Abstract
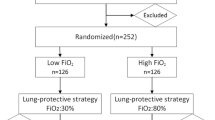
In the recently updated international “democracy-based” consensus conference aimed at identifying all nonsurgical strategies which have been shown by sufficiently strong randomized evidence to affect mortality in the perioperative and critical care setting, restrictive inspiratory oxygen fraction (FiO2) was included among interventions reducing mortality. This conclusion was based on the findings of two randomized controlled trials showing a lower intensive care unit (ICU) mortality with a “conservative” FiO2 approach in critically ill patients and an increased long-term mortality in surgical patients receiving high intraoperative FiO2, respectively. However, there is also evidence that high perioperative FiO2 may reduce mortality (possibly through prevention of surgical site infection) among surgical patients, while recent investigations did not confirm (or found a high level of uncertainty about) the survival benefit of restrictive FiO2 strategies in ICU patients. This chapter discusses the main evidences about the topic, the possible mechanisms of the association between FiO2 and mortality, and the implications for clinical practice.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Young PJ, Beasley RW, Capellier G, et al. Oxygenation targets, monitoring in the critically ill: a point prevalence study of clinical practice in Australia and New Zealand. Crit Care Resusc. 2015;17:202–7.
Kraft F, Andel H, Gamper J, et al. Incidence of hyperoxia and related in-hospital mortality in critically ill patients: a retrospectivedata analysis. Acta Anaesthesiol Scand. 2018;62(3):347–56.
Palmer E, Post B, Klapaukh R, et al. The association between supraphysiologic arterial oxygen levels and mortality in critically ill patients: a multicenter observational cohort study. Am J Respir Crit Care Med. 2019;200:1373–80.
Blum JM, Fetterman DM, Park PK, et al. A description of intraoperative ventilator management and ventilation strategies in hypoxic patients. Anesth Analg. 2010;110:1616–22.
Staehr-Rye AK, Meyhoff CS, Scheffenbichler FT, et al. High intraoperative inspiratory oxygen fraction and risk of major respiratory complications. Br J Anaesth. 2017;119(1):140–9.
Chu DK, Kim LH, Young PJ, et al. Mortality and morbidity in acutely ill adults treated with liberal versus conservative oxygen therapy (IOTA): a systematic review and meta-analysis. Lancet. 2018;391(10131):1693–705.
Pisano A, Capasso A. Perioperative supplemental oxygen to reduce perioperative mortality. In: Landoni G, Ruggeri L, Zangrillo A, editors. Reducing mortality in the perioperative period. Cham: Springer; 2014. p. 77–83.
Hedenstierna G, Meyhoff CS. Oxygen toxicity in major emergency surgery-anything new? Intensive Care Med. 2019;45(12):1802–5.
O’Driscoll BR, Howard LS, Earis J, Mak V, British Thoracic Society Emergency Oxygen Guideline Group. BTS guideline for oxygen use in adults in healthcare and emergency settings. Thorax. 2017;72(suppl 1):ii1–ii90.
Girardis M, Busani S, Damiani E, et al. Effect of conservative vs conventional oxygen therapy on mortality among patients in an intensive care unit: the oxygen-ICU randomized clinical trial. JAMA. 2016;316(15):1583–9.
Meyhoff CS, Jorgensen LN, Wetterslev J, et al; PROXI Trial Group. Increased long-term mortality after a high perioperative inspiratory oxygen fraction during abdominal surgery: follow-up of a randomized clinical trial. Anesth Analg. 2012;115(4):849–54.
Sartini C, Lomivorotov V, Pieri M, et al. A systematic review and international web-based survey of randomized controlled trials in the perioperative and critical care setting: interventions reducing mortality. J Cardiothorac Vasc Anesth. 2019;33(5):1430–9.
Pisano A, Oppizzi M, Turi S, Landoni G. Reducing major adverse cardiac events and all-cause mortality in noncardiac surgery: perioperative strategies. In: Kaplan JA, Cronin B, Maus TM, editors. Kaplan’s essentials of cardiac anesthesia for noncardiac surgery. Philadelphia, PA: Elsevier; 2019. p. 538–77.
Pisano A. Perioperative supplemental oxygen to reduce surgical site infection: too easy to be true. J Trauma Acute Care Surg. 2014;76(5):1332.
