Abstract
Aims/hypothesis
The age-specific associations between type 2 diabetes and cancer risk are not fully understood. The aim of this study was to assess how age at diagnosis modifies the associations between type 2 diabetes and cancer risk.
Methods
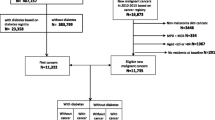
We used data from the Yinzhou Health Information System, and included 42,279 individuals who were newly diagnosed with type 2 diabetes between 2010 and 2014, as well as 166,010 age- and sex-matched control individuals without diabetes who were selected randomly from the electronic health records of the entire population. Patients were divided into four age groups according to age at diagnosis: <50, 50–59, 60–69 and ≥70 years. Stratified Cox proportional hazards regression models, with age as the time scale, were used to estimate the HRs and 95% CIs for the associations of type 2 diabetes with the risks of overall and site-specific cancers. Population-attributable fractions were also calculated for outcomes associated with type 2 diabetes.
Results
During median follow-up periods of 9.20 and 9.32 years, we identified 15,729 incident cancer cases and 5383 cancer deaths, respectively. Patients diagnosed with type 2 diabetes before 50 years of age had the highest relative risks of cancer incidence and mortality, with HRs (95% CI) of 1.35 (1.20, 1.52) for overall cancer incidence, 1.39 (1.11, 1.73) for gastrointestinal cancer incidence, 2.02 (1.50, 2.71) for overall cancer mortality, and 2.82 (1.91, 4.18) for gastrointestinal cancer mortality. Risk estimates decreased gradually with each decade increase in diagnostic age. The population-attributable fractions for overall cancer and gastrointestinal cancer mortality also decreased with increasing age.
Conclusions/interpretation
The associations of type 2 diabetes with cancer incidence and mortality varied by age at diagnosis, with a higher relative risk among patients who were diagnosed at a younger age.
Graphical Abstract




Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are not publicly available due to privacy protection for patients, but are available from the corresponding authors on reasonable request.
Funding
This work was supported by the National Natural Science Foundation of China (grant number 82173587) and the Ningbo Major Science and Technology Task Project (grant number 2021Z054).
Abbreviations
- PAF:
-
Population-attributable fraction
References
Ali MK, Pearson-Stuttard J, Selvin E, Gregg EW (2022) Interpreting global trends in type 2 diabetes complications and mortality. Diabetologia 65(1):3–13. https://doi.org/10.1007/s00125-021-05585-2
Zheng Y, Ley SH, Hu FB (2018) Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nat Rev Endocrinol 14(2):88–98. https://doi.org/10.1038/nrendo.2017.151
Tomic D, Shaw JE, Magliano DJ (2022) The burden and risks of emerging complications of diabetes mellitus. Nat Rev Endocrinol 18(9):525–539. https://doi.org/10.1038/s41574-022-00690-7
Ma RCW (2018) Epidemiology of diabetes and diabetic complications in China. Diabetologia 61(6):1249–1260. https://doi.org/10.1007/s00125-018-4557-7
Pearson-Stuttard J, Bennett J, Cheng YJ et al (2021) Trends in predominant causes of death in individuals with and without diabetes in England from 2001 to 2018: an epidemiological analysis of linked primary care records. Lancet Diabetes Endocrinol 9(3):165–173. https://doi.org/10.1016/S2213-8587(20)30431-9
Peila R, Rohan TE (2020) Diabetes, glycated hemoglobin, and risk of cancer in the UK Biobank study. Cancer Epidemiol Biomarkers Prev 29(6):1107–1119. https://doi.org/10.1158/1055-9965.EPI-19-1623
Hu Y, Zhang X, Ma Y et al (2021) Incident type 2 diabetes duration and cancer risk: a prospective study in two US cohorts. J Natl Cancer Inst 113(4):381–389. https://doi.org/10.1093/jnci/djaa141
