Abstract
Background and Objective
Polypharmacy, regarded as an indicator of potentially inappropriate medications (PIMs), may lead to a higher risk of serious health consequences in elderly patients with osteoporosis. Thus, this study aimed to analyze the association between polypharmacy and hip fracture in patients with osteoporosis because only a limited number of studies have reported on this association, with inconsistent results to date.
Methods
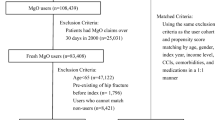
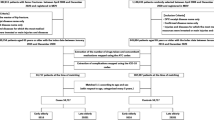
In this nested case–control study using a population-based sample cohort, the target cases were female patients with hip fracture diagnosed with osteoporosis and aged ≥ 50 years. Polypharmacy (prescription of an average of five or more daily drugs), PIMs for hip fracture (such as benzodiazepines and glucocorticoids), Charlson Comorbidity Index (CCI) score, and other comorbidities were analyzed during the year preceding the diagnosis of hip fracture. Adjusted odds ratios (ORs) for hip fracture for the variables were also analyzed.
Results
The cases (n = 1003) showed higher exposure rates to polypharmacy, glucocorticoids, and benzodiazepines, and had more severe comorbidity statuses compared with the controls. The ORs for hip fracture adjusted for confounders increased with polypharmacy level, with persistent statistical significance in most analyses. The ORs (95% confidence intervals), with reference to the 0 to < 1 drug group, were 1.65 (1.31–2.08) and 2.11 (1.12–3.96) for the 5 to < 10 and 10 + drug groups, respectively, with adjustment for PIMs, and 1.34 (1.04–1.72) and 1.45 (0.76–2.80) for the 5 to < 10 and 10 + drug groups, respectively, with adjustment for PIMs and CCI score.
Conclusions
The results suggest that polypharmacy is associated with an increased risk of hip fracture after adjustment for confounders in patients with osteoporosis. These results highlight the importance of polypharmacy management in preventing hip fractures in patients with osteoporosis.

Similar content being viewed by others
References
Cadogan CA, Ryan C, Hughes CM. Appropriate polypharmacy and medicine safety: when many is not too many. Drug Saf. 2016;39(2):109–16.
Jokanovic N, Tan EC, Dooley MJ, Kirkpatrick CM, Bell JS. Prevalence and factors associated with polypharmacy in long-term care facilities: a systematic review. J Am Med Direct Assoc. 2015;16(6):535 e1-12.
Maher RL, Hanlon J, Hajjar ER. Clinical consequences of polypharmacy in elderly. Expert Opin Drug Saf. 2014;13(1):57–65.
Kuijpers MA, van Marum RJ, Egberts AC, Jansen PA. Relationship between polypharmacy and underprescribing. Br J Clin Pharmacol. 2008;65(1):130–3.
Fried TR, O’Leary J, Towle V, Goldstein MK, Trentalange M, Martin DK. Health outcomes associated with polypharmacy in community-dwelling older adults: a systematic review. J Am Geriatr Soc. 2014;62(12):2261–72.
Dhalwani NN, Fahami R, Sathanapally H, Seidu S, Davies MJ, Khunti K. Association between polypharmacy and falls in older adults: a longitudinal study from England. BMJ Open. 2017;7(10):e016358.
Laflamme L, Monarrez-Espino J, Johnell K, Elling B, Moller J. Type, number or both? A population-based matched case-control study on the risk of fall injuries among older people and number of medications beyond fall-inducing drugs. PLoS One. 2015;10(3):e0123390.
Kannus P, Niemi S, Palvanen M, Parkkari J. Continuously increasing number and incidence of fall-induced, fracture-associated, spinal cord injuries in elderly persons. Arch Intern Med. 2000;160(14):2145–9.
Jacqmin-Gadda H, Fourrier A, Commenges D, Dartigues JF. Risk factors for fractures in the elderly. Epidemiology. 1998;9(4):417–23.
Lai SW, Liao KF, Liao CC, Muo CH, Liu CS, Sung FC. Polypharmacy correlates with increased risk for hip fracture in the elderly: a population-based study. Medicine. 2010;89(5):295–9.
Pan HH, Li CY, Chen TJ, Su TP, Wang KY. Association of polypharmacy with fall-related fractures in older Taiwanese people: age- and gender-specific analyses. BMJ Open. 2014;4(3):e004428.
Mohd-Tahir NA, Li SC. Economic burden of osteoporosis-related hip fracture in Asia: a systematic review. Osteoporos Int. 2017;28(7):2035–44.
Caeiro JR, Bartra A, Mesa-Ramos M, Etxebarria I, Montejo J, Carpintero P, et al. Burden of first osteoporotic hip fracture in Spain: a prospective, 12-month. Observational study. Calcif Tissue Int. 2017;100(1):29–39.
Lee JH, Lee YH, Moon SH. Association between bone mineral density and clinical consequences: cross-sectional study of Korean postmenopausal women in an orthopaedic outpatient clinic. J Korean Med Sci. 2014;29(8):1152–60.
Coughlan T, Dockery F. Osteoporosis and fracture risk in older people. Clin Med. 2014;14(2):187–91.
Lee J, Lee JS, Park SH, Shin SA, Kim K. Cohort profile: the national health insurance service-national sample cohort (NHIS-NSC), South Korea. Int J Epidemiol. 2017;46(2):e15.
Park HY, Park JW, Sohn HS, Kwon JW. Association of parkinsonism or parkinson disease with polypharmacy in the year preceding diagnosis: a nested case-control study in South Korea. Drug Saf. 2017;40(11):1109–18.
Yu NW, Chen PJ, Tsai HJ, Huang CW, Chiu YW, Tsay WI, et al. Association of benzodiazepine and Z-drug use with the risk of hospitalisation for fall-related injuries among older people: a nationwide nested case-control study in Taiwan. BMC Geriatr. 2017;17(1):140.
