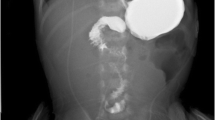
Abstract
Congenital anomalies of the bowel can affect any portion of the gastrointestinal tract. Bowel atresia and stenosis concern abnormal closure, discontinuity or narrowing from the duodenum to sigmoid colon, and the incidence is about 2/10,000 live births. The pathogenesis was previously believed to be an embryologic trouble of bowel recanalization or a disruption compromising small bowel vascular supply, but new genetic hypothesis emerges since a few years to explain the occurrence of bowel atresia and stenosis.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Hemming V, Rankin J. Small intestinal atresia in a defined population: occurrence, prenatal diagnosis and survival. Prenat Diagn. 2007;27:1205–11.
Nichol PF, Reeder A, Botham R. Humans, mice, and mechanisms of intestinal atresias: a window into understanding early intestinal development. J Gastrointest Surg. 2011;15:694–700.
Best KE, Tennant PWG, Addor MC, et al. Epidemiology of small intestinal atresia in Europe: a register-based study. Arch Dis Child Fetal Neonatal Ed. 2012;97:F353–8.
Tandler J. Zur Entwicklungsgeschichte des Menschlichen Duodenum in Frühen Embryonal Stadien. Gegenbaurs Morphol Jahrb. 1900;29:187–216.
Santulli TV, Blanc WA. Congenital atresia of the intestine: pathogenesis and treatment. Ann Surg. 1961;154:939–48.
Clogg HS. Congenital intestinal atresia. Lancet. 1904;164:P1770–4.
Louw JH, Barnard CN. Congenital intestinal atresia: observations on its origin. Lancet. 1955;2:1065–7.
Baglaj M, Carachi R, Lawther S. Multiple atresia of the small intestine: a 20-year review. Eur J Pediatr Surg. 2008;18:13–8.
Pavri DR, Marshall DG, Armstrong RF, et al. Intrauterine intussusception: case report and literature review. Can J Surg. 1983;26:376–8.
Romeo C, Arena F, Impellizzeri G. Intrauterine intussusception, rare cause of intestinal atresia: case report. It J Ped Surg Sci. 1994;8:157–60.
Kilic N, Kiristioglu I, Kirkpinar A, et al. A very rare cause of intestinal atresia: intrauterine intussusception due to Meckel's diverticulum. Acta Paediatr. 2003;92:756–7.
Pueyo C, Maldonado J, Royo Y, et al. Intrauterine intussusception: a rare cause of intestinal atresia. J Pediatr Surg. 2009;44:2028–30.
Lewis MP, Emberton M, Owen ER, et al. Delayed presentation of intestinal atresia and intussusception. a case report and literature review. Eur J Pediatr Surg. 1993;3:296–8.
Chiari H. Über eine intrauterin entstandene und von Darmatresie gefolgte Intussusception des lleums. Prag Med Wschr. 1888;13:399–401.
Guttman FM, Braun P, Garance PH, et al. Multiple atresias and a new syndrome of hereditary multiple atresias involving the gastrointestinal tract from stomach to rectum. J Pediatr Surg. 1973;8:633–40.
Puri P, Fujimoto T. New observations on the pathogenesis of multiple intestinal atresias. J Pediatr Surg. 1988;23:221–5.
Cole C, Freitas A, Clifton MS, et al. Hereditary multiple intestinal atresias: 2 new cases and review of the literature. J Pediatr Surg. 2010;45:E21–4.
Bilodeau A, Prasil P, Cloutier R, et al. Hereditary multiple intestinal atresia: thirty years later. J Pediatr Surg. 2004;39:726–30.
Robinson I, Gill H, Ng LY, et al. Familial distal foregut atresia in a family with likely autosomal dominant inheritance pattern. Pediatr Surg Int. 2012;28:1151–5.
Fourcade L, Shima H, Miyazaki E, et al. Multiple gastrointestinal atresias result from disturbed morphogenesis. Pediatr Surg Int. 2001;17:361–4.
Cheng W, Tam PK. Murine duodenum does not go through a “solid core” stage in its embryological development. Eur J Pediatr Surg. 1998;8:212–5.
Ornitz DM, Itoh N. Fibroblast growth factors. Genome Biol. 2001;2:1–9.
