Abstract
Aims/hypothesis
Recent studies suggest that photoreceptor cells produce mediators or products that contribute to retinal capillary damage in diabetes. The purpose of this study was to determine if photoreceptor cells release soluble factors that contribute to retinal vascular permeability in diabetes.
Methods
To assess retinal vascular leakage, a streptozotocin-induced mouse model of diabetes, with hyperglycaemia for 8 months, and age-matched control mice, were injected with FITC-BSA. Fluorescence microscopy was used to detect leakage of FITC-BSA from the retinal vasculature into the neural retina. Ex vivo and in vitro experiments were performed to determine if photoreceptor cells released products that directly increased retinal endothelial cell permeability or cell death. Effects of products released by photoreceptors on tight junction and cell adhesion proteins were assessed by quantitative reverse transcription PCR (qRT-PCR). Inflammatory products released by photoreceptors into media were measured using protein arrays.
Results
Eight months duration of diabetes increased retinal vascular permeability in wild-type mice, but this defect was inhibited in opsin-deficient diabetic mice in which photoreceptor cells had degenerated earlier. Photoreceptor cells from diabetic wild-type mice released inflammatory products (e.g. IL-1α, IL-1β, IL-6, IL-12, chemokine C-X-C motif ligand 1 [CXCL1], monocyte chemoattractant protein 1 [MCP-1], CXCL12a, I-309, chemokine ligand 25 [CCL25] and TNF-α), which directly contributed to increased retinal endothelial cell permeability, at least in part via changes in claudin (tight junction) mRNA. Products released from photoreceptor cells from diabetic mice or under diabetes-like conditions did not directly kill retinal endothelial cells in vitro.
Conclusions/interpretation
Photoreceptor cells can produce inflammatory products that contribute to retinal vascular permeability in mouse models of diabetes.
Similar content being viewed by others
Introduction
Diabetic retinopathy is a leading cause of visual impairment and blindness in people aged 24–64 years old, and it affects over 60% of individuals who have had diabetes for ≥10 years [1, 2]. Many studies of the pathogenesis of diabetic retinopathy have focused on vascular abnormalities, because diabetes-induced abnormalities of the retinal vasculature (i.e. increased permeability and degeneration) have been directly implicated in visual loss and impairment. Nevertheless, alterations in the neural retina (including photoreceptor cells) also have been detected, and recent studies have demonstrated that molecular abnormalities that develop in photoreceptor cells can contribute to retinal vascular damage and early characteristics of diabetic retinopathy [3,4,5,6].
Photoreceptor cells not only regulate the increase in inflammatory proteins in the retina in diabetes [3, 6], but are themselves a source of inflammatory proteins [4, 7]. Increased production of inflammatory proteins in diabetic retinopathy is important because the development of vascular lesions characteristic of diabetic retinopathy are inhibited when the production of proinflammatory proteins are inhibited [8,9,10]. Moreover, photoreceptors in diabetes or diabetes-like conditions produce inflammatory products that can stimulate nearby cells, such as circulating leucocytes, retinal endothelial cells and glial cells [4, 5]. Photoreceptor cells have been shown to stimulate leucocyte-mediated killing of retinal endothelial cells in diabetes [4, 5, 11,12,13], potentially contributing to diabetes-induced degeneration of retinal capillaries. Whether photoreceptor cells contribute to diabetes-induced retinal vascular permeability has not been investigated to date.
Breakdown of the blood–retinal barrier (BRB) (i.e. retinal vascular permeability) is characteristic of diabetic retinopathy in both human and experimental diabetes [14,15,16,17,18,19,20,21,22,23]. The BRB is comprised of endothelial proteins that contribute to tight junctions (e.g. claudin) and cell adhesion (e.g. vascular endothelial [VE] cadherin), thereby regulating the passage of solutes and other molecules from the blood into the neural retina and vice versa [17, 24]. It has been shown that diabetes leads to reduced levels of endothelial tight junction proteins, thereby increasing retinal vascular permeability [14, 18]. In the present study, we investigated the possibility that photoreceptor cells contribute to retinal vascular permeability in mouse models of diabetes, and release inflammatory products that can directly increase retinal endothelial cell permeability and death.
Methods
Experimental animals
Rhodopsin knockout (Rho −/−) mice on C57BL/6J background and wild-type C57BL/6J mice were obtained from J. Lem (Tufts University, Boston, MA, USA) and Jackson Laboratory (Bar Harbor, ME, USA), respectively. In the Rho −/− mice, the rod opsin that forms rhodopsin was knocked out. The Rho −/− mice were from the same line as that studied previously by our group and de Gooyer et al [3,4,5,6, 25]. The Rho −/− mice display a retinitis pigmentosa-like phenotype with progressive, age-dependent decline in rod cell number and function [26], and the electroretinogram response is absent at 48 days of age [5, 26]. In Rho −/− animals, the thickness of all the retinal regions (except the outer nuclear layer [ONL]) does not change compared with wild-type animals (see electronic supplementary material [ESM] Fig. 1).
