Abstract
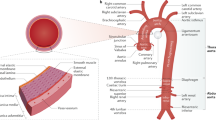
Acute aortic dissection (AAD)—characterized by the presence of an intimal flap separating the true and false lumen—represents a life-treating medical condition affecting the aorta wall interesting predominantly the media layer. Most frequently it affects men (~65%), in the sixth decade of life (mean age 63 years). Overall incidence ranges from approximately 2.6 and 3.5 cases per 100,000 person-years (6000–10,000 cases annually in the USA. AAD may be caused by a wide spectrum of congenital or acquired diseases, either acute or chronic, variably leading to increased aortic wall stress (e.g. systemic arterial hypertension, cocaine, physical trauma, etc.). and/or aortic media abnormalities (e.g. syndromic and non-syndromic genetic diseases, inflammatory vasculitis, atherosclerosis, etc.). However, despite recent diagnostic and therapeutic advances, aortic disease burden is still high. Thus there is an urgent need to design and implement preventive strategies at individual and population levels targeting cardiovascular risk factors. In this context it is “conditio sine qua non” promoting health life style along with screening programs for early detection of systemic arterial hypertension and abdominal aneurysms. Consistent patients long term follow-up after acute index event represents an evident gap to be filled.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Braverman AC, Schermerhorn M. Diseases of the aorta. In: Braunwald’s heart disease: a textbook of cardiovascular medicine. 11th ed. Philadelphia, PA: Elsevier; 2018. p. 1295–337.
Erbel R, Aboyans V, Boileau C, Bossone E, Bartolomeo RD, Eggebrecht H, et al. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases: document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult. The Task Force for the Diagnosis and Treatment of Aortic Diseases of the European Society of Cardiology (ESC). Eur Heart J. 2014;35:2873–926. https://doi.org/10.1093/eurheartj/ehu281.
Hiratzka LF, Bakris GL, Beckman JA, Bersin RM, Carr VF, Casey DE, et al. 2010 ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM Guidelines for the diagnosis and management of patients with thoracic aortic disease. A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. J Am Coll Cardiol. 2010;55:e27–e129. https://doi.org/10.1016/j.jacc.2010.02.015.
Evangelista A, Isselbacher EM, Bossone E, Gleason TG, Eusanio MD, Sechtem U, et al. Insights from the international registry of acute aortic dissection: a 20-year experience of collaborative clinical research. Circulation. 2018;137:1846–60. https://doi.org/10.1161/CIRCULATIONAHA.117.031264.
Mészáros I, Mórocz J, Szlávi J, et al. Epidemiology and clinicopathology of aortic dissection. Chest. 2000;117:1271–8. https://doi.org/10.1378/chest.117.5.1271.
Clouse WD, Hallett JW Jr, Schaff HV, et al. Acute aortic dissection: population-based incidence compared with degenerative aortic aneurysm rupture. Mayo Clin Proc. 2004;79:176–80. https://doi.org/10.4065/79.2.176.
Bossone E, LaBounty TM, Eagle KA. Acute aortic syndromes: diagnosis and management, an update. Eur Heart J. 2018;39:739–749d. https://doi.org/10.1093/eurheartj/ehx319.
Nienaber CA, Clough RE. Management of acute aortic dissection. Lancet. 2015;385:800–11. https://doi.org/10.1016/S0140-6736(14)61005-9.
Bossone E, Ranieri B, Romano L, et al. Acute aortic syndromes: diagnostic and therapeutic pathways. Heart Fail Clin. 2020;16:305–15. https://doi.org/10.1016/j.hfc.2020.03.002.
Pape LA, Tsai TT, Isselbacher EM, Oh JK, O'gara PT, Evangelista A, et al. Aortic diameter >or = 5.5 cm is not a good predictor of type A aortic dissection: observations from the International Registry of Acute Aortic Dissection (IRAD). Circulation. 2007;116:1120–7. https://doi.org/10.1161/CIRCULATIONAHA.107.702720.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension [published correction appears in Eur Heart J. 2019 Feb 1;40:475]. Eur Heart J. 2018;39:3021–104. https://doi.org/10.1093/eurheartj/ehy339.
