Abstract
Purpose
Graft failure following anterior cruciate ligament reconstruction (ACLR) is a devastating injury among patients returning to activity. The goals of this study were to define the long-term rate of graft failure after ACLR in the general population and evaluate factors associated with graft failure.
Methods
This long-term observational study included a population-based incidence cohort of patients who underwent primary ACLR after diagnosis with new-onset, isolated ACL tears between 1990 and 2010. For all patients, a chart review was performed to collect information related to the initial injury, treatment, and outcomes. Patients were retrospectively followed to determine the incidence of graft failure following ACLR.
Results
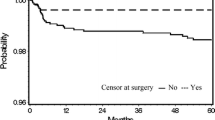
The study cohort consisted of 1355 patients with new-onset, isolated ACL tears treated with ACLR. At a mean follow-up of 10.0 years (±6.4 years) following ACLR, a total of 72 patients (5.3 %) sustained ipsilateral graft failure. The graft survival following ACLR was 99.7 % at 1 year, 96 % at 5 years, 94 % at 10 years, 93 % at 15 years, 92 % at 20 years and 91 % at 25 years. Among patients 22 years or younger (n = 571), the rate of graft failure was significantly higher compared to patients older than 22 years (6.3 vs. 4.6 %, p = 0.04). The rate of graft failure decreased significantly over the 21-year observation period of this study (p < 0.0001).
Conclusions
Among all patients receiving primary ACLR, graft failure remains an uncommon but functionally devastating outcome with an estimated graft survival rate of 91 % at 25 years following surgery. Patients aged 22 or younger had a significantly higher rate of graft failure than older patients. The rate of graft failure decreased over the 21-year span of this study.
Level of evidence
Retrospective case series, Level IV.





Similar content being viewed by others
References
Bernstein J, McGuire K, Freedman K (2003) Statistical sampling and hypothesis testing in orthopaedic research. Clin Orthop Relat Res 413:55–62
Carmont M, Scheffler S, Spalding T, Brown J, Sutton P (2011) Anatomical single bundle anterior cruciate ligament reconstruction. Curr Rev Musculoskelet Med 4:65–72
Freedman K, Back S, Bernstein J (2001) Sample size and statistical power of randomized, controlled trials in orthopaedics. J Bone Joint Surg Br 83:397–402
Gomoll A, Bach B (2006) Managing tunnel malposition and widening in revision anterior cruciate ligament surgery. Oper Techn Sport Med 14:36–44
Kaeding C, Aros B, Pedroza A, Pifel E, Amendola A, Andrish J, Dunn W, Marx R, McCarty E, Parker R, Wright R, Spindler K (2011) Allograft versus autograft anterior cruciate ligament reconstruction: predictors of failure from a MOON prospective longitudinal cohort. Sports Health Multidiscip Approach 3:73–81
Kaeding C, Pedroza A, Reinke E, Huston L, MOON Consortium, Spindler K (2015) Risk factors and predictors of subsequent ACL injury in either knee after ACL reconstruction: prospective analysis of 2488 primary ACL reconstructions from the MOON cohort. Am J Sports Med 43:1583–1590
Krych A, Jackson J, Hoskin T, Dahm D (2008) A meta-analysis of patellar tendon autograft versus patellar tendon allograft in anterior cruciate ligament reconstruction. Arthroscopy 24:292–298
Leys T, Salmon L, Waller A, Linklater J, Pinczewski L (2012) Clinical results and risk factors for reinjury 15 years after anterior cruciate ligament reconstruction: a prospective study of hamstring and patellar tendon grafts. Am J Sports Med 40:595–605
Maletis G, Inacio M, Funahashi T (2015) Risk factors associated with revision and contralateral anterior cruciate ligament reconstructions in the Kaiser Permanente ACLR registry. Am J Sports Med 43:641–647