Bragg F, Holmes MV, Iona A et al (2017) Association between diabetes and cause-specific mortality in rural and urban areas of China. JAMA 317(3):280–289. https://doi.org/10.1001/jama.2016.19720
Pan X-F, He M, Yu C et al (2018) Type 2 diabetes and risk of incident cancer in China: a prospective study among 0.5 million Chinese adults. Am J Epidemiol 187(7):1380–1391. https://doi.org/10.1093/aje/kwx376
Magliano DJ, Sacre JW, Harding JL, Gregg EW, Zimmet PZ, Shaw JE (2020) Young-onset type 2 diabetes mellitus – implications for morbidity and mortality. Nat Rev Endocrinol 16(6):321–331. https://doi.org/10.1038/s41574-020-0334-z
Yeung RO, Zhang Y, Luk A et al (2014) Metabolic profiles and treatment gaps in young-onset type 2 diabetes in Asia (the JADE programme): a cross-sectional study of a prospective cohort. Lancet Diabetes Endocrinol 2(12):935–943. https://doi.org/10.1016/S2213-8587(14)70137-8
Sattar N, Rawshani A, Franzén S et al (2019) Age at diagnosis of type 2 diabetes mellitus and associations with cardiovascular and mortality risks. Circulation 139(19):2228–2237. https://doi.org/10.1161/CIRCULATIONAHA.118.037885
Zhao M, Song L, Sun L et al (2021) Associations of type 2 diabetes onset age with cardiovascular disease and mortality: the Kailuan study. Diabetes Care 44(6):1426–1432. https://doi.org/10.2337/dc20-2375
Lin H, Tang X, Shen P et al (2018) Using big data to improve cardiovascular care and outcomes in China: a protocol for the CHinese Electronic health Records Research in Yinzhou (CHERRY) Study. BMJ Open 8(2):e019698. https://doi.org/10.1136/bmjopen-2017-019698
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 15(7):539–553. https://doi.org/10.1002/(SICI)1096-9136(199807)15:7%3c539::AID-DIA668%3e3.0.CO;2-S
Chen C, Lu FC (2004) The guidelines for prevention and control of overweight and obesity in Chinese adults. Biomed Environ Sci 17(Suppl):1–36
Cao M, Li H, Sun D, Chen W (2020) Cancer burden of major cancers in China: a need for sustainable actions. Cancer Commun (Lond) 40(5):205–210. https://doi.org/10.1002/cac2.12025
Fiolet T, Srour B, Sellem L et al (2018) Consumption of ultra-processed foods and cancer risk: results from NutriNet-Santé prospective cohort. BMJ 360:k322. https://doi.org/10.1136/bmj.k322
Cologne J, Hsu W-L, Abbott RD et al (2012) Proportional hazards regression in epidemiologic follow-up studies: an intuitive consideration of primary time scale. Epidemiology 23(4):565–573. https://doi.org/10.1097/EDE.0b013e318253e418
Shinozaki T, Mansournia MA, Matsuyama Y (2017) On hazard ratio estimators by proportional hazards models in matched-pair cohort studies. Emerg Themes Epidemiol 14:6. https://doi.org/10.1186/s12982-017-0060-8
Grambsch PM, Therneau TM (1994) Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 81(3):515–526. https://doi.org/10.1093/biomet/81.3.515%JBiometrika
Mehta NK, Zheng H, Myrskylä M (2019) How do age and major risk factors for mortality interact over the life-course? Implications for health disparities research and public health policy. SSM Popul Health 8:100438. https://doi.org/10.1016/j.ssmph.2019.100438
Rod NH, Lange T, Andersen I, Marott JL, Diderichsen F (2012) Additive interaction in survival analysis: use of the additive hazards model. Epidemiology 23(5):733–737. https://doi.org/10.1097/EDE.0b013e31825fa218
Zapata-Diomedi B, Barendregt JJ, Veerman JL (2018) Population attributable fraction: names, types and issues with incorrect interpretation of relative risks. Br J Sports Med 52(4):212–213. https://doi.org/10.1136/bjsports-2015-095531
Levin ML (1953) The occurrence of lung cancer in man. Acta Unio Int Contra Cancrum 9(3):531–541
Wang L, Peng W, Zhao Z et al (2021) Prevalence and treatment of diabetes in China, 2013–2018. JAMA 326(24):2498–2506. https://doi.org/10.1001/jama.2021.22208
Johnson JA, Carstensen B, Witte D, Bowker SL, Lipscombe L, Renehan AG (2012) Diabetes and cancer (1): evaluating the temporal relationship between type 2 diabetes and cancer incidence. Diabetologia 55(6):1607–1618. https://doi.org/10.1007/s00125-012-2525-1
