Abstract
Purpose
To present the results of a return to sports bridge program designed to reduce knee injuries following ACL reconstruction and physical therapy.
Methods
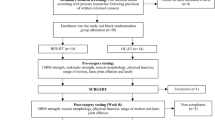
One hundred and fifty (male = 83, female = 67) patients participated in a whole body neuromuscular control, progressive resistance strength and agility training program. Post-program testing included functional movement form, dynamic knee stability, lower extremity power, agility, and sports skill assessments. Participants completed the Knee Outcome Survey–Sports Activity Scale (KOS-SAS) before and after program initiation. Pre-participation scores were re-estimated following program completion.
Results
Global rating KOS-SAS score at program entry was 75 ± 13. Post-program global rating and calculated KOS-SAS were 91.0 ± 9.8 and 90.9 ± 9.7, respectively (p < 0.0001). Pre-participation KOS-SAS score re-estimates at program completion were 54.5 ± 23.3 and 57.3 ± 18.5, respectively. The approximately 20% lower pre-program KOS-SAS score re-estimates (p < 0.0001) observed at program completion suggests that subjects had inaccurately high sports readiness perceptions at program entry. Perceived overall sports activity knee function ratings improved from 2.9 ± 0.6 (abnormal) at program entry to 1.3 ± 0.5 (normal) at completion (p < 0.0001). Most subjects returned back to sports at or above their pre-injury performance skill/performance level (84%, 126/150). By 6.8 ± 3.2 years (range = 2–13 years) post-surgery, ten subjects had sustained an ipsilateral knee re-injury or contralateral knee injury (6.7%). The 2.7% non-contact contralateral and 1.3% non-contact ipsilateral knee injury rates observed were significantly lower than those cited in previous reports.
Conclusion
Supplementing primary ACL reconstruction and standard physical therapy with a return to sports bridge program prior to release to unrestricted sports performance was effective at improving patient outcomes and decreasing ipsilateral knee re-injury and contralateral knee injury rates.
Level of evidence
II.



Similar content being viewed by others
References
Amano H, Toritsuka Y, Uchida R, Mae T, Ohzono K, Shino K (2015) Outcome of anatomical double-bundle ACL reconstruction using hamstring tendons via an outside-in approach. Knee Surg Sports Traumatol Arthrosc 23:1222–1230
Beck NA, Lawrence JTR, Nordin JD, DeFor TA, Tompkins M (2017) ACL tears in school-aged children and adolescents over 20 years. Pediatrics 139:e20161877. https://doi.org/10.1542/peds.2016-1877
Bradley JP, Klimkiewicz JJ, Rytel MJ, Powell JW (2002) Anterior cruciate ligament injuries in the National Football League: epidemiology and current treatment trends among team physicians. Arthroscopy 18:502–509
Brewer BW, Cornelius AE, Stephan Y, Van Raalte J (2010) Self-protective changes in athletic identity following anterior cruciate ligament reconstruction. Psychol Sport Exerc 11:1–5
Brewer BW, Petitpas AJ (2017) Athletic identity foreclosure. Curr Opin Psychol 16:118–122
Buckthorpe M, Della Villa F, Della Villa S, Sergio Roi G (2019) On-field rehabilitation Part 1: 4 pillars of high-quality on-field rehabilitation are restoring movement quality, physical conditioning, restoring sport-specific skills, and progressively developing chronic training load. J Orthop Sports Phys Ther 49:565–569
Caprin JJ, Failla M, Zarzycki R et al (2019) Superior 2-year functional outcomes among young female athletes after ACL reconstruction in 10 return-to-sport training sessions. Orthop J Sports Med 7:2325967119861311. https://doi.org/10.1177/2325967119861311
Chang WH, Wu C-H, Kuo C-C, Chen LH (2018) The role of athletic identity in the development of athlete burnout: the moderating role of psychological flexibility. Psychol Sports Exerc 39:45–51
Coakley J (1992) Burnout among adolescent athletes: a personal failure or social problem? Sociol Sport J 9:271–285
Crawford SN, Waterman BR, Lubowitz JH (2013) Long-term failure of anterior cruciate ligament reconstruction. Arthroscopy 29:1566–1571
Davis-Wilson HC, Pfeiffer SJ, Johnston CD, Seeley MK, Harkey MS, Blackburn JT, Fockler RP, Spang JT, Pietrosimone B (2020) Bilateral gait 6 and 12 months post-anterior cruciate ligament reconstruction compared with controls. Med Sci Sports Exerc 52:785–794
Dekker TJ, Godin JA, Dale KM, Garrett WE, Taylor DC, Riboh JC (2017) Return to sport after pediatric anterior cruciate ligament reconstruction and its effect on subsequent anterior cruciate ligament injury. J Bone Jt Surg Am 99:897–904
