Abstract
Introduction and hypothesis
Our aim was to estimate agreement between transperineal and endovaginal ultrasound in assessing levator ani biometry and avulsion in nullipara and primipara women and determine agreement between levator avulsion palpation and ultrasound.
Methods
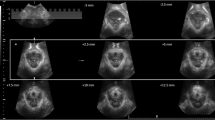
This longitudinal cohort study assessed 269 nullipara women at 36 weeks gestation and 191 primipara women 13 weeks postpartum. Women underwent levator palpation, and avulsion was diagnosed if no attachment to the pubic bone was felt. Subsequently, 3/4D transperineal and 3D endovaginal ultrasound were performed. A standardized protocol was used to perform measurements at rest. Levator avulsion was diagnosed on endovaginal ultrasound at rest if >50 % was avulsed and on transperineal tomographic ultrasound imaging at maximum contraction if the central three slices were avulsed. Levator avulsion was analyzed by two independent, blinded investigators. A third investigator resolved discrepancies. Intraclass correlation coefficient and limits of agreement were calculated for each time point.
Results
Intraclass correlation coefficient for levator urethra gap was 0.44–0.54, hiatus area 0.76–0.79, transverse diameter 0.51–0.59, anteroposterior diameter 0.70–0.72. Levator thickness correlated poorly. Endovaginal ultrasound measurements were generally smaller; however limits of agreement were acceptable for hiatus measurements. Overall agreement between both ultrasound techniques in diagnosing levator avulsion was 95 %; correlation 0.72 [95 % confidence interval (CI) 0.67–0.76]. Agreement between palpation and transperineal ultrasound was 92 % (kappa = 0.34), and between palpation and endovaginal ultrasound was 92 % (kappa = 0.37).
Conclusions
Transperineal and endovaginal ultrasound can both be used to analyze hiatus area and anteroposterior diameter with the patient at rest and to diagnose levator avulsion. Palpation correlates only fairly with both methods.



Similar content being viewed by others
References
DeLancey JO, Morgan DM, Fenner DE et al (2007) Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol 109:295–302
Dietz HP, Simpson JM (2008) Levator trauma is associated with pelvic organ prolapse. BJOG 115:979–984
Dietz HP, Shek C, De Leon J, Steensma AB (2008) Ballooning of the levator hiatus. Ultrasound Obstet Gynecol 31:676–680
Dietz HP, Franco AVM, Shek KL, Kirby A (2012) Avulsion injury and levator hiatal ballooning: two independent risk factors for prolapse? An observational study. Acta Obstet Gynecol Scand 91:211–214
Kearney R, Miller JM, DeLancey JO (2006) Interrater reliability and physical examination of the pubovisceral portion of the levator ani muscle, validity comparisons using MR imaging. Neurourol Urodyn 25:50–54
Dietz HP, Bernardo MJ, Kirby A, Shek KL (2011) Minimal criteria for the diagnosis of avulsion of the puborectalis muscle by tomographic ultrasound. Int Urogynecol J 22:699–704
Shobeiri SA, Rostaminia G, White D, Quiroz LH (2013) The determinants of minimal levator hiatus and their relationship to the puborectalis muscle and the levator plate. BJOG 120:205–211
Schwertner-Tiepelmann N, Thakar R, Sultan AH, Tunn R (2012) Obstetric levator ani muscle injuries: current status. Ultrasound Obstet Gynecol 39:372–383
Kruger JA, Heap SW, Murphy BA, Dietz HP (2008) Pelvic floor function in nulliparous women using three-dimensional ultrasound and magnetic resonance imaging. Obstet Gynecol 111:631–638
Majida M, Braekken IH, Bø K, Benth JS, Engh ME (2010) Validation of three-dimensional perineal ultrasound and magnetic resonance imaging measurements of the pubovisceral muscle at rest. Ultrasound Obstet Gynecol 35:715–722
Zhuang RR, Song YF, Chen ZQ et al (2011) Levator avulsion using a tomographic ultrasound and magnetic resonance-based model. Am J Obstet Gynecol 205:232.e1-8