Runyan B, Hanak CR, Mahendiran S, Allamaneni S, Vester S. Type A aortic dissection complicated by pheochromocytoma. Ann Thorac Surg. 2019;107:e13–4. https://doi.org/10.1016/j.athoracsur.2018.05.084.
Lenders JW, Duh QY, Eisenhofer G, Gimenez-Roqueplo AP, Grebe SK, Murad MH, et al. Pheochromocytoma and paraganglioma: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2014;99:1915–42. https://doi.org/10.1210/jc.2014-1498.
Eagle KA, Isselbacher EM, De Sanctis RW, International Registry for Aortic Dissection (IRAD) Investigators. Cocaine-related aortic dissection in perspective. Circulation. 2002;105:1529–30. https://doi.org/10.1161/01.cir.105.13.1529.
Dean JH, Woznicki EM, O'Gara P, Montgomery DG, Trimarchi S, Myrmel T, et al. Cocaine-related aortic dissection: lessons from the International Registry of Acute Aortic Dissection. Am J Med. 2014;127:878–85. https://doi.org/10.1016/j.amjmed.2014.05.005.
Hatzaras I, Tranquilli M, Coady M, Barrett PM, Bible J, Elefteriades JA. Weight lifting and aortic dissection: more evidence for a connection. Cardiology. 2007;107:103–6. https://doi.org/10.1159/000094530.
January 2020 - n°1 by Orphanet: an online database of rare diseases and 890 orphan drugs. Copyright, INSERM 1997. Available at http://www.orpha.net
Aftab M, Cikach FS, Zhu Y, Idrees JJ, Rigelsky CM, Kalahasti V, et al. Loeys-Dietz syndrome: Intermediate-term outcomes of medically and surgically managed patients. J Thorac Cardiovasc Surg. 2019;157:439–50.e5. https://doi.org/10.1016/j.jtcvs.2018.03.172.
Loughborough WW, Minhas KS, Rodrigues JCL, et al. Cardiovascular manifestations and complications of Loeys-Dietz syndrome: CT and MR imaging findings. Radiographics. 2018;38:275–86. https://doi.org/10.1148/rg.2018170120.
Williams JA, Hanna JM, Shah AA, et al. Adult surgical experience with Loeys-Dietz syndrome. Ann Thorac Surg. 2015;99:1275–81. https://doi.org/10.1016/j.athoracsur.2014.11.021.
Thunström S, Krantz E, Thunström E, Hanson C, Bryman I, Landin-Wilhelmsen K. Incidence of aortic dissection in turner syndrome. Circulation. 2019;139:2802–4. https://doi.org/10.1161/CIRCULATIONAHA.119.040552.
D’Souza RS, Slavov D, Graw S, Jirikowic J, Todd E, Rogers RK, et al. Clinical and genetic characterization of adult patients presenting with non-syndromic vascular aneurysms and dissections. Int Angiol. 2017;36:417–27. https://doi.org/10.23736/S0392-9590.17.03757-9.
Di Eusanio M, Pape L, Braverman AC, et al. Characteristics of acute aortic dissection in patients with bicuspid 781 aortic valve: insights from the IRAD registry [abstract]. Circulation. 2013;128:A15913.
Bossone E, Pluchinotta FR, Andreas M, et al. Aortitis. Vasc Pharmacol. 2016;80:1–10. https://doi.org/10.1016/j.vph.2015.11.084.
Yoshimoto R, Tanaka K, Kawahata T, Takatori S, Takatori K, Eguchi K, et al. Unusual manifestations of giant cell arteritis and granulomatosis with polyangiitis. Immunol Med. 2019;42:94–8. https://doi.org/10.1080/25785826.2019.1657377.
