Abstract
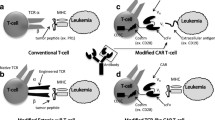
T cells specific for major histocompatibility complex (MHC)-presented tumor antigens are capable of inducing durable remissions when adoptively transferred to patients with refractory cancers presenting such antigens. When such T cells are derived from healthy donors, they can be banked for off-the-shelf administration in appropriately tissue matched patients. Therefore, tumor antigen-specific, donor-derived T cells are expected to be a mainstay in the cancer immunotherapy armamentarium. In this chapter, we analyze clinical evidence that tumor antigen-specific donor-derived T cells can induce tumor regressions when administered to appropriately matched patients whose tumors are refractory to standard therapy. We also delineate the landscape of MHC-presented and unconventional tumor antigens recognized by T cells in healthy individuals that have been targeted for adoptive T cell therapy, as well as emerging antigens for which mounting evidence suggests their utility as targets for adoptive T cell therapy. We discuss the growing technological advancements that have facilitated sequence identification of such antigens and their cognate T cells, and applicability of such technologies in the pre-clinical and clinical settings.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Fefer A, Buckner CD, Thomas ED, Cheever MA, Clift RA, Glucksberg H et al (1977) Cure of hematologic neoplasia with transplantation of marrow from identical twins. N Engl J Med 297(3):146–148
Weiden PL, Flournoy N, Thomas ED, Prentice R, Fefer A, Buckner CD et al (2010) Antileukemic effect of graft-versus-host disease in human recipients of allogeneic-marrow grafts. 300(19):1068–73. https://doi.org/10.1056/NEJM197905103001902
Apperley JF, Jones L, Hale G, Waldmann H, Hows J, Rombos Y et al (1986) Bone marrow transplantation for patients with chronic myeloid leukaemia: T-cell depletion with Campath-1 reduces the incidence of graft-versus-host disease but may increase the risk of leukaemic relapse. Bone Marrow Transplant 1(1):53–66
Kolb HJ, Mittermuller J, Clemm C, Holler E, Ledderose G, Brehm G et al (1990) Donor leukocyte transfusions for treatment of recurrent chronic myelogenous leukemia in marrow transplant patients. Blood 76(12):2462–2465
Mackinnon S, Papadopoulos E, Carabasi M, Reich L, Collins N, Boulad F et al (1995) Adoptive immunotherapy evaluating escalating doses of donor leukocytes for relapse of chronic myeloid leukemia after bone marrow transplantation: separation of graft-versus-leukemia responses from graft-versus-host disease. Blood 86(4):1261–1268
Collins RH, Shpilberg O, Drobyski WR, Porter DL, Giralt S, Champlin S et al (1997) Donor leukocyte infusions in 140 patients with relapsed malignancy after allogeneic bone marrow transplantation. J Clin Oncol 15(2):433–44
Smit WM, Rijnbeek M, Van Bergen CAM, Fibbe WE, Willemze R, Frederik Falkenburg JH (1998) T cells recognizing leukemic CD34+ progenitor cells mediate the antileukemic effect of donor lymphocyte infusions for relapsed chronic myeloid leukemia after allogeneic stem cell transplantation. Proc Natl Acad Sci USA 95(17):10152–10157
Marijt WAE, Heemskerk MHM, Kloosterboer FM, Goulmy E, Kester MGD, Van der Hoorn MAWG et al (2003) Hematopoiesis-restricted minor histocompatibility antigens HA-1- or HA-2-specific T cells can induce complete remissions of relapsed leukemia. Proc Natl Acad Sci USA 100(5):2742–2747
de Rijke B, van Horssen-Zoetbrood A, Beekman JM, Otterud B, Maas F, Woestenenk R et al (2005) A frameshift polymorphism in P2X5 elicits an allogeneic cytotoxic T lymphocyte response associated with remission of chronic myeloid leukemia. J Clin Invest 115(12):3506–3516
Griffioen M, Kessler JH, Borghi M, van Soest RA, van der Minne CE, Nouta J et al (2006) Detection and functional analysis of CD8+ T cells specific for PRAME: a target for T-cell therapy. Clin Cancer Res 12(10):3130–3136
Molldrem JJ, Lee PP, Wang C, Felio K, Kantarjian HM, Champlin RE et al (2000) Evidence that specific T lymphocytes may participate in the elimination of chronic myelogenous leukemia. Nat Med 6(9):1018–23