Fairbanks TJ, Sala FG, Kanard R, et al. The fibroblast growth factor pathway serves a regulatory role in proliferation and apoptosis in the pathogenesis of intestinal atresia. J Pediatr Surg. 2006;41:132–6.
Ramalho-Santos M, Melton DA, McMahon AP. Hedgehog signals regulate multiple aspects of gastrointestinal development. Development. 2000;127:2763–72.
Gao N, White P, Kaestner KH. Establishment of intestinal identity and epithelial-mesenchymal signaling by Cdx2. Dev Cell. 2009;16:588–99.
Johnson SM, Meyers RL. Inherited thrombophilia: a possible cause of in utero vascular thrombosis in children with intestinal atresia. J Pediatr Surg. 2001;36:1146–9.
Gupta T, Yang W, Iovannisci DM, et al. Considering the vascular hypothesis for the pathogenesis of small intestinal atresia: a case control study of genetic factors. Am J Med Genet A. 2013;161:702–10.
Werler MM, Sheehan JE, Mitchell AA. Maternal medication use and risks of gastroschisis and small intestinal atresia. Am J Epidemiol. 2002;155:26–31.
Milla PJ. Feeding, tasting, and sucking. In: Walker-Smith WA, Watkins JB, editors. Pediatric gastrointestinal disease. Philadelphia: BC Decker; 1991. p. 217–23.
Gross RE. The surgery of infancy and childhood. Philadelphia: WB Saunders Co; 1953. p. 150–66.
Gray SW, Skandalakis JE. Embryology for surgeons. Philadelphia, PA: WB Saunders Co; 1972. p. 147–8.
Grosfeld JL, Ballantine TVN, Shoemaker R. Operative management of intestinal atresia and stenosis based on pathologic findings. J Pediatr Surg. 1979;14:368–75.
Escobar MA, Ladd AP, Grosfeld JL, et al. Duodenal atresia and stenosis: long-term follow-up over 30 years. J Pediatr Surg. 2004;39:867–71.
Dalla Vecchia LK, Grosfeld JL, West KW, et al. Intestinal atresia and stenosis: a 25-year experience with 277 cases. Arch Surg. 1998;133:490–7.
Nusinovich Y, Revenis M, Torres C. Long-term outcomes for infants with intestinal atresia studied at Children’s National Medical Center. J Pediatr Gastroenterol Nutr. 2013;57:324–9.
St. Peter SD, Little DC, Barsness KA, et al. Should we be concerned about jejunoileal atresia during repair of duodenal atresia? J Laparoendosc Adv Surg Tech A. 2010;20:773–5.
Kimura K. Diamond-shaped anastomosis for duodenal atresia: an experience with 44 patients over 15 years. J Pediatr Surg. 1990;25:977–8.
Bax NMA, Ure BM, Van der Zee DC, et al. Laparoscopic duodenoduodenostomy for duodenal atresia. Surg Endosc. 2001;15:217.
Kay S, Yoder S, Rothenberg S. Laparoscopic duodenoduodenostomy in the neonate. J Pediatr Surg. 2009;44:906–8.
Mentessidou A, Saxena AK. Laparoscopic repair of duodenal atresia: systematic review and meta-analysis. World J Surg. 2017;41:2178–84.
Chiarenza SF, Bucci V, Conighi ML, et al. Duodenal atresia: open versus MIS repair-analysis of our experience over the last 12 years. Biomed Res Int. 2017;2017:7.
Van der Zee DC. Laparoscopic repair of duodenal atresia: revisited. World J Surg. 2011;35:1781–4.
Valusek PA, Spilde TL, Tsao K, et al. Laparoscopic duodenal atresia repair using surgical U-clips: a novel technique. Surg Endosc. 2007;21:1023–4.
Parmentier B, Peycelon M, Muller CO, et al. Laparoscopic management of congenital duodenal atresia or stenosis: a single center early experience. J Pediatr Surg. 2015;50:1833–6.
Spilde TL, St. Peter SD, Keckler SJ, et al. Open vs laparoscopic repair of congenital duodenal obstructions: a concurrent series. J Pediatr Surg. 2008;43:1002–5.
Hill S, Koontz CS, Langness SM, et al. Laparoscopic versus open repair of congenital duodenal obstruction in infant. J Laparoendosc Adv Surg Tech A. 2011;21:961–3.
