Abstract
Long-term functional outcomes of microsurgical resection for cavernous malformations of the brainstem (CMB) have been largely unknown. Favorable outcomes after CMB surgery might be related to the achievement of complete resection and mRS at 1 month after the surgery. Preoperative sensory, cerebellar, trigeminal nerve, and lower cranial nerve symptoms tended to improve after surgery.
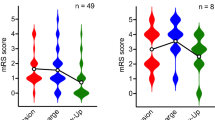
We evaluated 25 consecutive patients with CMB surgically treated at our center between 2006 and 2021. The subjects included 11 men and 14 women, with ages ranging from 13 to 61 years (mean ± SD = 37 ± 12 years). Modified Rankin Scale (mRS) scores and neurological symptoms of the patients were evaluated before surgery, 1 month after surgery, and at the final follow-up at the outpatient clinic. The mean number of previous hemorrhages was 7 ± 1.0 and the mean lesion size was 21 ± 8 mm. The mRS scores on admission and at the final follow-up were 2.9 points and 1.7 points, respectively. The mRS scores at the final follow-up were significantly improved compared to those on admission. There was no statistical difference between the preoperative mRS and mRS at 1 month after the operation. Multivariable analysis indicated that mRS scores at 1 month after surgery were the most significant predictive factors for favorable outcomes. Complete resection was achieved in 24 of 33 operations. Incomplete resection was significantly related to the frequency of subsequent recurrent hemorrhage and high mRS scores at the final follow-up. Preoperative sensory, cerebellar, trigeminal nerve, and lower cranial nerve symptoms improved significantly after surgery.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Porter RW, Detwiler PW, Spetzler RF, Lawton MT, Baskin JJ, Derksen PT, Zabramski JM. Cavernous malformations of the brainstem: experience with 100 patients. J Neurosurg. 1999;90(1):50–8. https://doi.org/10.3171/jns.1999.90.1.0050.
Samii M, Eghbal R, Carvalho GA, Matthies C. Surgical management of brainstem cavernomas. J Neurosurg. 2001;95(5):825–32. https://doi.org/10.3171/jns.2001.95.5.0825.
Russel DS, Rubinstein LJ. Tumors and hematomas of the blood vessels. In: Russel DS, Rubinstein LJ, editors. The pathology of tumors of the nervous system. London: Arnold; 1959. p. 72–92.
Zabramski JM, Henn JS, Coons S. Pathology of cerebral vascular malformations. Neurosurg Clin N Am. 1999;10(3):395–410.
Zabramski JM, Wascher TM, Spetzler RF, Johnson B, Golfinos J, Drayer BP, Brown B, Rigamonti D, Brown G. The natural history of familial cavernous malformations: results of an ongoing study. J Neurosurg. 1994;80(3):422–32. https://doi.org/10.3171/jns.1994.80.3.0422.
Eisner W, Schmid UD, Reulen HJ, Oeckler R, Olteanu-Nerbe V, Gall C, Kothbauer K. The mapping and continuous monitoring of the intrinsic motor nuclei during brain stem surgery. Neurosurgery. 1995;37(2):255–65. https://doi.org/10.1227/00006123-199508000-00010.
Bertalanffy H, Tissira N, Krayenbühl N, Bozinov O, Sarnthein J. Inter- and intrapatient variability of facial nerve response areas in the floor of the fourth ventricle. Neurosurgery. 2011;68(1 Suppl Operative):23–31.; ; discussion 31. https://doi.org/10.1227/NEU.0b013e31820781fb.
Sarnthein J, Bozinov O, Melone AG, Bertalanffy H. Motor-evoked potentials (MEP) during brainstem surgery to preserve corticospinal function. Acta Neurochir. 2011;153(9):1753–9. https://doi.org/10.1007/s00701-011-1065-7. Epub 2011 Jun 10
Fritschi JA, Reulen HJ, Spetzler RF, Zabramski JM. Cavernous malformations of the brain stem. A review of 139 cases. Acta Neurochir. 1994;130(1–4):35–46. https://doi.org/10.1007/BF01405501.
Sandalcioglu IE, Wiedemayer H, Secer S, Asgari S, Stolke D. Surgical removal of brain stem cavernous malformations: surgical indications, technical considerations, and results. J Neurol Neurosurg Psychiatry. 2002;72(3):351–5. https://doi.org/10.1136/jnnp.72.3.351.
Chen LH, Zhang HT, Chen L, Liu LX, Xu RX. Minimally invasive resection of brainstem cavernous malformations: surgical approaches and clinical experiences with 38 patients. Clin Neurol Neurosurg. 2014;116:72–9. https://doi.org/10.1016/j.clineuro.2013.10.012. Epub 2013 Oct 31
Kikuta K, Nozaki K, Takahashi JA, Miyamoto S, Kikuchi H, Hashimoto N. Postoperative evaluation of microsurgical resection for cavernous malformations of the brainstem. J Neurosurg. 2004;101(4):607–12. https://doi.org/10.3171/jns.2004.101.4.0607.
Tsuji Y, Kar S, Bertalanffy H. Microsurgical management of midbrain cavernous malformations: predictors of outcome and lesion classification in 72 patients. Oper Neurosurg (Hagerstown). 2019;17(6):562–72. https://doi.org/10.1093/ons/opz026.
de Oliveira JG, Lekovic GP, Safavi-Abbasi S, Reis CV, Hanel RA, Porter RW, Preul MC, Spetzler RF. Supracerebellar infratentorial approach to cavernous malformations of the brainstem: surgical variants and clinical experience with 45 patients. Neurosurgery. 2010;66(2):389–99. https://doi.org/10.1227/01.NEU.0000363702.67016.5D.
Bertalanffy H, Ichimura S, Kar S, Tsuji Y, Huang C. Optimal access route for pontine cavernous malformation resection with preservation of abducens and facial nerve function. J Neurosurg. 2020:1–10. https://doi.org/10.3171/2020.7.JNS201023.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Kikuta, Ki. et al. (2022). Functional Outcomes of Microsurgical Resection for Cavernous Malformations of the Brainstem. In: Kato, Y., Ansari, A. (eds) Cerebrovascular Surgery. Advances and Technical Standards in Neurosurgery, vol 44. Springer, Cham. https://doi.org/10.1007/978-3-030-87649-4_6
Download citation
DOI: https://doi.org/10.1007/978-3-030-87649-4_6
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-87648-7
Online ISBN: 978-3-030-87649-4
eBook Packages: MedicineMedicine (R0)