Molldrem J, Dermime S, Parker K, Jiang Y, Mavroudis D, Hensel N et al (1996) Targeted T-cell therapy for human leukemia: cytotoxic T lymphocytes specific for a peptide derived from proteinase 3 preferentially lyse human myeloid leukemia cells. Blood 88(7):2450–2457
Molldrem JJ, Lee PP, Wang C, Champlin RE, Davis MM (1999) A PR1-human leukocyte antigen-A2 tetramer can be used to isolate low-frequency cytotoxic T lymphocytes from healthy donors that selectively lyse chronic myelogenous leukemia 1. Cancer Res 59:2675–2681
Doubrovina ES, Doubrovin MM, Lee S, Shieh JH, Heller G, Pamer E et al (2004) In vitro stimulation with WT1 peptide-loaded epstein-barr virus-positive B cells elicits high frequencies of WT1 peptide-specific T cells with in vitro and in vivo tumoricidal activity. Clin Cancer Res 10(21):7207–7219
Doubrovina E, Carpenter T, Pankov D, Selvakumar A, Hasan A, O’Reilly RJ (2012) Mapping of novel peptides of WT-1 and presenting HLA alleles that induce epitope-specific HLA-restricted T cells with cytotoxic activity against WT-1+ leukemias. Blood 120(8):1633–1646
Ohminami H, Yasukawa M, Fujita S (2000) HLA class I-restricted lysis of leukemia cells by a CD8+ cytotoxic T-lymphocyte clone specific for WT1 peptide. Blood 95(1):286–293
Tyler EM, Jungbluth AA, O’Reilly RJ, Koehne G (2013) WT1-specific T-cell responses in high-risk multiple myeloma patients undergoing allogeneic T cell–depleted hematopoietic stem cell transplantation and donor lymphocyte infusions. Blood 121(2):308–317
Ishikawa T, Fujii N, Imada M, Aoe M, Meguri Y, Inomata T et al (2017) Graft-versus-leukemia effect with a WT1-specific T-cell response induced by azacitidine and donor lymphocyte infusions after allogeneic hematopoietic stem cell transplantation. Cytotherapy 19(4):514–520
Tyler EM, Jungbluth AA, Gnjatic S, O’Reilly RJ, Koehne G (2014) Cancer-testis antigen 7 expression and immune responses following allogeneic stem cell transplantation for multiple myeloma. Cancer Immunol Res 2(6):547–558
Yotnda P, Firat H, Garcia-Pons F, Garcia Z, Gourru G, Vernant JP et al (1998) Cytotoxic T cell response against the chimeric p210 BCR-ABL protein in patients with chronic myelogenous leukemia. J Clin Invest 101(10):2290
Bocchia M, Korontsvit T, Xu Q, Mackinnon S, Yang SY, Sette A et al (1996) Specific human cellular immunity to bcr-abl oncogene-derived peptides. Blood 87(9):3587–92
Clark RE, Dodi IA, Hill SC, Lill JR, Aubert G, Macintyre AR et al (2001) Direct evidence that leukemic cells present HLA-associated immunogenic peptides derived from the BCR-ABL b3a2 fusion protein. Blood 98(10):2887–2893
Butt NM, Rojas JM, Wang L, Christmas SE, Abu-Eisha HM, Clark RE (2005) Circulating bcr-abl-specific CD8+ T cells in chronic myeloid leukemia patients and healthy subjects. Haematologica 90(10 SE-Comparative Studies):1315–23
Wu CJ, Biernacki M, Kutok JL, Rogers S, Chen L, Yang X-F et al (2005) Graft-versus-leukemia target antigens in chronic myelogenous leukemia are expressed on myeloid progenitor cells. Clin Cancer Res 11(12):4504–4511
Wang Q, Li M, Wang Y, Zhang Y, Jin S, Xie G et al (2008) RNA interference targeting CML66, a novel tumor antigen, inhibits proliferation, invasion and metastasis of HeLa cells. Cancer Lett 269(1):127–138
Zhang W, Choi J, Zeng W, Rogers SA, Alyea EP, Rheinwald JG et al (2010) Graft-versus-leukemia antigen CML66 elicits coordinated B-cell and T-cell immunity after donor lymphocyte infusion. Clin Cancer Res 16(10):2729–2739
Suemori K, Fujiwara H, Ochi T, Azuma T, Yamanouchi J, Narumi H et al (2008) Identification of an epitope derived from CML66, a novel tumor-associated antigen expressed broadly in human leukemia, recognized by human leukocyte antigen-A*2402-restricted cytotoxic T lymphocytes. Cancer Sci 99(7):1414–1419
van Baren N, Chambost H, Ferrant A, Michaux L, Ikeda H, Millard I et al (1998) PRAME, a gene encoding an antigen recognized on a human melanoma by cytolytic T cells, is expressed in acute leukaemia cells. Br J Haematol 102(5):1376–9
