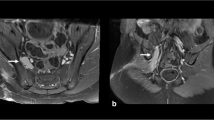
Abstract
This chapter reviews a variety of non-neurogenic tumoral and pseudotumoral lesions affecting nerve. These may include benign entities such as ganglion cysts, adipose lesions of nerve, and neuromuscular choristomas or malignant ones such as metastases with perineural spread. Knowledge of their clinicoradiological features can generate a differential diagnosis, in some cases establishing a diagnosis without the need for biopsy. These findings have treatment implications.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Desy NM, Wang H, Elshiekh MA, et al. Intraneural ganglion cysts: a systematic review and reinterpretation of the world’s literature. J Neurosurg. 2016;125(3):615–30.
Spinner RJ, Atkinson JL, Tiel RL. Peroneal intraneural ganglia: the importance of the articular branch. A unifying theory. J Neurosurg. 2003;99(2):330–43.
Spinner RJ, Atkinson JL, Scheithauer BW, et al. Peroneal intraneural ganglia: the importance of the articular branch. Clinical series. J Neurosurg. 2003;99(2):319–29.
Prasad N, Amrami KK, Winn J, Spinner RJ. Cystic adventitial disease in the popliteal artery with a joint connection to the superior tibiofibular joint: radiological evidence to support the unifying articular theory. Clin Anat. 2015;28(8):957–9.
McCarthy CL, McNally EG. The MRI appearance of cystic lesions around the knee. Skeletal Radiol. 2004;33(4):187–209.
Shahid KR, Spinner RJ, Skinner JA, et al. Evaluation of intraneural ganglion cysts using three-dimensional fast spin echo-cube. J Magn Reson Imaging. 2010;32(3):714–8.
Spinner RJ, Scheithauer BW, Amrami KK, Wenger DE, Hebert-Blouin MN. Adipose lesions of nerve: the need for a modified classification. J Neurosurg. 2012;116(2):418–31.
Marek T, Amrami KK, Mahan MA, Spinner RJ. Intraneural lipomas: institutional and literature review. Acta Neurochir. 2018;160(11):2209–18.
Teles AR, Finger G, Schuster MN, Gobbato PL. Peripheral nerve lipoma: case report of an intraneural lipoma of the median nerve and literature review. Asian J Neurosurg. 2016;11(4):458.
Kamble P, Vanan K, Mohanty SS, Rathod T, Sahay A. Intraneural lipoma with cartilagenous metaplasia of median nerve. J Case Rep. 2017;7(3):303–5.
Park SE, Lee JU, Ji JH. Intraneural chondroid lipoma on the common peroneal nerve. Knee Surg Sports Traumatol Arthrosc. 2011;19(5):832–4.
Marek T, Spinner RJ, Syal A, Mahan MA. Strengthening the association of lipomatosis of nerve and nerve-territory overgrowth: a systematic review. J Neurosurg. 2019;132(4):1286–94.
Fletcher C, Unni K, Mertens F. World Health Organisation classification of tumours. In: Pathology and genetics: tumours of soft tissue and bone. Lyon: IARC Press; 2002.
Marek T, Mahan MA, Carter JM, Amrami KK, Atkinson JL, Spinner RJ. Can lipomatosis of the nerve occur or extend intradurally? World Neurosurg. 2019;129:e555–60.
Marom EM, Helms CA. Fibrolipomatous hamartoma: pathognomonic on MR imaging. Skeletal Radiol. 1999;28(5):260–4.
Mahan MA, Niederhauser BD, Amrami KK, Spinner RJ. Long-term progression of lipomatosis of nerve. World Neurosurg. 2014;82(3–4):492–9.
Marek T, Howe BM, Amrami KK, Taunton MJ, Spinner RJ. Unrecognized lipomatosis of the femoral nerve and nerve-territory overgrowth. Clin Anat. 2018;31(8):1210–4.
Mahan MA, Amrami KK, Spinner RJ. Sciatic nerve lipomatosis and knee osteochondroma. J Neurosurg. 2013;119(4):934.
Keppler-Noreuil KM, Rios JJ, Parker VE, et al. PIK3CA-related overgrowth spectrum (PROS): diagnostic and testing eligibility criteria, differential diagnosis, and evaluation. Am J Med Genet A. 2015;167A(2):287–95.
Blackburn PR, Milosevic D, Marek T, et al. PIK3CA mutations in lipomatosis of nerve with or without nerve territory overgrowth. Mod Pathol. 2020;33(3):420–30.
Marek T, Mahan MA, Carter JM, Amrami KK, Benarroch EE, Spinner RJ. Lipomatosis of nerve and overgrowth: is there a preference for motor (mixed) vs. sensory nerve involvement? Acta Neurochir. 2019;161(4):679–84.