Markolf K, Hame S, Hunter D, Oakes D, Zoric B, Gause P, Finerman G (2002) Effects of femoral tunnel placement on knee laxity and forces in an anterior cruciate ligament graft. J Orthop Res 20:1016–1024
Morgan J, Dahm D, Levy B, Stuart M, MARS Study Group (2012) Femoral tunnel malposition in ACL revision reconstruction. J Knee Surg 25:361–368
Pallis M, Svoboda S, Cameron K, Owens B (2012) Survival comparison of allograft and autograft anterior cruciate ligament reconstruction at the United States Military Academy. Am J Sports Med 40:1242–1246
Paterno M, Rauh M, Schmitt L, Ford K, Hewett T (2014) Incidence of second ACL injuries 2 years after primary ACL reconstruction and return to sport. Am J Sports Med 42:1567–1573
Pinczewski L, Lyman J, Salmon L, Russell V, Roe J, Linklater J (2007) A 10-year comparison of anterior cruciate ligament reconstructions with hamstring tendon and patellar tendon autograft: a controlled, prospective trial. Am J Sports Med 35:564–574
Rocca W, Yawn B, St Sauver J, Grossardt B, Melton L (2012) History of the Rochester epidemiology project: half a century of medical records linkage in a US population. Mayo Clin Proc 87:1202–1213
Salmon L, Russell V, Musgrove T, Pinczewski L, Refshauge K (2005) Incidence and risk factors for graft rupture and contralateral rupture after anterior cruciate ligament reconstruction. Arthroscopy 21:948–957
Sanders T, Maradit Kremers H, Bryan A, Kremers W, Stuart M, Krych A (2015) Procedural intervention for arthrofibrosis after ACL reconstruction: trends over two decades. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3799-x
Shelbourne K, Gray T, Haro M (2009) Incidence of subsequent injury to either knee within 5 years after anterior cruciate ligament reconstruction with patellar tendon autograft. Am J Sports Med 37:246–251
St Sauver J, Grossardt B, Yawn B et al (2012) Data resource profile: the Rochester Epidemiology Project (REP) medical records-linkage system. Int J Epidemiol 41:1614–1624
Tanaka Y, Yonetani Y, Shiozaki Y, Kitaguchi T, Sato N, Takashita S, Horibe S (2010) Retear of anterior cruciate ligament grafts in female basketball players: a case series. Sports Med Arthrosc Rehabil Ther Technol 9:7
Van Eck C, Lesniak B, Schreiber V, Fu F (2010) Anatomic single- and double-bundle anterior cruciate ligament reconstruction flowchart. Arthroscopy 26:258–268
Webster K, Feller J (2016) Exploring the high reinjury rate in younger patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med. doi:0363546516651845
Wright R, Dunn W, Amendola A, Andrish J, Bergfeld J, Kaeding C, Marx R, McCarty E, Parker R, Wolcott M, Wolf B, Spindler K (2007) Risk of tearing the intact anterior cruciate ligament in the contralateral knee and rupturing the anterior cruciate ligament graft during the first 2 years after anterior cruciate ligament reconstruction: a prospective MOON cohort study. Am J Sports Med 35:1131–1134
Wright R, Magnussen R, Dunn W, Spindler K (2011) Ipsilateral and contralateral ACL rupture at five years or more following ACL reconstruction. J Bone Joint Surg 93:1159–1165
Yagi M, Wong E, Kanamori A, Debski R, Fu F, Woo S (2002) Biomechanical analysis of an anatomic anterior cruciate ligament reconstruction. Am J Sports Med 30:660–666
Acknowledgments
This study was made possible by the Rochester Epidemiology Project which is supported by the National Institute on Aging of the National Institutes of Health under award number R01AG034676. The findings and conclusions of this report are solely the responsibility of the authors and do not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sanders, T.L., Pareek, A., Hewett, T.E. et al. Long-term rate of graft failure after ACL reconstruction: a geographic population cohort analysis. Knee Surg Sports Traumatol Arthrosc 25, 222–228 (2017). https://doi.org/10.1007/s00167-016-4275-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4275-y