Abstract
This study is one of the first to present causal evidence of the morbidity costs of fine particulates (PM2.5) for all age cohorts in a developing country, using individual-level health spending data from a basic medical insurance program in Wuhan, China. Our instrumental variable (IV) approach uses thermal inversion to address potential endogeneity in PM2.5 concentrations and shows that PM2.5 imposes a significant impact on healthcare expenditures. The two-stage least squares (2SLS) estimates suggest that a 10 μg/m3 (micrograms per cubic meter) reduction in monthly average PM2.5 leads to a 2.36% decrease in the value of health spending and a 0.79% decline in the number of transactions at pharmacies and healthcare facilities. Also, this effect, largely driven by spending at pharmacies, is more salient for males and children, as well as middle-aged and older adults. Moreover, our estimates may provide a lower bound on individuals’ willingness to pay, amounting to CNY 43.87 (or USD 7.09) per capita per year for a 10 μg/m3 reduction in PM2.5.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the first author, Xin Zhang, upon reasonable request.
Notes
Medical expenses at pharmacies and healthcare facilities respectively account for 29.3% and 70.7% of the total spending in our data.
There are three main methods for valuing air quality. Each approach has its particular advantages and disadvantages. The hedonic approach infers the value of air quality from property values across regions with differing levels of air pollution exposure (Bayer, Keohane, and Timmins 2009; Chay and Greenstone 2005; Ito and Zhang 2020; Smith and Huang 1995). This approach generally suffers from omitted variable problems, which make the value of air quality endogenous. On the other hand, the contingent valuation method (CVM) directly asks about people’s WTP for better air quality (Sun, Yuan, and Yao 2016; Wang et al. 2015). However, this method is subject to the initial hypothetical monetary value adopted in the survey options and the manner in which the questions are framed. The happiness approach calculates the marginal rate of substitution between a reduction in air pollution and household per capita income by holding happiness constant to assess the monetary value of air pollution (Levinson 2012; Welsch 2006; Zhang et al. 2017b). This approach treats self-reported happiness as a proxy of utility and assumes that utility is comparable among respondents.
Refer to Appendix B for the theoretical model. The model illustrates that people’s WTP for clean air can be estimated by adding up different components of the impact of air pollution on the population’s health and behavior. The marginal effect of air pollution on health spending is just one of the components, other components include mortality impact, reduction in quality of life, and the sub-optimal level of consumption distortion by the exposure to pollution.
According to the 2018 Environmental Performance Index published by Yale University, the five countries with the most polluted air in the world are Nepal, Bangladesh, India, China, and Pakistan.
The UEBMI was launched in 1998 as an employment-based insurance program in urban areas, and its coverage reached 92% in 2010. The URBMI was launched in 2007 to target the unemployed, children, students, and the disabled in urban areas. It covered 93% of the target population as of 2010 (Yu 2015).
As medical expenses covered by the Chinese public health insurance programs are directly billed on medical payment cards, all the payments for people enrolled in public insurance programs—UEBMI and URBMI—are included in the official database by design. Any money saved in the insurance account can be conveyed to the next year. Using others’ insurance accounts to purchase any health services was not allowed during the sample period.
The medication expenses include Western medicine fees, Chinese patent medicine fees, and Chinese herb medicine fees. The examination expenses include laboratory examination fees and imaging examination (B ultrasound, CT and MRI) fees. The treatment expenses include non-surgical treatment fees, surgical treatment fees, and anesthesia fees.
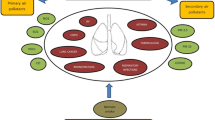
The six air pollutant measures are particulate matter with a diameter smaller than 2.5 µm (PM2.5, fine particulates); particulate matter with a diameter smaller than 10 µm (PM10, coarse particulates); carbon monoxide (CO); nitrogen dioxide (NO2); ozone (O3); and sulfur dioxide (SO2).
Zhang et al. (2017b) suggest that people have a much greater WTP for a reduction in PM2.5 than they do for PM10.
For each individual, we calculate the number of visits to each pharmacy during the sample period and sort the number of visits in descending order. We pick the location of the pharmacy that a person visited most as their home address. If the person did not visit any pharmacy during the sample period, we choose the health facility that the person most often visited. The average number of pharmacies a person visited is 5.27.
The average matching distance between the residential address and the nearest monitoring station is 3.85 km.