Male mice (2 months old) were randomly assigned to the ‘diabetic’ or ‘non-diabetic control’ groups. Mice in the diabetic group were given five sequential daily i.p. injections of a freshly prepared solution of streptozotocin in citrate buffer (pH 4.5) at 60 mg/kg of body weight. Hyperglycaemia was verified at least three times during the second week after streptozotocin administration. Mice having three consecutive measurements of blood glucose >15.26 mmol/l were classified as diabetic. Insulin was given as needed to prevent weight loss without preventing hyperglycaemia and glucosuria (0–0.2 units of NPH insulin s.c., 0–3 times per week). Food consumption (7004 diet; Harlan Teklad, Indianapolis, IN, USA) and body weight were measured weekly. Treatment of animals conformed to the Association for Research in Vision and Ophthalmology Resolution on Treatment of Animals in Research, as well as to the Case Western Reserve University Institutional Animal Care and Use Committee. At 2 and 8 months of diabetes (4 and 10 months of age, respectively), animals were euthanised and eyes were enucleated.
Leakage of albumin into neural retina
Accumulation of the blood albumin protein in the neural retina has been viewed as a marker of increased vascular permeability [14, 19, 20]. At 8 months of diabetes, sterile FITC-BSA (50 μg/μl) in phosphate-buffered saline (0.138 mol/l NaCl, 0.0027 mol/l KCl [pH 7.4]) was injected into the tail veins of mice at 100 μg/g. After 20 min, mice were euthanised, blood was collected from the heart using heparinised tubes, and their eyes were collected, fixed in ice-cold 4% paraformaldehyde, cryopreserved with sucrose and then frozen in optimal cutting temperature (OCT) compound in isopentane on dry ice. Blood from the heart was centrifuged at 18,000 g for 20 min and FITC fluorescence in the plasma was measured using 2030 Multilabel Reader VICTORTM X3 (PerkinElmer, Waltham, MA, USA). Retinal cryosections (three sections per animal at 11 μm thickness) were cut, imaged at 20× objective and analysed by fluorescence microscopy. FITC fluorescence in each retinal section was analysed using NIS-Elements AR Analysis 3.2 64-bit software (www.nikoninstruments.com/Products/Software/NIS-Elements-Advanced-Research). Light intensity and duration of exposure were kept equal in all retinal images. Leakage of albumin into the neural retina was estimated from measurements of FITC-BSA in the outer plexiform layer (OPL), inner nuclear layer (INL) and inner plexiform layer (IPL) by computer-assisted microscopy as reported previously [19, 20]. Fluorescence from the blood vessels were selected and excluded from the analysis in order to effectively measure how much FITC-BSA had leaked into the neural retina. Background fluorescence (i.e. fluorescence from outside the retina) was subtracted from the FITC fluorescence from the neural retina. Vascular permeability in diabetes is expressed as the ratio of FITC fluorescence intensity in the neural retina divided by that in the plasma, and this is normalised to the fluorescence intensity from non-diabetic animals.
Vibratome isolation of photoreceptor cells from mouse retina
We used a vibratome (Leica VT1000 S) to bisect fresh unfixed retina into outer (photoreceptor layer) and inner retina as previously described [4, 27]. Retinas from 2 months diabetic wild-type mice were bisected because molecular abnormalities (e.g. increase in inflammatory proteins and oxidative stress) in photoreceptors were increased after 2 months of diabetes in mice [3, 4]. Cells of haematopoietic lineage (e.g. microglia and leucocytes) are unlikely to be present in the sectioned photoreceptor sheets (at this age and duration of diabetes) because, as previously reported, CD45+ cells are not present in the outer retina in diabetes but are present in the inner retina [4]. In addition, we reported that about 79% of the photoreceptor layer (i.e. inner and outer segments and ONL) were sectioned from the retina using the vibratome method [4]. Therefore, it is very unlikely that the isolated photoreceptor sheet was contaminated with cells predominantly present in the inner retina. Isolated sheets of photoreceptor cells from mice diabetic for 2 months were incubated in 30 mmol/l glucose in DMEM, and photoreceptor sheets from age-matched non-diabetic mice were incubated in 5 mmol/l glucose in DMEM for 14–16 h to approximate the glucose environment they had been exposed to in vivo. Relatively equal amounts of photoreceptor sheets were isolated from diabetic and non-diabetic mouse retinas because previous evidence showed no statistically significant change in photoreceptor degeneration in diabetes [5] (ESM Fig. 1). To test for endothelial cell permeability, conditioned medium from photoreceptor sheets was harvested, mixed with 0.02 g of FITC-albumin and transferred undiluted onto mouse retinal endothelial cells (cultured to 100% confluence) grown on the permeable upper chamber of transwell plates (6.5 mm insert, 0.4 μm polycarbonate membrane; Corning Costar, Kennebunk, ME, USA) for 24 h. After this interval, FITC fluorescence that had passed through the confluent endothelial cells into the lower chamber was quantified with a PerkinElmer 2030 MultiLabel Fluorescence Reader. RNA from these retinal endothelial cells was then isolated for quantitative reverse transcription PCR (qRT-PCR) analysis.
Cell death
We tested for cell death of freshly isolated photoreceptor cells incubated in media for 45 min compared with 15 h by using two different measures of cell death: lactate dehydrogenase release (assay kit by Pierce Biotechnology, Rockford, IL, USA) and Trypan Blue exclusion assay.
