Abstract
Purpose
Traumas cause great casualties, accompanied by heavy economic burdens every year. The study aimed to use ML (machine learning) survival algorithms for predicting the 8-and 24-hour survival of severe traumas.
Methods
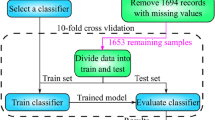
A retrospective study using data from National Trauma Data Bank (NTDB) was conducted. Four ML survival algorithms including survival tree (ST), random forest for survival (RFS) and gradient boosting machine (GBM), together with a Cox proportional hazard model (Cox), were utilized to develop the survival prediction models. Following this, model performance was determined by the comparison of the C-index, integrated Brier score (IBS) and calibration curves in the test datasets.
Results
A total of 191,240 individuals diagnosed with severe trauma between 2015 and 2018 were identified. Glasgow Coma Scale (GCS), trauma type, age, SaO2, respiratory rate (RR), systolic blood pressure (SBP), EMS transport time, EMS on-scene time, pulse, and EMS response time were identified as the main predictors. For predicting the 8-hour survival with the complete cases, the C-indexes in the test sets were 0.853 (0.845, 0.861), 0.823 (0.812, 0.834), 0.871 (0.862, 0.879) and 0.857 (0.849, 0.865) for Cox, ST, RFS and GBM, respectively. Similar results were observed in the 24-hour survival prediction models. The prediction error curves based on IBS also showed a similar pattern for these models. Additionally, a free web-based calculator was developed for potential clinical use.
Conclusion
The RFS survival algorithms provide non-parametric alternatives to other regression models to be of clinical use for estimating the survival probability of severe trauma patients.




Similar content being viewed by others
Data availability
Publicly available datasets were analyzed in this study. These data can be found here: https://www.facs.org/quality-programs/trauma/quality/national-trauma-data-bank.
References
Rhee P, Joseph B, Pandit V, et al. Increasing trauma deaths in the United States. Annals Surg. 2014;260(1):13–21. https://doi.org/10.1097/sla.0000000000000600.
Gruen RL, Brohi K, Schreiber M, et al. Haemorrhage control in severely injured patients. Lancet (London, England). 2012;380(9847):1099–108. https://doi.org/10.1016/s0140-6736(12)61224-0.
Cunningham RM, Walton MA, Carter PM. The Major Causes of Death in Children and Adolescents in the United States. New England J Med. 2018;379(25):2468–75. https://doi.org/10.1056/NEJMsr1804754.
Acosta JA, Yang JC, Winchell RJ, et al. Lethal injuries and time to death in a level I trauma center. J Ame College Surgeons. 1998;186(5):528–33. https://doi.org/10.1016/s1072-7515(98)00082-9.
Clark DE, Qian J, Sihler KC, Hallagan LD, Betensky RA. The distribution of survival times after injury. World J Surg. 2012;36(7):1562–70. https://doi.org/10.1007/s00268-012-1549-5.
Baker SP, O’Neill B, Haddon W Jr, Long WB. The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma. 1974;14(3):187–96.
Champion HR, Sacco WJ, Carnazzo AJ, Copes W, Fouty WJ. Trauma score. Critical Care Med. 1981;9(9):672–6. https://doi.org/10.1097/00003246-198109000-00015.
Boyd CR, Tolson MA, Copes WS: Evaluating trauma care: the TRISS method trauma score and the injury severity score. J Trauma 1987:27(4) 370-8.
Champion HR, Copes WS, Sacco WJ, et al. A new characterization of injury severity. J Trauma. 1990;30(5):539-45; discussion 45-6. https://doi.org/10.1097/00005373-199005000-00003
Osler T, Rutledge R, Deis J, Bedrick E. ICISS: an international classification of disease-9 based injury severity score. J Trauma. 1996;41(3):380-6; discussion 6-8. https://doi.org/10.1097/00005373-199609000-00002
Burd RS, Ouyang M, Madigan D. Bayesian logistic injury severity score: a method for predicting mortality using international classification of disease-9 codes. Academic Emergency Med: Official J Soc Acad Emerg Med. 2008;15(5):466–75. https://doi.org/10.1111/j.1553-2712.2008.00105.x.