Oehler VG, Guthrie KA, Cummings CL, Sabo K, Wood BL, Gooley T et al (2009) The preferentially expressed antigen in melanoma (PRAME) inhibits myeloid differentiation in normal hematopoietic and leukemic progenitor cells. Blood 114(15):3299
De Carvalho DD, Binato R, Pereira WO, Leroy JMG, Colassanti MD, Proto-Siqueira R et al (2011) BCR–ABL-mediated upregulation of PRAME is responsible for knocking down TRAIL in CML patients. Oncogene 30(2):223–33
Kessler JH, Beekman NJ, Bres-Vloemans SA, Verdijk P, Van Veelen PA, Kloosterman-Joosten AM et al (2001) Efficient identification of novel HLA-A * 0201-presented cytotoxic T lymphocyte epitopes in the widely expressed tumor antigen PRAME by proteasome-mediated digestion analysis. J Exp Med 193(1):73–88
Sommermeyer D, Conrad H, Krönig H, Gelfort H, Bernhard H, Uckert W (2013) NY-ESO-1 antigen-reactive T cell receptors exhibit diverse therapeutic capability. Int J Cancer 132(6):1360–1367
Zarour HM, Storkus WJ, Brusic V, Williams E, Kirkwood JM (2000) NY-ESO-1 Encodes DRB1*0401-restricted epitopes recognized by melanoma-reactive CD4+ T cells. Cancer Res 60(17):4946–4952
Zarour HM, Maillere B, Brusic V, Coval K, Williams E, Pouvelle-Moratille S et al (2002) NY-ESO-1 119–143 is a promiscuous major histocompatibility complex class II T-helper epitope recognized by Th1- and Th2-type tumor-reactive CD4+ T cells. Cancer Res 62(1):213–218
Kayser S, Boβ C, Feucht J, Witte K-E, Scheu A, Bülow H-J et al (2015) Rapid generation of NY-ESO-1-specific CD4+ THELPER1 cells for adoptive T-cell therapy. Oncoimmunology 4(5):e1002723
Valmori D, Souleimanian NE, Hesdorffer CS, Old LJ, Ayyoub M (2005) Quantitative and qualitative assessment of circulating NY-ESO-1 specific CD4+ T cells in cancer-free individuals. Clin Immunol 117(2):161–167
Hofmann S, Schmitt M, Götz M, Döhner H, Wiesneth M, Bunjes D et al (2019) Donor lymphocyte infusion leads to diversity of specific T cell responses and reduces regulatory T cell frequency in clinical responders. Int J Cancer 144(5):1135–1146
van Balen P, Jedema I, van Loenen MM, de Boer R, van Egmond HM, Hagedoorn RS et al (2020) HA-1H T-cell receptor gene transfer to redirect virus-specific T cells for treatment of hematologic malignancies after allogeneic stem cell transplantation: a phase 1 clinical study. Front Immunol 20:1804
Warren EH, Fujii N, Akatsuka Y, Chaney CN, Mito JK, Loeb KR et al (2010) Therapy of relapsed leukemia after allogeneic hematopoietic cell transplantation with T cells specific for minor histocompatibility antigens. Blood 115(19):3869–3878
Meij P, Jedema I, van der Hoorn MAWG, Bongaerts R, Cox L, Wafelman AR et al (2012) Generation and administration of HA-1-specific T-cell lines for the treatment of patients with relapsed leukemia after allogeneic stem cell transplantation: a pilot study. Haematologica 97(8):1205
Chapuis AG, Egan DN, Bar M, Schmitt TM, Mcafee MS, Paulson KG et al (2019) T cell receptor gene therapy targeting WT1 prevents acute myeloid leukemia relapse post-transplant. Nat Med 25
Comoli P, Basso S, Riva G, Barozzi P, Guido I, Gurrado A et al (2017) BCR-ABL–specific T-cell therapy in Ph+ ALL patients on tyrosine-kinase inhibitors. Blood 129(5):582–586
Chapuis AG, Ragnarsson GB, Nguyen HN, Chaney CN, Pufnock JS, Schmitt TM et al (2013) Transferred WT1-reactive CD8+ T cells can mediate antileukemic activity and persist in post-transplant patients. Sci Transl Med 5(174):174ra27–174ra27
Prockop SE, Doubrovina E, Adams R, Boulad F, Kernan NA, O’Reilly RJ (2013) Adoptive transfer of WT-1 specific HLA class 2 restricted donor-derived T-cells induces sustained remission of AML relapse post transplant presenting as leukemia cutis. Blood 122(21):2085–2085
Lulla PD, Naik S, Vasileiou S, Tzannou I, Watanabe A, Kuvalekar M et al (2021) Clinical effects of administering leukemia-specific donor T cells to patients with AML/MDS after allogeneic transplant. Blood 137(19):2585–97
