Abstract
Introduction and hypothesis
Jorge and Wexner devised a questionnaire for anal incontinence (AI), known as the Wexner scale (WS). Specific validated questionnaires are essential for the assessment of symptom severity. The objective was to accomplish the cultural adaptation and validation of the Portuguese version of the WS.
Methods
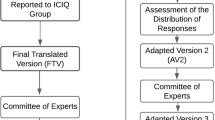
The WS was validated according to the international criteria. A Brazilian version was tested, including the item “I do not understand” at the end of each question. If this answer was reported at a rate higher than 15 %, the item would be considered difficult to understand and would thus be modified. The final version of the WS and the Fecal Incontinence Quality of Life (FIQL) were completed by 50 women. Convergent validity was assessed by comparing the data from the first interview of the WS with the FIQL using Spearman’s test. Reproducibility was assessed by means of a 2-week test–retest procedure using Cronbach’s alpha coefficient.
Results
In the initial version of the questionnaire, we did not obtain a response of “I do not understand” at a rate greater than 15 % and this version was considered definitive. A significant negative relationship (r = −0.63) was found between the FIQL total score and the WS. The answers obtained on the “test–re-est” questionnaires showed a significant correlation according to the intraclass correlation coefficient (ICC). A high level of internal consistency was found, as demonstrated by a Cronbach’s alpha of 0.932.
Conclusion
The Brazilian Portuguese version of the WS is a reliable, consistent, and valid instrument.

Similar content being viewed by others
References
Haylen BT, de Ridder D, Freeman RM et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn 29(1):4–20
Andromanakos NP, Filippou DK, Pinis SI, Kostakis AI (2013) Anorectal incontinence: a challenge in diagnostic and therapeutic approach. Eur J Gastroenterol Hepatol 25(11):1247–1256
Bellicini N, Molloy PJ, Caushaj P, Kozlowski P (2008) Fecal incontinence: a review. Dig Dis Sci 53(1):41–46
Nevler A (2014) The epidemiology of anal incontinence and symptom severity scoring. Gastroenterol Rep (Oxf) 2(2):79–84
Norton C, Whitehead WE, Bliss DZ, Harari D, Lang J; Conservative Management of Fecal Incontinence in Adults Committee of the International Consultation on Incontinence (2010) Management of fecal incontinence in adults. Neurourol Urodyn 29(1):199–206
Whitehead WE, Borrud L, Goode PS et al (2009) Fecal incontinence in US adults: epidemiology and risk factors. Gastroenterology 137(2):512–517
Melville JL, Fan MY, Newton K, Fenner D (2005) Fecal incontinence in US women: a population-based study. Am J Obstet Gynecol 193(6):2071–2076
Gordon D, Groutz A, Goldman G et al (1999) Anal incontinence: prevalence among female patients attending a urogynecologic clinic. Neurourol Urodyn 18(3):199–204
Cam C, Selcuk S, Asoglu MR et al (2011) Validation of the Wexner scale in women with fecal incontinence in a Turkish population. Int Urogynecol J 22(11):1375–1379
Jorge JM, Wexner SD (1993) Etiology and management of fecal incontinence. Dis Colon Rectum 36(1):77–97
Rusavy Z, Jansova M, Kalis V (2014) Anal incontinence severity assessment tools used worldwide. Int J Gynaecol Obstet 126(2):146–150
Yusuf SA, Jorge JM, Habr-Gama A, Kiss DR, Gama Rodrigues J (2004) Evaluation of quality of life in anal incontinence: validation of the questionnaire FIQL (fecal incontinence quality of life). Arq Gastroenterol 41(3):202–208
Guillemin F, Bombardier C, Beaton D (1993) Cross-cultural adaptation of health-related quality of life measures: literature review and proposed guidelines. J Clin Epidemiol 46(12):1417–1432
Ferraz MB, Oliveira LM, Araujo PM, Atra E, Tugwell P (1990) Crosscultural reliability of the physical ability dimension of the health assessment questionnaire. J Rheumatol 17(6):813–817
Barber MD (2007) Questionnaires for women with pelvic floor disorders. Int Urogynecol J Pelvic Floor Dysfunct 18(4):461–465
Patrick DL, Martin ML, Bushnell DM, Marquis P, Andrejasich CM, Buesching DP (1999) Cultural adaptation of a quality-of-life measure for urinary incontinence. Eur Urol 36(5):427–435
Cronbach LJ (1951) Coefficient alpha and the internal structure of tests. Psychometrika 16:297–334
Deyo RA, Diehr P, Patrick DL (1991) Reproducibility and responsiveness of health status measures. Statistics and strategies for evaluation. Control Clin Trials 12 [4 Suppl]:142S–158S
Tamanini JT, Almeida FG, Girotti ME, Riccetto CL, Palma PC, Rios LA (2008) The Portuguese validation of the International Consultation on Incontinence Questionnaire-Vaginal Symptoms (ICIQ-VS) for Brazilian women with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 19(10):1385–1391
Barber MD, Walters MD, Bump RC (2005) Short forms of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol 193(1):103–113
Geller EJ, Barbee ER, Wu JM, Loomis MJ, Visco AG (2007) Validation of telephone administration of 2 condition-specific quality-of-life questionnaires. Am J Obstet Gynecol 197(6):632.e1–632.e4
Meschia M, Buonaguidi A, Pifarotti P, Somigliana E, Spennacchio M, Amicarelli F (2002) Prevalence of anal incontinence in women with symptoms of urinary incontinence and genital prolapse. Obstet Gynecol 100(4):719–723
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Funding
Minas Gerais Foundation of Support Research (FAPEMIG).
Rights and permissions
About this article
Cite this article
Fonseca, A.M., Meinberg, M.F., Lucas, D.V. et al. Cultural adaptation and validation of the Wexner scale in patients with anal incontinence in a Brazilian population. Int Urogynecol J 27, 959–963 (2016). https://doi.org/10.1007/s00192-015-2927-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2927-y