RNA isolation and qRT-PCR
Total RNA was isolated from cells (RNeasy kit, Qiagen, MD, USA). cDNA was synthesised (iScript, cDNA synthesis kit, Bio-Rad, USA) in a final reaction volume of 20 μl. Real-time PCR was performed using SYBR green (Roche Diagnostics, Indianapolis, IN, USA) with a qPCR system (CFX Connect Real-Time PCR Detection System, Bio-Rad, Hercules, CA, USA). The following primer sequences were used for 18S forward (5′-ACTCAACACGGGAAACCTCACC-3′) and reverse (5′-CCAGACAAATCGCTCCACCAAC-3′), claudin forward (5′-CTGGGTTTCATCCTGGCTTC-3′) and reverse (5′-TTGATGGGGGTCAAGGGGTC-3′), VE cadherin forward (5′-AGAAGCTATGTCGGCAGGAA-3′) and reverse (5′-GCTCTGCATGTTTGGTCTCA-3′). 18S was used as the reference for normalisation. cDNA samples were run in duplicates. PCR products were confirmed by agarose gel electrophoresis and melting temperature. \( {2}^{\varDelta \varDelta {\mathrm{C}}_{\mathrm{q}}} \) = fold change in gene expression.
Cell culture
The following cell lines were grown in DMEM containing 5 mmol/l glucose and 10% fetal bovine serum: 661W photoreceptor-like cells (our group previously confirmed 661W identity by positive identification of cone opsin mRNA [20]) and mouse retinal endothelial cells (identity of endothelial cells was previously confirmed by us by positive identification of the PECAM1 gene [4]). The retinal endothelial cells were kindly provided by N. Sheibani (University of Wisconsin, Madison, WI, USA) and were originally isolated from Immortomice [28]. 661W cells (200,000 cells) were cultured in 5 mmol/l glucose (normal glucose) and 30 mmol/l glucose (high glucose) in 12-well plates for 40–48 h. Conditioned medium from 661W photoreceptor cells was harvested and added undiluted to 200,000 mouse retinal endothelial cells in 12-well plates for 24 h. For cell viability, endothelial cells were harvested and determination of Trypan Blue exclusion was conducted. Cell viability was calculated by using the formula: (alive)/(alive + dead) × 100%.
Protein array
Isolated sheets of photoreceptor cells (generated from vibratome isolation as described above) from 2 months old diabetic mice were incubated in 30 mmol/l glucose in DMEM, and photoreceptor sheets from age-matched non-diabetic mice were incubated in 5 mmol/l glucose in DMEM for 14–16 h. Conditioned medium was harvested and subjected to inflammation protein array analysis using Ray Biotech Mouse Inflammation Array C1 kit (Norcross, GA, USA) and following the manufacturer’s instructions.
ELISA
Protein concentrations of TNF-α and IL-1β released by photoreceptor sheets from mice diabetic for 2 months and age-matched non-diabetic mice were measured in their respective conditioned medium with mouse ELISA kits (Biolegend, San Diego, CA, USA). Based on results of TNF-α and IL-1β released by photoreceptor sheets, identical concentrations of TNF-α and IL-1β mouse recombinant protein (Biolegend) were added to retinal endothelial cells in transwell inserts for 24 h and permeability was estimated as described above.
Statistical analysis
Because of the small number of animals, data were analysed using Mann–Whitney (non-parametric test). For the convenience of readers, data are graphically provided as mean ± SEM. Differences were considered statistically significant at p < 0.05.
Results
At 10 months of age, essentially all photoreceptor cells were missing in Rho −/− mice (ESM Fig. 1) [5]. Diabetes of 8 months duration did not significantly affect the thickness of any retinal layers in either wild-type or Rho −/− animals (ESM Fig. 1) [5].
Photoreceptor cells contribute to retinal vascular permeability in diabetes
At 8 months of diabetes, leakage of FITC-BSA from the retinal vasculature into the neural retina was evaluated in wild-type control animals and Rho −/− animals in which photoreceptors had degenerated. Diabetes gave rise to statistically significant increases in permeability in the OPL, INL and IPL in retinas of wild-type mice (Fig. 1a–e). Diabetic Rho −/−animals (in which photoreceptor cells had degenerated due to opsin deficiency) were partially protected from this defect. In the Rho −/−animals, diabetes did not alter the permeability in the OPL or INL (Fig. 1a, f, g), although permeability of retinal vessels within the IPL was still increased. Because photoreceptor cells had totally degenerated in these Rho −/−mice (Fig. 1f, g), this result is consistent with the postulate that photoreceptor cells contribute to retinal vascular permeability in diabetes (at least in the OPL and INL).
Retinal vascular permeability is inhibited in diabetic mice in which photoreceptor cells had degenerated due to opsin deficiency. (a) Fluorescence of FITC-BSA was increased in all retinal layers of diabetic wild-type mice. However, when photoreceptors were completely degenerated in diabetic animals lacking photoreceptors due to opsin deficiency (Rho −/−) the diabetes-induced increase in fluorescence of FITC-BSA in part of the retina (OPL and INL) was inhibited. By contrast, fluorescence of FITC-BSA in the IPL was significantly greater than normal in Rho −/− mice. White bars, non-diabetic animals; black bars, diabetic animals; grey bars, diabetic Rho −/−animals. (b–g) show retinal images for non-diabetic (b, c), diabetic (d, e) and diabetic Rho −/− (f, g) animals, respectively. Blue, nuclei stained with Hoechst DNA dye; green, FITC-BSA. n = 4–5 animals per group were used in the analysis. Duration of diabetes was 8 months and mice were 10 months of age when killed. Scale bars: 0.14 mm. **p < 0.01
To help establish how photoreceptors contribute to vascular permeability in diabetes, we also conducted ex vivo and in vitro studies.