Erickson BJ, Harris JD, Fillingham YA et al (2014) Anterior cruciate ligament reconstruction practice patterns by NFL and NCAA football team physicians. Arthroscopy 30:731–738
Failla MJ, Logerstedt DS, Grindem H et al (2016) Does extended preoperative rehabilitation influence outcomes 2 years after ACL reconstruction? A comparative effectiveness study between the MOON and Delaware-Oslo ACL cohorts. Am J Sports Med 44:2608–2614
Grindem H, Snyder-Mackler L, Moksnes H, Engebretsen L, Risberg MA (2016) Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: the Delaware-Oslo ACL cohort study. Br J Sports Med 50:804–808
Hegedus EJ, McDonough S, Bleakley C, Cook CE, Baxter GD (2015) Clinician-friendly lower extremity physical performance measures in athletes: a systematic review of measurement properties and correlation with injury, part 1. The tests for knee function including hop tests. Br J Sports Med 49:642–648
Hewett TE, Myer GD (2011) The mechanistic connection between the trunk, hip, knee, and anterior cruciate ligament injury. Exerc Sport Sci Rev 39:161–166
Kaeding CC, Pedroza AD, Reinke EK, Huston LJ, MOON Consortium, Spindler KP (2015) Risk factors and predictors of subsequent ACL injury in either knee after ACL reconstruction: prospective analysis of 2488 primary ACL reconstructions from the MOON cohort. Am J Sports Med 43:1583–1590
Keller RA, Mehran N, Austin W, Marshall NE, Bastin K, Moutzouros V (2015) Athletic performance at the NFL scouting combine after anterior cruciate ligament reconstruction. Am J Sports Med 43:3022–3026
Kline PW, Burnham J, Yonz M, Johnson D, Ireland ML, Noehren B (2018) Hip external rotation strength predicts hop performance after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:1137–1144
Kyritsis P, Bahr R, Landreau P, Miladi R, Witvrouw E (2016) Likelihood of ACL graft rupture: not meeting six clinical discharge criteria before return to sport is associated with a four times greater risk of rupture. Br J Sports Med 50:946–951
Lilly P (2007) Identity and athletic retirement: a prospective study. Psychol Sport Exerc 8:85–99
Lindanger L, Strand T, Molester AO, Solheim E, Inderhaug E (2019) Return to play and long-term participation in pivoting sports after anterior cruciate ligament reconstruction. Am J Sports Med. https://doi.org/10.1177/0363546519878159
Logerstedt D, Scalzitti D, Risberg M, Engebretsen L, Webster K, Feller J, Snyder-Mackler L, Axe M, McDonough C (2017) Knee stability and movement coordination impairments: knee ligament sprain revision 2017. J Orthop Sports Phys Ther 47:A1–A47
Marcacci M, Zaffagnini S, Iacono F, Vascellari A, Loreti I, Kon E, Presti M (2003) Intra- and extra-articular anterior cruciate ligament reconstruction utilizing autogeneous semitendinosus and gracilis tendons: 5-year clinical results. Knee Surg Sports Traumatol Arthrosc 11:2–8
Martin EM, Horn TS (2013) The role of athletic identity and passion in predicting burnout in adolescent female athletes. Sport Psychol 27:338–348
Mascarenhas R, Tranovich M, Karpie JC, Irrgang JJ, Fu FH, Harner CD (2010) Patellar tendon anterior cruciate ligament reconstruction in the high-demand patient: evaluation of autograft versus allograft reconstruction. Arthroscopy 26(9 Suppl):S58–S66
McCullough KA, Phelps KD, Spindler KP, Matava MJ, Dunn WR, Parker RD, MOON Group, Reinke EK (2012) Return to high school and college level football following ACL reconstruction: a MOON cohort study. Am J Sports Med 40:2523–2529
Nagelli CV, Hewett TE (2017) Should return to sport be delayed until 2 years after anterior cruciate ligament reconstruction? Biological and functional considerations. Sports Med 47:221–232
Nyland J, Brand E (2012) Return-to-play decision making following anterior cruciate ligament reconstruction. In: Doral MN, et al. (eds) Sports injuries. Springer, Berlin, pp 485–493
Nyland J, Gamble C, Franklin T, Caborn DNM (2017) Permanent knee sensorimotor system changes following ACL injury and surgery. Knee Surg Sports Traumatol Arthrosc 25:1461–1474
Nyland J, Klein S, Caborn DNM (2010) Lower extremity compensatory neuromuscular and biomechanical adaptations 2 to 11 years after anterior cruciate ligament reconstruction. Arthroscopy 26:1212–1225
Nyland J, Mattocks A, Kibbe S, Kalloub A, Greene JW, Caborn DNM (2016) Anterior cruciate ligament reconstruction, rehabilitation, and return to play: 2015 update. Open Access J Sports Med 7:21–32
Nyland J, Taniyama D (2019) Editorial commentary: rehabilitation and return-to-sports readiness, the “Black Box” of anterior cruciate ligament reconstruction patient recovery. Arthroscopy 35:2080–2082
