Abstract
Purpose
To determine the reoperation rate, risk factors for reoperation, and patient-reported outcomes after isolated or combined tibial tubercle transfer and medial patellofemoral ligament reconstruction, for patellofemoral instability surgery.
Methods
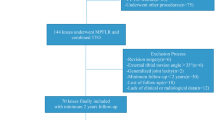
Patient’s records who underwent medial patellofemoral ligament reconstruction and/or tibial tubercle transfer for patellar instability by 35 surgeons from 2002 to 2018 at a single academic institution were retrospectively reviewed using CPT codes. Four-hundred-and-eighty-six patients were identified. Radiographic measurements, demographic parameters, and subsequent revision procedures and their indications were identified. A modified anterior knee pain survey was conducted by mail and with follow-up phone survey.
Results
The overall rate of reoperation was 120/486 (24.7%). The most common cause for reoperation was removal of hardware 42/486 (8.6%). The rate of reoperation for isolated medial patellofemoral ligament reconstruction 43/226 (19%) was lower than that of isolated tibial tubercle transfer 45/133 (33.8%) or a combined procedure 32/127 (25.2%) (P = 0.007). Woman had a higher rate of reoperation (29.4%) compared to men (15.9%) (P = 0.002). Patients at risk for a revision stabilization procedure included those with severe trochlear morphology (C or D) (6.1%) and those with Caton–Deschamps index > 1.3 (7.3%). Patients who underwent reoperation of any kind had poorer patient-reported outcomes.
Conclusion
The overall reoperation rate after patellofemoral instability surgery remains high, and any reoperation portends worse patient-reported outcomes. Re-operations for instability are more likely in patients with trochlear dysplasia and patella alta and may benefit from more aggressive initial treatment, such as medial patellofemoral ligament reconstruction and tibial tubercle transfer in combination. Using the results of this study, surgeons will be able to engage in meaningful discussion with patients to counsel patients on expectations postoperatively.
Level of evidence
IV.

Similar content being viewed by others
References
Agarwalla A, Gowd AK, Liu JN, Puzzitiello RN, Yanke AB, Verma NN, Forsythe B (2019) Concomitant medial patellofemoral ligament reconstruction and tibial tubercle osteotomy do not increase the incidence of 30-day complications: an analysis of the NSQIP database. Orthop J Sports Med 7:2325967119837639
An VV, Sivakumar BS, Phan K, Fritsch BA, Sher D (2019) Isolated versus combined medial patellofemoral ligament reconstruction for lateral instability of the patella. J Orthop Surg 27:2309499018820698
Balcarek P, Rehn S, Howells NR, Eldridge JD, Kita K, Dejour D, Nelitz M, Banke IJ, Lambrecht D, Harden M, Friede T (2017) Results of medial patellofemoral ligament reconstruction compared with trochleoplasty plus individual extensor apparatus balancing in patellar instability caused by severe trochlear dysplasia: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 25:3869–3877
Berruto M, Uboldi FM, Ferrua P, Vergottini G, Manunta A (2018) Surgical treatment of objective patellar instability: long-term results. Joints 6:33–36
Carstensen SE, Feeley SM, Burrus MT, Deasey M, Rush J, Diduch DR (2020) Sulcus deepening trochleoplasty and medial patellofemoral ligament reconstruction for patellofemoral instability: a 2-year study. Arthroscopy 36:2237–2245
Chatterton A, Nielsen TG, Sørensen OG, Lind M (2018) Clinical outcomes after revision surgery for medial patellofemoral ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:739–745
Christensen TC, Sanders TL, Pareek A, Mohan R, Dahm DL, Krych AJ (2017) Risk factors and time to recurrent ipsilateral and contralateral patellar dislocations. Am J Sports Med 45:2105–2110
Colvin AC, West RV (2008) Patellar instability. J Bone Jt Surg Am 90:2751–2762
Damasena I, Blythe M, Wysocki D, Kelly D, Annear P (2017) Medial patellofemoral ligament reconstruction combined with distal realignment for recurrent dislocations of the patella: 5-year results of a randomized controlled trial. Am J Sports Med 45:369–376
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Erickson BJ, Nguyen J, Gasik K, Gruber S, Brady J, Shubin Stein BE (2019) Isolated medial patellofemoral ligament reconstruction for patellar instability regardless of tibial tubercle-trochlear groove distance and patellar height: outcomes at 1 and 2 years. Am J Sports Med 47:1331–1337
Franciozi CE, Ambra LF, Albertoni LJB, Debieux P, Granata GSdM, Kubota MS, Carneiro M, Abdalla RJ, Luzo MVM, Cohen M (2019) Anteromedial tibial tubercle osteotomy improves results of medial patellofemoral ligament reconstruction for recurrent patellar instability in patients with tibial tuberosity-trochlear groove distance of 17 to 20 mm. Arthroscopy 35:566–574
Frings J, Balcarek P, Tscholl P, Liebensteiner M, Dirisamer F, Koenen P (2020) Conservative versus surgical treatment for primary patellar dislocation. Dtsch Arztebl Int 117:279–286
Hiemstra LA, Kerslake S, Loewen M, Lafave M (2016) Effect of trochlear dysplasia on outcomes after isolated soft tissue stabilization for patellar instability. Am J Sports Med 44:1515–1523
Huntington LS, Webster KE, Devitt BM, Scanlon JP, Feller JA (2020) Factors associated with an increased risk of recurrence after a first-time patellar dislocation: a systematic review and meta-analysis. Am J Sports Med 48:2552–2562
