Abstract
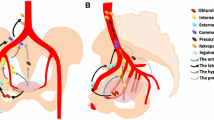
The spread of pelvic tumors to loco-regional lymph nodes is an important means of tumor dissemination. Nodal metastases have therapeutic implications for prognosis and management. Pelvic tumors usually metastasize first to regional lymph nodes, which are specific groups of nodes for each type of tumor, and are classified according to the TNM system as N-stage disease (TNM classification of malignant tumors, Oxford, 2009). If a pelvic tumor metastasize to a lymph node outside of the defined regional nodes, this is considered M-stage disease, which may in turn affect the patient’s treatment options and prognosis. Thus, exact knowledge of the regional pelvic lymph node spread of each tumor located within the small pelvis is essential for diagnostic purposes, surgical treatment options, tumor staging and follow-up strategies. A key element in assessing each patient is the correct and precise anatomical description of pelvic nodal metastases to facilitate proper staging and treatment. In the present overview pelvic lymph node anatomy and nomenclature are reviewed with schematic illustrations.
Similar content being viewed by others
References
Sobin L, Gospodarowicz M, Wittekind C, editors. TNM classification of malignant tumors. 7th ed. Oxford: Wiley-Blackwell; 2009.
Baluk P, Fuxe J, Hashizume H, et al. Functionally specialized junctions between endothelial cells of lymphatic vessels. J Exp Med. 2007;204:2349–62.
Gerli R, Ibba L, Fruschelli C. A fibrillar elastic apparatus around human lymph capillaries. Anat Embryol (Berl). 1990;181:281–6.
Zawieja D. Lymphatic biology and the microcirculation: past, present and future. Microcirculation. 2005;12:141–50.
Weiss L, Schmid-Schonbein GW. Biomechanical interactions of cancer cells with the microvasculature during metastasis. Cell Biophys. 1989;14:187–215.
Cueni LN, Detmar M. The lymphatic system in health and disease. Lymphat Res Biol. 2008;6:109–22.
Brown P. Lymphatic system: unlocking the drains. Nature. 2005;436:456–8.
Karpanen T, Egeblad M, Karkkainen MJ, et al. Vascular endothelial growth factor C promotes tumor lymphangiogenesis and intralymphatic tumor growth. Cancer Res. 2001;61:1786–90.
Cuneo B, Marcille BM. Topographie des ganglions iliopelviens. Bull Mem Soc Anat Paris. 1901;86:653–63.
Gray H. The lymphatics of the abdomen and pelvis. In: Gray’s anatomy. 20th ed. New York: Bartlebycom; 1918. http://bartlebycom/107/180/html.
Lengele B, Hamoir M, Scalliet P, Gregoire V. Anatomical bases for the radiological delineation of lymph node areas. Major collecting trunks, head and neck. Radiother Oncol. 2007;85:146–55.
Poirier P, Cunéo B, Delamere G. The lymphatics. Westminster: Archibald Constable; 1903.
Warwick R, Williams P. Topography of the lymph nodes and vessels. In: Gray’s anatomy. Edinburgh: Longman; 1973. p. 727–44.
Plentl A, Friedman E. Lymphatic system of the female genitalia. The morphologic basis of oncologic diagnosis and therapy. Philadelphia: Saunders; 1971.
Whitemore I. Lymphoid system. In: Federative commitee on anatomical terminology—terminologica anatomica. Stuttgart: Thieme Verlag; 1998.
Sappey P. Des vaisseaux lymphatiques. In: Delahaye A, Lecrosnier E, editors. Traité d’anatomie descriptive, vol. 2. Paris; 1888. p. 731–842.
Henriksen E. The lymphatic spread of carcinoma of the cervix and of the body of the uterus; a study of 420 necropsies. Am J Obstet Gynecol. 1949;58:924–42.
Rouvière H, Tobias M. Anatomy of the human lymphatic system. Ann Arbor: Edward; 1938.
Smith JA Jr, Whitmore WF Jr. Regional lymph node metastasis from bladder cancer. J Urol. 1981;126:591–3.
Roth B, Wissmeyer MP, Zehnder P, et al. A new multimodality technique accurately maps the primary lymphatic landing sites of the bladder. Eur Urol. 2010;57:205–11.
Thoeny HC, Ross BD. Predicting and monitoring cancer treatment response with diffusion-weighted MRI. J Magn Reson Imaging. 2010;32:2–16.
Ganswindt U, Schilling D, Muller AC, Bares R, Bartenstein P, Belka C. Distribution of prostate sentinel nodes: a SPECT-derived anatomic atlas. Int J Radiat Oncol Biol Phys. 2011;79:1364–72.
Hegemann NS, Wenter V, Spath S, Kusumo N, Li M, Bartenstein P, Fendler WP, Stief C, Belka C, Ganswindt U. Distribution of prostate nodes: a PET/CT-derived anatomic atlas of prostate cancer patients before and after surgical treatment. Radiat Oncol. 2016;11:37. https://doi.org/10.1186/s13014-016-0615-9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Schumacher, M.C. (2018). Surgical Anatomy of Pelvic Lymph Nodes. In: John, H., Wiklund, P. (eds) Robotic Urology. Springer, Cham. https://doi.org/10.1007/978-3-319-65864-3_11
Download citation
DOI: https://doi.org/10.1007/978-3-319-65864-3_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-65863-6
Online ISBN: 978-3-319-65864-3
eBook Packages: MedicineMedicine (R0)