Abstract
Purpose
The purpose of the study was to examine the association between socio-demographic and clinical characteristics and perceived social support among patients with a diagnosis of depression and/or anxiety and co-morbid medical conditions from rural south India.
Methods
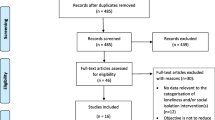
The study was conducted in 49 PHCs in Ramanagara district, Karnataka, and included 2481 participants, who were 30 years or older with co-morbid CMD (Common Mental Disorder) and hypertension, diabetes or ischemic heart disease. Socio-demographic characteristics of the participants were collected, and instrumental, emotional and total social support, quality of life, severity of disability, depression and anxiety were measured via face-to-face interviews using structured questionnaires.
Results
The sample predominantly consisted of Hindu (98.5%) females (75%) in their middle to late adulthood. In multivariate models, age showed a significant curvilinear relation with all forms of social support (B = 0.001 and p < 0.05), and emotional social support (B = − 0.056, p = 0.004) was lower in employed than non-working participants. Household size was positively related to all forms of social support (B = 0.029 for instrumental, B = 0.022 for emotional, B = 0.025 for total social support, all p < 0.001). Quality of life was positively associated with all forms of social support (B = 0.019 for instrumental, B = 0.016 for emotional, B = 0.018 for total social support, all p < 0.001).
Conclusions
For this sample of outpatients diagnosed with both CMD and at least one comorbid medical condition in rural south India, greater household size was associated with better social support. The role of family in providing support can be utilized while designing interventions.
Trial Registration Number
http://Clinicaltrials.gov: NCT02310932 registered December 8, 2014 URL: https://clinicaltrials.gov/ct2/show/record/NCT02310932; Clinical Trials Registry India: CTRI/2018/04/013001 retrospectively registered on April 4, 2018.

Similar content being viewed by others
References
House JS (1981) Work stress and social support. Addison-Wesley Pub. Co, Reading
Cohen S, Wills TA (1985) Stress, social support, and the buffering hypothesis. Psychol Bull 98:310–357
Tomaka J, Thompson S, Palacios R (2006) The relation of social isolation, loneliness, and social support to disease outcomes among the elderly. J Aging Health 18:359–384. https://doi.org/10.1177/0898264305280993
Kruithof WJ, van Mierlo ML, Visser-Meily JMA et al (2013) Associations between social support and stroke survivors’ health-related quality of life—a systematic review. Patient Educ Couns 93:169–176. https://doi.org/10.1016/j.pec.2013.06.003
Uchino BN (2006) Social support and health: a review of physiological processes potentially underlying links to disease outcomes. J Behav Med 29(4):377–387. https://doi.org/10.1007/s10865-006-9056-5(Epub 2006 Jun 7 PMID: 16758315)
Dayapoglu N, Tan M (2010) Quality of life in stroke patients. Neurol India 58:697. https://doi.org/10.4103/0028-3886.72165
Huang C-Y, Hsu M-C, Hsu S-P et al (2010) Mediating roles of social support on poststroke depression and quality of life in patients with ischemic stroke. J Clin Nurs 19:2752–2762. https://doi.org/10.1111/j.1365-2702.2010.03327.x
Teoh V, Sims J, Milgrom J (2009) Psychosocial predictors of quality of life in a sample of community-dwelling stroke survivors: a longitudinal study. Top Stroke Rehabil 16:157–166. https://doi.org/10.1310/tsr1602-157
Padhy M, Lalnuntluangi R, Chelli K, Padiri RA (2016) Social support and adherence among hypertensive patients. Amity J Healthcare Manag 1:33–40
Smyth N, Siriwardhana C, Hotopf M, Hatch SL (2015) Social networks, social support and psychiatric symptoms: social determinants and associations within a multicultural community population. Soc Psychiatry Psychiatr Epidemiol 50:1111–1120. https://doi.org/10.1007/s00127-014-0943-8
Brinker J, Cheruvu VK (2017) Social and emotional support as a protective factor against current depression among individuals with adverse childhood experiences. Prev Med Rep 5:127–133. https://doi.org/10.1016/j.pmedr.2016.11.018
Kumar PNS, George B (2013) Life events, social support, coping strategies, and quality of life in attempted suicide: a case-control study. Indian J Psychiatry 55:46–51. https://doi.org/10.4103/0019-5545.105504
Wang J, Mann F, Lloyd-Evans B et al (2018) Associations between loneliness and perceived social support and outcomes of mental health problems: a systematic review. BMC Psychiatry 18:156. https://doi.org/10.1186/s12888-018-1736-5
