Abstract
Introduction and hypothesis
The aim of the study was to evaluate the predictors and reasons for help-seeking behavior among women with urinary incontinence (UI) in Germany and Denmark.
Methods
This international postal survey was conducted in 2014. In each country, 4,000 women of at least 18 years of age were randomly selected. The questionnaires included validated items regarding help-seeking behavior and the ICIQ-UI SF. UI was defined as any involuntary loss of urine. Binary logistic regression analysis was used to assess factors predicting help-seeking behavior. Reasons for seeking or not seeking help were evaluated in terms of the severity of UI and as the most frequently reported.
Results
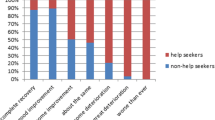
Of 1,063 Danish women with UI, 25.3% had consulted a physician compared with 31.4% of 786 German women with UI (p = 0.004). The severity and duration of UI, and actively seeking information regarding UI, were significant independent predictors of help-seeking behavior. Women with slight/moderate UI did not seek help because they did not consider UI as a problem, whereas of women with severe/very severe UI, German women reported that other illnesses were more important and Danish women reported that they did not have enough resources to consult a physician.
Conclusions
Only a small proportion of women with UI had consulted a physician, and the driving forces for help-seeking behavior were severity and duration of UI and actively seeking information regarding UI. Public information campaigns might enhance consultation rates providing that passively receiving and actively seeking information have the same effects on help-seeking behavior. We show for the first time that reasons for not consulting a physician for UI vary depending on the severity of the UI.
Similar content being viewed by others
References
Haylen B, Ridder DD, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21:5–26. doi:10.1007/s00192-009-0976-9.
Hunskaar S, Arnold EP, Burgio K, et al. Epidemiology and natural history of urinary incontinence. Int Urogynecol J. 2000;11:301–19. doi:10.1007/s001920070021.
Buckley BS, Lapitan MC; Epidemiology Committee of the Fourth International Consultation on Incontinence, Paris, 2008. Prevalence of urinary incontinence in men, women, and children – current evidence: findings of the Fourth International Consultation on Incontinence. Urology. 2010;76:265–70. doi:10.1016/j.urology.2009.11.078.
Schreiber Pedersen L, Lose G, Høybye MT, et al. Prevalence of urinary incontinence among women and analysis of potential risk factors in Germany and Denmark. Acta Obstet Gynecol Scand. 2017;96:939–48. doi:10.1111/aogs.13149.
O’Donnell M, Lose G, Sykes D, et al. Help-seeking behaviour and associated factors among women with urinary incontinence in France, Germany, Spain and the United Kingdom. Eur Urol. 2005;47:385–92. doi:10.1016/j.eururo.2004.09.014.
Hannestad Y, Rortveit G, Hunskaar S. Help-seeking and associated factors in female urinary incontinence. The Norwegian EPINCONT Study. Epidemiology of Incontinence in the County of Nord-Trøndelag. Scand J Prim Health Care. 2002;20:102–7. doi:10.1080/713796408.
Hägglund D, Walker-Engström ML, Larsson G, Leppert J. Reasons why women with long-term urinary incontinence do not seek professional help: a cross-sectional population-based cohort study. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14:296–304. doi:10.1007/s00192-003-1077-9.
Kinchen KS, Burgio K, Diokno AC, et al. Factors associated with women’s decisions to seek treatment for urinary incontinence. J Womens Health. 2003;12:687–98.
Yu H-J, Wong W, Chen J, Chie W-C. Quality of life impact and treatment seeking of Chinese women with urinary incontinence. Qual Life Res. 2003;12:327–33. doi:10.1023/a:1023250632395.
Abrams P, Cardozo L, Khoury S, Wein A. Incontinence, 5th International Consultation on Incontinence, Paris, February 2012. 5th ed. Paris: ICUD-EAU; 2013.
Papanicolaou S, Hunskaar S, Lose G, Sykes D. Assessment of bothersomeness and impact on quality of life of urinary incontinence in women in France, Germany, Spain and the UK. BJU Int. 2005;96:831–8. doi:10.1111/j.1464-410X.2005.05722.x.
Monz B, Chartier-Kastler E, Hampel C, et al. Patient characteristics associated with quality of life in European women seeking treatment for urinary incontinence: results from PURE. Eur Urol. 2007;51:1073–82. doi:10.1016/j.eururo.2006.09.022.
Ebbesen MH, Hunskaar S, Rortveit G, Hannestad YS. Prevalence, incidence and remission of urinary incontinence in women: longitudinal data from the Norwegian HUNT study (EPINCONT). BMC Urol. 2013;13:27. doi:10.1186/1471-2490-13-27.
