function After Pelvic Organ Prolapse Surgery: A Systematic Review. Obstet Gynecol. 2020;136(5):922–31. https://doi.org/10.1097/AOG.0000000000004125.
Moroni RM, CRTT Juliato, Cosson M, Giraudet G, LGOO Brito. Does sacrocolpopexy present heterogeneity in its surgical technique? A systematic review. Neurourol Urodyn 2018;37(July (8))2335–45 https://doi.org/10.1002/nau.23764
Costantini E, Brubaker L, Cervigni M, Matthews CA, O'Reilly BA, Rizk D, Giannitsas K, Maher CF. Sacrocolpopexy for pelvic organ prolapse: evidence-based review and recommendations. Eur J Obstet Gynecol Reprod Biol. 2016;205:60-5. https://doi.org/10.1016/j.ejogrb.2016.07.503.
O'Sullivan OE, Matthews CA, O'Reilly BA. Sacrocolpopexy: is there a consistent surgical technique? Int Urogynecol J. 2016;27(5):747-50. https://doi.org/10.1007/s00192-015-2880-9.
Christmann-Schmid C, Koerting I, Ruess E, Faehnle I, Krebs J. Functional outcome after laparoscopic nervesparing sacrocolpopexy: a prospective cohort study. Acta Obstet Gynecol Scand 2018;97:744–750. https://doi.org/10.1111/aogs.13337
Sarlos D, Aigmueller T, Magg H, Schaer G. Laparoscopic sacrocolpopexy. American Journal of Obstetrics and Gynecology. 2015;212(6):824.e1–3. https://doi.org/10.1016/j.ajog.2014.12.005.
Shiozawa T, Huebner M, Hirt B, Wallwiener D, Reisenauer C. Nerve-preserving sacrocolpopexy: anatomical study and surgical approach. Eur J Obstet Gynecol Reprod Biol. 2010;152(1):103–7. https://doi.org/10.1016/j.ejogrb.2010.05.009.
Wattiez A, Goldchmit R, Chew S, Mage G, Pouly JL, Bruhat MA. Laparoscopic treatment of uterine and vault prolapse. In: Ultrasound and Endoscopic Surgery in Obstetrics and Gynaecology. 2003. Springer, London. https://doi.org/10.1007/978-1-4471-0655-5_15
Abdullah B, Nomura J, Moriyama S, Huang T, Tokiwa S, Togo M. Clinical and urodynamic assessment in patients with pelvic organ prolapse before and after laparoscopic sacrocolpopexy. Int Urogynecol J. 2017;28(10):1543-1549. https://doi.org/10.1007/s00192-017-3306-7.
LeClaire EL, Mukati MS, Juarez D, White D, Quiroz LH. Is de novo stress incontinence after sacrocolpopexy related to anatomical changes and surgical approach? Int Urogynecol J. 2014;25(9):1201–6. https://doi.org/10.1007/s00192-014-2366-1.
El Hamamsy D, Fayyad AM. New onset stress urinary incontinence following laparoscopic sacrocolpopexy and its relation to anatomical outcomes. Int Urogynecol J. 2015;26:1041–5. https://doi.org/10.1007/s00192-015-2641-9.
Cameron AP, Smith AR, Lai HH, Bradley CS, Liu AB, Merion RM, Gillespie BW, Amundsen CL, Cella D, Griffith JW, Wiseman JB, Kreder KJ, Kenton KS, Helmuth ME, Fraser MO, Clemens JQ, Kirkali Z, Kusek JW, Siddiqui NY; LURN Study Group. Bowel function, sexual function, and symptoms of pelvic organ prolapse in women with and without urinary incontinence. Neurourol Urodyn. 2018;37(8):2586-2596. https://doi.org/10.1002/nau.23587.
Christmann-Schmid C, Koerting I, Ruess E, Faehnle I, Krebs J. Functional outcome after laparoscopic nerve-sparing sacrocolpopexy: a prospective cohort study. Acta Obstet Gynecol Scand. 2018;97:744–50.
Song XC, Zhu L, Liang S, Xu T. Changes in voiding function after laparoscopic sacrocolpopexy for advanced pelvic organ prolapse: a cohort study of 76 cases. Int Urogynecol J. 2018;29(4):505-512. https://doi.org/10.1007/s00192-017-3412-6.
Illiano E, Natale F, Giannantoni A, et al. Urodynamic findings and functional outcomes after laparoscopic sacrocolpopexy for symptomatic pelvic organ prolapse. Int Urogynecol J. 2019;30:589–94. https://doi.org/10.1007/s00192-019-03874-4.
Cosma S, Petruzzelli P, Danese S, Benedetto C. Nerve preserving vs standard laparoscopic sacropexy: Postoperative bowel function. World J Gastrointest Endosc. 2017;9(5):211-219. https://doi.org/10.4253/wjge.v9.i5.211.
Author information
Authors and Affiliations
Contributions
Cortes ARB: Project development, Data collection/analysis, Manuscript writing
Hayashi T: Data analysis, Manuscript writing
Nomura M: Project development, Data collection
Sawada Y, Tokiwa S, Nagae M: Data collection
Corresponding author
Ethics declarations
Financial disclaimer/conflict of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cortes, A.R.B., Hayashi, T., Nomura, M. et al. Medium term anatomical and functional outcomes following modified laparoscopic sacrocolpopexy. Int Urogynecol J 33, 3111–3121 (2022). https://doi.org/10.1007/s00192-022-05076-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05076-x