Lindfors O, Ojanen S, Jääskeläinen T, Knekt P (2014) Social support as a predictor of the outcome of depressive and anxiety disorder in short-term and long-term psychotherapy. Psychiatry Res 216(1):44–51. https://doi.org/10.1016/j.psychres.2013.12.050(Epub 2014 Jan 9 PMID: 24508367)
Gariépy G, Honkaniemi H, Quesnel-Vallée A (2016) Social support and protection from depression: systematic review of current findings in Western countries. Br J Psychiatry 209:284–293. https://doi.org/10.1192/bjp.bp.115.169094
Muñoz-Laboy M, Severson N, Perry A, Guilamo-Ramos V (2014) Differential impact of types of social support in the mental health of formerly incarcerated latino men. Am J Mens Health 8:226–239. https://doi.org/10.1177/1557988313508303
Sonnenberg CM, Deeg DJH, van Tilburg TG et al (2013) Gender differences in the relation between depression and social support in later life. Int Psychogeriatr 25:61–70. https://doi.org/10.1017/S1041610212001202
Mechakra-Tahiri S-D, Zunzunegui MV, Préville M, Dubé M (2010) Gender, social relationships and depressive disorders in adults aged 65 and over in Quebec. Chronic Dis Can 30:56–65
Djundeva M, Mills M, Wittek R, Steverink N (2015) Receiving instrumental support in late parent-child relationships and parental depression. J Gerontol B Psychol Sci Soc Sci 70:981–994. https://doi.org/10.1093/geronb/gbu136
Rook KS (2009) Gaps in social support resources in later life: an adaptational challenge in need of further research. J Soc Pers Relatsh 26:103–112. https://doi.org/10.1177/0265407509105525
Knoll N, Schwarzer R (2002) Gender and age differences in social support: a study of east german migrants. In: Weidner G, Kopp MS, Kristenson M (eds) Heart disease: environment, stress and gender, edition: NATO science series, series I: life and behavioural sciences, volume: 327. IOS Press, Amsterdam, pp 198–210
Conte KP, Schure MB, Goins RT (2015) Correlates of social support in older American Indians: the native elder care study. Aging Ment Health 19:835–843. https://doi.org/10.1080/13607863.2014.967171
Wilson DK, Kliewer W, Bayer L et al (1999) The influence of gender and emotional versus instrumental support on cardiovascular reactivity in African-American adolescents. Ann Behav Med 21:235–243. https://doi.org/10.1007/BF02884840
Antonucci TC, Ajrouch KJ, Janevic M (1999) Socioeconomic status, social support, age, and health. Ann N Y Acad Sci 896:390–392. https://doi.org/10.1111/j.1749-6632.1999.tb08150.x
Huurre T, Eerola M, Rahkonen O, Aro H (2007) Does social support affect the relationship between socioeconomic status and depression? A longitudinal study from adolescence to adulthood. J Affect Disord 100:55–64. https://doi.org/10.1016/j.jad.2006.09.019
Soman S, Bhat SM, Latha KS, Praharaj SK (2016) Gender differences in perceived social support and stressful life events in depressed patients. East Asian Arch Psychiatry 26:22–29
Letvak S (2002) The importance of social support for rural mental health. Issues Ment Health Nurs 23:249–261. https://doi.org/10.1080/016128402753542992
Deaton A, Dreze J (2002) Poverty and inequality in india: a re-examination. economic and political weekly 37(36):3729–3748. http://www.jstor.org/stable/4412578. Accessed 24 Oct 2020
Rath T, Panigrahi D (2017) Instrumental social support for the rural elderly: study of a rural block a costal district of Odisha. Int J Commun Med Public Health 4:2320. https://doi.org/10.18203/2394-6040.ijcmph20172818
Abe Y, Fujise N, Fukunaga R et al (2012) Comparisons of the prevalence of and risk factors for elderly depression between urban and rural populations in Japan. Int Psychogeriatr 24:1235–1241. https://doi.org/10.1017/S1041610212000099
Kim J-M, Stewart R, Shin I-S et al (2004) Lifetime urban/rural residence, social support and late-life depression in Korea. Int J Geriatr Psychiatry 19:843–851. https://doi.org/10.1002/gps.1175
Katon Wayne J (2011) Epidemiology and treatment of depression in patients with chronic medical illness. Dialog Clin Neurosci 13:7–23
Ford DE (2008) Optimizing outcomes for patients with depression and chronic medical illnesses. Am J Med 121:S38–S44. https://doi.org/10.1016/j.amjmed.2008.09.012
Srinivasan K, Mazur A, Mony PK et al (2018) Improving mental health through integration with primary care in rural Karnataka: study protocol of a cluster randomized control trial. BMC Fam Pract 19:158. https://doi.org/10.1186/s12875-018-0845-z