Kamel H, Roman MJ, Pitcher A, Devereux RB. Pregnancy and the risk of aortic dissection or rupture: a cohort-crossover analysis. Circulation. 2016;134:527–33. https://doi.org/10.1161/CIRCULATIONAHA.116.021594.
Tajima Y, Goto H, Ohara M, Hashimoto M, Akamatsu D, Shimizu T, et al. Oral steroid use and abdominal aortic aneurysm expansion - positive association. Circ J. 2017;81:1774–82. https://doi.org/10.1253/circj.CJ-16-0902.
Lee CC, Lee MG, Hsieh R, Porta L, Lee W-C, Lee SH, Chang S-S. Oral fluoroquinolone and the risk of aortic dissection. J Am Coll Cardiol. 2018;72:1369–78. https://doi.org/10.1016/j.jacc.2018.06.067.
Hartlage GR, Palios J, Barron BJ, et al. Multimodality imaging of aortitis. JACC Cardiovasc Imaging. 2014;7:605–19. https://doi.org/10.1016/j.jcmg.2014.04.002.
Meel R, Gonçalves R. Human immunodeficiency virus associated large artery disease. In Aortic aneurysm and aortic dissection [Working Title]. IntechOpen (2019). doi:https://doi.org/10.5772/intechopen.85956.
Núñez-Gil IJ, Bautista D, Cerrato E, Salinas P, Varbella F, Omedè P, et al. Incidence, management, and immediate- and long-term outcomes after iatrogenic aortic dissection during diagnostic or interventional coronary procedures. Circulation. 2015;131:2114–9. https://doi.org/10.1161/CIRCULATIONAHA.115.015334.
Sampson UK, Norman PE, Fowkes FG, et al. Global and regional burden of aortic dissection and aneurysms: mortality trends in 21 world regions, 1990 to 2010. Glob Heart. 2014;9:171–180.e10. https://doi.org/10.1016/j.gheart.2013.12.010.
Piepoli MF, Hoes AW, Agewall S, Albus C, Brotons C, Catapano AL, et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts) Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur Heart J. 2016;37:2315–81. https://doi.org/10.1093/eurheartj/ehw106.
Mach F, Baigent C, Catapano AL, et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J. 2020;41:111–88. https://doi.org/10.1093/eurheartj/ehz455.
Chaddha A, Kline-Rogers E, Woznicki EM, Brook R, Housholder-Hughes S, Braverman AC, et al. Cardiology patient page. Activity recommendations for postaortic dissection patients. Circulation. 2014;130:e140–2. https://doi.org/10.1161/CIRCULATIONAHA.113.005819.
Chaddha A, Kline-Rogers E, Braverman AC, et al. Survivors of aortic dissection: activity, mental health, and sexual function. Clin Cardiol. 2015;38:652–9. https://doi.org/10.1002/clc.22418.
Chaddha A, Eagle KA, Braverman AC, et al. Exercise and physical activity for the post-aortic dissection patient: the clinician’s conundrum. Clin Cardiol. 2015;38:647–51. https://doi.org/10.1002/clc.22481.
Chaddha A, Erickson S, Kline-Rogers E, et al. Medication adherence patterns in aortic dissection survivors. Indian J Med Res. 2018;147:183–8. https://doi.org/10.4103/ijmr.IJMR_1198_15.
Acknowledgments
We are grateful to Dr. Brigida Ranieri and to Chiara Sepe for data management and technical support.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Bossone, E., Russo, V., Salzano, A., Eagle, K. (2021). Medical Conditions Predisposing to Aortic Dissection and Preventive Strategies. In: Sellke, F.W., Coselli, J.S., Sundt, T.M., Bavaria, J.E., Sodha, N.R. (eds) Aortic Dissection and Acute Aortic Syndromes. Springer, Cham. https://doi.org/10.1007/978-3-030-66668-2_7
Download citation
DOI: https://doi.org/10.1007/978-3-030-66668-2_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-66667-5
Online ISBN: 978-3-030-66668-2
eBook Packages: MedicineMedicine (R0)