Soluble products released by photoreceptor cells in diabetes can directly cause increased retinal endothelial cell permeability
We tested whether photoreceptors from diabetic mice release soluble products that can directly increase retinal endothelial cell permeability in vitro. Conditioned media from freshly isolated sheets of photoreceptor cells (generated via vibratome isolation [4, 27]) from non-diabetic and diabetic mice were mixed with FITC-albumin and added to mouse retinal endothelial cells in upper chambers of transwell plates for 24 h. Retinal endothelial cells incubated with conditioned media from photoreceptors of diabetic mice showed a statistically significant increase in permeability of FITC-albumin as compared with endothelial cells incubated with conditioned media from photoreceptors of non-diabetic mice (Fig. 2a). This increase in permeability was not due to the direct influence of elevated glucose concentration on endothelial cells because endothelial cells incubated in high glucose alone (without previous exposure to photoreceptors) showed no detectable change in permeability compared with endothelial cells incubated in normal glucose (Fig. 2a). During the in vitro incubation, we found little or no death of photoreceptor cells (ESM Fig. 2), but we acknowledge the possibility that products released as a result of the in vitro incubation might have contributed to the increased endothelial cell permeability detected.
Products released from isolated photoreceptor sheets from diabetic mice can directly increase retinal endothelial cell permeability. (a) Retinal endothelial cells incubated with conditioned media from photoreceptor sheets of mice diabetic for 2 months exhibited increased permeability of FITC-albumin compared with endothelial cells incubated with conditioned media from photoreceptors from age-matched non-diabetic mice. Retinal endothelial cells incubated with 30 mmol/l glucose alone did not manifest increased endothelial cell permeability compared with endothelial cells incubated with 5 mmol/l glucose. Retinal endothelial cells incubated with conditioned media from photoreceptors of diabetic mice showed decreased (b) claudin and (c) VE cadherin mRNA levels compared with endothelial cells incubated with conditioned media from photoreceptors of non-diabetic mice. Retinal endothelial cells incubated in 30 mmol/l glucose alone exhibited (b) no change in claudin mRNA levels, but (c) a decrease in VE cadherin mRNA when compared with endothelial cells incubated in 5 mmol/l glucose. CM, conditioned media; D, diabetic; N, non-diabetic; PR, photoreceptor; –, not present. n = 5 animals per group were used in the analysis. Duration of diabetes was 2 months and mice were 4 months of age when killed. *p < 0.05
mRNA from retinal endothelial cells in transwell plates was harvested and qRT-PCR was carried out to evaluate potential changes in genes that regulate endothelial cell permeability. Retinal endothelial cells incubated with conditioned media from photoreceptors of diabetic mice had about a 50% reduction in claudin and VE cadherin gene expression as compared with endothelial cells incubated with conditioned media from photoreceptors from non-diabetic mice (Fig. 2b, c). When retinal endothelial cells were incubated with high glucose alone, there was no change in claudin gene expression, whereas VE cadherin gene expression decreased (Fig. 2b, c).
These results demonstrate that photoreceptor cells from diabetic animals release products that directly increase retinal endothelial cell permeability. Because endothelial cell viability could affect the passage of FITC-albumin between endothelial cells, we tested if products released by photoreceptor cells caused the death of endothelial cells.
Products released by photoreceptor cells in diabetes or diabetes-like conditions do not directly kill retinal endothelial cells
Conditioned media from photoreceptors of diabetic and non-diabetic mice were incubated with retinal endothelial cells for 24 h and then the viability of the endothelial cells was evaluated with a Trypan Blue exclusion assay. Retinal endothelial cells incubated with conditioned media from photoreceptors of diabetic mice or high glucose exhibited no change in cell viability compared with endothelial cells incubated in conditioned media from photoreceptors of non-diabetic mice or normal glucose (Fig. 3a, b).
Products released from (a) isolated photoreceptor sheets or (b) 661W cells (photoreceptor-like cells) in diabetes or diabetes-like conditions, respectively, do not directly kill retinal endothelial cells during 24 h incubation. Retinal endothelial cells incubated with conditioned media from (a) isolated photoreceptor sheets from diabetic mice or (b) 661W photoreceptor-like cells in 30 mmol/l glucose resulted in no change in endothelial cell viability. (a, b) Retinal endothelial cells incubated in 30 mmol/l glucose also exhibited no change in cell viability compared with endothelial cells incubated in 5 mmol/l. CM, conditioned media; D, diabetic; N, non-diabetic; PR, photoreceptor; +, present; –, not present. n = 4 animals per group for (a) and n = 4–5 replicates for (b). Duration of diabetes was 2 months and mice were 4 months of age when killed
Conditioned media collected from 661W (photoreceptor-like) cells incubated in high glucose gave similar results. Retinal endothelial cells incubated for 24 h with conditioned media from 661W cells in high glucose resulted in no change in endothelial cell viability compared with endothelial cells incubated with conditioned media from 661W cells in normal glucose (Fig. 3b).
