Abstract
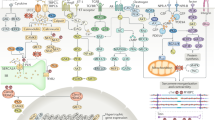
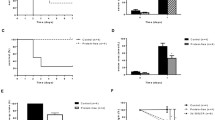
Cardiorenal syndrome is defined as the coexistence of heart failure and renal failure. Under this term, several syndromes with distinct etiology and pathophysiology can be discriminated. This short review focuses on what we have learned from basic research approaches, using animal models. The use of animal models, albeit useful, should always be followed with reservations about extrapolation of results. Two models are presented in detail, one where heart dysfunction is caused by ligation of the left anterior descending artery and another where renal dysfunction is caused by subtotal nephrectomy; in both cases, anatomical and functional alterations in the other organ are presented. Next, future directions in this field are proposed, focused mainly on the need to use system biology approaches for gaining a more holistic understanding and on the promise that interventions on histone deacetylases holds for generating specific and effective pharmaceuticals.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- ANP:
-
Atrial Natriuretic Peptide
- αSMA:
-
Alpha Smooth Muscle Actin
- BiP:
-
Binding immunoglobulin Protein
- βΜΗC:
-
Beta-Myosin Heavy Chain
- CKD:
-
Chronic Kidney Disease
- GFR:
-
Glomerular Filtration Rate
- GRP78:
-
Glucose Responsive Protein 78
- IL-6:
-
Interleukine-6
- IS:
-
Indoxyl Sulfate
- KIM-1:
-
Kidney Injury Molecule-1
- MAPK:
-
Mitogen-Activated Protein Kinase
- MI:
-
Myocardial Infarction
- NFκB:
-
Nuclear Factor κΒ
- NGAL:
-
Neutrophil Gelatinase Associated Lipocalin
- RAAS:
-
Rennin-Angiotensin-Aldosterone System
- SMAD:
-
Similar to Mothers Against Decapentaplegic protein
- STN:
-
Subtotal Nephrectomy
- TGF-β:
-
Transforming Growth Factor-beta
- UPR:
-
Unfolded Protein Response
References
Ronco C, House AA, Haapio M. Cardiorenal syndrome: refining the definition of a complex symbiosis gone wrong. Intensive Care Med. 2008;34:957–62.
Parikh CR, Coca SG, Wang Y, Masudi FA, Krumholz HM. Long-term prognosis of acute kidney injury after acute myocardial infarction. Arch Intern Med. 2008;168:987–95.
Sarnak MJ, Levey AS, Schoolwerth AC, Coresh J, Culleton B, et al. Kidney disease as a risk factor for development of cardiovascular disease: a statement from the American Heart Association Councils on Kidney in cardiovascular Disease, High Blood Pressure Research, Clinical Cardiology and Epidemiology and Prevention. Circulation. 2003;108:2154–69.
Ronco C. Cardiorenal Syndromes: Definition and Classification. In: Ronco C, Costanzo MR, Bellomo R, Maisel AS, editors. Fluid overload: diagnosis and management, vol. 64. Basel: Karger; 2010. p. 33–8.
Bongartz LG, Braam B, Gaillard CA, Cramer MJ, Goldschmeding R, Verhaar MC, et al. Target organ cross talk in cardiorenal syndrome: animal models. Am J Physiol Renal Physiol. 2012;303:F1253–63.
Lekawanvijit S, Kompa AR, Zang Y, Wang BH, Kelly DJ, Krum H. Myocardial infarction impairs renal function, induces renal interstitial fibrosis, and increases renal KIM-1 expression: implications for cardiorenal syndrome. Am J Physiol Heart Circ Physiol. 2012;302:H1884–93.
Tzanidis A, Lim S, Hannan RD, See F, Ugoni AM, Krum H. Combined angiotensin and endothelin receptor blockade attenuates adverse cardiac remodeling post-myocardial infarction in the rat: possible role of transforming growth factor beta. J Mol Cell Cardiol. 2001;33:969–81.
Wolf G. Renal injury due to rennin-angiotensin-aldosterone system activation of the transforming growth factor-beta pathway. Kidney Int. 2006;70:1914–9.
Lekawanvijit S, Kompa AR, Manabe M, Wang BH, Langham RG, Nishijima F, et al. Chronic kidney disease-induced cardiac fibrosis is ameliorated by reducing circulating levels of a non-dialysable uremic toxin, indoxyl sulfate. PLoS One. 2012;7:e41281.
Niwa T. Uremic toxicity of indoxyl sulfate. Nagoya J Med Sci. 2010;72:1–11.
Lekawanvijit S, Adrahtas A, Kelly DJ, Kompa AR, Wang BH, Krum H. Does indoxyl sulfate, a uraemic toxin, have direct effects on cardiac fibroblasts and myocytes? Eur Heart J. 2010;31:1771–9.
Ben-Shoshan J, Entin-Meer M, Guzner-Gur H, Keren G. The cardiorenal syndrome: a mutual approach to concomitant cardiac and renal failure. Isr Med Assoc J. 2012;14:570–6.
Xu C, Bailly-Maitre B, Reed JC. Endoplasmic reticulum stress: cell life and death decisions. J Clin Invest. 2005;115:2656–64.
Kim I, Xu W, Reed JC. Cell death and endoplasmic reticulum stress: diseases relevance and therapeutic opportunities. Nat Rev Drug Discov. 2008;7:1013–30.
Dickhout JG, Carlisle RE, Austin RC. Interrelationship between cardiac hypertrophy, heart failure and chronic kidney disease. Endoplasmic reticulum stress as a mediator of pathogenesis. Circ Res. 2011;106:629–42.
Bush EW, McKinsey TA. Protein acetylation in the cardiorenal axis: the promise of histone deacetylase inhibitors. Circ Res. 2010;106:272–84.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Charonis, A.S. (2015). Cardiorenal Syndrome: What Basic Research Can Contribute. In: Cokkinos, D. (eds) Introduction to Translational Cardiovascular Research. Springer, Cham. https://doi.org/10.1007/978-3-319-08798-6_26
Download citation
DOI: https://doi.org/10.1007/978-3-319-08798-6_26
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-08797-9
Online ISBN: 978-3-319-08798-6
eBook Packages: MedicineMedicine (R0)