Abstract
Purpose
The purpose of this meta-analysis was to investigate patient and diagnostic parameters influencing the reported rates of recurrent rotator cuff defects after ARCR.
Methods
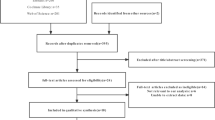
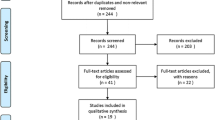
PubMed, EMBASE, Cochrane Library and Scopus databases were searched for clinical studies on tendon defects after ARCR. Imaging modalities, definitions, detection time points, and other known patient risk factors (patient age, tear severity, grade of fatty infiltration, repair technique) as well as reported defect rates were extracted. A meta-analysis of proportion and meta-regression analysis were used to investigate independent variables influencing reported defect rates.
Results
Of 109 articles reviewed, the diagnostic studies used magnetic resonance imaging (MRI) only (n = 56), ultrasound (US) only (n = 28), MRI or computed tomography (CT) arthrography (CTA, n = 14) or a combination of US, MRI and CTA (n = 11) up to 57 months after ARCR. Definitions of tendon defects were highly variable, including those of partial tendon healing with insufficient thickness defined as either an acceptable outcome (n = 72) or a recurrent defect (n = 22). Reported defect rates demonstrated highly significant heterogeneity between studies and groups. Follow-up time and the evaluation of partial tendon healing were independent factors of the defect rate alongside age, tear severity and repair technique. The type of imaging did not significantly alter defect rates.
Conclusion
A number of specific factors significantly alter the rates of rotator cuff defects reported after ARCR. Standardized protocols in clinical practice are required for consistent diagnosis of recurrent defects after ARCR.
Level of evidence
IV.


Similar content being viewed by others
Abbreviations
- ARCR:
-
Arthroscopic rotator cuff repair
- CT:
-
Computed tomography
- CTA:
-
Computed tomographic arthrography
- MRI:
-
Magnetic resonance imaging
- US:
-
Ultrasound
References
Audigé L, Flury M, Mueller AM, ARCR CES Consensus Panel, Durchholz H (2016) Complications associated with arthroscopic rotator cuff tear repair: definition of core event set by Delphi consensus process. J Shoulder Elbow Surg 25(12):1907–1917. doi:10.1016/j.jse.2016.04.036
Audigé L, Bhandari M, Griffin D, Middleton P, Reeves BC (2004) Systematic reviews of nonrandomized clinical studies in the orthopaedic literature. Clin Orthop Relat Res 427:249–257
Audigé L, Blum R, Muller AM, Flury M, Durchholz H (2015) Complications following arthroscopic rotator cuff tear repair: a systematic review of terms and definitions with focus on shoulder stiffness. Orthop J Sports Med. doi:10.1177/2325967115587861
Barendregt JJ, Doi SA, Lee YY, Norman RE, Vos T (2013) Meta-analysis of prevalence. J Epidemiol Community Health 67(11):974–978
Chen M, Xu W, Dong Q, Huang Q, Xie Z, Mao Y (2013) Outcomes of single-row versus double-row arthroscopic rotator cuff repair: a systematic review and meta-analysis of current evidence. Arthroscopy 29(8):1437–1449
Cho NS, Moon SC, Jeon JW, Rhee YG (2015) The influence of diabetes mellitus on clinical and structural outcomes after arthroscopic rotator cuff repair. Am J Sports Med 43(4):991–997
Cho NS, Yi JW, Rhee YG (2009) Arthroscopic biceps augmentation for avoiding undue tension in repair of massive rotator cuff tears. Arthroscopy 25(2):183–191
Codsi MJ, Rodeo SA, Scalise JJ, Moorehead TM, Ma CB (2014) Assessment of rotator cuff repair integrity using ultrasound and magnetic resonance imaging in a multicenter study. J Shoulder Elbow Surg 23(10):1468–1472
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Duquin TR, Buyea C, Bisson LJ (2010) Which method of rotator cuff repair leads to the highest rate of structural healing? A systematic review. Am J Sports Med 38(4):835–841
Galatz LM, Ball CM, Teefey SA, Middleton WD, Yamaguchi K (2004) The outcome and repair integrity of completely arthroscopically repaired large and massive rotator cuff tears. J Bone Joint Surg Am 86-A(2):219–224
Gerber C, Fuchs B, Hodler J (2000) The results of repair of massive tears of the rotator cuff. J Bone Joint Surg Am 82(4):505–515
Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC (1994) Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res 304:78–83
Goutallier D, Postel JM, Gleyze P, Leguilloux P, Van Driessche S (2003) Influence of cuff muscle fatty degeneration on anatomic and functional outcomes after simple suture of full-thickness tears. J Shoulder Elbow Surg 12(6):550–554
Harbord RM, Higgins JPT (2008) Meta-regression in Stata. Stata J 8(4):493–519
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2):377–381
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Iannotti JP, Deutsch A, Green A, Rudicel S, Christensen J, Marraffino S, Rodeo S (2013) Time to failure after rotator cuff repair: a prospective imaging study. J Bone Joint Surg Am 95(11):965–971
Kim JH, Hong IT, Ryu KJ, Bong ST, Lee YS, Kim JH (2014) Retear rate in the late postoperative period after arthroscopic rotator cuff repair. Am J Sports Med 42(11):2606–2613
Lee KW, Seo DW, Bae KW, Choy WS (2013) Clinical and radiological evaluation after arthroscopic rotator cuff repair using suture bridge technique. Clin Orthop Surg 5(4):306–313. doi:10.4055/cios.2013.5.4.306