Nyland J, Wera J, Klein S, Caborn DNM (2014) Lower extremity neuromuscular compensations during instrumented single leg hop testing 2–10 years following ACL reconstruction. Knee 21:1191–1197
Nyland J, Wera J, Mackinlay KGW, Caborn DNM (2015) Perioperative and postoperative anterior cruciate ligament rehabilitation focused on soft tissue grafts. In: Doral MN, Karlsson J (eds) Sports injuries. Springer, Berlin, pp 1295–1313
Pantano KJ, Irrgang JJ, Burdett R, Delitto A, Harner C, Fu FH (2001) A pilot study on the relationship between physical impairment and activity restriction in persons with anterior cruciate ligament reconstruction at long-term follow-up. Knee Surg Sports Traumatol Arthrosc 9:369–378
Paterno MV, Rauh MJ, Schmitt LC, Ford KR, Hewett TE (2014) Incidence of second ACL injuries 2 years after primary ACL reconstruction and return to sport. Am J Sports Med 42:1567–1573
Pfile KR, Curioz B (2017) Coach-led prevention programs are effective in reducing anterior cruciate ligament injury risk in female athletes: a number-needed-to-treat analysis. Scand J Med Sci Sports 27:1950–1958
Piussi R, Beischer S, Thomee R, Senorski EH (2019) Superior knee self-efficacy and quality of life throughout the first year in patients who recover symmetrical muscle function after ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05703-z
Renstrom PA (2013) Eight clinical conundrums relating to anterior cruciate ligament (ACL) injury in sport: recent evidence and a personal reflection. Br J Sports Med 47:367–372
Ronkainen NJ, Kavoura A, Ryba TA (2016) A meta-study of athletic identity research in sport psychology: current status and future directions. Int Rev Sport Psychol 9:45–64
Sandon A, Engstrom B, Forssblad M (2020) High risk of further anterior cruciate ligament injury in a 10-year follow-up study of anterior cruciate ligament-reconstructed soccer players in the Swedish National Knee Ligament Registry. Arthroscopy 36:189–195
Singhal MC, Gardiner JR, Johnson DL (2007) Failure of primary anterior cruciate ligament surgery using anterior tibialis allograft. Arthroscopy 23:469–475
Webster KE, Feller JA, Leigh WB, Richmond AK (2014) Younger patients are at increased risk for graft rupture and contralateral injury after anterior cruciate ligament reconstruction. Am J Sports Med 42:641–647
Webster KE, McPherson AL, Hewett TE, Feller JA (2019) Factors associated with a return to preinjury level of sport performance after anterior cruciate ligament reconstruction surgery. Am J Sports Med 47:2557–2562
Wellsandt E, Failla MJ, Snyder-Mackler L (2017) Limb symmetry indexes can overestimate knee function after anterior cruciate ligament injury. J Orthop Sports Phys Ther 47:334–338
Wiese-Bjornstal DM, Smith AM, Shaffer SM, Morrey MA (1998) An integrated model of response to sport injury: psychological and sociological dimensions. J Appl Sport Psychol 10:46–59
Wiggins AJ, Grandhi RK, Schneider DK, Stanfield D, Webster KE, Myer GD (2016) Risk of secondary injury in younger athletes after anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Am J Sport Med 44:1861–1876
Wright RW, Dunn WR, Amendola A et al (2007) Risk of tearing the intact anterior cruciate ligament in the contralateral knee and rupturing the anterior cruciate ligament graft during the first 2 years after anterior cruciate ligament reconstruction. Am J Sports Med 36:1131–1134
Wright RW, Magnussen RA, Dunn WR, Spindler KP (2011) Ipsilateral graft and contralateral ACL rupture at five years or more following ACL reconstruction. J Bone Jt Surg Am 93:1159–1165
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have nothing to disclose that could have direct or potential influence or impart bias on the work. All authors have read and approved the final submitted manuscript.
Funding
No external source of funding was used.
Ethical approval
This experimental research has been performed with the approval of the local ethics committee (Spalding University Research Ethics Committee REC #02-192020). Research is in compliance with the Helsinki Declaration.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nyland, J., Greene, J., Carter, S. et al. Return to sports bridge program improves outcomes, decreases ipsilateral knee re-injury and contralateral knee injury rates post-ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 28, 3676–3685 (2020). https://doi.org/10.1007/s00167-020-06162-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06162-7