Abstract
Purpose
There is a theoretical risk of injury to neurovascular structures during inside-out meniscal repair without a safety incision, although there are limited studies assessing this risk. This simulation study on archival MRI films was performed to assess the risk for the popliteal neurovascular bundle and the peroneal nerve during passage of needles for inside-out meniscus repair without a “safety incision”, thereby defining a “safe zone” of the menisci that can be safely repaired using this technique.
Methods
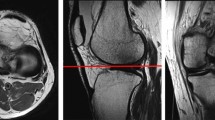
Archival MRI scans (n = 50) were retrieved and axial sections through the menisci were used for simulation. The needle passage was simulated for different points on the posterior horn and body of lateral and medial menisci at “half-hour” intervals using clock method (15° intervals) with three different portals and two different needle cannulas, resulting in six different scenarios of needle passage for each point on the meniscus. The distance of the needle in each scenario was measured from popliteal vessels (n = 50) and peroneal nerve (n = 10). The value “mean-3SD” was calculated for positive means and “Mean + 3SD” was calculated if the mean was negative. An additional 2 mm was defined as “safe distance”. Thus, simulation models in which the mean − 3SD was less than 2 mm (or mean + 3SD was greater than − 2 mm for negative means) were labelled as “unsafe”.
Results
Needle passage through medial meniscus at and medial to 1 o’clock position for a right knee (or 11 o’clock position for a left knee) was safe, irrespective of the portal and needle type. For the lateral meniscus, only the equatorial region was found to be safe with this method.
Conclusions
The popliteal neurovascular bundle is safe during the inside-out medial meniscal repair without a safety incision. For the terminal-most part of the posterior horn, the AM portal and the straight cannula should be avoided. However, this method without safety incision cannot be recommended for lateral meniscus because of the risk to the popliteal vessels and the peroneal nerve. Instead, the inside-out method with a safety incision, or an all-inside method should be used for lateral meniscus.
Level of evidence
III.






Similar content being viewed by others
References
Abouheif MM, Shibuya H, Niimoto T, Kongcharoensombat W, Deie M, Adachi N, Ochi M (2011) Determination of the safe penetration depth during all-inside meniscal repair of the posterior part of the lateral meniscus using the FasT-Fix suture repair system. Knee Surg Sports Traumatol Arthrosc 19:1868–1875
Ahn JH, Kim CH, Lee SH (2016) Repair of the posterior third of the meniscus during meniscus allograft transplantation: conventional inside-out repair versus FasT-Fix All-Inside Repair. Arthroscopy 32(2):295–305
Amis AA, Jakob RP (1998) Anterior cruciate ligament graft positioning, tensioning and twisting. Knee Surg Sports Traumatol Arthrosc 6(Suppl 1):S2–S12
Baena AE, Castilla BM, Fernandez JS, de Rota Conde AF, Reina AE, Rubio FE (2011) Inside-out medial meniscus suture: an analysis of the risk of injury to the popliteal neurovascular bundle. Arthroscopy 27(4):516–521
Baena AE. Arthroscopic inside–out repair of the posterior horn of the medial meniscus. Video. https://www.vumedi.com/video/arthroscopic-insideout-repair-of-the-posterior-horn-of-the-medial-meniscus
Bernard M, Grothues-Spork M, Georgoulis A, Hertel P (1994) Neural and vascular complications of arthroscopic meniscal surgery. Knee Surg Sports TraumatolArthrosc 2(1):14–18
Buckland D, Sadoghi P, Wimmer MD, Vavken P, Pagenstert GI, Valderrabano V, Rosso C (2015) Meta-analysis on biomechanical properties of meniscus repairs: are devices better than sutures? Knee Surg Sports Traumatol Arthrosc 23:83–89
Cannon WD, Vittori JM (1992) The incidence of healing in arthroscopic meniscal repairs in anterior cruciate ligament-reconstructed knees versus stable knees. Am J Sports Med 20(2):176–181
Chen NC, Martin SD, Gill TJ (2007) Risk to the lateral geniculate artery during arthroscopic lateral meniscal suture passage. Arthroscopy 23:642–646
Cuéllar A, Cuéllar R, Heredia JD, Cuéllar A, García-Alonso I, Ruiz-Ibán MA (2018) The all-inside meniscal repair technique has less risk of injury to the lateral geniculate artery than the inside-out repair technique when suturing the lateral meniscus. Knee Surg Sports Traumatol Arthrosc 26:793–798
