Abstract
Introduction and hypothesis
There has been renewed interest in the management of postoperative pain after benign gynecological surgery. The purpose of the study was to determine if the use of intraoperative and immediate postoperative pain medication differs between vaginal and laparoscopic surgery in women with pelvic organ prolapse.
Methods
The study included women who had undergone pelvic organ prolapse repair between 2014 and 2019 in two tertiary care hospitals. We collected demographic data and pain medication used during and after surgery, including opioids, local anesthetics, gabapentin, ketorolac, ibuprofen, and acetaminophen. Data analyses were performed using STATA Version 16.1. A p value <0.05 was considered to indicate statistical significance.
Results
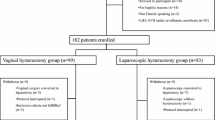
A total of 195 women were included in the study, with 98 in the vaginal and 97 in the laparoscopic group. Intraoperative opioid use in the two groups was similar (25 morphine milligram equivalent [MME], p = 0.34). However, women in the laparoscopic group received significantly more intravenous and local anesthesia (lidocaine: 60 vs 40 mg; bupivacaine 49.6 vs 20 ml, p < 0.001). Postoperatively, although women in the vaginal group required almost twice as many narcotics as those in the laparoscopy group (MME = 28 vs 15, p < 0.001), after controlling for confounders in the multivariate analysis, there were no differences in postoperative pain requirements between the two groups. Recovery time had a significant impact on opioid and acetaminophen use (p < 0.05).
Conclusion
Use of pain medication was similar in the intraoperative and immediate postoperative period after pelvic organ prolapse surgery when comparing the vaginal and laparoscopic approaches after controlling for potential confounding factors.
Similar content being viewed by others
References
Steinberg AC, Schimpf MO, White AB, Matthews C, Ellington DR, Jeppson P, et al. Preemptive analgesia for postoperative pain control: systematic review and clinical practice guidelines. Am J Obstet Gynecol. 2017;217:303–13.e6.
As-Sanie S, Till SR, Mowers EL, Lim CS, Skinner BD, Fritsch L, et al. Opioid patterns, patient use, and postoperative pain after hysterectomy for benign indications. Obstet Gynecol. 2017;130:1261–8.
Young JC, Wu JM, Willis-Gray M, Pate V, Jonsson FM. Persistent opioid use after hysterectomy in the United States, 2005–2015. Obstet Gynecol. 2020;135:123–32.
Urman RD, Boing EA, Pham AT, Khangulov V, Fain R, Nathanson BH, et al. Improved outcomes with the use of intravenous acetaminophen for management of acute post-surgical pain in cesarean sections and hysterectomies. J Clin Med Res. 2018;10:499–507.
Margolis B, Andriani L, Baumann K, Hirsch AM, Pothuri B. Safety and feasibility of discharge without an opioid prescription for patients undergoing gynecologic surgery. Obstet Gynecol. 2020;136:1126–34.
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997;89:501–6.
Nascimento MC, Kelley A, Martitsch C, Weidner I, Obermair A. Postoperative analgesic requirements—total laparoscopic hysterectomy versus vaginal hysterectomy. Aust N Z J Obstet Gynaecol. 2005;45:140–3.
Pokkinen SM, Kalliomaki ML, Yli-Hankala A, Nieminen K. Less postoperative pain after laparoscopic hysterectomy than after vaginal hysterectomy. Arch Obstet Gynecol. 2015;292(1):149–54.
Leach DA, Scarlotta LS, Habermann EB, Glasgow AE, Occhino JA. Characteristics of opioid users undergoing surgery for pelvic organ prolapse. Int Urogynecol J. 2020;31:1891–7.
Nguyen JN, Yang ST. Perioperative outcomes after robotic versus vaginal surgery for pelvic organ surgery. J Robot Surg. 2020;14:415–21.
Willis-Gray MG, Young JC, Pate V, Jonsson Funk M, Wu JM. Perioperative opioid prescriptions associated with stress incontinence and pelvic organ prolapse. Am J Obstet Gynecol. 2020;223(6):894.e1–9.
Winkelman WD, Kim Y, Erlinger AL, Haviland MJ, Hacker MR, Elkadry EA. Optimizing perioperative pain control after ambulatory urogynecologic surgery. Female Pelvic Med Reconstr Surg. 2020;26:483–7.
Petrikovets A, Sheyn D, Sun HH, Chapman GC, Mahajan ST, Pollard R, et al. Multimodal opioid-sparing postoperative pain regimen compared with the standard postoperative pain regimen in vaginal pelvic reconstructive surgery: a multicenter randomized controlled trial. Am J Obstet Gynecol. 2019;221(5):511.e1–10.
Gillingham A, Kenton K, Geynisman-Tan J, Brown O, Collins SA, Lewicky-Gaupp C, et al. Does a hysterectomy hurt? Comparing narcotic requirements and pain scores in patients undergoing apical prolapse repair with and without hysterectomy. Female Pelvic Med Reconstr Surg. 2021;27:356–9.
Crisp CC, Khan M, Lambers DL, Westermann L, Mazloomdoost D, Yeung J, et al. The effect of intravenous acetaminophen on postoperative pain and narcotic consumption after vaginal reconstructive surgery: a double-blind randomized placebo-controlled trial. Female Pelvic Med Reconstr Surg. 2017;23:80–5.
Trowbridge ER, Kim D, Caldwell L, Franko D, Jackson J, Shilling A, et al. Use of ketorolac after outpatient urogynecologic surgery: a randomized controlled trial. Female Pelvic Med Reconstruct Surg. 2018;24:281–6.
Li ALK, Wadsworth K, Siddiqui NT, Alarab M, McDermott C, Lemos N, et al. Does low-dose gabapentin reduce opioid use postoperatively? A randomized controlled trial in women undergoing reconstructive pelvic surgery. Int Urogynecol J. 2019;30:211–7.
Bauchat JR, Milad MP, Kolb S, Hilao J, McCarthy RJ. Effects of preoperatively administered Oral gabapentin and acetaminophen on opioid consumption when added to an analgesic regimen containing dexamethasone for abdominal and vaginal hysterectomies. J Gynecol Surg. 2017;33:243–7.
Jokela R, Ahonen J, Tallgren M, Haanpää M, Korttila K. A randomized controlled trial of perioperative administration of pregabalin for pain after laparoscopic hysterectomy. Pain. 2008;134:106–12.
Ramaseshan AS, O’Sullivan DM, Steinberg AC, Tunitsky-Bitton E. A comprehensive model for pain management in patients undergoing pelvic reconstructive surgery: a prospective clinical practice study. Am J Obstet Gynecol. 2020;223(2):263.e1–8.
Author information
Authors and Affiliations
Contributions
Iwona Gabriel: data collection, manuscript writing; Talar Abdalian: data collection, statistical analysis; Vatche Minassian: study protocol preparation, manuscript writing.
Corresponding author
Ethics declarations
Conflicts of interest
All authors state that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gabriel, I., Abdalian, T. & Minassian, V.A. Perioperative use of pain medications in vaginal versus laparoscopic pelvic organ prolapse surgery. Int Urogynecol J 33, 2455–2461 (2022). https://doi.org/10.1007/s00192-021-05068-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-021-05068-3