Jensen AR, Short SS, Anselmo DM, et al. Laparoscopic versus open treatment of congenital duodenal obstruction: multicenter short-term outcomes analysis. J Laparoendosc Adv Surg Tech A. 2013;23:876–80.
Okamatsu T, Arai K, Yatsuzuka M, et al. Endoscopic membranectomy for congenital duodenal stenosis in an infant. J Pediatr Surg. 1989;24:367–8.
Ziegler K, Schier F, Waldschmidt J. Endoscopic laser resection of a duodenal membrane. J Pediatr Surg. 1992;27:1582–3.
Van Rijn RR, Van Lienden KP, Fortuna TL, et al. Membranous duodenal stenosis: initial experience with balloon dilatation in four children. Eur J Radiol. 2006;59:29–32.
Torroni F, De Angelis P, Caldaro T, et al. Endoscopic membranectomy of duodenal diaphragm: pediatric experience. Gastrointest Endosc. 2006;63:530–1.
Barabino A, Gandullia P, Arrigo S, et al. Successful endoscopic treatment of a double duodenal web in an infant. Gastrointest Endosc. 2011;73:401–2.
Bittencourt PFS, Malheiros RS, Ferreira AR, et al. Endoscopic treatment of congenital duodenal membrane. Gastrointest Endosc. 2012;76:1273–5.
Di Maio CJ, Kamal N, Hogan CM, et al. Pediatric therapeutic endoscopy: endoscopic management of a congenital duodenal web. Gastrointest Endosc. 2014;80:166–7.
Bleve C, Costa L, Bertoncello V, et al. Endoscopic resection of a duodenal web in an 11-month-old infant with multiple malformations. Endoscopy. 2015;47:E210–1.
Huang MH, Bian HQ, Liang C, et al. Gastroscopic treatment of membranous duodenal stenosis in infants and children: report of 6 cases. J Pediatr Surg. 2015;50:413–6.
Poddar U, Jain V, Yachha SK, et al. Congenital duodenal web: successful management with endoscopic dilatation. Endosc Int Open. 2016;4:E238–41.
Virgone C, D’Antonio F, Khalil A, et al. Accuracy of prenatal ultrasound in detecting jejunal and ileal atresia: systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2015;45:523–9.
John R, D’Antonio F, Khalil A, et al. Diagnostic accuracy of prenatal ultrasound in identifying jejunal and ileal atresia. Fetal Diagn Ther. 2015;38:142–6.
Goruppi I, Arevalo S, Gander R, et al. Role of intraluminal bowel echogenicity on prenatal ultrasounds to determine the anatomical level of intestinal atresia. J Matern Fetal Neonatal Med. 2017;30:103–8.
Sammour RN, Leibovitz Z, Degani S, et al. Prenatal diagnosis of small-bowel volvulus using 3-dimensional doppler sonography. J Ultrasound Med. 2008;27:1655–61.
Ozguner IF, Savas C, Ozguner M, et al. Intestinal atresia with segmental musculature and neural defect. J Pediatr Surg. 2005;40:1232–7.
Gfroerer S, Metzger R, Fiegel H, et al. Changes of smooth muscle contractile filaments in small bowel atresia. World J Gastroenterol. 2010;16:5716–21.
Wang X, Yuan C, Xiang L, et al. The clinical significance of pathological studies of congenital intestinal atresia. J Pediatr Surg. 2013;48:2084–91.
Louw JH. Resection and end-to-end anastomosis in the management of atresia and stenosis of the small bowel. Surgery. 1967;62:940–50.
Martin LW, Zerella JT. Jejunoileal atresia: a proposed classification. J Pediatr Surg. 1976;11:399–403.
Stollman TH, de Blaauw I, Wijnen MHWA, et al. Decreased mortality but increased morbidity in neonates with jejunoileal atresia; a study of 114 cases over a 34-year period. J Pediatr Surg. 2009;44:217–21.
Tsuji Y, Maeda K, Ono S, et al. A new paradigm of scarless abdominal surgery in children: transumbilical minimal incision surgery. J Pediatr Surg. 2014;49:1605–9.
Sawai T, Yonekura T, Yamauchi K, et al. A novel approach to neonatal abdominal surgery via a circular incision around the umbilical cord. Pediatr Surg Int. 2016;32:1009–11.
Lima M, Ruggieri G, Domini M, et al. Evolution of the surgical management of bowel atresia in newborn: laparoscopically assisted treatment. Pediatr Med Chir. 2009;31:215–9.