Espejo-Baena A, Golano P, Meschian S, Garcia-Herrera JM, Serrano Jiménez JM (2007) Complications in medial meniscus suture: a cadaveric study. Knee Surg Sports Traumatol Arthrosc 15:811–816
Feucht MJ, Grande E, Brunhuber J, Rosenstiel N, Burgkart R, Imhoff AB, Braun S (2015) Biomechanical evaluation of different suture materials for arthroscopic transtibial pull-out repair of posterior meniscus root tears. Knee Surg Sports Traumatol Arthrosc 23:132–139
Fox J (2005) The R commander: a basic statistics graphical user interface to R. J Stat Softw 14(9):1–42
Gliatis J, Kouzelis A, Panagopoulos A, Lambiris E (2005) Chondral injury due to migration of a Mitek RapidLoc meniscal repair implant after successful meniscal repair: a case report. Knee Surg Sports Traumatol Arthrosc 13:280–282
Grant JA, Wilde J, Miller BS, Bedi A (2012) Comparison of inside-out and all-inside techniques for the repair of isolated meniscal tears: a systematic review. Am J Sports Med 40(2):459–468
Gwathmey FW, Golish SR, Diduch DR (2012) Complications in brief: meniscus repair. Clin Orthop Relat Res 470(7):2059–2066
James W, Johannsen M, Cinque M, Chahla J, LaPrade RF (2017) An evidence-based approach to the diagnosis and treatment of meniscal root tears. Minerva Ortop Traumatol 68:81–90
Krych AJ, Johnson NR, Wu IT, Smith PA, Stuart MJ (2017) A simple cinch is superior to a locking loop for meniscus root repair: a human biomechanical comparison of suture constructs in a transtibial pull-out model. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4652-1
Kwak DS, Han CW, Han SH (2010) Tibial intramedullary canal axis and its influence on the intramedullary alignment system entry point in Koreans. Anat Cell Biol 43(3):260–267
Mutsaerts ELAR, van Eck CF, van de Graaf VA, Doornberg JN, van den Bekerom MPJ (2016) Surgical interventions for meniscal tears: a closer look at the evidence. Arch Orthop Trauma Surg 136(3):361–370
Nelson CG, Bonner KF (2013) Inside-out meniscus repair. Arthrosc Tech 2:e453–e460
R Development Core Team (2011) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. ISBN 3-900051-07-0. http://www.R-project.org/
Stäubli HU, Rauschning W (1994) Tibial attachment area of the anterior cruciate ligament in the extended knee position. Anatomy and cryosections in vitro complemented by magnetic resonance arthrography in vivo. Knee Surg Sports Traumatol Arthrosc 2(3):138–146
Turman KA, Diduch DR, Miller MD (2009) All-inside meniscal repair. Sports Health 1(5):438–444
Warren RF (1990) Meniscectomy and repair in the anterior cruciate ligament-deficient patient. Clin Orthop Relat Res 252:55–63
Yang G, Wang Z, Wen X, Jiang Z, Qi X, Yang C (2016) The relationship between the midpoints connecting the tibial attachments of the anterior and posterior cruciate ligaments and the transepicondylar axis: in vivo three-dimensional measurement in the Chinese population. Knee 23(5):777–784
Funding
There was no source of funding.
Author information
Authors and Affiliations
Contributions
HG conceived the study, designed the study, was involved in performance of simulation study and data collection, coordination, statistical analysis, and drafted the manuscript. RGG was involved in design of study, performance of simulation and data collection, and performed critical review of the manuscript. HK was involved in design of study, data collection, and performed critical review of the manuscript. VJ was involved in design of study, data collection, and performed critical review of the manuscript. VSh was involved in design of study, and performed critical review of the manuscript. RKD was involved in performance of simulation study and data collection, and performed critical review of the manuscript. ADU was involved in design of study, statistical analysis, and performed critical review of the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
Prior ethical approval was obtained from Institutional Ethics Committee (approval no. IEC/SJH/VMMC/Project/May-2016/583).
Informed consent
Waiver for informed consent was obtained from the Institutional Ethics Committee as the study was performed on archival MRI data.
Rights and permissions
About this article
Cite this article
Gupta, H., Ghasi, R.G., Kataria, H. et al. Popliteal neurovascular bundle is safe during inside-out repair of medial meniscus without a safety incision. Knee Surg Sports Traumatol Arthrosc 27, 153–165 (2019). https://doi.org/10.1007/s00167-018-5060-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5060-x