Ignozzi AJ, Hyde Z, Dart SE, Diduch DR (2021) Sulcus-deepening trochleoplasty for trochlear dysplasia. Video J Sports Med 1:263502542110111
Keilani M, Palma S, Crevenna R, Gaudart C, Hasenöhrl T, Reschl M, Huto N, Hajdu S, Widhalm HK (2019) Functional outcome after recurrent patellar dislocation: comparison of two surgical techniques-Medial patellofemoral ligament reconstruction (MPFL) vs. Elmslie Trillat procedure. Wien Klin Wochenschr 131:614–619
Krych AJ, O’Malley MP, Johnson NR, Mohan R, Hewett TE, Stuart MJ, Dahm DL (2018) Functional testing and return to sport following stabilization surgery for recurrent lateral patellar instability in competitive athletes. Knee Surg Sports Traumatol Arthrosc 26:711–718
Liu JN, Wu H-H, Garcia GH, Kalbian IL, Strickland SM, Shubin Stein BE (2018) Return to sports after tibial tubercle osteotomy for patellofemoral pain and osteoarthritis. Arthroscopy 34:1022–1029
Longo UG, Berton A, Salvatore G, Migliorini F, Ciuffreda M, Nazarian A, Denaro V (2016) Medial patellofemoral ligament reconstruction combined with bony procedures for patellar instability: current indications, outcomes, and complications. Arthroscopy 32:1421–1427
Luceri F, Roger J, Randelli PS, Lustig S, Servien E (2020) How does isolated medial patellofemoral ligament reconstruction influence patellar height? Am J Sports Med 48:895–900
Malatray M, Magnussen R, Lustig S, Servien E (2019) Lateral retinacular release is not recommended in association to MPFL reconstruction in recurrent patellar dislocation. Knee Surg Sports Traumatol Arthrosc 27:2659–2664
Mulliez A, Lambrecht D, Verbruggen D, Van Der Straeten C, Verdonk P, Victor J (2017) Clinical outcome in MPFL reconstruction with and without tuberositas transposition. Knee Surg Sports Traumatol Arthrosc 25:2708–2714
Myer GD, Barber Foss KD, Gupta R, Hewett TE, Ittenbach RF (2016) Analysis of patient-reported anterior knee pain scale: implications for scale development in children and adolescents. Knee Surg Sports Traumatol Arthrosc 24:653–660
Neri T, Parker DA, Beach A, Gensac C, Boyer B, Farizon F, Philippot R (2019) Medial patellofemoral ligament reconstruction with or without tibial tubercle transfer is an effective treatment for patellofemoral instability. Knee Surg Sports Traumatol Arthrosc 27:805–813
Nolan JE, Schottel PC, Endres NK (2018) Trochleoplasty: indications and technique. Curr Rev Musculoskelet Med 11:231–240
Saltzman BM, Rao A, Erickson BJ, Cvetanovich GL, Levy D, Bach BR, Cole BJ (2017) A systematic review of 21 tibial tubercle osteotomy studies and more than 1000 knees: indications, clinical outcomes, complications, and reoperations. Am J Orthop 46:E396–E407
van Sambeeck JDP, van de Groes SAW, Verdonschot N, Hannink G (2018) Trochleoplasty procedures show complication rates similar to other patellar-stabilizing procedures. Knee Surg Sports Traumatol Arthrosc 26:2841–2857
Sanders TL, Pareek A, Hewett TE, Stuart MJ, Dahm DL, Krych AJ (2018) Incidence of first-time lateral patellar dislocation: a 21-year population-based study. Sports Health 10:146–151
Sappey-Marinier E, Sonnery-Cottet B, O’Loughlin P, Ouanezar H, Reina Fernandes L, Kouevidjin B, Thaunat M (2019) Clinical outcomes and predictive factors for failure with isolated MPFL reconstruction for recurrent patellar instability: a series of 211 reconstructions with a minimum follow-up of 3 years. Am J Sports Med 47:1323–1330
Song SY, Kim T-S, Seo Y-J (2020) Initial conservative treatment of osteochondral fracture of the patella following first-time patellar dislocation. BMC Musculoskelet Disord 21:617
Tecklenburg K, Feller JA, Whitehead TS, Webster KE, Elzarka A (2010) Outcome of surgery for recurrent patellar dislocation based on the distance of the tibial tuberosity to the trochlear groove. J Bone Jt Surg Br 92:1376–1380
Vogel LA, Pace JL (2019) Trochleoplasty, medial patellofemoral ligament reconstruction, and open lateral lengthening for patellar instability in the setting of high-grade trochlear dysplasia. Arthrosc Tech 8:e961–e967
Walch G, Dejour H (1989) Radiology in femoro-patellar pathology. Acta Orthop Belg 55:371–380
Weber AE, Nathani A, Dines JS, Allen AA, Shubin-Stein BE, Arendt EA, Bedi A (2016) An algorithmic approach to the management of recurrent lateral patellar dislocation. J Bone Jt Surg Am 98:417–427
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no direct conflict of interest related to the study. However, author S.M.O. has received consulting fees from American Joint Replacement Registry. D.P.P. is a paid presenter for Zimmer. B.M.S. received publishing royalties, financial or material support from Nova Science Publishers. J.E.F. received research support from Arthrix and Smith & Nephew.
Ethical approval
This study was IRB approved, Pro00024253.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gorbaty, J.D., Varkey, D.T., Hong, I.S. et al. Outcomes and reoperation rates after tibial tubercle transfer and medial patellofemoral ligament reconstruction: higher revision stabilization in patients with trochlear dysplasia and patella alta. Knee Surg Sports Traumatol Arthrosc 30, 2227–2234 (2022). https://doi.org/10.1007/s00167-021-06784-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06784-5