Champion HR, Sacco WJ, Copes WS, Gann DS, Gennarelli TA, Flanagan ME. A revision of the Trauma Score. J Trauma. 1989;29(5):623–9. https://doi.org/10.1097/00005373-198905000-00017.
Lavoie A, Emond M, Moore L, Camden S, Liberman M. Evaluation of the Prehospital Index, presence of high-velocity impact and judgment of emergency medical technicians as criteria for trauma triage. Cjem. 2010;12(2):111–8. https://doi.org/10.1017/s1481803500012136.
Gray A, Goyder EC, Goodacre SW, Johnson GS. Trauma triage: a comparison of CRAMS and TRTS in a UK population. Injury. 1997;28(2):97–101. https://doi.org/10.1016/s0020-1383(96)00170-2.
Morris RS, Karam BS, Murphy PB, Jenkins P, Milia DJ, Hemmila MR, et al. Field-triage, hospital-triage and triage-assessment: a literature review of the current phases of adult trauma triage. J Trauma Acute Care Surg. 2021;90(6):e138–45. https://doi.org/10.1097/TA.0000000000003125.
Osler T. Injury severity scoring: perspectives in development and future directions. Ame J Surg. 1993;165(2A Suppl):43s–51s. https://doi.org/10.1016/s0002-9610(05)81206-1.
West TA, Rivara FP, Cummings P, Jurkovich GJ, Maier RV. Harborview assessment for risk of mortality: an improved measure of injury severity on the basis of ICD-9-CM. J Trauma. 2000;49(3):530-40; discussion 40-1. https://doi.org/10.1097/00005373-200009000-00022
Glance LG, Osler TM, Mukamel DB, Meredith W, Wagner J, Dick AW. TMPM-ICD9: a trauma mortality prediction model based on ICD-9-CM codes. Annals Sur. 2009;249(6):1032–9. https://doi.org/10.1097/SLA.0b013e3181a38f28.
Gorczyca MT, Toscano NC, Cheng JD. The trauma severity model: An ensemble machine learning approach to risk prediction. Comput Biology Med. 2019;108:9–19. https://doi.org/10.1016/j.compbiomed.2019.02.025.
Larsson A, Berg J, Gellerfors M, Gerdin Wärnberg M. The advanced machine learner XGBoost did not reduce prehospital trauma mistriage compared with logistic regression: a simulation study. BMC Med Inform Decision Making. 2021;21(1):192. https://doi.org/10.1186/s12911-021-01558-y.
Hashmi ZG, Kaji AH, Nathens AB. Practical Guide to Surgical Data Sets: National Trauma Data Bank (NTDB). JAMA Surg. 2018;153(9):852–3. https://doi.org/10.1001/jamasurg.2018.0483.
Collins GS, Reitsma JB, Altman DG, Moons KG. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ (Clinical research ed.). 2015;350:g7594. https://doi.org/10.1136/bmj.g7594
Chester JG, Rudolph JL. Vital signs in older patients: age-related changes. J Ame Med Directors Assoc. 2011;12(5):337–43. https://doi.org/10.1016/j.jamda.2010.04.009.
Miller PJ, McArtor DB, Lubke GH. A Gradient Boosting Machine for Hierarchically Clustered Data. Multivariate Behav Res. 2017;52(1):117. https://doi.org/10.1080/00273171.2016.1265433.
Harrell FE Jr, Califf RM, Pryor DB, Lee KL, Rosati RA. Evaluating the yield of medical tests. Jama. 1982;247(18):2543–6.
Mogensen UB, Ishwaran H, Gerds TA. Evaluating Random Forests for Survival Analysis using Prediction Error Curves. Journal of statistical software. 2012;50(11):1-23. https://doi.org/10.18637/jss.v050.i11
Martin AB, Hartman M, Washington B, Catlin A. National Health Spending: Faster Growth In 2015 As Coverage Expands And Utilization Increases. Health affairs (Project Hope). 2017;36(1):166–76. https://doi.org/10.1377/hlthaff.2016.1330.
