Abstract
Background
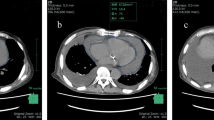
Pericardial effusion (PE) is a common clinical condition that can develop as a result of systemic or cardiac diseases. Here, we report the results of cytology for patients who underwent pericardiocentesis for PE.
Methods
The study comprised 283 patients who underwent primary percutaneous pericardiocentesis between 2007 and 2016. The mean age of the patients was 60.0 ± 16.6 years; 162 (57.2%) were male and 121 (42.8%) were female. The presence of reactive mesothelial cells, acute and chronic inflammatory cells, and/or blood without evidence of malignant cells was considered as benign. The presence of malignant cells with/without reactive mesothelial cells, inflammatory cells, and/or blood was considered as malignant.
Results
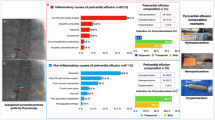
The vast majority of PE specimens (219 cases; 77.4%) were classified as benign. Only 20 cases (7.1%) were classified as atypical, and malignant cells were present in the PE specimens of 44 cases (15.5%). The most common diagnosis was benign PE. The most commonly encountered malignancy was lung cancer. The rate of malignancy was 1.9% in the serous group and 24% in the hemorrhagic group, which was statistically significant.
Conclusion
Benign PE was the most frequent cytological diagnosis in our study. Chronic nonspecific pericarditis was the most frequent type of pericarditis in the benign PE group, while lung adenocarcinoma was the most frequent malignancy in the malignant PE group. The rate of malignancy was significantly higher in the hemorrhagic group than in the serous group.
Zusammenfassung
Hintergrund
Ein Perikarderguss (PE) ist ein häufiges klinisches Ereignis, dass infolge systemischer oder kardialer Erkrankungen auftreten kann. Im vorliegenden Beitrag wird über die zytologischen Ergebnisse von Patienten berichtet, bei denen wegen eines PE eine Perikardpunktion erfolgte.
Methoden
Die Studie umfasste 283 Patienten, bei denen zwischen 2007 und 2016 eine primäre Perikardpunktion durchgeführt wurde. Das Durchschnittsalter der Patienten lag bei 60,0 ± 16,6 Jahren; 162 (57,2 %) Männer und 121 (42,8 %) Frauen. Das Vorliegen reaktiver Mesothelialzellen, akuter und chronischer Entzündungszellen und/oder von Blut ohne Anhalt für maligne Zellen wurde als benigne eingestuft. Das Vorliegen maligner Zellen mit/ohne reaktive Mesothelialzellen, Entzündungszellen und/oder Blut wurde als maligne eingestuft.
Ergebnisse
Die überwiegende Mehrheit der PE-Punktate (219 Fälle; 77,4 %) wurde als benigne klassifiziert. Nur 20 Fälle (7,1 %) wurden als atypisch eingestuft, und in den PE-Punktaten von 44 Fällen (15,5 %) lagen maligne Zellen vor. Die häufigste Diagnose war ein benigner PE. Häufigstes Malignom war das Bronchialkarzinom. Die Malignomrate betrug 1,9 % in der Gruppe mit serösem PE, aber 24 % in der Gruppe mit hämorrhagischem PE, was statistisch signifikant war.
Schlussfolgerung
Ein benigner PE war die häufigste zytologische Diagnose in der vorliegenden Studie. In der Gruppe mit benignem PE kam als häufigster Typ der Perikarditis die chronische nichtspezifische Form vor, während in der Gruppe mit malignem PE das Bronchialkarzinom das häufigste Malignom darstellte. Die Malignomrate war in der Gruppe mit hämorrhagischem PE signifikant höher als in der Gruppe mit serösem PE.
Similar content being viewed by others
Change history
20 July 2017
An erratum to this article has been published.
