Abstract
Objectives
To examine the effects of holiday and weekend admission on in-hospital mortality for patients with acute myocardial infarction (AMI) in China.
Methods
Patients with AMI in 31 tertiary hospitals in Shanxi, China from 2014 to 2017 were included (N = 54,968). Multivariable logistic regression models were used to examine the effects of holiday and weekend admission on in-hospital mortality.
Results
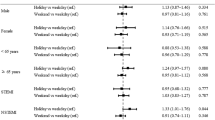
Compared to non-holiday and weekday admissions, holiday and weekend admissions, respectively, were associated with increases in risk-adjusted mortality rates. Chinese National Day was associated with an additional 10 deaths per 1000 admissions (95% confidence interval (CI): (0, 20))—a relative increase from baseline mortality of 64% (95% CI: (1%, 128%)). Sunday was associated with an additional 4 deaths per 1000 admissions (95% CI: (0, 7))—a relative increase from baseline mortality of 23% (95% CI: (3%, 45%)). We found no evidence of gender differences in holiday or weekend effects on mortality.
Conclusions
Holiday and weekend admissions were associated with in-hospital AMI mortality. The admissions on Chinese National Day and Sunday contributed to the observed “holiday effect” and “weekend effect,” respectively.
Similar content being viewed by others
References
Aldridge C, Bion J, Boyal A et al (2016) Weekend specialist intensity and admission mortality in acute hospital trusts in England: a cross-sectional study. Lancet 388:178–186. https://doi.org/10.1016/S0140-6736(16)30442-1
Anselmi L, Meacock R, Kristensen SR et al (2017) Arrival by ambulance explains variation in mortality by time of admission: retrospective study of admissions to hospital following emergency department attendance in England. BMJ Qual Saf 26:613–621. https://doi.org/10.1136/bmjqs-2016-005680
Arellano M (1987) PRACTITIONERS’ CORNER: computing robust standard errors for within-groups estimators*. Oxf Bull Econ Stat 49:431–434. https://doi.org/10.1111/j.1468-0084.1987.mp49004006.x
Becker DJ (2007) Do hospitals provide lower quality care on weekends? Health Serv Res 42:1589–1612. https://doi.org/10.1111/j.1475-6773.2006.00663.x
Bell CM, Redelmeier DA (2001) Mortality among patients admitted to hospitals on weekends as compared with weekdays. N Engl J Med 345:663–668. https://doi.org/10.1056/NEJMsa003376
Bray BD, Steventon A (2017) What have we learnt after 15 years of research into the ‘weekend effect’? BMJ Qual Saf 26:607–610. https://doi.org/10.1136/bmjqs-2016-005793
Cai M, Liu E, Zhang R et al (2020) Comparing the performance of Charlson and Elixhauser comorbidity indices to predict in-hospital mortality among a Chinese population. Clin Epidemiol 12:307–316. https://doi.org/10.2147/CLEP.S241610
Cannon CP (2000) Relationship of symptom-onset-to-balloon time and door-to-balloon time with mortality in patients undergoing angioplasty for acute myocardial infarction. JAMA 283:2941–2947. https://doi.org/10.1001/jama.283.22.2941
Chen H, Shi L, Xue M et al (2018) Geographic variations in in-hospital mortality and use of percutaneous coronary intervention following acute myocardial infarction in China: a nationwide cross-sectional analysis. J Am Heart Assoc 7:e008131. https://doi.org/10.1161/JAHA.117.008131
Chen YF, Armoiry X, Higenbottam C et al (2019) Magnitude and modifiers of the weekend effect in hospital admissions: a systematic review and meta-analysis. BMJ Open 9:e025764. https://doi.org/10.1136/bmjopen-2018-025764
Dowd BE, Greene WH, Norton EC (2014) Computation of standard errors. Health Serv Res 49:731–750. https://doi.org/10.1111/1475-6773.12122
Elixhauser A, Steiner C, Harris DR, Coffey RM (1998) Comorbidity measures for use with administrative data. Med Care 36:8–27
Fedeli U, Gallerani M, Manfredini R (2017) Factors contributing to the weekend effect. JAMA 317:1582. https://doi.org/10.1001/jama.2017.2424
Fiorentino F, Ascenção R, Rosati N (2018) Does acute myocardial infarction kill more people on weekends? Analysis of in-hospital mortality rates for weekend admissions in Portugal. J Health Serv Res Policy 23:87–97. https://doi.org/10.1177/1355819617750687
Geng J, Ye X, Liu C et al (2016) Outcomes of off- and on-hours admission in ST-segment elevation myocardial infarction patients undergoing primary percutaneous coronary intervention. Medicine (Baltimore) 95:e4093. https://doi.org/10.1097/MD.0000000000004093
Han L, Sutton M, Clough S et al (2018) Impact of out-of-hours admission on patient mortality: longitudinal analysis in a tertiary acute hospital. BMJ Qual Saf 27:445–454. https://doi.org/10.1136/bmjqs-2017-006784
Hansen KW, Hvelplund A, Abildstrøm SZ et al (2013) Prognosis and treatment in patients admitted with acute myocardial infarction on weekends and weekdays from 1997 to 2009. Int J Cardiol 168:1167–1173. https://doi.org/10.1016/j.ijcard.2012.11.071
Hong J, Kang H, Yi S-W et al (2006) A comparison of perinatal mortality in Korea on holidays and working days. BJOG An Int J Obstet Gynaecol 113:1235–1238. https://doi.org/10.1111/j.1471-0528.2006.01054.x