These results demonstrate that products released from photoreceptors in diabetes or diabetes-like conditions do not directly kill retinal endothelial cells, at least within the tested period of 24 h. Because no change in retinal endothelial cell viability was detected in our experiments, the effect of the photoreceptor conditioned media that we detected on retinal endothelial cell permeability (Fig. 2) was not due to endothelial cell death.
Photoreceptor cells release cytokines and inflammatory products in diabetes
The products released by isolated photoreceptor sheets from 2 months diabetic and age-matched non-diabetic mice were evaluated with protein arrays that detect inflammatory proteins. Photoreceptors from diabetic mice released increased amounts of IL-1α, IL-1β, IL-6, IL-12, chemokine C-X-C motif ligand 1 (CXCL1), monocyte chemoattractant protein 1 (MCP-1), CXCL12a, I-309, chemokine ligand25 (CCL25) and TNF-α proteins compared with photoreceptors from non-diabetic mice (Fig. 4). Although IL-6 and IL-12 protein levels also tended to increase, the increase was not statistically significant (Fig. 4).
Photoreceptor cells release cytokines and inflammatory products in diabetes. (a) Photoreceptor sheets from diabetic mice released significantly more IL-1α, IL-1β, IL-6, IL-12, CXCL1, MCP-1, CXCL12a, I-309, CCL25 and TNF-α than photoreceptors from non-diabetic mice. Data are presented as the percent increase of proteins in the diabetic animals above the non-diabetic animals. (b) and (c) show respective blots of released proteins from photoreceptor sheets of non-diabetic and diabetic mice. Blot maps can be found from RayBiotech Mouse Inflammation Array C1. N, non-diabetic. n = 3 animals for non-diabetic groups and n = 4 animals for diabetic groups. Duration of diabetes was 2 months and mice were 4 months of age when killed. *p < 0.05
IL-1β released by photoreceptor cells in diabetes can directly increase retinal endothelial cell permeability
We focused on TNF-α and IL-1β because they had been reported previously to directly cause increased endothelial cell permeability [29,30,31,32,33]. We quantified the concentration of IL-1β and TNF-α proteins released by photoreceptor cells in diabetes by immunoassay and then tested if pure (commercially available) forms of the same cytokines could directly increase retinal endothelial cell permeability.
ELISA was performed to detect the exact concentrations of TNF-α and IL-1β released by photoreceptor cells from mice diabetic for 2 months (4 months of age) or age-matched non-diabetic control mice. Isolated photoreceptor sheets from diabetic mice released greater than normal amounts of IL-1β and TNF-α compared with those of non-diabetic mice (Fig. 5a, b).
Concentrations of IL-1β released by photoreceptor cells in diabetes can directly increase retinal endothelial cell permeability. ELISA was performed to detect the protein amounts released by photoreceptors from mice retina for (a) IL-1β (69 pg/ml in diabetic mice vs 49 pg/ml in non-diabetic mice) and (b) TNF-α (29 pg/ml in diabetic mice vs 9 pg/ml in non-diabetic mice). Adding the same concentration of IL-1β released by photoreceptor sheets from diabetic mice to endothelial cells for 24 h resulted in increased endothelial cell permeability compared with adding the same concentration of IL-1β released by photoreceptors from non-diabetic mice (c). Adding the same concentration of TNF-α released by photoreceptors from diabetic and non-diabetic mice to endothelial cells did not produce an increase in permeability (c). IL-1β and TNF-α added together to endothelial cells caused an increase in permeability (c), but did not enhance endothelial cell permeability in an additive or synergistic manner. White bars, same concentration of cytokine added to endothelial cells as the concentration released from photoreceptor sheets of non-diabetic animals; black bars, same concentration of cytokine added as the concentration released from photoreceptor sheets of diabetic animals. D, diabetic; N, non-diabetic. n = 4 for all groups. Duration of diabetes was 2 months and mice were 4 months of age when killed. *p < 0.05, **p < 0.01
Using the same concentrations of IL-1β and TNF-α released by photoreceptor sheets from non-diabetic and diabetic mice, we tested for the effect of these inflammatory proteins (using mouse recombinant protein forms of IL-1β and TNF-α) on retinal endothelial cell permeability in vitro. Adding the same concentration of IL-1β released from photoreceptors from diabetic mice to endothelial cells for 24 h resulted in statistically significant increases in endothelial cell permeability as compared with adding the same concentration of IL-1β released from photoreceptors from non-diabetic mice (Fig. 5c). In contrast, incubating endothelial cells with the same concentration of TNF-α released from photoreceptors from diabetic mice did not cause a change in permeability compared with incubating them with the same concentration from photoreceptors of non-diabetic mice (Fig. 5c). Addition of IL-1β and TNF-α together at their exact concentrations as those released from photoreceptor sheets from diabetic mice resulted in statistically significant increases in endothelial cell permeability (Fig. 5c). However, IL-1β and TNF-α added together did not produce an additive or synergistic effect on endothelial cell permeability. The glucose concentration used during the 24 h incubations did not appear to exacerbate the effect of these cytokines on endothelial cell permeability (Fig. 5c).
