Abstract
Purpose
Lateral patellar instability is a debilitating condition not only to athletes, but also to a wide range of highly active individuals. Many of these patients experience symptoms bilaterally, though it is unknown how these patients fair with return to sports following a second medial patellofemoral ligament reconstruction (MPFLR). The purpose of this study is to evaluate the rate of return to sport following bilateral MPFLR compared to a unilateral comparison group.
Methods
Patients who underwent primary MPFLR with minimum 2-year follow-up were identified from 2014 to 2020 at an academic center. Those who underwent primary MPFLR of bilateral knees were identified. Pre-injury sport participation and Tegner score, Kujala score, Visual Analog Score (VAS) for pain, satisfaction, and MPFL-Return to Sport after Injury (MPFL-RSI) scale were collected. Bilateral and unilateral MPFLRs were matched in a 1:2 ratio based on age, sex, body mass index, and concomitant tibial tubercle osteotomy (TTO). A sub-analysis was performed regarding concomitant TTO.
Results
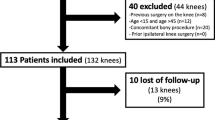
The final cohort consisted of 63 patients, including 21 patients who underwent bilateral MPFLR, matched to 42 unilateral patients at mean follow-up of 47 ± 27 months. Patients who underwent bilateral MPFLR returned to sport at a rate of 62% at a mean of 6.0 ± 2.3 months, compared to a unilateral rate of 72% at 8.1 ± 4.2 months (n.s.). The rate of return to pre-injury level was 43% among bilateral patients and 38% in the unilateral cohort. There were no significant differences in VAS pain, Kujala, current Tegner, satisfaction, and MPFL-RSI scores between cohorts. Approximately half of those (47%) who failed to return to sport cited psychological factors and had significantly lower MPFL-RSI scores (36.6 vs 74.2, p = 0.001).
Conclusion
Patients who underwent bilateral MPFLR returned to sports at a similar rate and level compared to a unilateral comparison group. MPFL-RSI was found to be significantly associated with return to sport.
Level of evidence
III.


Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Ambrožič B, Novak S (2016) The influence of medial patellofemoral ligament reconstruction on clinical results and sports activity level. Phys Sportsmed 44(2):133–140
Ardern CL, Taylor NF, Feller JA, Webster KE (2014) Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med 48(21):1543–1552
Arendt EA, Askenberger M, Agel J, Tompkins MA (2018) Risk of redislocation after primary patellar dislocation: a clinical prediction model based on magnetic resonance imaging variables. Am J Sports Med 46(14):3385–3390
Balcarek P, Oberthür S, Hopfensitz S, Frosch S, Walde TA, Wachowski MM, Schüttrumpf JP, Stürmer KM (2014) Which patellae are likely to redislocate? Knee Surg Sports Traumatol Arthrosc 22(10):2308–2314
Bi AS, Shankar DS, Vasavada KD, Fisher ND, Strauss EJ, Alaia MJ, Campbell KA (2022) Increasing patient-reported allergies are not associated with pain, functional outcomes, or satisfaction following medial patellofemoral ligament reconstruction: a retrospective comparative cohort study. Knee Surg Relat Res 34(1):19. https://doi.org/10.1186/s43019-022-00147-1
Cohen D, Le N, Zakharia A, Blackman B, de Sa D (2022) MPFL reconstruction results in lower redislocation rates and higher functional outcomes than rehabilitation: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 30(11):3784–3795
Erickson BJ, Nguyen J, Gasik K, Gruber S, Brady J, Shubin Stein BE (2019) Isolated medial patellofemoral ligament reconstruction for patellar instability regardless of tibial tubercle-trochlear groove distance and patellar height: outcomes at 1 and 2 years. Am J Sports Med 47(6):1331–1337
