Abstract
Purpose
We retrospectively compared the treatment outcomes of localized prostate cancer between radical prostatectomy (RP) and external beam radiotherapy (EBRT).
Materials and methods
We retrospectively analyzed 738 patients with localized prostate cancer who underwent either RP (n = 549) or EBRT (n = 189) with curative intent at our institution between March 2001 and December 2011. Biochemical failure was defined as a prostate-specific antigen (PSA) level of ≥ 0.2 ng/ml in the RP group and the nadir of + ≥ 2 ng/ml in the EBRT group.
Results
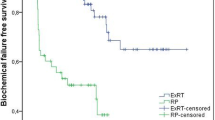
The median (range) follow-up duration was 48.8 months (0.7–133.2 months) and 48.7 months (1.0–134.8 months) and the median age was 66 years (45–89 years) and 71 years (51–84 years; p < 0.001) in the RP and EBRT groups, respectively. Overall, 21, 42, and 36 % of patients in the RP group, and 15, 27, and 58 % of patients in the EBRT group were classified as low, intermediate, and high risk, respectively (p < 0.001). Androgen-deprivation therapy was more common in the EBRT group (59 vs. 27 %, respectively; p < 0.001). The 8-year biochemical failure-free survival rates were 44 and 72 % (p < 0.001) and the disease-specific survival rates were 98 % and 97 % (p = 0.543) in the RP and EBRT groups, respectively.
Conclusions
Although the EBRT group included more high-risk patients than did the RP group, the outcomes of EBRT were not inferior to those of RP. Our data suggest that EBRT is a viable alternative to RP for treating localized prostate cancer.
Zusammenfassung
Ziel
Wir vergleichen retrospektiv die Verfahrensergebnisse des lokal begrenzten Prostatakarzinoms zwischen radikaler Prostatektomie (RP) und externer Strahlentherapie (EBRT).
Material und Methoden
Wir analysieren zurückblickend 738 Patienten mit lokal begrenztem Prostatakarzinom, die zwischen März 2001 und Dezember 2011 in unserem Institut entweder eine RP (n = 549) oder eine EBRT (n = 189) mit kurativer Intention durchliefen. Biochemischer Fehler wurde als prostataspezifisches Antigen (PSA) ≥ 0,2 ng/ml in der RP-Gruppe und ein Nadir + ≥ 2 ng/ml in EBRT-Gruppe definiert.
Ergebnisse
Die mediane Follow-up-Dauer betrug in der RP- bzw. der EBRT-Gruppe jeweils 48,8 Monate (Spanne 0,7–133,2 Monate) bzw. 48,7 Monate (Spanne 1,0–134,8 Monate) und das mittlere Alter 66 Jahre (Spanne 45–89 Jahre) bzw. 71 Jahre (Spanne 51–84 Jahre; p < 0,001). Insgesamt 21, 42, und 36 % der Patienten in der RP-Gruppe und 15, 27, und 58 % der Patienten in der EBRT-Gruppe waren jeweils klassifiziert als niedriges, mittleres bzw. hohes Risiko (P < 0,001). Eine Androgendeprivationstherapie war in der EBRT-Gruppe üblicher (59 vs. 27 %; p < 0,001). Die biochemischen fehlerfreien 8-Jahres-Überlebensraten lagen in der RP- bzw. der EBRT-Gruppe jeweils bei 44 und 72 % (p < 0,001) und die krankheitsspezifischen Überlebensraten bei 98 und 97 % (p = 0,543).
Schussfolgerung
Obwohl die EBRT-Gruppe mehr Hochrisiko-Patienten als die RP-Gruppe umfasste, waren die Ergebnisse der EBRT nicht minderwertig zu den der RP. Unsere Daten weisen darauf hin, dass EBRT für das lokal begrenzte Prostatakarzinom eine verfügbare Alternative ist.