Discussion
Retinal vascular permeability associated with diabetic retinopathy has been demonstrated by multiple investigators [14,15,16,17,18,19,20,21,22,23, 34]. Here, we provide evidence that photoreceptor cells contribute to diabetes-induced increase in retinal vascular permeability. Diabetes of 8 months duration in wild-type mice significantly increased the accumulation of fluorescently labelled albumin in the neural retina (outside of the vasculature) in multiple retinal layers (i.e. OPL, INL and IPL), each of which is perfused by a different network of the retinal vasculature, whereas the diabetes-induced permeability defect was significantly inhibited in other animals whose photoreceptors had degenerated earlier due to opsin deficiency. We and others had previously provided evidence that retinal vascular permeability is also increased at 2–3 months of diabetes in rodents [14, 21]. Photoreceptor cells have shown no increase in cell death in our wild-type mice diabetic for 8 months [5], but the induction of diabetes in a known model of photoreceptor degeneration clearly shows the importance of photoreceptors in the diabetes-induced increase in retinal vascular permeability.
Interestingly, in animals lacking photoreceptors, the diabetes-induced increase in permeability was inhibited in the retinal layers closest to photoreceptors (i.e. OPL and INL), but not inhibited in the IPL. Several possible reasons for this non-uniform effect across the retinal vasculature can be considered, but one possibility is that soluble factors released by photoreceptors adversely affect the retinal vasculature in a diffusion-limited manner. If true, one might expect the permeability defect to occur first in the outer vascular plexus because photoreceptor degeneration due to opsin deficiency has been reported to stimulate degeneration of the retinal vasculature [5, 6]. However, we acknowledge the possibility that the surviving vasculature in the Rho −/− mice might be less susceptible to leak in diabetes or that the retinal reorganisation after photoreceptor degeneration in the Rho −/− mutants might induce the release of anti-permeability factors.
Previous evidence had shown that photoreceptor cells release products that could cause induction of proinflammatory proteins in diabetes and in other pathological models [4, 35], so we tested to see if photoreceptors released products that directly contributed to increased permeability of retinal endothelial cells. Photoreceptors from wild-type diabetic animals released products that directly enhanced endothelial cell permeability, and this increase was not reproduced by incubating endothelial cells in elevated glucose alone. Photoreceptors from wild-type diabetic mice also released products that reduced levels of at least one protein (claudin) that regulates endothelial cell permeability [17, 24]. We do acknowledge the possibility that in diabetes photoreceptor cells may release products that stimulate nearby cells (e.g. circulating leucocytes, microglia and inner retinal neurons) to regulate endothelial cell permeability, but whether or not these effects on other cells are initiated by products released from photoreceptor cells remains to be determined. In fact, we have previously reported in vitro and ex vivo evidence that photoreceptor cells can release products that can stimulate nearby cells [4].
To detect for possible inflammatory proteins released by photoreceptors in diabetes, we carried out a protein array. Photoreceptors from diabetic mice released greater than normal protein amounts of a variety of proteins including IL-1α, IL-1β, IL-6, IL-12, CXCL1, MCP-1, CXCL12a, I-309, CCL25 and TNF-α. Some of these proteins had been previously reported to increase endothelial permeability or alter tight junction and cell adhesion proteins [29,30,31, 36]. Thus, we added the same concentrations of IL-1β and TNF-α released by photoreceptors from diabetic mice to cultured endothelial cells to determine if they would increase endothelial permeability in vitro. Our results indicate that IL-1β probably contributes to the photoreceptor-mediated increase in endothelial permeability in diabetes, but we found no evidence that the amount of TNF-α released by photoreceptors in diabetes contributes to the permeability defect, at least acutely. It is important to recognise that photoreceptor cells in diabetes also could be releasing many other products or mediators (e.g. lipids, neurotransmitters, etc.) that may contribute to retinal vascular permeability or other characteristics of early diabetic retinopathy.
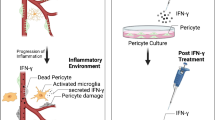
Increased permeability of the retinal vasculature in diabetes also might be a consequence of endothelial cell death, which is known to occur in diabetes [11, 37]. We investigated whether soluble products released by photoreceptors in diabetes or diabetes-like conditions can directly kill retinal endothelial cells, but found no evidence for direct cytotoxicity, at least during a 24 h exposure. Thus, these data fail to provide evidence that photoreceptors affect permeability in diabetes by directly contributing to endothelial cell death. Previous evidence, however, has revealed that incubating leucocytes from diabetic individuals or animals with retinal endothelial cells can directly kill endothelial cells [11,12,13], and that photoreceptors contribute to the activation of leucocytes to cause this endothelial cytotoxicity [4, 5]. Thus, although soluble factors released from photoreceptors in diabetes seem not to directly kill endothelial cells, photoreceptors can influence endothelial cell death in other ways (Fig. 6).
