Abstract
Purpose
To perform a systematic review and meta-analysis of the impact of brachytherapy (BT) technique (two-dimensional [2D] or three-dimensional image-guided [3D]) on outcomes of cervical cancer patients.
Methods
PubMed and EMBASE databases were searched up to April 16, 2019, for studies which evaluated the effect of 3D-BT compared to 2D-BT in cervical cancer. Endpoints included cumulative incidence of severe toxicity, locoregional recurrence-free survival (LRRFS), progression-free survival (PFS), and overall survival (OS). Hazard ratios (HRs) were pooled in the meta-analysis using the random-effects model.
Results
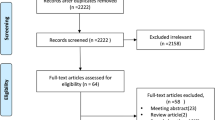
Six studies of eight cohorts were included in the quantitative synthesis. The pooled HR regarding toxicity was evaluated in five cohorts in three studies, and the HR of 3D-BT compared to 2D-BT was 0.54 (95% confidence interval [CI] 0.37–0.77). All six studies were included for the synthesis for LRRFS, and the pooled HR favors 3D-BT (0.61 [95% CI 0.40–0.93]). For PFS, three studies were included for analysis and 3D-BT was superior to 2D-BT (HR = 0.75 [95% CI 0.59–0.96]). Five studies were included for the pooled HR regarding OS, and pooled HR of 3D-BT compared to 2D-BT was 0.65 (95% CI 0.40–1.06).
Conclusion
3D-BT might reduce severe toxicity and improve LRRFS and PFS in patients with cervical cancer. 3D-BT should be considered for standard management of cervical cancer, and efforts for adopting this procedure in Korea should be pursued.




Similar content being viewed by others
Abbreviations
- BT:
-
Brachytherapy
- CI:
-
Confidence interval
- CIs:
-
Confidence intervals
- CT:
-
Computed tomography
- CTCAE:
-
Common Terminology Criteria for Adverse Events
- EBRT:
-
External beam radiotherapy
- EMBRACE:
-
Image-guided intensity-modulated external beam radiochemotherapy and MRI-based adaptive brachytherapy in locally advanced cervical cancer
- GEC-ESTRO:
-
Groupe Européen de Curiethérapie/European Society for Therapeutic Radiology and Oncology
- HR:
-
Hazard ratio
- HRs:
-
Hazard ratios
- IMRT:
-
Intensity-modulated radiotherapy
- LRRFS:
-
Locoregional recurrence-free survival
- MRI:
-
Magnetic resonance imaging
- OAR:
-
Organs at risk
- OS:
-
Overall survival
- PICOS:
-
Patient/Intervention/Comparator/Outcome/Study
- PFS:
-
Progression-free survival
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- QUIPS:
-
Quality in Prognostic Studies
- RTOG/EORTC:
-
Radiation Therapy Oncology Group and the European Organization for Research and Treatment of Cancer
- STIC:
-
Soutien aux Techniques Innovantes et Coûteuses
- 2D:
-
Two-dimensional
- 3D:
-
Three-dimensional
References
Narayan K, Barkati M, van Dyk S, Bernshaw D (2010) Image-guided brachytherapy for cervix cancer: from Manchester to Melbourne. Expert Rev Anticancer Ther 10(1):41–46. https://doi.org/10.1586/era.09.166
Roeske JC, Mundt AJ, Halpern H, Sweeney P, Sutton H, Powers C, Rotmensch J, Waggoner S, Weichselbaum RR (1997) Late rectal sequelae following definitive radiation therapy for carcinoma of the uterine cervix: a dosimetric analysis. Int J Radiat Oncol Biol Phys 37(2):351–358. https://doi.org/10.1016/S0360-3016(96)00490-7
Perez CA, Grigsby PW, Lockett MA, Chao KSC, Williamson J (1999) Radiation therapy morbidity in carcinoma of the uterine cervix: dosimetric and clinical correlation. Int J Radiat Oncol Biol Phys 44(4):855–866. https://doi.org/10.1016/S0360-3016(99)00111-X
Pötter R, Knocke T, Fellner C, Baldass M, Reinthaller A, Kucera H (2000) Definitive radiotherapy based on HDR brachytherapy with iridium 192 in uterine cervix carcinoma: report on the Vienna University Hospital findings (1993–1997) compared to the preceding period in the context of ICRU 38 recommendations. Cancer Radiother 4(2):159–172
Haie-Meder C, Pötter R, Van Limbergen E, Briot E, De Brabandere M, Dimopoulos J, Dumas I, Hellebust TP, Kirisits C, Lang S (2005) Recommendations from Gynaecological (GYN) GEC-ESTRO Working Group (I): concepts and terms in 3D image based 3D treatment planning in cervix cancer brachytherapy with emphasis on MRI assessment of GTV and CTV. Radiother Oncol 74(3):235–245