Similar content being viewed by others
References
Jung KW, Won YJ, Kong HJ et al (2013) Cancer statistics in Korea: incidence, mortality, survival and prevalence in 2010. Cancer Res Treat 45:1–14
Zeliadt SB, Ramsey SD, Penson DF et al (2006) Why do men choose one treatment over another?: a review of patient decision making for localized prostate cancer. Cancer 106:1865–1874
Jang TL, Bekelman JE, Liu Y et al (2010) Physician visits prior to treatment for clinically localized prostate cancer. Archives Intern Med 170:440–450
Lee DH, Jung HB, Chung MS et al (2013) The change of prostate cancer treatment in Korea: 5 year analysis of a single institution. Yonsei Med J 54:87–91
Kim YJ, Cho KH, Pyo HR et al (2013) A phase II study of hypofractionated proton therapy for prostate cancer. Acta oncologica (Stockholm, Sweden) 52:477–485
Stephenson AJ, Kattan MW, Eastham JA et al (2006) Defining biochemical recurrence of prostate cancer after radical prostatectomy: a proposal for a standardized definition. J Clin Oncol 24:3973–3978
Roach M 3rd, Hanks G, Thames H Jr et al (2006) Defining biochemical failure following radiotherapy with or without hormonal therapy in men with clinically localized prostate cancer: recommendations of the RTOG-ASTRO Phoenix Consensus Conference. Int J Radiat Oncol Biol Phys 65:965–974
National Comprehensive Cancer Network guidelines (2013) http://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Accessed 1 Aug 2013
D’amico AV, Whittington R, Malkowicz SB et al (1998) Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280:969–974
Akakura K, Suzuki H, Ichikawa T et al (2006) A randomized trial comparing radical prostatectomy plus endocrine therapy versus external beam radiotherapy plus endocrine therapy for locally advanced prostate cancer: results at median follow-up of 102 months. Jpn J Clin Oncol 36:789–793
Kuban DA, Tucker SL, Dong L et al (2008) Long-term results of the M. D. Anderson randomized dose-escalation trial for prostate cancer. Int J Radiat Oncol Biol Phys 70:67–74
Kupelian PA (2002) Comparison of the efficacy of local therapies for localized prostate cancer in the prostate-specific antigen era: a large single-institution experience with radical prostatectomy and external-beam radiotherapy. J Clin Oncol 20:3376–3385
Arcangeli G, Strigari L, Arcangeli S et al (2009) Retrospective comparison of external beam radiotherapy and radical prostatectomy in high-risk, clinically localized prostate cancer. Int J Radiat Oncol Biol Phys 75:975–982
Zelefsky MJ, Eastham JA, Cronin AM et al (2010) Metastasis after radical prostatectomy or external beam radiotherapy for patients with clinically localized prostate cancer: a comparison of clinical cohorts adjusted for case mix. J Clin Oncol 28:1508–1513
Sooriakumaran P, Nyberg T, Akre O et al (2014) Comparative effectiveness of radical prostatectomy and radiotherapy in prostate cancer: observational study of mortality outcomes. BMJ 348:g1502
Winkelmayer WC, Kurth T (2004) Propensity scores: help or hype? Nephrol Dial Transplant 19:1671–1673
Hoffman RM, Hunt WC, Gilliland FD et al (2003) Patient satisfaction with treatment decisions for clinically localized prostate carcinoma. Results from the Prostate Cancer Outcomes Study. Cancer 97:1653–1662
Fellin G, Rancati T, Fiorino C et al (2014) Long term rectal function after high-dose prostatecancer radiotherapy: results from a prospective cohort study. Radiother Oncol 110:272–277
Zelefsky MJ, Levin EJ, Hunt M et al (2008) Incidence of late rectal and urinary toxicities after three-dimensional conformal radiotherapy and intensity-modulated radiotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys 70:1124–1129
Guckenberger M, Ok S, Polat B et al (2010) Toxicity after intensity-modulated, image-guided radiotherapy for prostate cancer. Strahlenther Onkol 186:535–543
Ghadjar P, Gwerder N, Manser P et al (2010) High-dose (80 Gy) intensity-modulated radiation therapy with daily image-guidance as primary treatment for localized prostate cancer. Strahlenther Onkol 186:687–692
Razzaghdoust A, Mozdarani H, Mofid B (2014) Famotidine as a radioprotector for rectal mucosa in prostate cancer patients treated with radiotherapy: phase I/II randomized placebo-controlled trial. Strahlenther Onkol 190:739–744
Bolla M, Van Poppel H, Tombal B et al (2012) Postoperative radiotherapy after radical prostatectomy for high-risk prostate cancer: long-term results of a randomised controlled trial (EORTC trial 22911). Lancet 380:2018–2027
Compliance with ethical guidelines
Acknowledgments
This study was supported by Grant No.1010480 from the National Cancer Center, Korea.
Conflict of interest
Y-J. Kim, K.H. Cho, H.R. Pyo, K.H. Lee, S.H. Moon, T.H. Kim, K.H. Shin, J-Y. Kim, Y-K. Kim, and S.B. Lee state that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, YJ., Cho, K., Pyo, H. et al. Radical prostatectomy versus external beam radiotherapy for localized prostate cancer. Strahlenther Onkol 191, 321–329 (2015). https://doi.org/10.1007/s00066-014-0765-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-014-0765-3