In summary, we provide in vivo evidence that photoreceptor cells in diabetes contribute to increased retinal vascular permeability, and ex vivo evidence that photoreceptors from diabetic animals release soluble products and inflammatory proteins that directly contribute to increased retinal endothelial cell permeability (but not death) (Fig. 6), in part by regulating retinal endothelial cell tight junction proteins. Photoreceptor cells may also contribute to endothelial permeability indirectly, however, by activating leucocytes (Fig. 6). Talahalli et al demonstrated that diabetic chimeric mice in which leucocytes were deficient in 5-lipoxygenase did not develop the expected diabetes-induced increase in retinal vascular permeability defect [22], but chimeric mice, in which marrow-derived cells were deficient in toll-like receptor 2/4, IL-1β or MyD88 did develop the diabetes-induced retinal vascular permeability defect [21]. More studies are needed to better clarify this discrepancy and elucidate the specific role(s) of leucocytes in diabetes-induced retinal vascular permeability.
Studies of diabetic retinopathy have focused especially on the retinal vasculature, but recent studies suggest that the neural retina (particularly photoreceptors) is also involved. This study suggests a mechanism by which photoreceptor cells can initiate retinal vascular permeability characteristic of diabetic retinopathy (Fig. 6). In the future, we would like to investigate the specific vascular regions undergoing permeability. Photoreceptor cells might not be unique in their ability to influence nearby cells, and inner retinal neurons likewise might have local effects on permeability. The large number and metabolic activity of photoreceptor cells in the retina, however, suggests that photoreceptors play a dominant role over other neuronal cells in the regulation of vascular physiology.
Abbreviations
- BRB:
-
Blood retinal barrier
- CCL:
-
Chemokine ligand
- CXCL:
-
Chemokine (C-X-C motif) ligand
- INL:
-
Inner nuclear layer
- IPL:
-
Inner plexiform layer
- MCP-1:
-
Monocyte chemoattractant protein 1
- ONL:
-
Outer nuclear layer
- OPL:
-
Outer plexiform layer
- qRT-PCR:
-
Quantitative reverse transcription PCR
- VE:
-
Vascular endothelial
References
Engelgau MM, Geiss LS, Saaddine JB et al (2004) The evolving diabetes burden in the United States. Ann Intern Med 140:945–950
Arden GB, Ramsey DJ (1995) Diabetic retinopathy and a novel treatment based on the biophysics of rod photoreceptors and dark adaptation. University of Utah Health Sciences Center
Du Y, Veenstra A, Palczewski K, Kern TS (2013) Photoreceptor cells are major contributors to diabetes-induced oxidative stress and local inflammation in the retina. Proc Natl Acad Sci U S A 110:16586–16591
Tonade D, Liu H, Kern TS (2016) Photoreceptor cells produce inflammatory mediators that contribute to endothelial cell death in diabetes. Invest Ophthalmol Vis Sci 57:4264–4271
Liu H, Tang J, Du Y et al (2016) Photoreceptor cells influence retinal vascular degeneration in mouse models of retinal degeneration and diabetes. Invest Ophthalmol Vis Sci 57:4272–4281
de Gooyer TE, Stevenson KA, Humphries P et al (2006) Retinopathy is reduced during experimental diabetes in a mouse model of outer retinal degeneration. Invest Ophthalmol Vis Sci 47:5561–5568
Scuderi S, D’amico AG, Federico C et al (2015) Different retinal expression patterns of IL-1α, IL-1β, and their receptors in a rat model of type 1 STZ-induced diabetes. J Mol Neurosci 56:431–439
Zheng L, Du Y, Miller C et al (2007) Critical role of inducible nitric oxide synthase in degeneration of retinal capillaries in mice with streptozotocin-induced diabetes. Diabetologia 50:1987–1996
Joussen AM, Poulaki V, Le ML et al (2004) A central role for inflammation in the pathogenesis of diabetic retinopathy. FASEB J 18:1450–1452
Tang J, Kern TS (2011) Inflammation in diabetic retinopathy. Prog Retin Eye Res 30:343–358
Li G, Veenstra AA, Talahalli RR et al (2012) Marrow-derived cells regulate the development of early diabetic retinopathy and tactile allodynia in mice. Diabetes 61:3294–3303
Tian P, Ge H, Liu H et al (2013) Leukocytes from diabetic patients kill retinal endothelial cells: effects of berberine. Mol Vis 19:2092–2105
Veenstra AA, Tang J, Kern TS (2013) Antagonism of CD11b with neutrophil inhibitory factor (NIF) inhibits vascular lesions in diabetic retinopathy. PLoS One 8:e78405
Antonetti DA, Barber AJ, Khin S et al (1998) Vascular permeability in experimental diabetes is associated with reduced endothelial occludin content: vascular endothelial growth factor decreases occludin in retinal endothelial cells. Penn State Retina Research Group. Diabetes 47:1953–1959
Cunha-Vaz J, Faria de Abreu JR, Campos AJ (1975) Early breakdown of the blood-retinal barrier in diabetes. Br J Ophthalmol 59:649–656
Enea NA, Hollis TM, Kern JA, Gardner TW (1989) Histamine H1 receptors mediate increased blood-retinal barrier permeability in experimental diabetes. Arch Ophthalmol (Chicago, IL 1960) 107:270–274