van Bergen CAM, van Luxemburg-Heijs SAP, de Wreede LC, Eefting M, von dem Borne PA, van Balen P et al (2017) Selective graft-versus-leukemia depends on magnitude and diversity of the alloreactive T cell response. J Clin Invest 127(2):517–529
Bleakley M, Riddell SR (2011) Exploiting T cells specific for human minor histocompatibility antigens for therapy of leukemia. Immunol Cell Biol 89(3):396
Bykova NA, Malko DB, Efimov GA (2018) In silico analysis of the minor histocompatibility antigen landscape based on the 1000 genomes project. Front Immunol 1819
Kloosterboer FM, van Luxemburg-Heijs SA, van Soest RA, Barbui AM, van Egmond HM, Strijbosch MP et al (2004) Direct cloning of leukemia-reactive T cells from patients treated with donor lymphocyte infusion shows a relative dominance of hematopoiesis-restricted minor histocompatibility antigen HA-1 and HA-2 specific T cells. Leukemia 18(4):798–808
Molldrem JJ, Clave E, Jiang YZ, Mavroudis D, Raptis A, Hensel N et al (1997) Cytotoxic T lymphocytes specific for a nonpolymorphic proteinase 3 peptide preferentially inhibit chronic myeloid leukemia colony-forming units. Blood 90(7):2529–2534
Rao NV, Wehner NG, Marshall BC, Gray WR, Gray BH, Hoidal JR (1991) Characterization of proteinase-3 (PR-3), a neutrophil serine proteinase. Structural and functional properties. J Biol Chem 266(15):9540–8
Yang T-H, John LS St, Garber HR, Kerros C, Ruisaard KE, Clise-Dwyer K et al (2018) Membrane-associated proteinase 3 on granulocytes and acute myeloid leukemia inhibits T cell proliferation. J Immunol Author Choice 201(5):1389
Qazilbash MH, Wieder E, Thall PF, Wang X, Rios R, Lu S et al (2017) PR1 peptide vaccine induces specific immunity with clinical responses in myeloid malignancies. Leukemia 31(3):697–704
Alatrash G, Molldrem JJ, Qazilbash MH (2017) Targeting PR1 in myeloid leukemia. Oncotarget 9(4):4280–4281
Bornhäuser M, Thiede C, Platzbecker U, Kiani A, Oelschlaegel U, Babatz J et al (2011) Prophylactic transfer of BCR-ABL–, PR1-, and WT1-reactive donor T cells after T cell–depleted allogeneic hematopoietic cell transplantation in patients with chronic myeloid leukemia. Blood 117(26):7174–7184
Buckler AJ, Pelletier J, Haber DA, Glaser T, Housman DE (1991) Isolation, characterization, and expression of the murine Wilms’ tumor gene (WT1) during kidney development. Mol Cell Biol 11(3):1707–1712
Mundlos S, Pelletier J, Darveau A, Bachmann M, Winterpacht A, Zabel B (1993) Nuclear localization of the protein encoded by the Wilms’ tumor gene WT1 in embryonic and adult tissues. Development 119(4):1329–1341
Keilholz U, Menssen HD, Gaiger A, Menke A, Oji Y, Oka Y et al (2005) Wilms’ tumour gene 1 (WT1) in human neoplasia. Leuk 19(8):1318–23
Tatsumi N, Oji Y, Tsuji N, Tsuda A, Higashio M, Aoyagi S et al (2008) Wilms’ tumor gene WT1-shRNA as a potent apoptosis-inducing agent for solid tumors. Int J Oncol 32(3):701–711
Glienke W, Maute L, Koehl U, Esser R, Milz E, Bergmann L (2007) Effective treatment of leukemic cell lines with wt1 siRNA. Leuk 21(10):2164–70
Doubrovina ES, Doubrovin MM, Lee S, Shieh J-H, Heller G, Pamer E et al (2004) In vitro stimulation with WT1 peptide-loaded epstein-barr virus-positive B cells elicits high frequencies of WT1 peptide-specific T cells with in vitro and in vivo tumoricidal activity. Clin Cancer Res 10(21):7207–7219
Gao L, Xue SA, Hasserjian R, Cotter F, Kaeda J, Goldman JM et al (2003) Human cytotoxic T lymphocytes specific for Wilms’ tumor antigen-1 inhibit engraftment of leukemia-initiating stem cells in non-obese diabetic-severe combined immunodeficient recipients. Transplantation 75(9):1429–1436
Xue S-A, Gao L, Hart D, Gillmore R, Qasim W, Thrasher A et al (2005) Elimination of human leukemia cells in NOD/SCID mice by WT1-TCR gene–transduced human T cells. Blood 106(9):3062–3067
Maslak PG, Dao T, Bernal Y, Chanel SM, Zhang R, Frattini M et al (2018) Phase 2 trial of a multivalent WT1 peptide vaccine (galinpepimut-S) in acute myeloid leukemia. Blood Adv 2(3):224–234
Koehne G, Devlin S, Chung DJ, Landau HJ, Korde N, Mailankody S et al (2017) WT1 heteroclitic epitope immunization following autologous stem cell transplantation in patients with high-risk multiple myeloma (MM). 35(15_suppl):8016–8016. https://doi.org/10.1200/JCO20173515_suppl8016
