Abstract
Advances in the fields of reconstructive and gender-affirming surgery during the last three to four decades have resulted in there being a multitude of surgical options available for patients who seek genital gender affirming surgery (gGAS). Advances in gender transition-related mental health and sexual medicine have also enriched the field and improved surgical care options for people undergoing gender transition.
It follows, then, that, for a surgeon, the process of facilitating informed patient centered decision-making about surgical options has become more complex and nuanced. Which specific surgical options are offered to patients, and how these options are presented, explained, and contrasted, is essential to meeting their varied needs and expectations.
While the gGAS literature has an increasing number of studies that retrospectively study surgical outcomes, there is significantly less in the literature about discussion approaches for how to prospectively present the relative advantages and disadvantages of different gGAS options to patients.
Herein we review common surgical options and techniques, and highlight relative advantages and disadvantages with respect to functionality, cosmesis, morbidity, short- and long-term surgical risks, and self-care requirements.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Notes
- 1.
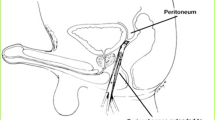
Penile foreskin that is tight owing to phimosis, or which is of poor quality due to chronic inflammation, is often unusable for use to line the vaginal canal space. In such cases, the surgeon should explain to the patient that, in order to achieve satisfactory vaginal depth, the surgeon will likely need to harvest skin or other epithelium from an additional source to line the vaginal canal (e.g., full-thickness or pedicled scrotal skin grafts or peritoneal local advancement or rotational flaps) and achieve satisfactory vaginal depth.
References
Coleman E, Bockting W, Botzer M, et al. Standards of care for the health of transsexual, transgender, and gender-nonconforming people, version 7. Int J Transgender. 2012;13(4):165–232.
Garcia MM. Men’s health and transgender surgery: a urologist’s perspective. Transl Androl Urol. 2016;5(2):225–7.
Garcia MM, Christopher NA, Thomas P, Ralph DJ. AUA updates series lesson 5: genital gender affirming surgeries for transgender patient. AUA Updates. 2017.
Bockting W, Coleman E, De Cuypere G. Care of transsexual persons. N Engl J Med. 2011;364(26):2559–60; author reply 2560
Bockting WO, Knudson G, Goldberg JM. Counseling and mental health care for transgender adults and loved ones. Int J Transgender. 2006;9:35–82.
Gardner IS, Joshua D. Progress on the road to better medical care for transgender patients. Curr Opin Endocrinol Diabet Obes. 2013;20(6):553–8.
Djordjevic ML, Stanojevic D, Bizic M, et al. Metoidioplasty as a single stage sex reassignment surgery in female transsexuals: Belgrade experience. J Sex Med. 2009;6(5):1306–13.
Djordjevic ML, Stojanovic B, Bizic M. Metoidioplasty: techniques and outcomes. Transl Androl Urol. 2019;8(3):248–53.
Lin-Brande M, Clennon E, Sajadi KP, Djordjevic ML, Dy GW, Dugi D. Metoidioplasty with urethral lengthening: a stepwise approach. Urology. 2020;S0090–4295(20)31152–3. https://doi.org/10.1016/j.urology.2020.09.013.
Garaffa G, Christopher NA, Ralph DJ. Total phallic reconstruction in female-to-male transsexuals. Eur Urol. 2010;57(4):715–22.
Monstrey S, Hoebeke P, Selvaggi G, et al. Penile reconstruction: is the radial forearm flap really the standard technique? Plast Reconstr Surg. 2009;124(2):510–8.
Monstrey SJ, Ceulemans P, Hoebeke P. Sex reassignment surgery in the female-to-male transsexual. Semin Plast Surg. 2011;25(3):229–44.
Rubino C, Figus A, Dessy LA, et al. Innervated island pedicled anterolateral thigh flap for neo-phallic reconstruction in female-to-male transsexuals. J Plast Reconstr Aesthet Surg. 2009;62(3):e45–9.
Chen ML, Reyblat P, Poh MM, Chi AC. Overview of surgical techniques in gender-affirming genital surgery. Transl Androl Urol. 2019;8(3):191–208.