Shobeiri SA, LeClaire E, Nihira MA, Quiroz LH, O’Donoghue D (2009) Appearance of the levator ani muscle subdivisions in endovaginal three-dimensional ultrasonography. Obstet Gynecol 114:66–72
Santoro GA, Wieczorek AP, Stankiewicz A, Woźniak MM, Bogusiewicz M, Rechberger T (2009) High-resolution three-dimensional endovaginal ultrasonography in the assessment of pelvic floor anatomy: a preliminary study. Int Urogynecol J 20:1213–1222
Santoro GA, Wieczorek AP, Shobeiri SA et al (2011) Interobserver and interdisciplinary reproducibility of 3D endovaginal ultrasound assessment of pelvic floor anatomy. Int Urogynecol J 22:53–59
van Delft K, Shobeiri SA, Thakar R, Schwertner-Tiepelmann N, Sultan AH (2014) Intra- and interrater reliability of levator ani muscle biometry and avulsion using three-dimensional endovaginal sonography. Ultrasound Obstet Gynecol 43:202–209
Dietz HP, Shek C (2008) Validity and reproducibility of the digital detection of levator trauma. Int Urogynecol J Pelvic Floor Dysfunct 19:1097–1101
van Delft K, Schwertner-Tiepelmann N, Thakar R, Sultan AH (2013) Interrater reliability of assessment of levator ani muscle strength and attachment to the pubic bone in nulliparous women. Ultrasound Obstet Gynecol 42:341–346
Dietz HP, Shek C, Clarke B (2005) Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol 25:580–585
Dietz HP, Abbu A, Shek KL (2008) The levator-urethra gap measurement: a more objective means of determining levator avulsion? Ultrasound Obstet Gynecol 32:941–945
Dietz H (2007) Quantification of major morphological abnormalities of the levator ani. Ultrasound Obstet Gynecol 29:329–334
Majida M, Braekken IH, Umek W, Bø K, Saltyte Benth J, Ellstrøm Engh M (2009) Interobserver repeatability of three- and four-dimensional transperineal ultrasound assessment of pelvic floor muscle anatomy and function. Ultrasound Obstet Gynecol 33:567–573
Dietz HP, Steensma AB (2006) The prevalence of major abnormalities of the levator ani in urogynaecological patients. BJOG 113:225–230
Rostaminia G, White D, Hegde A, Quiroz LH, Davila GW, Shobeiri SA (2013) Levator ani deficiency and pelvic organ prolapse severity. Obstet Gynecol 121:1017–1024
van Delft K, Thakar R, Sultan A, Schwertner-Tiepelmann N, Kluivers K (2014) Levator ani muscle avulsion during childbirth: a risk prediction model. BJOG. doi:10.1111/1471-0528.12676
Walter SD, Eliasziw M, Donner A (1998) Sample size and optimal designs for reliability studies. Stat Med 17:101–110
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Bland JM, Altman DG (2003) Applying the right statistics: analyses of measurement studies. Ultrasound Obstet Gynecol 22:85–93
Viera AJ, Garrett JM (2005) Understanding Interobserver Agreement: the Kappa Statistic. Fam Med 37:360–363
Strohbehn K, Ellis JH, Strohbehn JA, DeLancey JO (1996) Magnetic resonance imaging of the levator ani with anatomic correlation. Obstet Gynecol 87:277–285
Dietz HP, Shek KL, Moegni F (2012) Diagnosis of levator avulsion injury: a comparison of three methods. Ultrasound Obstet Gynecol 40:693–698
Weinstein MM, Jung S-A, Pretorius DH, Nager CW, den Boer DJ, Mittal RK (2007) The reliability of puborectalis muscle measurements with 3-dimensional ultrasound imaging. Am J Obstet Gynecol 197:68.e1–68.e6
Conflicts of Interest
RT is IUGA secretary and has accepted honoraria as speaker for Pfizer and Astellas. AS has accepted honoraria as speaker for Pfizer and Astellas. The other authors report no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van Delft, K.W.M., Sultan, A.H., Thakar, R. et al. Agreement between palpation and transperineal and endovaginal ultrasound in the diagnosis of levator ani avulsion. Int Urogynecol J 26, 33–39 (2015). https://doi.org/10.1007/s00192-014-2426-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-014-2426-6