O’Cearbhaill RE, Gnjatic S, Aghajanian C, Iasonos A, Konner JA, Losada N et al (2018) A phase I study of concomitant galinpepimut-s (GPS) in combination with nivolumab (nivo) in patients (pts) with WT1+ ovarian cancer (OC) in second or third remission. 36(15_suppl):5553–5553. https://doi.org/10.1200/JCO20183615_suppl5553
Ikeda H, Lethé B, Lehmann F, Van BN, Baurain J-F, De SC et al (1997) Characterization of an antigen that is recognized on a melanoma showing partial HLA loss by CTL expressing an NK inhibitory receptor. Immunity 6(2):199–208
Chang AY, Dao T, Gejman RS, Jarvis CA, Scott A, Dubrovsky L et al (2017) A therapeutic T cell receptor mimic antibody targets tumor-associated PRAME peptide/HLA-I antigens. J Clin Invest 127(7):1–14
Chang AY, Dao T, Gejman RS, Jarvis CA, Scott A, Dubrovsky L et al (2017) A therapeutic T cell receptor mimic antibody targets tumor-associated PRAME peptide/HLA-I antigens. J Clin Invest 127(7):2705
Kalaora S, Sang Lee J, Barnea E, Levy R, Greenberg P, Alon M et al Immunoproteasome expression is associated with better prognosis and response to checkpoint therapies in melanoma
Keller M, Ebstein F, Bürger E, Textoris-Taube K, Gorny X, Urban S et al (2015) The proteasome immunosubunits, PA28 and ER-aminopeptidase 1 protect melanoma cells from efficient MART-126-35-specific T-cell recognition. Eur J Immunol 45(12):3257–3268
Stanojevic M, Hont AB, Geiger A, O’Brien S, Ulrey R, Grant M et al (2021) Identification of novel HLA-restricted preferentially expressed antigen in melanoma peptides to facilitate off-the-shelf tumor-associated antigen-specific T-cell therapies. Cytotherapy 23(8):694–703
Mahoney KE, Shabanowitz J, Hunt DF (2021) MHC phosphopeptides: promising targets for immunotherapy of cancer and other chronic diseases. Mol Cell Proteomics 20:100112
Cobbold M, De La Peña H, Norris A, Polefrone JM, Qian J, English AM et al (2013) MHC class I-associated phosphopeptides are the targets of memory-like immunity in leukemia. Sci Transl Med 5(203):1–11
Zarling AL, Polefrone JM, Evans AM, Mikesh LM, Shabanowitz J, Lewis ST et al (2006) Identification of class I MHC-associated phosphopeptides as targets for cancer immunotherapy. Proc Natl Acad Sci 103(40):14889–14894
Engelhard VH, Obeng RC, Cummings KL, Petroni GR, Ambakhutwala AL, Chianese-Bullock KA et al (2020) MHC-restricted phosphopeptide antigens: preclinical validation and first-in-humans clinical trial in participants with high-risk melanoma. J Immunother Cancer 8(1):e000262
Mohammed F, Cobbold M, Zarling AL, Salim M, Barrett-Wilt GA, Shabanowitz J et al (2008) Phosphorylation-dependent interaction between antigenic peptides and MHC class I: a molecular basis for the presentation of transformed self. Nat Immunol 9(11):1236–1243
Kessler JH, Bres-Vloemans SA, van Veelen PA, de Ru A, Huijbers IJG, Camps M et al (2006) BCR-ABL fusion regions as a source of multiple leukemia-specific CD8+ T-cell epitopes. Leuk 20(10):1738–50.
Cai A, Keskin DB, DeLuca DS, Alonso A, Zhang W, Zhang GL et al (2012) Mutated BCR-ABL generates immunogenic T-cell epitopes in CML patients. Clin Cancer Res 18(20):5761–5772
Riva G, Luppi M, Barozzi P, Quadrelli C, Basso S, Vallerini D et al (2010) Emergence of BCR-ABL–specific cytotoxic T cells in the bone marrow of patients with Ph+ acute lymphoblastic leukemia during long-term imatinib mesylate treatment. Blood 115(8):1512–1518
Rojas JM, Knight K, Wang L, Clark RE (2007) Clinical evaluation of BCR-ABL peptide immunisation in chronic myeloid leukaemia: results of the EPIC study. Leuk 21(11):2287–95
Cathcart K, Pinilla-Ibarz J, Korontsvit T, Schwartz J, Zakhaleva V, Papadopoulos EB et al (2004) A multivalent bcr-abl fusion peptide vaccination trial in patients with chronic myeloid leukemia. Blood 103(3):1037–1042
Pinilla-Ibarz J, Cathcart K, Korontsvit T, Soignet S, Bocchia M, Caggiano J et al (2000) Vaccination of patients with chronic myelogenous leukemia with bcr-abl oncogene breakpoint fusion peptides generates specific immune responses. Blood 95(5):1781–1787