We also conduct empirical analysis using data at the individual-daily level without assigning zeros, controlling for demographic variables, daily weather covariates, individual, pharmacy, county-by-year, month and day-of-week fixed effects. The results are displayed in Table A1. The pattern of the estimates is similar to those based on the individual-monthly level data. As we estimate the results only using the subsample for those whose healthcare expenses are positive, indicating that they may either tend to be less healthy or could afford more healthcare expenses, the estimated WTP becomes much larger.
58.7% of the value of health spending/number of transactions are zeros.
The arcsinh transformation is \(\mathrm{arcsinh}\left(\mathrm{y}\right)=\mathrm{ln}(\mathrm{y}+\sqrt{{y}^{2}+1})\).
In the estimable equation of the form \(\mathrm{arcsinh}\left(\mathrm{y}\right)=\mathrm{\alpha }+\mathrm{\beta x}+\upvarepsilon\), the semi-elasticity is \(\frac{\partial y}{\partial x}\cdot \frac{1}{y}=\widehat{\beta }\frac{\sqrt{{y}^{2}+1}}{y}\). As \(\underset{y\to \infty }{\mathrm{lim}}\frac{\sqrt{{y}^{2}+1}}{y}=1\), for large values of y, \(\frac{\partial y}{\partial x}\cdot \frac{1}{y}=\widehat{\beta }\). Therefore, \(\widehat{\beta }\) indicates a semi-elasticity in the arcsinh transformation of y of no less than 10, as suggested by Bellemare and Wichman (2020). Please refer to Bellemare and Wichman (2020) for details.
For example, the IV estimates are substantially (6–17 times) larger than the OLS estimates in (Deryugina et al. 2019).
Table A2 presents the correlations between air pollutants.
We tried to instrument for PM2.5 and another co-pollutant using the thermal inversion strength and the number of occurrences in columns (2)–(6) of Table 4. However, we could not pass the weak identification test.
See columns (2) through (3) of Table 2 for the first-stage estimates.
A similar practice can be found in Williams and Phaneuf (2019), who also study medical expenditure data with a large number of zeros.
The holiday month refers to the month that contains holidays.
Using the average 2013–15 exchange rate of USD 1 = CNY 6.1880 from the Wind Economic Database.
The average disposal income per capita per year of Wuhan urban residents during 2013–2015 was 33,175.87 yuan (Wuhan Statistical Yearbook 2016).
Considering that our current WTP measure only accounts for willingness to pay to mitigate pollution-related morbidity costs (excluding other health aspects of social costs, such as mortality costs and avoidance costs, like facemasks and air filters), and that our individual-monthly level sample has a large share of zero healthcare expenses (i.e., people in a healthy status or who could not afford medical treatment), our measured WTP as a share of disposal income should be a lower-bound estimate. When we instead measure using individual-daily data with positive healthcare expenses only, i.e., among those who were sick and who could afford medical treatment, our estimates suggest that these people are willing to pay much more (CNY 699.29; around 2.11% of average disposal income) per capita per year for the same 10 μg/m3 reduction in PM2.5.
References
Anderson ML (2020) As the wind blows: the effects of long-term exposure to air pollution on mortality. J Eur Econ Assoc 18(4):1886–1927. https://doi.org/10.1093/jeea/jvz051
Arceo E, Hanna R, Oliva P (2016) Does the effect of pollution on infant mortality differ between developing and developed countries? Evidence from Mexico City. Econ J 126(591):257–280. https://doi.org/10.1111/ecoj.12273
Barwick PJ, Li S, Rao D, Zahur NB (2021) The healthcare cost of air pollution: evidence from the world’s largest payment network. NBER Working Paper No. 24688. https://doi.org/10.3386/w24688
Bayer P, Keohane N, Timmins C (2009) Migration and hedonic valuation: the case of air quality. J Environ Econ Manag 58(1):1–14. https://doi.org/10.1016/j.jeem.2008.08.004
Bellemare MF, Wichman CJ (2020) Elasticities and the inverse hyperbolic sine transformation. Oxford Bull Econ Stat 82(1):50–61. https://doi.org/10.1111/obes.12325