Abhyankar A, Mukhtar Z. Laparoscopy-assisted surgery for neonatal intestinal atresia: single-center experience. Asian J Endosc Surg. 2011;4:90–3.
Li B, Chen WB. Laparoscopy-assisted surgery for neonatal intestinal atresia and stenosis: a report of 35 cases. Pediatr Surg Int. 2012;28:1225–8.
Fockens P. Ein operativ geheilter Fall von Kongenitaler Dünndarmatresie. Zentralbl Chir. 1911;38:532–5.
von Mikulicz J. Chirurgische Erfahrungen über das Darmcarcinom. Arch Klin Chir. 1903;69:28–47.
Willital GH. Atlas der Kinderchirurgie. Indikationen und Operationstechnik. Stuttgart: Schattauer Verlag; 1981. p. 115.
Bishop HC, Koop CE. Management of meconium ileus: resection, Roux-en-y anastomosis and ileostomy irrigation with pancreatic enzymes. Ann Surg. 1957;145:410–4.
Kumaran N, Shankar KR, Lloyd DA, et al. Trends in the management and outcome of jejuno-ileal atresia. Eur J Pediatr Surg. 2002;12:163–7.
Wit J, Sellin S, Degenhardt P, et al. Is the Bishop-Koop anastomosis in treatment of neonatal ileus still current? Chirurg. 2000;71:307–10.
Levy E, Palmer DL, Frileux P, et al. Inhibition of upper gastrointestinal secretions by reinfusion of succus entericus into the distal small bowel. A clinical study of 30 patients with peritonitis and temporary enterostomy. Ann Surg. 1983;198:596–600.
Richardson L, Banerjee S, Rabe H. What is the evidence on the practice of mucous fistula refeeding in neonates with short bowel syndrome? J Pediatr Gastroenterol Nutr. 2006;43:267–70.
Wong KKY, Lan LCL, Lin SCL, et al. Mucous fistula refeeding in premature neonates with enterostomies. J Pediatr Gastroenterol Nutr. 2004;39:43–5.
Sato S, Nishijima E, Muraji T, et al. Jejunoileal atresia: a 27-year experience. J Pediatr Surg. 1998;33:1633–5.
Wang J, Du L, Cai W, et al. Prolonged feeding difficulties after surgical correction of intestinal atresia: a 13-year experience. J Pediatr Surg. 2014;49:1593–7.
Webb CH, Wangsteen OH. Congenital intestinal atresia. Am J Dis Child. 1931;41:262–84.
England RJ, Scammel S, Murthy GV. Proximal colonic atresia: is right hemicolectomy inevitable? Pediatr Surg Int. 2011;27:1059–62.
Etensel B, Temir G, Karkiner A, et al. Atresia of colon. J Pediatr Surg. 2005;40:1258–68.
Haxhija EQ, Schalamon J, Höllwarth ME. Management of isolated and associated colonic atresia. Pediatr Surg Int. 2011;27:411–6.
Mirza B, Iqbal S, Ijaz L. Colonic atresia and stenosis: our experience. J Neonatal Surg. 2012;1(1):4.
Ruggieri G, Libri M, Gargano T, et al. Congenital colonic stenosis: a case of late-onset. Pediatr Med Chir. 2009;31:130–3.
Guo JB, Li ZZ. A case report of congenital colonic stenosis. Chin J Contemp Pediatr. 2009;11:699–700.
Saha N, Talukder SA, Alam S. Congenital stenosis in the descending colon causing intestinal obstruction in a one and half years male child. Mymensingh Med J. 2013;22:574–7.
Zambaiti E, Chiaramonte C, Salemo S, et al. Multiple congenital colonic stenosis: a rare gastrointestinal malformation. Case Rep Pediatr. 2016;2016:4.
Acknowledgements
Thank you to Olivier Reinberg for reviewing this chapter.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Varlet, F., Vermersch, S., Scalabre, A. (2019). Bowel Atresia and Stenosis. In: Lima, M., Reinberg, O. (eds) Neonatal Surgery. Springer, Cham. https://doi.org/10.1007/978-3-319-93534-8_18
Download citation
DOI: https://doi.org/10.1007/978-3-319-93534-8_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-93532-4
Online ISBN: 978-3-319-93534-8
eBook Packages: MedicineMedicine (R0)