Johnson JA, Bowker SL, Richardson K, Marra CA (2011) Time-varying incidence of cancer after the onset of type 2 diabetes: evidence of potential detection bias. Diabetologia 54(9):2263–2271. https://doi.org/10.1007/s00125-011-2242-1
Ha ID, Jeong J-H, Lee Y (2017) Competing risks frailty models. In: Ha ID, Jeong J-H, Lee Y (eds) Statistical modelling of survival data with random effects: H-likelihood approach. Springer, Singapore, pp 125–171
Goto A, Yamaji T, Sawada N et al (2020) Diabetes and cancer risk: a Mendelian randomization study. Int J Cancer 146(3):712–719. https://doi.org/10.1002/ijc.32310
Yuan S, Kar S, Carter P et al (2020) Is type 2 diabetes causally associated with cancer risk? Evidence from a two-sample Mendelian randomization study. Diabetes 69(7):1588–1596. https://doi.org/10.2337/db20-0084
Lascar N, Brown J, Pattison H, Barnett AH, Bailey CJ, Bellary S (2018) Type 2 diabetes in adolescents and young adults. Lancet Diabetes Endocrinol 6(1):69–80. https://doi.org/10.1016/S2213-8587(17)30186-9
Saisho Y (2015) β-cell dysfunction: its critical role in prevention and management of type 2 diabetes. World J Diabetes 6(1):109–124. https://doi.org/10.4239/wjd.v6.i1.109
Hodge A (2017) Is there an association between β-cell function and cancer risk? eBioMedicine 22:24–25. https://doi.org/10.1016/j.ebiom.2017.07.006
Steinarsson AO, Rawshani A, Gudbjörnsdottir S, Franzén S, Svensson A-M, Sattar N (2018) Short-term progression of cardiometabolic risk factors in relation to age at type 2 diabetes diagnosis: a longitudinal observational study of 100,606 individuals from the Swedish National Diabetes Register. Diabetologia 61(3):599–606. https://doi.org/10.1007/s00125-017-4532-8
Browne JL, Nefs G, Pouwer F, Speight J (2015) Depression, anxiety and self-care behaviours of young adults with type 2 diabetes: results from the International Diabetes Management and Impact for Long-term Empowerment and Success (MILES) study. Diabet Med 32(1):133–140. https://doi.org/10.1111/dme.12566
American Diabetes Association Professional Practice Committee (2022) 2. Classification and diagnosis of diabetes: standards of medical care in diabetes – 2022. Diabetes Care 45(Suppl 1):S17–S38. https://doi.org/10.2337/dc22-S002
Aguilar-Salinas CA, Reyes-Rodríguez E, Ordóñez-Sánchez ML et al (2001) Early-onset type 2 diabetes: metabolic and genetic characterization in the Mexican population. J Clin Endocrinol Metab 86(1):220–226. https://doi.org/10.1210/jcem.86.1.7134
McCormack VA, Boffetta P (2011) Today’s lifestyles, tomorrow’s cancers: trends in lifestyle risk factors for cancer in low- and middle-income countries. Ann Oncol 22(11):2349–2357. https://doi.org/10.1093/annonc/mdq763
Acknowledgements
We would like to thank all staff of the Department of Chronic Disease and Health Promotion, Yinzhou District Center for Disease Control and Prevention, for data collection.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
ZY, YS, JW and KC contributed to the study concept and design. ZY, YW and LX drafted the manuscript. ZZ, TL, LY, KG and XZ performed data cleansing and statistical analysis. PS, HL, LS, MT and MJ supervised the study. All authors contributed to interpretation of the results and critical revision of the manuscript for important intellectual content, and approved the final version of the manuscript. YS, JW and KC are the guarantors of this work, and, as such, had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, Z., Wu, Y., Xu, L. et al. Age at diagnosis modifies associations of type 2 diabetes with cancer incidence and mortality: a retrospective matched-cohort study. Diabetologia 66, 1450–1459 (2023). https://doi.org/10.1007/s00125-023-05920-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-023-05920-9