Huang H, Chang W, Hsu J et al (2019) Holiday season and weekend effects on stroke mortality: a nationwide cohort study controlling for stroke severity. J Am Heart Assoc 8:e011888. https://doi.org/10.1161/JAHA.118.011888
Isogai T, Yasunaga H, Matsui H et al (2015) Effect of weekend admission for acute myocardial infarction on in-hospital mortality: a retrospective cohort study. Int J Cardiol 179:315–320. https://doi.org/10.1016/j.ijcard.2014.11.070
Jayawardana S, Salas-Vega S, Cornehl F et al (2019) The relationship between off-hours admissions for primary percutaneous coronary intervention, door-to-balloon time and mortality for patients with ST-elevation myocardial infarction in England: a registry-based prospective national cohort study. BMJ Qual Saf. https://doi.org/10.1136/bmjqs-2019-010067
Karaca-Mandic P, Norton EC, Dowd B (2012) Interaction terms in nonlinear models. Health Serv Res 47:255–274. https://doi.org/10.1111/j.1475-6773.2011.01314.x
Kostis WJ, Demissie K, Marcella SW et al (2007) Weekend versus weekday admission and mortality from myocardial infarction. N Engl J Med 356:1099–1109. https://doi.org/10.1056/NEJMoa063355
Lin S-M, Wang J-H, Huang L-K, Huang H-K (2019) Does the ‘Chinese New Year effect’ exist? Hospital mortality in patients admitted to internal medicine departments during official consecutive holidays: a nationwide population-based cohort study. BMJ Open 9:e025762. https://doi.org/10.1136/bmjopen-2018-025762
Mizuno S, Kunisawa S, Sasaki N et al (2018) Effects of night-time and weekend admissions on in-hospital mortality in acute myocardial infarction patients in Japan. PLoS ONE 13:e0191460. https://doi.org/10.1371/journal.pone.0191460
Mohammed M, Faisal M, Richardson D et al (2017) Impact of the level of sickness on higher mortality in emergency medical admissions to hospital at weekends. J Health Serv Res Policy 22:236–242. https://doi.org/10.1177/1355819617720955
Norton EC, Dowd BE (2018) Log odds and the interpretation of logit models. Health Serv Res 53:859–878. https://doi.org/10.1111/1475-6773.12712
Pauls LA, Johnson-Paben R, McGready J et al (2017) The weekend effect in hospitalized patients: a meta-analysis. J Hosp Med 12:760–766. https://doi.org/10.12788/jhm.2815
Shi L, Zhang D, Chen L, Truong KD (2016) “Weekend effect” or “Saturday effect”? An analysis of hospital mortality for patients with ischemic stroke in South Carolina. Circulation 134:1510–1512. https://doi.org/10.1161/CIRCULATIONAHA.116.024535
Smith S, Allan A, Greenlaw N et al (2014) Emergency medical admissions, deaths at weekends and the public holiday effect. Cohort study. Emerg Med J 31:30–34. https://doi.org/10.1136/emermed-2012-201881
Sun J, Girling AJ, Aldridge C et al (2019) Sicker patients account for the weekend mortality effect among adult emergency admissions to a large hospital trust. BMJ Qual Saf 28:223–230. https://doi.org/10.1136/bmjqs-2018-008219
Tang L, Chen P-F, Hu X-Q et al (2017) Effect of Chinese national holidays and weekends versus weekday admission on clinical outcomes in patients with STEMI undergoing primary PCI. J Geriatr Cardiol 14:604–613. https://doi.org/10.11909/j.issn.1671-5411.2017.10.003
Walker AS, Mason A, Quan TP et al (2017) Mortality risks associated with emergency admissions during weekends and public holidays: an analysis of electronic health records. Lancet 390:62–72. https://doi.org/10.1016/S0140-6736(17)30782-1
Wang S, Marquez P, Langenbrunner J et al (2011) Toward a healthy and harmonious life in China: stemming the rising tide of non-communicable diseases. World Bank, Washington
Wang H, Naghavi M, Allen C et al (2016) Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388:1459–1544. https://doi.org/10.1016/S0140-6736(16)31012-1
Zhang X, Khan AA, Haq EU et al (2017) Increasing mortality from ischaemic heart disease in China from 2004 to 2010: disproportionate rise in rural areas and elderly subjects. 438 million person-years follow-up. Eur Hear J Qual Care Clin Outcomes 3:47–52. https://doi.org/10.1093/ehjqcco/qcw041
Acknowledgments
This work was supported by National Natural Science Foundation of China [Grant Number: 71473099]. We thank the Health Commission in Shanxi for providing us with the data used in this study. We are grateful to Prof Carine Ronsmans, Prof Chaojie Liu, Dr. Lu Shi, Chang Xu, Ziling Ni, and Wei Lu for invaluable discussions, suggestions and comments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional research committee (the Ethics Committee of Tongji Medical College, Huazhong University of Science and Technology, IORG No.: IORG0003571) and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
The requirement for informed consent for this study was exempted because all patient data were de identified.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lin, X., Green, J.C., Xian, H. et al. Holiday and weekend effects on mortality for acute myocardial infarction in Shanxi, China: a cross-sectional study. Int J Public Health 65, 847–857 (2020). https://doi.org/10.1007/s00038-020-01443-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-020-01443-x