Marek T, Spinner RJ, Syal A, Wahood W, Mahan MA. Surgical treatment of lipomatosis of nerve: a systematic review. World Neurosurg. 2019;128:587–592.e582.
Kumar R, Howe BM, Amrami KK, Spinner RJ. Neuromuscular choristoma of the sciatic nerve and lumbosacral plexus: an association with nerve-territory undergrowth in the pelvis affecting soft tissue and bone. Acta Neurochir. 2014;156(5):1041–6.
Niederhauser BD, Spinner RJ, Jentoft ME, Everist BM, Matsumoto JM, Amrami KK. Neuromuscular choristoma: characteristic magnetic resonance imaging findings and association with post-biopsy fibromatosis. Skeletal Radiol. 2013;42(4):567–77.
Stone JJ, Prasad NK, Laumonerie P, et al. Recurrent desmoid-type fibromatosis associated with underlying neuromuscular choristoma. J Neurosurg. 2018;131(1):175–83.
Lazar AJ, Tuvin D, Hajibashi S, et al. Specific mutations in the beta-catenin gene (CTNNB1) correlate with local recurrence in sporadic desmoid tumors. Am J Pathol. 2008;173(5):1518–27.
Kayahara M, Nakagawara H, Kitagawa H, Ohta T. The nature of neural invasion by pancreatic cancer. Pancreas. 2007;35(3):218–23.
Brown IS. Pathology of perineural spread. J Neurol Surg B Skull Base. 2016;77(2):124–30.
Badger D, Aygun N. Imaging of perineural spread in head and neck cancer. Radiol Clin North Am. 2017;55(1):139–49.
Laumonerie P, Capek S, Amrami KK, Dyck PJ, Spinner RJ. Targeted fascicular biopsy of the brachial plexus: rationale and operative technique. Neurosurg Focus. 2017;42(3):E9.
Marek T, Howe BM, Amrami KK, Spinner RJ. Perineural spread of nonmelanoma skin cancer to the brachial plexus: identifying anatomic pathway(s). World Neurosurg. 2018;114:e818–23.
Capek S, Howe BM, Amrami KK, Spinner RJ. Perineural spread of pelvic malignancies to the lumbosacral plexus and beyond: clinical and imaging patterns. Neurosurg Focus. 2015;39(3):E14.
Stone JJ, Adamo DA, Khan DZ, et al. Multimodal imaging aids in the diagnosis of perineural spread of prostate cancer. World Neurosurg. 2019;122:e235–40.
Capek S, Amrami KK, Dyck PJ, Spinner RJ. Targeted fascicular biopsy of the sciatic nerve and its major branches: rationale and operative technique. Neurosurg Focus. 2015;39(3):E12.
Marek T, Stone JJ, Amrami KK, Spinner RJ. Targeted nerve biopsy: a technique in evolution. Clin Anat. 2018;31(8):1200–4.
Capek S, Hebert-Blouin MN, Puffer RC, et al. Tumefactive appearance of peripheral nerve involvement in hematologic malignancies: a new imaging association. Skeletal Radiol. 2015;44(7):1001–9.
DeVries AH, Howe BM, Spinner RJ, Broski SM. B-cell peripheral neurolymphomatosis: MRI and (18)F-FDG PET/CT imaging characteristics. Skeletal Radiol. 2019;48(7):1043–50.
Mathey EK, Park SB, Hughes RA, et al. Chronic inflammatory demyelinating polyradiculoneuropathy: from pathology to phenotype. J Neurol Neurosurg Psychiatry. 2015;86(9):973–85.
Dalakas MC. Medscape. Advances in the diagnosis, pathogenesis and treatment of CIDP. Nat Rev Neurol. 2011;7(9):507–17.
McKenzie GA, Broski SM, Howe BM, et al. MRI of pathology-proven peripheral nerve amyloidosis. Skeletal Radiol. 2017;46(1):65–73.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Marek, T., Amrami, K.K., Spinner, R.J. (2021). Non-neurogenic Tumoral and Pseudotumoral Lesions Affecting Peripheral Nerve. In: Guedes, F., Zager, E.L., Garozzo, D., Rasulic, L., Socolovsky, M. (eds) Diagnostic Assessment and Treatment of Peripheral Nerve Tumors. Springer, Cham. https://doi.org/10.1007/978-3-030-77633-6_18
Download citation
DOI: https://doi.org/10.1007/978-3-030-77633-6_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-77632-9
Online ISBN: 978-3-030-77633-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)