Frey T, Antonetti DA (2011) Alterations to the blood–retinal barrier in diabetes: cytokines and reactive oxygen species. Antioxid Redox Signal 15:1271–1284
Barber AJ, Antonetti DA, Kern TS et al (2005) The Ins2 Akita mouse as a model of early retinal complications in diabetes. Investig Opthalmology Vis Sci 46:2210
Liu H, Tang J, Du Y et al (2015) Retinylamine benefits early diabetic retinopathy in mice. J Biol Chem 290:21568–21579
Du Y, Cramer M, Lee CA et al (2015) Adrenergic and serotonin receptors affect retinal superoxide generation in diabetic mice: relationship to capillary degeneration and permeability. FASEB J 29:2194–2204
Tang J, Allen Lee C, Du Y et al (2013) MyD88-dependent pathways in leukocytes affect the retina in diabetes. PLoS One 8:e68871
Talahalli R, Zarini S, Tang J et al (2013) Leukocytes regulate retinal capillary degeneration in the diabetic mouse via generation of leukotrienes. J Leukoc Biol 93:135–143
Joussen AM, Poulaki V, Mitsiades N et al (2002) Nonsteroidal anti-inflammatory drugs prevent early diabetic retinopathy via TNF-a suppression. FASEB J 16:438–440
González-Mariscal L, Betanzos A, Nava P, Jaramillo BE (2003) Tight junction proteins. Prog Biophys Mol Biol 81:1–44
de Gooyer TE, Stevenson KA, Humphries P et al (2006) Rod photoreceptor loss in Rho-/- mice reduces retinal hypoxia and hypoxia-regulated gene expression. Invest Ophthalmol Vis Sci 47:5553–5560
Humphries MM, Rancourt D, Farrar GJ et al (1997) Retinopathy induced in mice by targeted disruption of the rhodopsin gene. Nat Genet 15:216–219
Clérin E, Yang Y, Forster V et al (2014) Vibratome sectioning mouse retina to prepare photoreceptor cultures. J Vis Exp: e51954
Su X, Sorenson CM, Sheibani N (2003) Isolation and characterization of murine retinal endothelial cells. Mol Vis 9:171–178
Aveleira CA, Lin C-M, Abcouwer SF et al (2010) TNF-α signals through PKCζ/NF-κB to alter the tight junction complex and increase retinal endothelial cell permeability. Diabetes 59:2872–2882
Rochfort KD, Collins LE, McLoughlin A, Cummins PM (2016) Tumour necrosis factor-α-mediated disruption of cerebrovascular endothelial barrier integrity in vitro involves the production of proinflammatory interleukin-6. J Neurochem 136:564–572
Rochfort KD, Collins LE, McLoughlin A, Cummins PM (2015) Shear-dependent attenuation of cellular ROS levels can suppress proinflammatory cytokine injury to human brain microvascular endothelial barrier properties. J Cereb Blood Flow Metab 35:1648–1656
Puhlmann M, Weinreich DM, Farma JM et al (2005) Interleukin-1beta induced vascular permeability is dependent on induction of endothelial tissue factor (TF) activity. J Transl Med 3:37
Partridge CA, Jeffrey JJ, Malik AB (1993) A 96-kDa gelatinase induced by TNF-alpha contributes to increased microvascular endothelial permeability. Am J Phys 265:L438–L447
Vinores SA, Derevjanik NL, Mahlow J et al (1998) Electron microscopic evidence for the mechanism of blood-retinal barrier breakdown in diabetic rabbits: comparison with magnetic resonance imaging. Pathol Res Pract 194:497–505
Yang L, Zhu X, Tso MOM (2007) A possible mechanism of microglia-photoreceptor crosstalk. Mol Vis 13:2048–2057
Rochfort KD, Collins LE, Murphy RP et al (2014) Downregulation of blood-brain barrier phenotype by proinflammatory cytokines involves NADPH oxidase-dependent ROS generation: consequences for interendothelial adherens and tight junctions. PLoS One 9:e101815
Joussen AM, Doehmen S, Le ML et al (2009) TNF-alpha mediated apoptosis plays an important role in the development of early diabetic retinopathy and long-term histopathological alterations. Mol Vis 15:1418–1428
Acknowledgements
We thank C.A. Lee, H. Butler and K. Franke at Case Western Reserve University for expert maintenance of the mice. Mouse retinal endothelial cells (from a transformed line) were kindly provided by N. Sheibani (University of Wisconsin, Madison, WI, USA).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Data availability
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
Funding
The studies reported in this manuscript were supported by grants from the National Eye Institute of the National Institutes of Health under awards R01EY00300, R01EY022938 and R24EY021126; and a Merit grant from the Department of Veterans Affairs.
Duality of interest
The authors declare no conflict of interest associated with this paper.
Contribution statement
DT and HL designed experiments and acquired data. DT, HL and TSK wrote the manuscript. DT, TSK and KP advised, interpreted and reviewed the manuscript. All the authors approved the final version of the manuscript to be published. DT and TSK are the guarantors of this work.
Electronic supplementary material
ESM Figs
(PDF 111 kb)
Rights and permissions
About this article
Cite this article
Tonade, D., Liu, H., Palczewski, K. et al. Photoreceptor cells produce inflammatory products that contribute to retinal vascular permeability in a mouse model of diabetes. Diabetologia 60, 2111–2120 (2017). https://doi.org/10.1007/s00125-017-4381-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-017-4381-5