References
Shabetai R (2004) Pericardial effusion: haemodynamic spectrum. Heart 90:255–256
Shabetai R (1999) Function of the normal pericardium. Clin Cardiol 22:I4–5
Spodick DH (2003) Acute cardiac tamponade. N Engl J Med 349:684–690
Braunwald E (1996) Pericardial disease. In: Braunwald E, Fauci AS, Kasper DL, Hauser SL, Lohr DC, Jameson JL (eds) Principles of Internal Medicine, 14th edn. McGraw-Hill, New York, pp 1334–1341
Imazio M, Adler Y (2013) Management of pericardial effusion. Eur Heart J 34:1186–1197
Syed FF, Ntsekhe M, Mayosi BM (2010) Tailoring diagnosis and management of pericardial disease to the epidemiological setting. Mayo Clin Proc 85:866 (author reply 866)
Imazio M, Cecchi E, Demichelis B et al (2007) Indicators of poor prognosis of acute pericarditis. Circulation 115:2739–2744
Adler Y, Charron P, Imazio M et al (2015) ESC Guidelines for the diagnosis and management of pericardial diseases: The Task Force for the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology (ESC)Endorsed by: The European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J 2015(36):2921–2964
Dragoescu EA, Liu L (2013) Pericardial fluid cytology: an analysis of 128 specimens over a 6-year period. Cancer Cytopathol 121:242–251
He B, Yang Z, Zhao P et al (2017) Cytopathologic analysis of pericardial effusions in 116 cases: Implications for poor prognosis in lung cancer patients with positive interpretations. Diagn Cytopathol 45(4):287–293
Gecmen C, Gecmen GG, Kahyaoglu M et al (2016) Pericardial effusion due to cholesterol pericarditis in case of rheumatoid arthritis. Echocardiography 33:1614–1616
Alexander SJ (1919) A pericardial effusion of “gold paint” appearance due to presence of cholesterin. Br Med J 2:463
Brawley RK, Vasko JS, Monrow AG (1966) Cholesterol pericarditis: consideration of its pathogenesis and treatment. Am J Cardiol 41:235–248
Knobel B, Rosman P (2001) Cholesterol pericarditis associated with rheumatoid arthritis. Harefuah 140:10–12 (87)
Mukai K, Shinkai T, Tominaga K et al (1988) The incidence of secondary tumours of the heart and pericardium: a 10 year study. Jpn J Clin Oncol 18:195–201
Posner MR, Cohen GI, Skarin AT (1981) Pericardial disease in patients with cancer. Am J Med 71:407–413
Wilding G, Green HL, Longo DL et al (1988) Tumours of the heart and pericardium. Cancer Treat Rev 15:165–181
Maisch B, Seferovic PM, Ristic AD et al (2004) Task Force on the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology. Guidelines in the diagnosis and management of pericardial diseases. Eur Heart J 25:587–610
Karatolios K, Pankuweit S, Maisch B (2013) Diagnostic value of biochemical biomarkers in malignant and non-malignant pericardial effusion. Heart Fail Rev 18:337–344
Ma W, Liu J, Zeng Y et al (2012) Causes of moderate to large pericardial effusion requiring pericardiocentesis in 140 Han Chinese patients. Herz 37:183–187
Sagristà-Sauleda J, Mercé J, Permanyer-Miralda G et al (2000) Clinical clues to the causes of large pericardial effusions. Am J Med 109:95–101
Rizzardi C, Barresi E, Brollo A et al (2010) Primary pericardial mesothelioma in an asbestos-exposed patient with previous heart surgery. Anticancer Res 30:1323–1325
Kwon HY, Cho KI, Kim SM et al (2010) A rare case with primary undifferentiated carcinoma of pericardium. J Cardiovasc Ultrasound 18:104–107
Petcu DP, Petcu C, Popescu CF et al (2009) Clinical and cytological correlations in pericardial effusions with cardiac tamponade. Rom J Morphol Embryol 50:251–256
Koss GL, Melamed MR (2006) Effusions in the absence of cancer and effusions in the presence of cancer. In: Koss GL, Melamed MR (eds) Koss’ diagnostic cytology and its histopathologic bases, 5th edn. Lippincott Williams & Wilkins, Philadelphia
Reuter H, Burgess L, van Vuuren W et al (2006) Diagnosing tuberculous pericarditis. QJM 99:827–839
Reynen K, Köckeritz U, Strasser RH (2004) Metastases to the heart. Ann Oncol 15:375–381
Patel J, Sheppard MN (2011) Primary malignant mesothelioma of the pericardium. Cardiovasc Pathol 20:107–109
Thomason R, Schlegel W, Lucca M et al (1994) Primary malignant mesothelioma of the pericardium. Case report and literature review. Tex Heart Inst J 21:170–174
Hillerdal G (1983) Malignant mesothelioma 1982: review of 4710 published cases. Br J Dis Chest 77(4):321–343
Meyers DG, Meyers RE, Prendergast TW (1997) The usefulness of diagnostic tests on pericardial fluid. Chest 111:1213–1221
Colombo A, Olson HG, Egan J et al (1988) Etiology and prognostic implications of a large pericardial effusion in men. Clin Cardiol 11:389–394
Zayas R, Anguita M, Torres F et al (1995) Incidence of specific etiology and role of methods for specific etiologic diagnosis of primary acute pericarditis. Am J Cardiol 75:378–382
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
C. Gecmen, G.G. Gecmen, D. Ece, M. Kahyaoğlu, A. Kalayci, C.Y. Karabay, O. Candan, M.E. Isik, F. Yilmaz, O. Akgun, M. Celik, I.A. Izgi, C. Kirma, S. Keser declare that they have no competing interests.
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Gecmen, C., Gecmen, G.G., Ece, D. et al. Cytopathology of pericardial effusions. Herz 43, 543–547 (2018). https://doi.org/10.1007/s00059-017-4596-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-017-4596-8