Cameron CA, Gelbach JB, Miller DL (2008) Bootstrap-based improvements for inference with clustered errors. Rev Econ Stat 90(3):414–427. https://doi.org/10.1162/rest.90.3.414
Chay KY, Greenstone M (2003) The impact of air pollution on infant mortality: evidence from geographic variation in pollution shocks induced by a recession. Quart J Econ 118(3):1121–1167. https://doi.org/10.1162/00335530360698513
Chay KY, Greenstone M (2005) Does air quality matter? Evidence from the Housing Market. J Polit Econ 113(2):376–424. https://doi.org/10.1086/427462
Chen Y, Ebenstein A, Greenstone M, Li H (2013) Evidence on the impact of sustained exposure to air pollution on life expectancy from China’s Huai River policy. Proc Natl Acad Sci USA 110(32):12936–12941. https://doi.org/10.1073/pnas.1300018110
Chen S, Guo C, Huang X (2018) Air pollution, student health, and school absences: evidence from China. J Environ Econ Manag 92:465–497. https://doi.org/10.1016/j.jeem.2018.10.002
Chen Y, Jin GZ, Kumar N, Shi G (2012) Gaming in air pollution data lessons from China. B.E. J Econ Analys Policy 12(3). https://doi.org/10.1515/1935-1682.3227
Chen S, Oliva P, Zhang P (2022) The effect of air pollution on migration: evidence from China. J Dev Econ 156. https://doi.org/10.1016/j.jdeveco.2022.102833
Currie J, Neidell M (2005) Air pollution and infant health: what can we learn from California’s recent experience? Q J Econ 120(3):1003–1030. https://doi.org/10.1093/qje/120.3.1003
Currie J, Neidell M, Schmieder JF (2009) Air pollution and infant health: lessons from New Jersey. J Health Econ 28(3):688–703. https://doi.org/10.1016/j.jhealeco.2009.02.001
Deryugina T, Heutel G, Miller NH, Molitor D, Reif J (2019) The mortality and medical costs of air pollution: evidence from changes in wind direction. Am Econ Rev 109(12):4178–4219. https://doi.org/10.1257/aer.20180279
Deschênes O, Greenstone M, Shapiro JS (2017) Defensive investments and the demand for air quality: evidence from the NOx budget program. Ame Econ Rev 107(10):2958–2989. https://doi.org/10.1257/aer.20131002
Ebenstein A, Fan M, Greenstone M, He G, Zhou M (2017) New evidence on the impact of sustained exposure to air pollution on life expectancy from China’s Huai River policy. Proc Natl Acad Sci USA 114(39):10384–10389. https://doi.org/10.1073/pnas.1616784114
Ghanem D, Zhang J (2014) Effortless Perfection: do Chinese cities manipulate air pollution data? J Environ Econ Manag 68(2):203–225. https://doi.org/10.1016/j.jeem.2014.05.003
Greenstone M, Hanna R (2014) Environmental regulations, air and water pollution, and infant mortality in India. Am Econ Rev 104(10):3038–3072. https://doi.org/10.1257/aer.104.10.3038
Grossman M (1972) On the concept of health capital and the demand for health. J Polit Econ 80(2):223–255
He G, Fan M, Zhou M (2016) The effect of air pollution on mortality in China: evidence from the 2008 Beijing Olympic Games. J Environ Econ Manag 79:18–39. https://doi.org/10.1016/j.jeem.2016.04.004
Ito K, Zhang S (2020) Willingness to pay for clean air: evidence from air purifier markets in China. J Polit Econ 128(5):1627–1672. https://doi.org/10.1086/705554
Levinson A (2012) Valuing public goods using happiness data: the case of air quality. J Public Econ 96(9–10):869–880. https://doi.org/10.1016/j.jpubeco.2012.06.007
Liao L, Du M, Chen Z (2021) Air pollution, health care use and medical costs: evidence from China. Energy Econ 95. https://doi.org/10.1016/j.eneco.2021.105132
Liu YM, Ao CK (2021) Effect of air pollution on health care expenditure: evidence from respiratory diseases. Health Econ 30(4):858–875. https://doi.org/10.1002/hec.4221
Long Y, Wang J, Wu K, Zhang J (2018) Population exposure to ambient PM2.5 at the subdistrict level in China. Int J Environ Res Public Health 15(12). https://doi.org/10.3390/ijerph15122683
Moretti E, Neidell M (2011) Pollution, health, and avoidance behavior: evidence from the ports of Los Angeles. J Hum Res 46(1):154–175. https://doi.org/10.3368/jhr.46.1.154