WHO|Process of translation and adaptation of instruments (2020) In: WHO. https://www.who.int/substance_abuse/research_tools/translation/en/. Accessed 30 Apr 2020
Wills TA, Shinar O (2000) Measuring perceived and received social support. In: Cohen S, Underwood LG, Gottlieb BH (eds) Social support measurement and intervention: a guide for health and social scientists. Oxford University Press, New York, pp 86–135
Tardy CH (1985) Social support measurement. Am J Commun Psychol 13:187–202
Malda M (2009) There is no place like home: on the relation between culture and children’s cognition. Ridderkerk, Ridderprint
The Whoqol Group (1998) Development of the world health organization WHOQOL-BREF quality of life assessment. Psychol Med 28:551–558. https://doi.org/10.1017/S0033291798006667
Durgoji S, Muliyala KP, Jayarajan D, Chaturvedi SK (2019) Quality of life in schizophrenia: what is important for persons with schizophrenia in India? Indian J Psychol Med 41:420–427. https://doi.org/10.4103/IJPSYM.IJPSYM_71_19
Vijayan A, Harshitha SN, Radhakrishnan G (2017) The resilience and quality of life people with mental illness attending psychiatric rehabilitation centre. Indian J Psychiatr Nurs 14:20. https://doi.org/10.4103/2231-1505.262416
Axelsson E, Lindsäter E, Ljótsson B et al (2017) The 12-item Self-Report World Health Organization Disability Assessment Schedule (WHODAS) 2.0 administered via the internet to individuals with anxiety and stress disorders: a psychometric investigation based on data from two clinical trials. JMIR Ment Health 4:4–58. https://doi.org/10.2196/mental.7497
Balhara YPS, Singh S, Modak T, Sarkar S (2017) A cross-sectional study to assess disability and its correlates among treatment seeking individuals with alcohol use disorders. Indian J Psychol Med 39:40. https://doi.org/10.4103/0253-7176.198941
Ramadass S, Rai SK, Gupta SK, Kant S, Wadhwa S, Sood M, Sreenivas V (2018) Prevalence of disability and its association with sociodemographic factors and quality of life in a rural adult population of northern India. Natl Med J India 31:268–273
Kroenke K, Spitzer RL, Williams JBW (2001) The PHQ-9. J Gen Intern Med 16:606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Na PJ, Yaramala SR, Kim JA et al (2018) The PHQ-9 Item 9 based screening for suicide risk: a validation study of the Patient Health Questionnaire (PHQ)-9 Item 9 with the Columbia Suicide Severity Rating Scale (C-SSRS). J Affect Disord 232:34–40. https://doi.org/10.1016/j.jad.2018.02.045
Kochhar PH, Rajadhyaksha SS, Suvarna VR (2007) Translation and validation of brief patient health questionnaire against DSM IV as a tool to diagnose major depressive disorder in Indian patients. J Postgrad Med 53:102. https://doi.org/10.4103/0022-3859.32209
Ingle VK, Pandey I, Singh AR et al (2017) Screening of patients with chronic medical disorders in the outpatient department for depression using handheld computers as interface and patient health questionnaire-9 as a tool. Int J Appl Basic Med Res 7:129. https://doi.org/10.4103/2229-516X.205809
Dutta D, Bharati S, Roy C, Das G (2013) Measurement of prevalence of “major depressive syndrome” among Indian patients attending pain clinic with chronic pain using PHQ-9 scale. J Anaesthesiol Clin Pharmacol 29:76. https://doi.org/10.4103/0970-9185.105808
De S (2011) Prevalence of depression in stable chronic obstructive pulmonary disease. Indian J Chest Dis Allied Sci 53:35–39
Spitzer RL, Kroenke K, Williams JBW, Löwe B (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166:1092–1097. https://doi.org/10.1001/archinte.166.10.1092
Shankar A, Dracham C, Ghoshal S, Grover S (2016) Prevalence of depression and anxiety disorder in cancer patients: an institutional experience. Indian J Cancer 53:432. https://doi.org/10.4103/0019-509X.200651
Rakesh PS, Ramesh R, Rachel P, Chanda R, Satish N, Mohan VR (2012) Quality of life among people with epilepsy: a cross-sectional study from rural southern India. Natl Med J India 25:261–264
Rose GA (1962) The diagnosis of ischaemic heart pain and intermittent claudication in field surveys. Bull World Health Organ 27:645–658
Nakagawa S, Schielzeth H (2013) A general and simple method for obtaining R2 from generalized linear mixed-effects models. Methods Ecol Evol 4:133–142. https://doi.org/10.1111/j.2041-210x.2012.00261.x
Geue K, Götze H, Friedrich M et al (2019) Perceived social support and associations with health-related quality of life in young versus older adult patients with haematological malignancies. Health Qual Life Outcomes 17:145. https://doi.org/10.1186/s12955-019-1202-1