Fältström A, Hägglund M, Kvist J (2013) Patient-reported knee function, quality of life, and activity level after bilateral anterior cruciate ligament injuries. Am J Sports Med 41(12):2805–2813
Feller JA, Richmond AK, Wasiak J (2014) Medial patellofemoral ligament reconstruction as an isolated or combined procedure for recurrent patellar instability. Knee Surg Sports Traumatol Arthrosc 22(10):2470–2476
Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, White LM (2004) Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 32(5):1114–1121
Hiemstra LA, Kerslake SA, Lafave MR (2019) Influence of risky pathoanatomy and demographic factors on clinical outcomes after isolated medial patellofemoral ligament reconstruction: a regression analysis. Am J Sports Med 47(12):2904–2909
Hurley ET, Markus DH, Mannino BJ, Gonzalez-Lomas G, Alaia MJ, Campbell KA, Jazrawi LM, Strauss EJ (2021) Patients unable to return to play following medial patellofemoral ligament reconstructions demonstrate poor psychological readiness. Knee Surg Sports Traumatol Arthrosc 29(11):3834–3838
Jaquith BP, Parikh SN (2017) Predictors of recurrent patellar instability in children and adolescents after first-time dislocation. J Pediatr Orthop 37(7):484–490
Johnson DS, Turner PG (2019) Management of the first-time lateral patellar dislocation. Knee 26(6):1161–1165
Kim J-M, Sim J-A, Yang H, Kim Y-M, Wang J-H, Seon J-K (2021) Clinical comparison of medial patellofemoral ligament reconstruction with or without tibial tuberosity transfer for recurrent patellar instability. Am J Sports Med 49(12):3335–3343
Koca F, Fältström A, Cristiani R, Stålman A (2022) Comparison of knee function and activity level between bilateral and unilateral ACL reconstruction: a matched-group analysis with minimum 5-year follow-up. Orthop J Sports Med 10(4):23259671221083576
Krych AJ, O’Malley MP, Johnson NR, Mohan R, Hewett TE, Stuart MJ, Dahm DL (2018) Functional testing and return to sport following stabilization surgery for recurrent lateral patellar instability in competitive athletes. Knee Surg Sports Traumatol Arthrosc 26(3):711–718
Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O (1993) Scoring of patellofemoral disorders. Arthroscopy 9(2):159–163
Kuroda Y, Matsushita T, Matsumoto T, Kawakami Y, Kurosaka M, Kuroda R (2014) Bilateral medial patellofemoral ligament reconstruction in high-level athletes. Knee Surg Sports Traumatol Arthrosc 22(10):2465–2469
Lippacher S, Dreyhaupt J, Williams SRM, Reichel H, Nelitz M (2014) Reconstruction of the medial patellofemoral ligament: clinical outcomes and return to sports. Am J Sports Med 42(7):1661–1668
Manjunath AK, Hurley ET, Jazrawi LM, Strauss EJ (2021) Return to play after medial patellofemoral ligament reconstruction: a systematic review. Am J Sports Med 49(4):1094–1100
Markus DH, Hurley ET, Gipsman A, Campbell KA, Jazrawi LM, Alaia MJ, Strauss EJ (2022) Adding a tibial tubercle osteotomy with anteromedialisation to medial patellofemoral ligament reconstruction does not impact patient-reported outcomes in the treatment of patellar instability. J ISAKOS 7(1):3–6
Meynard P, Malatray M, Sappey-Marinier E, Magnussen RA, Bodiou V, Lustig S, Servien E (2022) Medial patellofemoral ligament reconstruction for recurrent patellar dislocation allows a good rate to return to sport. Knee Surg Sports Traumatol Arthrosc 30(6):1865–1870
Mitchell J, Magnussen RA, Collins CL, Currie DW, Best TM, Comstock RD, Flanigan DC (2015) Epidemiology of patellofemoral instability injuries among high school athletes in the United States. Am J Sports Med 43(7):1676–1682
Parikh SN, Nathan ST, Wall EJ, Eismann EA (2013) Complications of medial patellofemoral ligament reconstruction in young patients. Am J Sports Med 41(5):1030–1038
Platt BN, Bowers LC, Magnuson JA, Marx SM, Liu JN, Farr J, Stone AV (2022) Return to sport after medial patellofemoral ligament reconstruction: a systematic review and meta-analysis. Am J Sports Med 50(1):282–291