McCarron JA, Derwin KA, Bey MJ, Polster JM, Schils JP, Ricchetti ET, Ianotti JP (2013) Failure with continuity in rotator cuff repair “healing”. Am J Sports Med 41(1):134–141
McElvany MD, McGoldrick E, Gee AO, Neradilek MB, Matsen FA 3rd (2015) Rotator cuff repair: published evidence on factors associated with repair integrity and clinical outcome. Am J Sports Med 43(2):491–500
Melis B, Nemoz C, Walch G (2009) Muscle fatty infiltration in rotator cuff tears: descriptive analysis of 1688 cases. Orthop Traumatol Surg Res 95(5):319–324. doi:10.1016/j.otsr.2009.05.001
Millett PJ, Warth RJ, Dornan GJ, Lee JT, Spiegl UJ (2014) Clinical and structural outcomes after arthroscopic single-row versus double-row rotator cuff repair: a systematic review and meta-analysis of level I randomized clinical trials. J Shoulder Elbow Surg 23(4):586–597
Morse K, Davis AD, Afra R, Kaye EK, Schepsis A, Voloshin I (2008) Arthroscopic versus mini-open rotator cuff repair: a comprehensive review and meta-analysis. Am J Sports Med 36(9):1824–1828
Neyton L, Godenèche A, Nové-Josserand L, Carrillon Y, Cléchet J, Hardy MB (2013) Arthroscopic suture-bridge repair for small to medium size supraspinatus tear: healing rate and retear pattern. Arthroscopy 29(1):10–17
Nho SJ, Shindle MK, Adler RS, Warren RF, Altchek DW, MacGillivray JD (2009) Prospective analysis of arthroscopic rotator cuff repair: subgroup analysis. J Shoulder Elbow Surg 18(5):697–704
Nyaga VN, Arbyn M, Aerts M (2014) Metaprop: a Stata command to perform meta-analysis of binomial data. Arch Public Health 72:39. doi:10.1186/2049-3258-72-39
Oh JH, Kim SH, Ji HM, Jo KH, Bin SW, Gong HS (2009) Prognostic factors affecting anatomic outcome of rotator cuff repair and correlation with functional outcome. Arthroscopy 25(1):30–39
Park JY, Siti HT, Keum JS, Moon SG, Oh KS (2010) Does an arthroscopic suture bridge technique maintain repair integrity?: a serial evaluation by ultrasonography. Clin Orthop Relat Res 468(6):1578–1587
Pearce N (2000) The ecological fallacy strikes back. J Epidemiol Community Health 54(5):326–327
Peters KS, McCallum S, Briggs L, Murrell GA (2012) A comparison of outcomes after arthroscopic repair of partial versus small or medium-sized full-thickness rotator cuff tears. J Bone Joint Surg Am 94(12):1078–1085
Roy JS, Braën C, Leblond J, Desmeules F, Dionne CE, MacDermid JC, Bureau NJ, Frémont P (2015) Diagnostic accuracy of ultrasonography, MRI and MR arthrography in the characterisation of rotator cuff disorders: a systematic review and meta-analysis. Br J Sports Med 49(20):1316–1328
Russell RD, Knight JR, Mulligan E, Khazzam MS (2014) Structural integrity after rotator cuff repair does not correlate with patient function and pain: a meta-analysis. J Bone Joint Surg Am 96(4):265–271
Saccomanno MF, Cazzato G, Fodale M, Sircana G, Milano G (2015) Magnetic resonance imaging criteria for the assessment of the rotator cuff after repair: a systematic review. Knee Surg Sports Traumatol Arthrosc 23(2):423–442
Saccomanno MF, Sircana G, Cazzato G, Donati F, Randelli P, Milano G (2015) Prognostic factors influencing the outcome of rotator cuff repair: a systematic review. Knee Surg Sports Traumatol Arthrosc 24(12):3809–3819. doi:10.1007/s00167-015-3700-y
Safran O, Schroeder J, Bloom R, Weil Y, Milgrom C (2011) Natural history of nonoperatively treated symptomatic rotator cuff tears in patients 60 years old or younger. Am J Sports Med 39(4):710–714
Sugaya H, Maeda K, Matsuki K, Moriishi J (2005) Functional and structural outcome after arthroscopic full-thickness rotator cuff repair: single-row versus dual-row fixation. Arthroscopy 21(11):1307–1316
Thomazeau H, Boukobza E, Morcet N, Chaperon J, Langlais F (1997) Prediction of rotator cuff repair results by magnetic resonance imaging. Clin Orthop Relat Res 344:275–283
Wu XL, Briggs L, Murrell GA (2012) Intraoperative determinants of rotator cuff repair integrity: an analysis of 500 consecutive repairs. Am J Sports Med 40(12):2771–2776
Yoo JH, Cho NS, Rhee YG (2013) Effect of postoperative repair integrity on health-related quality of life after rotator cuff repair: healed versus retear group. Am J Sports Med 41(11):2637–2644
Acknowledgements
Support for this research was provided by the Schulthess Clinic in Zurich and the University Hospital of Basel in Switzerland. The authors would like to acknowledge the support of Sebastian Kunz for extracting the data from selected articles and Melissa Wilhelmi, PhD, medical writer at the Schulthess Clinic, Zurich, Switzerland, for preparation and editing the manuscript as well as supporting the submission process.
Authors’ contributions
LA was the initiator, project coordinator and data analyst. LA and AMM were involved in the study design. Complementary literature search and data collection were undertaken by AMM and HNA. LA, MF and AMM contributed in the data analysis and interpretation. Preparation of the manuscript was done by AMM and LA. All authors have read, revised, and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Müller, A.M., Flury, M., Alsayed, H.N. et al. Influence of patient and diagnostic parameters on reported retear rates after arthroscopic rotator cuff repair. Knee Surg Sports Traumatol Arthrosc 25, 2089–2099 (2017). https://doi.org/10.1007/s00167-017-4481-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-017-4481-2