Abstract
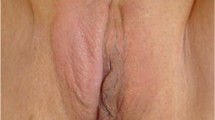
Acute and chronic vulvar conditions are noted in women throughout their life span. Several of these conditions, such as vulvar infections and intraepithelial neoplasia, have well-defined clinical pathways of treatment utilizing pharmacologic interventions that have been vetted through clinical trials. Others, such as vulvodynia, a chronic pain condition that has been recognized for over 100 years, continue to perplex clinicians regarding best options for pharmacologic intervention. This chapter will review the spectrum of pharmacologic interventions used in various vulvar conditions, with an emphasis on the ones used in the management of vulvodynia. Vulvodynia will be highlighted as it is a vulvar condition clinicians treat with scant data from clinical trials.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
American College of Obstetricians and Gynecologists. Vulvar disorders. ACOG clinical updates in women’s health care. VIII ed. Washington, DC: ACOG; 2010. p. 36.
Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2015. MMWR Recomm Rep. 2015;64(RR-3):1–137.
Portman DJ, Gass ML, Vulvovaginal Atrophy Terminology Consensus Conference Panel. Genitourinary syndrome of menopause: new terminology for vulvovaginal atrophy from the International Society for the Study of a Women’s sexual health and the North American Menopause Society. Menopause. 2014;10:1063–8.
Danby CS, Margesson LJ. Approach to the diagnosis and treatment of vulvar pain. Dermatol Ther. 2010;23:485–504.
Shifren JL, Gass ML. The North American Menopause Society recommendations for clinical care of midlife women. Menopause. 2014;21(10):1038–62.
Bornstein J, Goldstein AT, Stockdale CK, et al. 2015 ISSVD, ISSWSH and IPPS consensus terminology and classification of persistent vulvar pain and Vulvodynia. Obstet Gynecol. 2016;127(4):745–51.
Harlow BL, Kunitz CG, Nguyen RHN, Rydell SA, Turner RM, MacLehose RF. Prevalence of symptoms consistent with a diagnosis of vulvodynia: population-based estimates from 2 geographic regions. Am J Obstet Gynecol. 2014;210:40.e1–8.
Jasmin L, Tien D, Janni G, et al. Is noradrenaline a significant factor in the analgesic effect of antidepressants? Pain. 2003;106:3–8.
Foster DC, Kotok MB, Huang L, et al. Oral desipramine and topical lidocaine for vulvodynia: a randomized controlled trial. Obstet Gynecol. 2010;116:583–93.
Brown CS, Wan J, Bachmann G, et al. Self-management, amitriptyline, and amitriptyline plus triamcinolone in the management of vulvodynia. J Women’s Health. 2009;18:163–9.
Reed BD, Caron AM, Gorenflo DW, et al. Treatment of vulvodynia with tricyclic antidepressants: efficacy and associated factors. J Low Genit Tract Dis. 2006;10:245–51.
De Andres J, Sanchis-Lopez N, Asensio-Samper JM, et al. Vulvodynia—an evidence-based literature review and proposed treatment algorithm. Pain Pract. 2015;16(2):204–36.
Pagano R, Wong S. Use of amitriptyline cream in the management of entry dyspareunia due to provoked vestibulodynia. J Low Genit Tract Dis. 2012;16:394–7.
Nyirjesy P, Lev-Sagie A, Mathew L, Culhane JF. Topical amitriptyline-baclofen cream for the treatment of provoked vestibulodynia. J Low Genit Tract Dis. 2009;13:230–6.
Rogawski MA, Loscher W. The neurobiology of antiepileptic drugs for the treatment of nonepileptic conditions. Nat Med. 2004;10:685–92.
Boardman LA, Cooper AS, Blais LR, Raker CA. Topical gabapentin in the treatment of localized and generalized vulvodynia. Obstet Gynecol. 2008;112:579–85.
Brown CS, Foster DC, Wan JY, Rawlinson L, Bachmann GA, GABA Study Group. Rationale and design of a multicenter randomized clinical trial of extended release gabapentin in provoked vestibulodynia and biological correlates of response. Contemp Clin Trials. 2013;36:154–65.
Cummins TR. Setting up for the block: the mechanism underlying lidocaine’s use-dependent inhibition of sodium channels. J Physiol. 2007;582(Pt 1):11.
Zolnoun DA, Hartmann KE, Steege JF. Overnight 5% lidocaine ointment for treatment of vulvar vestibulitis. Obstet Gynecol. 2003;102:84–7.
