Abstract
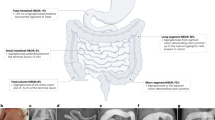
Hirschsprung’s disease (HD) or “congenital megacolon” is a congenital developmental disorder characterized by the absence of ganglion cells in the distal intestine with variable proximal extension. HD affects approximately 1 / 5,000 live births and is more common in males (M: F = 4: 1). According to the proximal extension is possible to indentify different forms of HD: ultrashort, short segment or classical form, long segment and total colonic aganglia. Most children with HD (50-90%) are diagnosed in the neonatal period. Typically the infant with HD is born at term and present with failure to pass meconium.When there is a clinical suspicion of HD, diagnostic investigations to be performed include: radiologic evaluation (plain radiographs, barium enema), anorectal manometry, rectal full-thickness biopsy or serum-muscle and / or rectal biopsy by suction (Rectal Suction biopsy - RSB).There are numerous surgical techniques described for the treatment of HD. The most commonly performed, and therefore considered “the major pull-through procedures”, are: Swenson rectosigmoidectomy, Duhamel retrorectal transanal pull-through, Rehbein pull-through with anterior colorectal anastomosis, Soave rectosigmoidectomy with aseptic endorectal colon pull-through.Early postoperative complication is represented by colo-anal anastomosis dehiscence (3.2%) which, if not massive, is solvable conservatively. Late postoperative complications are HAEC and colo-anal anastomosis stenosis.On rare occasions the child may require a RedoPT procedure. Indication for RedoPT in the recent review was most commonly for a retained aganglionosis/transition zone pathology (RA/TZP; 71% overall ). Other indications included stricture/obstructing Duhamel pouch (19%), excessively tight cuff (8%), twisted-PT (4%). Operative approach can vary widely and is heavily dependent on type of complication, underlying pathology, previous surgical history as well as surgeon preference as to the type of repair. Complications are quite similar after redo-PT compared to primary PT in experienced hands but stooling outcomes are significantly worse compared to those after a primaryPT. Importantly, continence is still retained in the majority of children.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Holschneider AM, Puri P (2000) Hirschsprung’s disease and allied disorders, 2nd edn. Springer, New York
Georgeson KE, Robertson DJ (2004) Laparoscopic-assisted approaches for the definitive surgery for Hirschsprung’s disease. Semin Pediatr Surg 13:256–262
Ruggeri G, Libri M, Randi B (2012) Morbo di Hirschsprung. In: Lima M (ed) Chirurgia Endoscopica e Mini-Invasiva Pediatrica. Clueb, Bologna
Swenson O, Bill AH Jr (1948) Resection of rectum and rectosigmoid with preservation of the sphincter for benign spastic lesions producing megacolon; an experimental study. Surgery 24(2):212–220
Raveenthiran V (2011) Knowledge of ancient Hindu surgeons on Hirschsprung disease: evidence from Sushruta Samhita of circa 1200–600 BC. J Pediatr Surg 46(11):2204–2208
Coe A, Collins MH, Lawal T, Louden E, Levitt MA, Pena A (2012) Reoperation for Hirschsprung disease: pathology of the resected problematic distal pull-through. Pediatr Dev Pathol Off J Soc Pediatr Pathol Paediatr Pathol Soc 15(1):30–38
Levitt MA, Dickie B, Pena A (2012) The Hirschsprungs patient who is soiling after what was considered a “successful” pull-through. Semin Pediatr Surg 21(4):344–353
Minford JL, Ram A, Turnock RR, Lamont GL, Kenny SE, Rintala RJ et al (2004) Comparison of functional outcomes of Duhamel and transanal endorectal coloanal anastomosis for Hirschsprung’s disease. J Pediatr Surg 39(2):161–165; discussion −5
Saleh W, Rasheed K, Mohaidly MA, Kfoury H, Tariq M, Rawaf AA (2004) Management of Hirschsprung’s disease: a comparison of Soave’s and Duhamel’s pull-through methods. Pediatr Surg Int 20(8):590–593
Craigie RJ, Conway SJ, Cooper L, Turnock RR, Lamont GL, Baillie CT et al (2007) Primary pull-through for Hirschsprung’s disease: comparison of open and laparoscopic-assisted procedures. J Laparoendosc Adv Surg Tech A 17(6):809–812