Schmid M, Haie-Meder C, Mahanshetty U, Jürgenliemk-Schulz IM, Segedin B, Hoskin P, Kirisits C, Lindegaard J, Tanderup K, Pötter R (2017) OC-0055: Local failures after radiochemotherapy and MR-image-guided brachytherapy in cervical cancer patients. Radiother Oncol 123:26. https://doi.org/10.1016/S0167-8140(17)30499-1
Mazeron R, Fokdal LU, Kirchheiner K, Georg P, Jastaniyah N, Segedin B, Mahantshetty U, Hoskin P, Jurgenliemk-Schulz I, Kirisits C, Lindegaard JC, Dorr W, Haie-Meder C, Tanderup K, Potter R (2016) Dose-volume effect relationships for late rectal morbidity in patients treated with chemoradiation and MRI-guided adaptive brachytherapy for locally advanced cervical cancer: results from the prospective multicenter EMBRACE study. Radiother Oncol 120(3):412–419. https://doi.org/10.1016/j.radonc.2016.06.006
Charra-Brunaud C, Harter V, Delannes M, Haie-Meder C, Quetin P, Kerr C, Castelain B, Thomas L, Peiffert D (2012) Impact of 3D image-based PDR brachytherapy on outcome of patients treated for cervix carcinoma in France: results of the French STIC prospective study. Radiother Oncol 103(3):305–313. https://doi.org/10.1016/j.radonc.2012.04.007
Cho O, Chun M (2018) Management for locally advanced cervical cancer: new trends and controversial issues. Radiat Oncol J 36(4):254–264. https://doi.org/10.3857/roj.2018.00500
Kang HC, Shin KH, Park SY, Kim JY (2010) 3D CT-based high-dose-rate brachytherapy for cervical cancer: clinical impact on late rectal bleeding and local control. Radiother Oncol 97(3):507–513. https://doi.org/10.1016/j.radonc.2010.10.002
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62(10):e1–34. https://doi.org/10.1016/j.jclinepi.2009.06.006
Hayden JA, van der Windt DA, Cartwright JL, Cote P, Bombardier C (2013) Assessing bias in studies of prognostic factors. Ann Intern Med 158(4):280–286. https://doi.org/10.7326/0003-4819-158-4-201302190-00009
Tierney JF, Stewart LA, Ghersi D, Burdett S, Sydes MR (2007) Practical methods for incorporating summary time-to-event data into meta-analysis. Trials 8:16. https://doi.org/10.1186/1745-6215-8-16
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Cochran WG (1954) The combination of estimates from different experiments. Biometrics 10(1):101–129
Fleiss JL (1986) Analysis of data from multiclinic trials. Control Clin Trials 7(4):267–275. https://doi.org/10.1016/0197-2456(86)90034-6
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Kang HC, Shin KH, Park SY, Kim JY (2010) 3D CT-based high-dose-rate brachytherapy for cervical cancer: clinical impact on late rectal bleeding and local control. Radiother Oncol 97(3):507–513. https://doi.org/10.1016/j.radonc.2010.10.002
Rijkmans EC, Nout RA, Rutten IHHM, Ketelaars M, Neelis KJ, Laman MS, Coen VLMA, Gaarenstroom KN, Kroep JR, Creutzberg CL (2014) Improved survival of patients with cervical cancer treated with image-guided brachytherapy compared with conventional brachytherapy. Gynecol Oncol 135(2):231–238. https://doi.org/10.1016/j.ygyno.2014.08.027
Thomas KM, Maquilan G, Stojadinovic S, Medin P, Folkert MR, Albuquerque K (2017) Reduced toxicity with equivalent outcomes using three-dimensional volumetric (3DV) image-based versus nonvolumetric point-based (NV) brachytherapy in a cervical cancer population. Brachytherapy 16(5):943–948. https://doi.org/10.1016/j.brachy.2017.05.001
Derks K, Steenhuijsen JL, van den Berg HA, Houterman S, Cnossen J, van Haaren P, De Jaeger K (2018) Impact of brachytherapy technique (2D versus 3D) on outcome following radiotherapy of cervical cancer. J Contemp Brachytherapy 10(1):17
Lin AJ, Kidd E, Dehdashti F, Siegel BA, Mutic S, Thaker PH, Massad LS, Powell MA, Mutch DG, Markovina S (2019) Intensity modulated radiation therapy and image-guided adapted brachytherapy for cervix cancer. Int J Radiat Oncol Biol Phys 103(5):1088–1097
Kirchheiner K, Nout RA, Tanderup K, Lindegaard JC, Westerveld H, Haie-Meder C, Petrič P, Mahantshetty U, Dörr W, Pötter R (2014) Manifestation pattern of early-late vaginal morbidity after definitive radiation (chemo)therapy and image-guided adaptive brachytherapy for locally advanced cervical cancer: an analysis from the EMBRACE study. Int J Radiat Oncol Biol Phys 89(1):88–95. https://doi.org/10.1016/j.ijrobp.2014.01.032