ICU-ROX Investigators and The Australian and New Zealand Intensive Care Society Clinical Trials Group, Mackle D, Bellomo R, Bailey M, et al. Conservative oxygen therapy during mechanical ventilation in the ICU. N Engl J Med. 2019; https://doi.org/10.1056/NEJMoa1903297. [Epub ahead of print]
Ferrando C, Aldecoa C, Unzueta C, et al. Effects of oxygen on post-surgical infections during an individualised perioperative open-lung ventilatory strategy: a randomised controlled trial. Br J Anaesth. 2020;124(1):110–20.
de Jonge S, Egger M, Latif A, et al. Effectiveness of 80% vs 30–35% fraction of inspired oxygen in patients undergoing surgery: an updated systematic review and meta-analysis. Br J Anaesth. 2019;122(3):325–34.
Barbateskovic M, Schjørring OL, Russo Krauss S, et al. Higher versus lower fraction of inspired oxygen or targets of arterial oxygenation for adultsadmitted to the intensive care unit. Cochrane Database Syst Rev. 2019;2019(11):8.
Smith BK, Roberts RH, Frizelle FA. O2 no longer the Go2: a systematic review and meta-analysis comparing the effects of giving perioperative oxygen therapy of 30% FiO2 to 80% FiO2 on surgical site infection and mortality. World J Surg. 2020;44(1):69–77.
Sartini C, Lomivorotov V, Pisano A, et al. A systematic review and international web-based survey of randomized controlled trials in the perioperative and critical care setting: interventions increasing mortality. J Cardiothorac Vasc Anesth. 2019;33(10):2685–94.
Meyhoff CS, Wetterslev J, Jorgensen LN, PROXI Trial Group, et al. Effect of high perioperative oxygen fraction on surgical site infection and pulmonary complications after abdominal surgery: the PROXI randomized clinical trial. JAMA. 2009;302:1543–50.
Smit B, Smulders YM, van der Wouden JC, et al. Hemodynamic effects of acute hyperoxia: systematic review and meta-analysis. Crit Care. 2018;22(1):45.
Hedenstierna G, Edmark L. Mechanisms of atelectasis in the perioperative period. Best Pract Res Clin Anaesthesiol. 2010;24(2):157–69.
Graham K, Unger E. Overcoming tumor hypoxia as a barrier to radiotherapy, chemotherapy and immunotherapy in cancer treatment. Int J Nanomedicine. 2018;13:6049–58.
Young P, Mackle D, Bellomo R, ICU-ROX Investigators the Australian New Zealand Intensive Care Society Clinical Trials Group, et al. Conservative oxygen therapy for mechanically ventilated adults with sepsis: a post hoc analysis of data from the intensive care unit randomized trial comparing two approaches to oxygen therapy (ICU-ROX). Intensive Care Med. 2020;46(1):17–26.
Young PJ, Bellomo R. The risk of hyperoxemia in ICU patients. Much ado about O2. Am J Respir Crit Care Med. 2019;200(11):1333–5.
Schjørring OL, Perner A, Wetterslev J, HOT-ICU Investigators, et al. Handling oxygenation targets in the intensive care unit (HOT-ICU)-protocol for a randomised clinical trial comparing a lower vs a higher oxygenation target in adults with acute hypoxaemic respiratory failure. Acta Anaesthesiol Scand. 2019;63:956–65.
Li XF, Jiang D, Jiang YL, et al. PROtective ventilation with a low versus high inspiratory oxygen fraction (PROVIO) and its effects on postoperative pulmonary complications: protocol for a randomized controlled trial. Trials. 2019;20(1):619.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Pisano, A., Venditto, M., Verniero, L. (2021). Restrictive Inspiratory Oxygen Fraction. In: Landoni, G., Baiardo Redaelli, M., Sartini, C., Zangrillo, A., Bellomo, R. (eds) Reducing Mortality in Critically Ill Patients. Springer, Cham. https://doi.org/10.1007/978-3-030-71917-3_4
Download citation
DOI: https://doi.org/10.1007/978-3-030-71917-3_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-71916-6
Online ISBN: 978-3-030-71917-3
eBook Packages: MedicineMedicine (R0)