Danielsson I, Torstensson T, Brodda-Jansen G, Bohm-Starke N. EMG biofeedback versus topical lidocaine gel: a randomized study for the treatment of women with vulvar vestibulitis. Acta Obstet Gynecol Scan. 2006;85:1360–7.
Rapkin AJ, McDonald JS, Morgan M. Multilevel local anesthetic nerve blockade for the treatment of vulvar vestibulitis syndrome. Amer J Obstet Gynecol. 2008;198:41.e1–5.
McDonald JS, Rapkin AJ. Multilevel local anesthetic nerve blockade for the treatment of generalized vulvodynia: a pilot study. J Sex Med. 2012;9:2919–26.
Murina F, Tassan P, Roberti P, Bianco V. Treatment of vulvar vestibulitis with submucous infiltrations of methylprednisolone and lidocaine: an alternative approach. J Reprod Med. 2001;46:713–6.
Tympanidis P, Casula MA, Yiangou Y, Terenghi G, Dowd P, Anand P. Increased vanilloid receptor VR1 innervation in vulvodynia. Eur J Pain. 2004;8:129–33.
Murina F, Radici G, Bianco V. Capsaicin and the treatment of vulvar vestibulitis syndrome: a valuable alternative? Med Gen Med. 2004;6:48.
Cui M, Khanijou S, Rubino J, Aoki KR. Subcutaneous administration of botulinum toxin a reduces formalin-induced pain. Pain. 2004;107:125–33.
Petersen CD, Giraldi A, Lundvall L, Kristensen E. Botulinum toxin type A—a novel treatment for provoked vestibulodynia? Results from a randomized, placebo controlled, double blinded study. J Sex Med. 2009;6:2523–37.
Pelletier F, Parratte B, Penze S, Moreno JP, Aubin F, Humbert P. Efficacy of high doses of botulinum toxin a for treating provoked vestibulodynia. Brit J Dermatol. 2011;164:617–22.
Foster DC, Hadsday JD. Elevated tissue levels of interleukin-1 beta and tumor necrosis factor-alpha in vulvar vestibulitis. Obstet Gynecol. 1997;89:291–6.
Snyder DS, Unanue ER. Corticosteroids inhibit murine macrophage 1a expression and interleukin 1 production. J Immunol. 1982;129:1803–5.
Munday PE. Treatment of vulval vestibulitis with a potent topical steroid. Sex Transm Infect. 2004;80:154–5.
Desrochers G, Bergeron S, Khalife S, Dupuis M-J, Jodoin M. Provoked vestibulodynia: psychological predictors of topical and cognitive-behavioral treatment outcome. Behav Res Ther. 2010;48:106–15.
Kieseier BC. The mechanism of action of interferon-β in relapsing multiple sclerosis. CNS Drugs. 2011;25:491–502.
Bornstein J, Abramovici H. Combination of subtotal perineoplasty and interferon for the treatment of vulvar vestibulitis. Gynecol Obstet Investig. 1997;44:53–6.
Marinoff SC, Turner ML, Hirsch RP, Richard G. Intralesional alpha interferon: cost effective therapy for vulvar vestibulitis syndrome. J Reprod Med. 1993;38:19–24.
Nyirjesy P, Sobel JD, Weitz MV, Leaman DJ, Small MJ, Gelone SP. Cromolyn cream for recalcitrant idiopathic vulvar vestibulitis: results of a placebo-controlled study. Sex Transm Inf. 2001;77:53–7.
Donders GG, Bellen G. Cream with cutaneous fibroblast lysate for the treatment of provoked vestibulodynia: a double-blind randomized placebo-controlled crossover study. J Lower Genital Tract Dis. 2012;16:427–36.
Kamdar N, Fisher L, MacNeill C. Improvement in vulvar vestibulitis with montelukast. J Reprod Med. 2007;52:912–6.
Farajun Y, Zarfati D, Abramov L, Livoff A, Bornstein J. Enoxaparin treatment of vulvodynia. A randomized controlled trial. Obstet Gynecol. 2012;120:565–73.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Brown, C.S., Bachour, C.C., Bachmann, G.A. (2019). Principles of Medical Treatment. In: Bornstein, J. (eds) Vulvar Disease. Springer, Cham. https://doi.org/10.1007/978-3-319-61621-6_6
Download citation
DOI: https://doi.org/10.1007/978-3-319-61621-6_6
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-61620-9
Online ISBN: 978-3-319-61621-6
eBook Packages: MedicineMedicine (R0)