Neidell M (2009) Information, avoidance behavior, and health: the effect of ozone on asthma hospitalizations. J Hum Resour 44(2):450–478. https://doi.org/10.1353/jhr.2009.0018
Pope CA, Dockery DW (2006) Health effects of fine particulate air pollution: lines that connect. J Air Waste Manag Assoc 56(6):709–742. https://doi.org/10.1080/10473289.2006.10464485
Roodman D, MacKinnon JG, Nielsen MØ, Webb MD (2019) Fast and wild: bootstrap inference in stata using boottest. Stata J 19(1):4–60. https://doi.org/10.1177/1536867X19830877
Schlenker W, Reed Walker W (2016) Airports, air pollution, and contemporaneous health. Rev Econ Stud 83(2):768–809. https://doi.org/10.1093/restud/rdv043
Smith VK, Huang J-C (1995) Can markets value air quality? A meta-analysis of hedonic property value models. J Polit Econ 103(1):209–227. https://doi.org/10.1086/261981
Sun C, Yuan X, Yao X (2016) Social acceptance towards the air pollution in China: evidence from public’s willingness to pay for smog mitigation. Energy Policy 92:313–324. https://doi.org/10.1016/j.enpol.2016.02.025
Sun C, Kahn ME, Zheng S (2017) Self-protection investment exacerbates air pollution exposure inequality in urban China. Ecol Econ 131:468–474. https://doi.org/10.1016/j.ecolecon.2016.06.030
Wang K, Jinyi Wu, Wang R, Yang Y, Chen R, Maddock JE, Yuanan Lu (2015) Analysis of Residents’ willingness to pay to reduce air pollution to improve children’s health in community and hospital settings in Shanghai, China. Sci Total Environ 533:283–289. https://doi.org/10.1016/j.scitotenv.2015.06.140
Welsch H (2006) Environment and happiness: valuation of air pollution using life satisfaction data. Ecol Econ 58(4):801–813. https://doi.org/10.1016/j.ecolecon.2005.09.006
Williams AM, Phaneuf DJ (2019) The morbidity costs of air pollution: evidence from spending on chronic respiratory conditions. Environ Resource Econ 74(2):571–603. https://doi.org/10.1007/s10640-019-00336-9
Xia F, Xing J, Jintao Xu, Pan X (2022) The short-term impact of air pollution on medical expenditures: evidence from Beijing. J Environ Econ Manag. https://doi.org/10.1016/j.jeem.2022.102680
Yu H (2015) Universal health insurance coverage for 1.3 billion people: what accounts for China’s success? Health Policy 119(9):1145–1152
Zhang J, Mu Q (2018) Air pollution and defensive expenditures: evidence from particulate-filtering facemasks. J Environ Econ Manag 92:517–536. https://doi.org/10.1016/j.jeem.2017.07.006
Zhang X, Zhang X, Chen Xi (2017) Happiness in the air: how does a dirty sky affect mental health and subjective well-being? J Environ Econ Manag 85:81–94. https://doi.org/10.1016/j.jeem.2017.04.001
Zhang X, Zhang X, Chen Xi (2017) Valuing air quality using happiness data: the case of China. Ecol Econ 137:29–36. https://doi.org/10.1016/j.ecolecon.2017.02.020
Zhang X, Chen Xi, Zhang X (2018) The impact of exposure to air pollution on cognitive performance. Proc Natl Acad Sci USA 115(37):9193–9197. https://doi.org/10.1073/pnas.1809474115
Acknowledgements
Xin Zhang acknowledges financial support from the National Natural Science Foundation of China (72003014). Xun Zhang thanks the National Natural Science Foundation of China (71973014) for financial support. Xi Chen is grateful for financial support from the James Tobin Research Fund at Yale Economics Department, Yale Macmillan Center Faculty Research Award (2017–2019), the U.S. PEPPER Center Scholar Award (P30AG021342, 2016–2018), NIH/NIA Career Development Award (K01AG053408, 2017–2022), and a NIH/NIA Research Award (R01AG077529, 2022-2027). The authors acknowledge helpful comments by participants and discussants at the various conferences, seminars and workshops, as well as from editor Kompal Sinha and three anonymous reviewers.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Responsible editor: Kompal Sinha
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, X., Zhang, X., Liu, Y. et al. The morbidity costs of air pollution through the Lens of Health Spending in China. J Popul Econ 36, 1269–1292 (2023). https://doi.org/10.1007/s00148-023-00948-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00148-023-00948-y