Ralls MW, Freeman JJ, Rabah R, Coran AG, Ehrlich PF, Hirschl RB et al (2014) Redo pull-through for Hirschsprung disease: a single surgical group’s experience. J Pediatr Surg 49(9):1394–1399
Murphy F, Puri P (2005) New insights into the pathogenesis of Hirschsprung’s associated enterocolitis. Pediatr Surg Int 21(10):773–779
Kim AC, Langer JC, Pastor AC, Zhang L, Sloots CE, Hamilton NA et al (2010) Endorectal pull-through for Hirschsprung’s disease-a multicenter, long-term comparison of results: transanal vs transabdominal approach. J Pediatr Surg 45(6):1213–1220
Ralls MW, Coran AG, Teitelbaum DH (2012) Reoperative surgery for Hirschsprung disease. Semin Pediatr Surg 21(4):354–363
Engum SA, Grosfeld JL (2004) Long-term results of treatment of Hirschsprung’s disease. Semin Pediatr Surg 13(4):273–285
Ieiri S, Nakatsuji T, Akiyoshi J, Higashi M, Hashizume M, Suita S et al (2010) Long-term outcomes and the quality of life of Hirschsprung disease in adolescents who have reached 18 years or older – a 47-year single-institute experience. J Pediatr Surg 45(12):2398–2402
Rintala RJ, Pakarinen MP (2012) Long-term outcomes of Hirschsprung’s disease. Semin Pediatr Surg 21(4):336–343
Dasgupta R, Langer JC (2008) Evaluation and management of persistent problems after surgery for Hirschsprung disease in a child. J Pediatr Gastroenterol Nutr 46(1):13–19
Langer J (1999) Repeat pull-through surgery for complicated Hirschsprung’s disease: indications, techniques, and results. J Pediatr Surg 34:1136–1141
Weber TR, Fortuna RS, Silen ML, Dillon PA (1999) Reoperation for Hirschsprung’s disease. J Pediatr Surg 34(1):153–156; discussion 6–7
Moore SW, Albertyn R, Cywes S (1996) Clinical outcome and long-term quality of life after surgical correction of Hirschsprung’s disease. J Pediatr Surg 31(11):1496–1502
Friedmacher F, Puri P (2011) Residual aganglionosis after pull-through operation for Hirschsprung’s disease: a systematic review and meta-analysis. Pediatr Surg Int 27(10):1053–1057
Schweizer P, Berger S, Schweizer M, Holschneider AM, Beck O (2007) Repeated pull-through surgery for complicated Hirschsprung’s disease – principles derived from clinical experience. J Pediatr Surg 42(3):536–543
Lawal TA, Chatoorgoon K, Collins MH, Coe A, Pena A, Levitt MA (2011) Redo pull-through in Hirschsprung’s [corrected] disease for obstructive symptoms due to residual aganglionosis and transition zone bowel. J Pediatr Surg 46(2):342–347
White FV, Langer JC (2000) Circumferential distribution of ganglion cells in the transition zone of children with Hirschsprung disease. Pediatr Devel Pathol 3(3):216–222
Shayan K, Smith C, Langer JC (2004) Reliability of intraoperative frozen sections in the management of Hirschsprung’s disease. J Pediatr Surg 39(9):1345–1348
Puri P, Gosemann JH (2012) Variants of Hirschsprung disease. Semin Pediatr Surg 21(4):310–318
West KW, Grosfeld JL, Rescorla FJ, Vane DW (1990) Acquired aganglionosis: a rare occurrence following pull-through procedures for Hirschsprung’s disease. J Pediatr Surg 25(1):104–108; discussion 8–9
Wildhaber B, Pakarinen M, Rintala R, Coran A, Teitelbaum D (2004) Posterior myotomy/myectomy for persistent stooling problems in Hirschsprung’s disease. J Ped Surg 39(6):920–926
van Leeuwen K, Teitelbaum DH, Elhalaby EA, Coran AG (2000) Long-term follow-up of redo pull-through procedures for Hirschsprung’s disease: efficacy of the endorectal pull-through. J Pediatr Surg 35(6):829–833; discussion 33–4
Pena A, Elicevik M, Levitt MA (2007) Reoperations in Hirschsprung disease. J Pediatr Surg 42(6):1008–1013; discussion 13–4
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Ralls, M.W., Coran, A.G., Teitelbaum, D.H., Destro, F., Lima, M. (2017). Hirschsprung’s Disease. In: Lima, M. (eds) Pediatric Digestive Surgery. Springer, Cham. https://doi.org/10.1007/978-3-319-40525-4_22
Download citation
DOI: https://doi.org/10.1007/978-3-319-40525-4_22
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-40523-0
Online ISBN: 978-3-319-40525-4
eBook Packages: MedicineMedicine (R0)