Zamora AE, Crawford JC, Allen EK, Guo XJ, Bakke J, Carter RA et al (2019) Pediatric patients with acute lymphoblastic leukemia generate abundant and functional neoantigen-specific CD8+ T cell responses. Sci Transl Med 11(498):eaat8549
Ali M, Foldvari Z, Giannakopoulou E, Böschen ML, Strønen E, Yang W et al (2019) Induction of neoantigen-reactive T cells from healthy donors. Nat Protoc 14(6):1926–1943
Kato T, Matsuda T, Ikeda Y, Park J-H, Leisegang M, Yoshimura S et al (2018) Effective screening of T cells recognizing neoantigens and construction of T-cell receptor-engineered T cells. Oncotarget 9(13):11009
Matsuda T, Leisegang M, Park J-H, Ren L, Kato T, Ikeda Y et al (2018) Induction of neoantigen-specific cytotoxic T cells and construction of T-cell receptor-engineered T cells for ovarian cancer. Clin Cancer Res 24(21):5357–67
Strønen E, Toebes M, Kelderman S, Van Buuren MM, Yang W, Van Rooij N et al (2016) Targeting of cancer neoantigens with donor-derived T cell receptor repertoires. Science (80- ) 352(6291):1337–41
Duval A, Reperant M, Hamelin R (2002) Comparative analysis of mutation frequency of coding and non coding short mononucleotide repeats in mismatch repair deficient colorectal cancers. Oncogene 21(52):8062–6
Mardis ER (2019) Neoantigens and genome instability: impact on immunogenomic phenotypes and immunotherapy response. Genome Med 11(1):1–12
Sahin IH, Akce M, Alese O, Shaib W, Lesinski GB, El-Rayes B et al (2019) Immune checkpoint inhibitors for the treatment of MSI-H/MMR-D colorectal cancer and a perspective on resistance mechanisms. Br J Cancer 121(10):809–18
Schwitalle Y, Linnebacher M, Ripberger E, Gebert J, Doeberitz MVK (2004) Immunogenic peptides generated by frameshift mutations in DNA mismatch repair-deficient cancer cells. 4:1–10
Linnebacher M, Gebert J, Rudy W, Woerner S, Yuan YP, Bork P et al (2001) Frameshift peptide-derived T-cell epitopes: a source of novel tumor-specific antigens. Int J Cancer 93(1):6–11
Garbe Y, Maletzki C, Linnebacher M (2011) An MSI tumor specific frameshift mutation in a coding microsatellite of MSH3 encodes for HLA-A0201-restricted CD8+ cytotoxic T cell epitopes. PLoS One 6(11)
Roudko V, Bozkus CC, Orfanelli T, McClain CB, Carr C, O’Donnell T et al (2020) Shared immunogenic poly-epitope frameshift mutations in microsatellite unstable tumors. Cell 183(6):1634-1649.e17
Kloor M, Reuschenbach M, Pauligk C, Karbach J, Rafiyan M-R, Al-Batran S-E et al (2020) A frameshift peptide neoantigen-based vaccine for mismatch repair-deficient cancers: a phase I/IIa clinical trial. Clin Cancer Res 26(17):4503–4510
Mohamed YS, Bashawri LA, Vatte C, Abu-Rish EY, Cyrus C, Khalaf WS et al (2016) The in vitro generation of multi-tumor antigen-specific cytotoxic T cell clones: candidates for leukemia adoptive immunotherapy following allogeneic stem cell transplantation. Mol Immunol 77:79–88
Gerdemann U, Katari U, Christin AS, Cruz CR, Tripic T, Rousseau A et al (2011) Cytotoxic T lymphocytes simultaneously targeting multiple tumor-associated antigens to treat EBV negative lymphoma. Mol Ther 19(12):2258–68
Vasileiou S, Lulla PD, Tzannou I, Watanabe A, Kuvalekar M, Callejas WL et al (2021) T-cell therapy for lymphoma using nonengineered multiantigen-targeted T cells is safe and produces durable clinical effects. J Clin Oncol 39(13):1415–1425
Hont AB, Cruz CR, Ulrey R, O’Brien B, Stanojevic M, Datar A et al (2019) Immunotherapy of relapsed and refractory solid tumors with ex vivo expanded multi-tumor associated antigen specific cytotoxic T lymphocytes: a phase I study. J Clin Oncol 37(26):2349
Dave H, Terpilowski M, Mai M, Toner K, Grant M, Stanojevic M et al (2021) Tumor associated antigen specific T cells with nivolumab are safe and persist in vivo in rel/ref Hodgkin Lymphoma. Blood Adv
Em J, Sh K, Rh S, Dm P (1989) Activation of gamma delta T cells in the primary immune response to mycobacterium tuberculosis. Science 244(4905):713–716