Ohaeri JU (1982) (1998) Perception of the social support role of the extended family network by some Nigerians with schizophrenia and affective disorders. Soc Sci Med 47:1463–1472. https://doi.org/10.1016/s0277-9536(98)00111-7
Heitzman J, Worden RL (1995) India: A Country Study. GPO for the Library of Congress, Washington DC. https://www.loc.gov/item/96019266/. Accessed 8 Jun 2020
Castiglia PT (1999) Extended families: social support systems for children. J Pediatr Health Care 13:139–141. https://doi.org/10.1016/S0891-5245(99)90076-7
Dressler WW (1985) Extended family relationships, social support, and mental health in a Southern Black community. J Health Soc Behav 26:39–48. https://doi.org/10.2307/2136725
Kim HS, Sherman DK, Taylor SE (2008) Culture and social support. Am Psychol 63:518–526. https://doi.org/10.1037/0003-066X
Jiang L, Drolet A, Kim HS (2018) Age and social support seeking: understanding the role of perceived social costs to others. Pers Soc Psychol Bull 44:1104–1116. https://doi.org/10.1177/0146167218760798
Aquino JA, Russell DW, Cutrona CE, Altmaier EM (1996) Employment status, social support, and life satisfaction among the elderly. J Couns Psychol 43:480–489. https://doi.org/10.1037/0022-0167.43.4.480
Cimarolli VR, Wang S (2006) Differences in social support among employed and unemployed adults who are visually impaired. J Vis Impair Blind 100:545–556. https://doi.org/10.1177/0145482X0610000906
Sinha S (2017) Multiple roles of working women and psychological well-being. Ind Psychiatry J 26:171. https://doi.org/10.4103/ipj.ipj_70_16
Asnani V, Pandey UD, Sawhney M (2004) Social support and occupational health of working women. J Health Manag 6:129–139. https://doi.org/10.1177/097206340400600204
Wang J, Xue J, Jiang Y et al (2020) Mediating effects of depressive symptoms on social support and quality of life among rural older Chinese. Health Qual Life Outcomes 18:242. https://doi.org/10.1186/s12955-020-01490-1
Liao J, Brunner EJ (2016) Structural and functional measures of social relationships and quality of life among older adults: does chronic disease status matter? Qual Life Res 25:153–164. https://doi.org/10.1007/s11136-015-1052-1
Helgeson VS (2003) Social support and quality of life. Qual Life Res Int J Qual Life Asp Treat Care Rehabil 12(Suppl 1):25–31
Patel SA, Dhillon PK, Kondal D et al (2017) Chronic disease concordance within Indian households: a cross-sectional study. PLOS Med 14:e1002395. https://doi.org/10.1371/journal.pmed.1002395
Mohd TAMT, Yunus RM, Hairi F et al (2019) Social support and depression among community dwelling older adults in Asia: a systematic review. BMJ Open 9:e026667. https://doi.org/10.1136/bmjopen-2018-026667
Acknowledgements
We thank the National Institute of Mental Health USA for grant support (R01 MH100311) and the Government of Karnataka, Directorate of Health and Family Welfare Service for the permission to conduct this study.
Funding
This work was supported by the US National Institute of Mental Health [R01MH100311].
Author information
Authors and Affiliations
Contributions
KS and MLE conceived of and designed the study. Statistical analyses were performed by ST and EH. The first draft of the manuscript was written by ST and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest.
Ethics approval
Ethics approval was obtained from the Institutional Ethics Committee at St. John’s National Academy of Health Sciences (reference 38/2013) and Committee on Human Research, University of California, San Francisco (reference 125,781).
Informed consent
Informed consent to participate in the study was taken from all participants. Information about the study was given verbally and in written form. Participants were informed that participation is voluntary, there are no negative consequences for refusing to participate, and that consent can be withdrawn at any time during the study without any repercussions. Interested participants provided written consent. Illiterate participants had an option of providing verbal consent or a thumb print and a witness, unaffiliated with the study, also signed the consent form.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Thomas, S., Srinivasan, K., Heylen, E. et al. Correlates of social support in individuals with a diagnosis of common mental disorders and non communicable medical diseases in rural South India. Soc Psychiatry Psychiatr Epidemiol 56, 1623–1631 (2021). https://doi.org/10.1007/s00127-020-01997-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-020-01997-4