Mazeron R, Fokdal LU, Kirchheiner K, Georg P, Jastaniyah N, Šegedin B, Mahantshetty U, Hoskin P, Jürgenliemk-Schulz I, Kirisits C, Lindegaard JC, Dörr W, Haie-Meder C, Tanderup K, Pötter R (2016) Dose–volume effect relationships for late rectal morbidity in patients treated with chemoradiation and MRI-guided adaptive brachytherapy for locally advanced cervical cancer: Results from the prospective multicenter EMBRACE study. Radiother Oncol 120(3):412–419. https://doi.org/10.1016/j.radonc.2016.06.006
Lim MC, Lee M, Shim SH, Nam EJ, Lee JY, Kim HJ, Lee Y-Y, Lee KB, Park JY, Kim YH (2017) Practice guidelines for management of cervical cancer in Korea: a Korean Society of Gynecologic Oncology Consensus Statement. J Gynecol Oncol 28(3)
Sturdza A, Pötter R, Fokdal LU, Haie-Meder C, Tan LT, Mazeron R, Petric P, Šegedin B, Jurgenliemk-Schulz IM, Nomden C (2016) Image guided brachytherapy in locally advanced cervical cancer: improved pelvic control and survival in RetroEMBRACE, a multicenter cohort study. Radiother Oncol 120(3):428–433
Nomden CN, Pötter R, de Leeuw AAC, Tanderup K, Lindegaard JC, Schmid MP, Fortin I, Haie-Meder C, Mahantshetty U, Hoskin P, Segedin B, Bruheim K, Rai B, Huang F, Cooper R, Van Der Steen Banasik E, Van Limbergen E, Jürgenliemk-Schulz IM (2019) Nodal failure after chemo-radiation and MRI guided brachytherapy in cervical cancer: patterns of failure in the EMBRACE study cohort. Radiother Oncol 134:185–190. https://doi.org/10.1016/j.radonc.2019.02.007
Viswanathan AN, Thomadsen B, American Brachytherapy Society Cervical Cancer Recommendations Committee, American Brachytherapy Society (2012) American Brachytherapy Society consensus guidelines for locally advanced carcinoma of the cervix. Part I: general principles. Brachytherapy 11(1):33–46
Yip WWL, Wong JSY, Lee VWY, Wong FCS, Tung SY (2017) Throwing the dart blind-folded: comparison of computed tomography versus magnetic resonance imaging-guided brachytherapy for cervical cancer with regard to dose received by the ‘actual’ targets and organs at risk. J Contemp Brachytherapy 9(5):446–452. https://doi.org/10.5114/jcb.2017.71050
Koh V, Choo BA, Lee KM, Tan TH, Low JHJ, Ng SYJ, Ilancheran A, Shen L, Tang J (2017) Feasibility study of toxicity outcomes using GEC-ESTRO contouring guidelines on CT based instead of MRI-based planning in locally advanced cervical cancer patients. Brachytherapy 16(1):126–132
Kim H, Rajagopalan MS, Beriwal S, Huq MS, Smith KJ (2015) Cost-effectiveness analysis of 3D image-guided brachytherapy compared with 2D brachytherapy in the treatment of locally advanced cervical cancer. Brachytherapy 14(1):29–36. https://doi.org/10.1016/j.brachy.2014.09.002
Grover S, Harkenrider MM, Cho LP, Erickson B, Small C, Small W, Viswanathan AN (2016) Image guided cervical brachytherapy: 2014 survey of the American Brachytherapy Society. Int J Radiat Oncol Biol Phys 94(3):598–604. https://doi.org/10.1016/j.ijrobp.2015.11.024
Ohno T, Toita T, Tsujino K, Uchida N, Hatano K, Nishimura T, Ishikura S (2015) A questionnaire-based survey on 3D image-guided brachytherapy for cervical cancer in Japan: advances and obstacles. J Radiat Res 56(6):897–903. https://doi.org/10.1093/jrr/rrv047
Han K, Milosevic M, Fyles A, Pintilie M, Viswanathan AN (2013) Trends in the utilization of brachytherapy in cervical cancer in the United States. Int J Radiat Oncol Biol Phys 87(1):111–119. https://doi.org/10.1016/j.ijrobp.2013.05.033
Author information
Authors and Affiliations
Contributions
Y.J. Kim and H.-C. Kang participated in data acquisition and analysis, literature research, and drafting of the manuscript. Y.S. Kim contributed to the conception and design of the study and revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Y.J. Kim, H.-C. Kang and Y.S. Kim declare that they have no competing interests.
Additional information
Availability of data and materials
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
Caption Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Kim, Y.J., Kang, HC. & Kim, Y.S. Impact of intracavitary brachytherapy technique (2D versus 3D) on outcomes of cervical cancer: a systematic review and meta-analysis. Strahlenther Onkol 196, 973–982 (2020). https://doi.org/10.1007/s00066-020-01658-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-020-01658-0