Ravens S, Schultze-Florey C, Raha S, Sandrock I, Drenker M, Oberdörfer L et al (2017) Human γδ T cells are quickly reconstituted after stem-cell transplantation and show adaptive clonal expansion in response to viral infection. Nat Immunol 18(4):393–401
Knight A, Madrigal AJ, Grace S, Sivakumaran J, Kottaridis P, Mackinnon S et al (2010) The role of Vδ2-negative γδ T cells during cytomegalovirus reactivation in recipients of allogeneic stem cell transplantation. Blood 116(12):2164–2172
Scheper W, van Dorp S, Kersting S, Pietersma F, Lindemans C, Hol S et al (2013) γδT cells elicited by CMV reactivation after allo-SCT cross-recognize CMV and leukemia. Leuk 27(6):1328–38
Vila LM, Haftel HM, Park HS, Lin MS, Romzek NC, Hanash SM et al (1995) Expansion of mycobacterium-reactive gamma delta T cells by a subset of memory helper T cells. Infect Immun 63(4):1211
Behr C, Poupot R, Peyrat MA, Poquet Y, Constant P, Dubois P et al (1996) Plasmodium falciparum stimuli for human gammadelta T cells are related to phosphorylated antigens of mycobacteria. Infect Immun 64(8):2892–6
Vavassori S, Kumar A, Wan GS, Ramanjaneyulu GS, Cavallari M, El Daker S et al (2013) Butyrophilin 3A1 binds phosphorylated antigens and stimulates human γδ T cells. Nat Immunol 14(9):908–16
Rigau M, Ostrouska S, Fulford TS, Johnson DN, Woods K, Ruan Z et al (2020) Butyrophilin 2A1 is essential for phosphoantigen reactivity by γδ T cells. Science (80- ) 367(6478)
Godder KT, Henslee-Downey PJ, Mehta J, Park BS, Chiang K-Y, Abhyankar S et al (2007) Long term disease-free survival in acute leukemia patients recovering with increased γδ T cells after partially mismatched related donor bone marrow transplantation. Bone Marrow Transplant 39(12):751–7
Lamb L, Musk P, Ye Z, van Rhee F, Geier S, Tong J-J et al (2001) Human γδ+ T lymphocytes have in vitro graft vs leukemia activity in the absence of an allogeneic response. Bone Marrow Transplant 27(6):601–6
Bauer S, Groh V, Wu J, Steinle A, Phillips JH, Lanier LL et al (1999) Activation of NK cells and T cells by NKG2D, a receptor for stress-inducible MICA. Science (80- ) 285(5428):727–9
Jin C, Lagoudas GK, Zhao C, Bullman S, Bhutkar A, Hu B et al (2019) Commensal microbiota promote lung cancer development via γδ T cells. Cell 176(5):998-1013.e16
Payne KK, Mine JA, Biswas S, Chaurio RA, Perales-Puchalt A, Anadon CM, et al (2020) BTN3A1 governs antitumor responses by coordinating αβ and γδ T cells. Science (80- ) 369(6506):942–9
Park JH, Kim H-J, Kim CW, Kim HC, Jung Y, Lee H-S et al (2021) Tumor hypoxia represses γδ T cell-mediated antitumor immunity against brain tumors. Nat Immunol 22(3):336–46
Treiner E, Lantz O (2006) CD1d- and MR1-restricted invariant T cells: of mice and men. Curr Opin Immunol 18(5):519–526
Brigl M, Brenner MB (2004) CD1: antigen presentation and T cell function. 22:817–90. https://doi.org/10.1146/annurev.immunol22012703104608
Han M, Hannick LI, DiBrino M, Robinson MA (1999) Polymorphism of human CD1 genes. Tissue Antigens 54(2):122–127
Barral DC, Brenner MB (2007) CD1 antigen presentation: how it works. Nat Rev Immunol 7(12):929–41
Mori L, Lepore M, De Libero G (2016) The Immunology of CD1- and MR1-restricted T cells. Annu Rev Immunol 34(1):479–510
de Lalla C, Lepore M, Piccolo FM, Rinaldi A, Scelfo A, Garavaglia C et al (2011) High-frequency and adaptive-like dynamics of human CD1 self-reactive T cells. Eur J Immunol 41(3):602–10
Lepore M, de Lalla C, Gundimeda SR, Gsellinger H, Consonni M, Garavaglia C et al (2014) A novel self-lipid antigen targets human T cells against CD1c+ leukemias. J Exp Med 211(7):1363–1377
Consonni M, Garavaglia C, Grilli A, de Lalla C, Mancino A, Mori L et al (2021) Human T cells engineered with a leukemia lipid-specific TCR enables donor-unrestricted recognition of CD1c-expressing leukemia. Nat Commun 12(1):1–14
Bassani-Sternberg M, Bräunlein E, Klar R, Engleitner T, Sinitcyn P, Audehm S et al (2016) Direct identification of clinically relevant neoepitopes presented on native human melanoma tissue by mass spectrometry. Nat Commun 7(1):13404