Miller YD, Brown WJ, Smith N, Chiarelli P. Managing urinary incontinence across the lifespan. Int J Behav Med. 2003;10:143–61.
Berger MB, Patel DA, Miller JM, et al. Racial differences in self-reported healthcare seeking and treatment for urinary incontinence in community-dwelling women from the EPI study. Neurourol Urodyn. 2011;30:1442–7.
OECD/Eurostat/UNESCO Institute for Statistics. ISCED 2011 Operational Manual: Guidelines for classifying national education programmes and related qualifications. Paris: OECD Publishing; 2015.doi:10.1787/9789264228368-en
Creswell JW, Clark VLP. Designing and conducting mixed methods research. 2nd ed. Los Angeles: Sage; 2011.
Jürgensen M, Elsner S, Schreiber Pedersen L, et al. "I really thought nothing could be done": help-seeking behaviour among women with urinary incontinence. Int J Res Med Sci. 2015;3:826–35. doi:10.5455/2320-6012.ijrms20150402.
Harkness JA, van de Vijver FJ, Mohler PP. Cross-cultural survey methods. New York: Wiley; 2003.
de Vet HC, Terwee CB, Mokkink LB, Knol DL. Measurement in medicine, 1st ed. New York: Cambridge University Press; 2011.
Willis GB. Cognitive interview: a tool for improving questionnaire design. Thousand Oaks: Sage; 2005.
Avery KN, Bosch JL, Gotoh M, et al. Questionnaires to assess urinary and anal incontinence: review and recommendations. J Urol. 2007;177:39–49. doi:10.1016/j.juro.2006.08.075.
Avery K, Donovan J, Peters TJ, et al. ICIQ: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn. 2004;23:322–30. doi:10.1002/nau.20041.
Espuña-Pons M, Dilla T, Castro D, et al. Analysis of the value of the ICIQ-UI SF questionnaire and stress test in the differential diagnosis of the type of urinary incontinence. Neurourol Urodyn. 2007;26:836–41.
Klovning A, Avery K, Sandvik H, Hunskaar S. Comparison of two questionnaires for assessing the severity of urinary incontinence: the ICIQ-UI SF versus the incontinence severity index. Neurourol Urodyn. 2009;28:411–5.
Hansen BB, Svare J, Viktrup L, et al. Urinary incontinence during pregnancy and 1 year after delivery in primiparous women compared with a control group of nulliparous women. Neurourol Urodyn. 2012;31:475–80. doi:10.1002/nau.21221.
World Medical Association. Declaration of Helsinki. Ethical principles for medical research involving human subjects. Jahr Wiss Ethik. 2014;18(1):363–8. doi:10.1515/jwiet-2014-0117.
Xu D, Wang X, Li J, Wang K. The mediating effect of “bothersome” urinary incontinence on help-seeking intentions among community-dwelling women. J Adv Nurs. 2015;71:315–25. doi:10.1111/jan.12514.
Doshi AM, Van Den Eeden SK, Morrill MY, et al. Women with diabetes: understanding urinary incontinence and help seeking behavior. J Urol. 2010;184:1402–7. doi:10.1016/j.juro.2010.06.014.
Milsom I, Kaplan SA, Coyne KS, et al. Effect of bothersome overactive bladder symptoms on health-related quality of life, anxiety, depression, and treatment seeking in the United States: results from EpiLUTS. Urology. 2012;80:90–6. doi:10.1016/j.urology.2012.04.004.
Coyne KS, Sexton CC, Kopp Z, et al. Assessing patients’ descriptions of lower urinary tract symptoms (LUTS) and perspectives on treatment outcomes: results of qualitative research. Int J Clin Pract. 2010;64:1260–78. doi:10.1111/j.1742-1241.2010.02450.x.
Acknowledgements
We thank Susanne Elsner and Jessica Lueckert, Institute for Social Medicine and Epidemiology, University of Luebeck, for assistance during the conduct of the survey, Tobias Windfeldt Klausen, Department of Hematology, Herlev Gentofte University Hospital, for statistical advice, and Philip Greenwood for language advice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was funded by tthe European Commission’s INTERREG IVA program.
Conflicts of interest
Louise Schreiber Pedersen: none.
Gunnar Lose has accepted payment for research from Astellas and has been a consultant for Contura. Neither this funding source nor this relationship influenced the performance of this study.
Mette Terp Høybye: none.
Martina Jürgensen: none.
Annika Waldmann: none.
Martin Rudnicki: none.
Rights and permissions
About this article
Cite this article
Schreiber Pedersen, L., Lose, G., Høybye, M.T. et al. Predictors and reasons for help-seeking behavior among women with urinary incontinence. Int Urogynecol J 29, 521–530 (2018). https://doi.org/10.1007/s00192-017-3434-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3434-0