Schmiesing A, Engelking M, Agel J, Arendt EA (2022) Distalization of the tibial tubercle for patellar stabilization combined with medial patellofemoral ligament reconstruction: length of distalization or residual patella alta and its affect on outcome. Am J Sports Med 50(6):1627–1634
Schneider DK, Grawe B, Magnussen RA, Ceasar A, Parikh SN, Wall EJ, Colosimo AJ, Kaeding CC, Myer GD (2016) Outcomes after isolated medial patellofemoral ligament reconstruction for the treatment of recurrent lateral patellar dislocations: a systematic review and meta-analysis. Am J Sports Med 44(11):2993–3005
Shubin Stein BE, Gruber S, Brady JM (2018) MPFL in first-time dislocators. Curr Rev Musculoskelet Med 11(2):182–187
Silverman AR, DeFroda SF, Cohen BH, Quinn MS, Tabaddor RR (2022) The brief resilience scale is associated with pre- and short-term postoperative outcomes following hip arthroscopy. Hip Int J Clin Exp Res Hip Pathol Ther 32(5):641–647
Slattery C, Kweon CY (2018) Classifications in brief: outerbridge classification of chondral lesions. Clin Orthop Relat Surg 476(10):2101–2104
Tanaka MJ, Chahla J, Farr J, LaPrade RF, Arendt EA, Sanchis-Alfonso V, Post WR, Fulkerson JP (2019) Recognition of evolving medial patellofemoral anatomy provides insight for reconstruction. Knee Surg Sports Traumatol Arthrosc 27(8):2537–2550
Waterman BR (2019) Editorial commentary: The “F” in MPFL (medial patellofemoral ligament) reconstruction-how should we fix it and does it matter? Arthroscopy 35(4):1138–1140
Webster KE, Feller JA, Kimp AJ, Whitehead TS (2019) Low rates of return to preinjury sport after bilateral anterior cruciate ligament reconstruction. Am J Sports Med 47(2):334–338
Webster KE, Feller JA, Lambros C (2008) Development and preliminary validation of a scale to measure the psychological impact of returning to sport following anterior cruciate ligament reconstruction surgery. Phys Ther Sport 9(1):9–15
Xu C, Dong Z, Ji G, Yan L, Wang X, Li K, Liu J, Zhao J, Wang F (2022) RNA-seq based integrative analysis of potential crucial genes and pathways associated with patellar instability. Bioengineered 13(5):11402–11416
Zhang JK, Barron J, Arvesen J, Israel H, Kim C, Kaar SG (2021) Effect of patient resilience and the single assessment numeric evaluation (SANE) score on return to sport following anterior cruciate ligament reconstruction surgery. Arch Bone Joint Surg 9(5):512–518
Funding
No grant funding was received for this investigation.
Author information
Authors and Affiliations
Contributions
ZIL drafted the original manuscript and assisted with data curation. JT contributed to the writing of the original manuscript and assisted with data collection. AL contributed to formal analysis and conceptualization of the study idea. NR performed the formal analysis and reviewed and edited the manuscript. TJ curated project data and reviewed and edited the manuscript. SRM contributed to writing of the original manuscript. MBL curated project data and reviewed and edited the manuscript. MJA conceptualized the study idea and reviewed and edited the manuscript. EJS designed the methodology and reviewed and edited the manuscript. LMJ revised the manuscript. KAC conceptualized and supervised the study and reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to disclose.
Ethical approval
IRB protocol #19–01430 (New York University School of Medicine).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, Z.I., Triana, J., Lott, A. et al. Patients who undergo bilateral medial patellofemoral ligament reconstruction return to sport at a similar rate as those that undergo unilateral reconstruction. Knee Surg Sports Traumatol Arthrosc 31, 4195–4203 (2023). https://doi.org/10.1007/s00167-023-07462-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07462-4