Djordjevic ML, Bizic M, Stanojevic D, et al. Urethral lengthening in metoidioplasty (female-to-male sex reassignment surgery) by combined buccal mucosa graft and labia minora flap. Urology. 2009;74(2):349–53.
Djordjevic ML, Bizic MR. Comparison of two different methods for urethral lengthening in female to male (metoidioplasty) surgery. J Sex Med. 2013;10(5):1431–8.
van der Sluis WB, Smit JM, Pigot GLS, et al. Double flap phalloplasty in transgender men: surgical technique and outcome of pedicled anterolateral thigh flap phalloplasty combined with radial forearm free flap urethral reconstruction. Microsurgery. 2017;37(8):917–23.
Nikolavsky D, Hughes M, Zhao LC. Urologic complications after phalloplasty or metoidioplasty. Clin Plast Surg. 2018;45(3):425–35.
Neuville P, Morel-Journel N, Maucourt-Boulch D, Ruffion A, Paparel P, Terrier JE. Surgical outcomes of erectile implants after phalloplasty: retrospective analysis of 95 procedures. J Sex Med. 2016;13(11):1758–64.
Santucci RA. Urethral complications after transgender phalloplasty: strategies to treat them and minimize their occurrence. Clin Anat. 2018;31(2):187–90.
Esmonde N, Bluebond-Langner R, Berli JU. Phalloplasty flap-related complication. Clin Plast Surg. 2018;45(3):415–24.
Hoebeke P, Selvaggi G, Ceulemans P, et al. Impact of sex reassignment surgery on lower urinary tract function. Eur Urol. 2005;47(3):398–402.
Hoebeke PB, Decaestecker K, Beysens M, Opdenakker Y, Lumen N, Monstrey SM. Erectile implants in female-to-male transsexuals: our experience in 129 patients. Eur Urol. 2010;57(2):334–40.
Al-Tamimi M, Pigot GL, van der Sluis WB, et al. Colpectomy significantly reduces the risk of urethral fistula formation after urethral lengthening in transgender men undergoing genital gender affirming surgery. J Urol. 2018;200(6):1315–22.
Garcia MCN, Thomas P, Ralph D. Genital gender affirming surgery for transgender patients. American Urologic Association. 2017; AUA Update Series 2017.
Isaacson D, Aghili R, Wongwittavas N, Garcia M. How big is too big? The girth of bestselling insertive sex toys to guide maximal neophallus dimensions. J Sex Med. 2017;14(11):1455–61.
Garcia MM. Decision-making challenges for patients and surgeons regarding genital gender affirming surgery. In: Nikolavsky D, Blakely SA, editors. Urological care for the transgender patient. Switzerland: Springer Nature; 2020.
Garcia MM, Christopher NA, De Luca F, Spilotros M, Ralph DJ. Overall satisfaction, sexual function, and the durability of neophallus dimensions following staged female to male genital gender confirming surgery: the Institute of Urology, London U.K. experience. Transl Androl Urol. 2014;3(2):156–62.
Wessells H, Lue TF, McAninch JW. Penile length in the flaccid and erect states: guidelines for penile augmentation. J Urol. 1996;156(3):995–7.
Falcone M, Garaffa G, Gillo A, Dente D, Christopher AN, Ralph DJ. Outcomes of inflatable penile prosthesis insertion in 247 patients completing female to male gender reassignment surgery. BJU Int. 2018;121(1):139–44.
Pigot GLS, Al-Tamimi M, Ronkes B, et al. Surgical outcomes of neoscrotal augmentation with testicular prostheses in transgender men. J Sex Med. 2019;16(10):1664–71.
Garcia MM. Sexual function after shallow and full-depth vaginoplasty: challenges, clinical findings, and treatment strategies – urologic perspectives. Clin Plast Surg. 2018;45(3):437–46.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Garcia, M.M. (2021). Decision-Making in Masculinizing Surgery and Feminizing Surgery. In: Nikolavsky, D., Blakely, S.A. (eds) Urological Care for the Transgender Patient. Springer, Cham. https://doi.org/10.1007/978-3-030-18533-6_2
Download citation
DOI: https://doi.org/10.1007/978-3-030-18533-6_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-18532-9
Online ISBN: 978-3-030-18533-6
eBook Packages: MedicineMedicine (R0)