Vittinghoff E, McCulloch CE. Relaxing the rule of ten events per variable in logistic and Cox regression. Ame J Epidemiol. 2007;165(6):710–8. https://doi.org/10.1093/aje/kwk052.
Gauss T, Ageron FX, Devaud ML, et al. Association of Prehospital Time to In-Hospital Trauma Mortality in a Physician-Staffed Emergency Medicine System. JAMA Surg. 2019;154(12):1117–24. https://doi.org/10.1001/jamasurg.2019.3475.
Brown JB, Rosengart MR, Forsythe RM, et al. Not all prehospital time is equal: Influence of scene time on mortality. J Trauma Acute Care Surg. 2016;81(1):93–100. https://doi.org/10.1097/ta.0000000000000999.
Nasser AAH, Nederpelt C, El Hechi M, et al. Every minute counts: The impact of pre-hospital response time and scene time on mortality of penetrating trauma patients. Ame J Surg. 2020;220(1):240–4. https://doi.org/10.1016/j.amjsurg.2019.11.018.
Kay R. Goodness of fit methods for the proportional hazards regression model: a review. Revue d’epidemiologie et de sante publique. 1984;32(3–4):185–98.
Du M, Haag DG, Lynch JW, Mittinty MN. Comparison of the Tree-Based Machine Learning Algorithms to Cox Regression in Predicting the Survival of Oral and Pharyngeal Cancers: Analyses Based on SEER Database. Cancers. 2020;12(10). https://doi.org/10.3390/cancers12102802
Ishwaran H, Kogalur UB, Blackstone EH, Lauer MS. Random survival forests. Annals Appli Stat. 2008;2(3):841-60, 20.
Strobl C, Malley J, Tutz G. An introduction to recursive partitioning: rationale, application, and characteristics of classification and regression trees, bagging, and random forests. Psycho Meth. 2009;14(4):323–48. https://doi.org/10.1037/a0016973.
Ishwaran H, Gerds TA, Kogalur UB, Moore RD, Gange SJ, Lau BM. Random survival forests for competing risks. Biostatistics (Oxford, England). 2014;15(4):757–73. https://doi.org/10.1093/biostatistics/kxu010.
Wang H, Li G. A Selective Review on Random Survival Forests for High Dimensional Data. Quantitative bio-science. 2017;36(2):85-96. https://doi.org/10.22283/qbs.2017.36.2.85
Li Y, Wang L, Liu Y, et al. Development and Validation of a Simplified Prehospital Triage Model Using Neural Network to Predict Mortality in Trauma Patients: The Ability to Follow Commands, Age, Pulse Rate, Systolic Blood Pressure and Peripheral Oxygen Saturation (CAPSO) Model. Front Med. 2021;8:810195. https://doi.org/10.3389/fmed.2021.810195.
Acknowledgements
Not applicable.
Funding
This study was supported by the San Hang Program of Naval Medical University and Clinical Research Program of Shanghai Municipal Health Commission (202340037).
Author information
Authors and Affiliations
Contributions
Shuogui xu and Zhichao Jin contributed to the conception and design; Chi Peng, Hang Yu, Qi Chen and Yibin Guo analyzed and interpreted of data; Fan Yang, Chi Peng and Liwei Peng drafted the manuscript or revised it critically for important intellectual content: Chi Peng performed the statistical analysis; All authors read and approved the final manuscript
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study protocol was approved and the requirement for informed consent from the participants was waived by the Institutional Review Board of Naval Medical University.
Consent for publication
Not applicable.
Competing interests
None declared.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Peng, C., Peng, L., Yang, F. et al. The prediction of the survival in patients with severe trauma during prehospital care: Analyses based on NTDB database. Eur J Trauma Emerg Surg (2024). https://doi.org/10.1007/s00068-024-02484-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00068-024-02484-0