Yadav M, Jhunjhunwala S, Phung QT, Lupardus P, Tanguay J, Bumbaca S et al (2014) Predicting immunogenic tumour mutations by combining mass spectrometry and exome sequencing. Nature 515(7528):572–576
Kalaora S, Barnea E, Merhavi-Shoham E, Qutob N, Teer JK, Shimony N et al (2016) Use of HLA peptidomics and whole exome sequencing to identify human immunogenic neo-antigens. Oncotarget 7(5):5110–5117
Chong C, Müller M, Pak H, Harnett D, Huber F, Grun D et al (2020) Integrated proteogenomic deep sequencing and analytics accurately identify non-canonical peptides in tumor immunopeptidomes. Nat Commun 11(1):1–21
Ho WY, Nguyen HN, Wolfl M, Kuball J, Greenberg PD (2006) In vitro methods for generating CD8+ T-cell clones for immunotherapy from the naïve repertoire. J Immunol Methods 310(1–2):40–52
Wölfl M, Greenberg PD (2014) Antigen-specific activation and cytokine-facilitated expansion of naive, human CD8+ T cells. Nat Protoc 9(4):950–966
Krutzik PO, Nolan GP (2006) Fluorescent cell barcoding in flow cytometry allows high-throughput drug screening and signaling profiling. Nat Methods 3(5):361–8
Krutzik PO, Clutter MR, Trejo A, Nolan GP (2011) Fluorescent cell barcoding for multiplex flow cytometry. Curr Protoc Cytom 55(1):6.31.1–6.31.15
Dolton G, Tungatt K, Lloyd A, Bianchi V, Theaker SM, Trimby A et al (2015) More tricks with tetramers: a practical guide to staining T cells with peptide-MHC multimers. Immunology 146(1):11–22
Wooldridge L, Lissina A, Cole DK, Van Den Berg HA, Price DA, Sewell AK (2009) Tricks with tetramers: how to get the most from multimeric peptide-MHC. Immunology 126(2):147–164
Toebes M, Coccoris M, Bins A, Rodenko B, Gomez R, Nieuwkoop NJ et al (2006) Design and use of conditional MHC class I ligands. Nat Med 12(2):246–51
Bakker AH, Hoppes R, Linnemann C, Toebes M, Rodenko B, Berkers CR et al (2008) Conditional MHC class I ligands and peptide exchange technology for the human MHC gene products HLA-A1, -A3, -A11, and -B7. Proc Natl Acad Sci 105(10):3825–3830
Anjanappa R, Garcia-Alai M, Kopicki J-D, Lockhauserbäumer J, Aboelmagd M, Hinrichs J et al (2020) Structures of peptide-free and partially loaded MHC class I molecules reveal mechanisms of peptide selection. Nat Commun 11(1):1–11
Saini SK, Tamhane T, Anjanappa R, Saikia A, Ramskov S, Donia M et al (2019) Empty peptide-receptive MHC class I molecules for efficient detection of antigen-specific T cells. Sci Immunol 4(37)
Hadrup SR, Bakker AH, Shu CJ, Andersen RS, van Veluw J, Hombrink P et al (2009) Parallel detection of antigen-specific T-cell responses by multidimensional encoding of MHC multimers. Nat Methods 6(7):520–6
Bentzen AK, Marquard AM, Lyngaa R, Saini SK, Ramskov S, Donia M et al (2016) Large-scale detection of antigen-specific T cells using peptide-MHC-I multimers labeled with DNA barcodes. Nat Biotechnol 34(10):1037–45
Leen AM, Bollard CM, Mendizabal AM, Shpall EJ, Szabolcs P, Antin JH et al (2013) Multicenter study of banked third-party virus-specific T cells to treat severe viral infections after hematopoietic stem cell transplantation. Blood 121(26):5113–5123
Tzannou I, Papadopoulou A, Naik S, Leung K, Martinez CA, Ramos CA et al (2017) Off-the-shelf virus-specific T cells to treat BK virus, human herpesvirus 6, cytomegalovirus, epstein-barr virus, and adenovirus infections after allogeneic hematopoietic stem-cell transplantation. J Clin Oncol 35(31):3547
Withers B, Blyth E, Clancy LE, Yong A, Fraser C, Burgess J et al (2017) Long-term control of recurrent or refractory viral infections after allogeneic HSCT with third-party virus-specific T cells. Blood Adv 1(24):2193–2205
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Molvi, Z., O’Reilly, R.J. (2022). Allogeneic Tumor Antigen-Specific T Cells for Broadly Applicable Adoptive Cell Therapy of Cancer. In: Hays, P. (eds) Cancer Immunotherapies. Cancer Treatment and Research, vol 183. Springer, Cham. https://doi.org/10.1007/978-3-030-96376-7_4
Download citation
DOI: https://doi.org/10.1007/978-3-030-96376-7_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-96375-0
Online ISBN: 978-3-030-96376-7
eBook Packages: MedicineMedicine (R0)