Weinstein RS. Clinical practice. Glucocorticoid-induced bone disease. N Engl J Med. 2011;365(1):62–70.
Buckley L, Guyatt G, Fink HA, Cannon M, Grossman J, Hansen KE, et al. 2017 American College of Rheumatology guideline for the prevention and treatment of glucocorticoid-induced osteoporosis. Arthritis Rheumatol. 2017;69(8):1521–37.
Vatcheva KP, Lee M, McCormick JB, Rahbar MH. Multicollinearity in regression analyses conducted in epidemiologic studies. Epidemiology (Sunnyvale). 2016;6(2):227.
Rodriguez JM, Monsalves-Alvarez M, Henriquez S, Llanos MN, Troncoso R. Glucocorticoid resistance in chronic diseases. Steroids. 2016;115:182–92.
Kanis JA, Johansson H, Oden A, Johnell O, de Laet C, Melton IL, et al. A meta-analysis of prior corticosteroid use and fracture risk. J Bone Miner Res. 2004;19(6):893–9.
Lai SW, Lin CL, Liao KF. Use of oral corticosteroids and risk of hip fracture in the elderly in a case-control study. Front Pharmacol. 2017;8:625.
Emkey GR, Epstein S. Secondary osteoporosis: pathophysiology & diagnosis. Best Pract Res Clin Endocrinol Metab. 2014;28(6):911–35.
Gosch M, Jeske M, Kammerlander C, Roth T. Osteoporosis and polypharmacy. Z Gerontol Geriatr. 2012;45(6):450–4.
Ziere G, Dieleman JP, Hofman A, Pols HA, van der Cammen TJ, Stricker BH. Polypharmacy and falls in the middle age and elderly population. Br J Clin Pharmacol. 2006;61(2):218–23.
Richardson K, Bennett K, Kenny RA. Polypharmacy including falls risk-increasing medications and subsequent falls in community-dwelling middle-aged and older adults. Age Ageing. 2015;44(1):90–6.
Ambrose AF, Cruz L, Paul G. Falls and fractures: a systematic approach to screening and prevention. Maturitas. 2015;82(1):85–93.
Zia A, Kamaruzzaman SB, Tan MP. The consumption of two or more fall risk-increasing drugs rather than polypharmacy is associated with falls. Geriatr Gerontol Int. 2017;17(3):463–70.
Thorell K, Ranstad K, Midlov P, Borgquist L, Halling A. Is use of fall risk-increasing drugs in an elderly population associated with an increased risk of hip fracture, after adjustment for multimorbidity level: a cohort study. BMC Geriatr. 2014;14:131.
Woolcott JC, Richardson KJ, Wiens MO, Patel B, Marin J, Khan KM, et al. Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch Intern Med. 2009;169(21):1952–60.
Beunza-Sola M, Hidalgo-Ovejero AM, Marti-Ayerdi J, Sanchez-Hernandez JG, Menendez-Garcia M, Garcia-Mata S. Study of fall risk-increasing drugs in elderly patients before and after a bone fracture. Postgrad Med J. 2018;94(1108):76–80.
Park H, Satoh H, Miki A, Urushihara H, Sawada Y. Medications associated with falls in older people: systematic review of publications from a recent 5-year period. Eur J Clin Pharmacol. 2015;71(12):1429–40.
Kragh Ekstam A, Elmstahl S. Do fall-risk-increasing drugs have an impact on mortality in older hip fracture patients? A population-based cohort study. Clin Interv Aging. 2016;11:489–96.
Freeland KN, Thompson AN, Zhao Y, Leal JE, Mauldin PD, Moran WP. Medication use and associated risk of falling in a geriatric outpatient population. Ann Pharmacother. 2012;46(9):1188–92.
Bromfield SG, Ngameni CA, Colantonio LD, Bowling CB, Shimbo D, Reynolds K, et al. Blood pressure, antihypertensive polypharmacy, frailty, and risk for serious fall injuries among older treated adults with hypertension. Hypertension. 2017;70(2):259–66.
Bonaga B, Sanchez-Jurado PM, Martinez-Reig M, Ariza G, Rodriguez-Manas L, Gnjidic D, et al. Frailty, polypharmacy, and health outcomes in older adults: the frailty and dependence in albacete study. J Am Med Direct Assoc. 2018;19(1):46–52.
Veronese N, Stubbs B, Noale M, Solmi M, Pilotto A, Vaona A, et al. Polypharmacy is associated with higher frailty risk in older people: an 8-year longitudinal cohort study. J Am Med Direct Assoc. 2017;18(7):624–8.
Silay K, Yalcin A, Akinci S, Gursoy FG, Sener Dede D. Charlson Comorbidity Index, inappropriate medication use and cognitive impairment: bermuda Triangle. Wien Klin Wochenschr. 2017;129(21–22):799–804.
Johnell K. Inappropriate drug use in people with cognitive impairment and dementia: a systematic review. Curr Clin Pharmacol. 2015;10(3):178–84.
Jyrkka J, Enlund H, Lavikainen P, Sulkava R, Hartikainen S. Association of polypharmacy with nutritional status, functional ability and cognitive capacity over a three-year period in an elderly population. Pharmacoepidemiol Drug Saf. 2011;20(5):514–22.
Patterson SM, Cadogan CA, Kerse N, Cardwell CR, Bradley MC, Ryan C et al. Interventions to improve the appropriate use of polypharmacy for older people. The Cochrane Database Syst Rev. 2014;(10):CD008165.
Oboh L, Qadir MS. Deprescribing and managing polypharmacy in frail older people: a patient-centred approach in the real world. Eur J Hosp Pharm. 2017;24(1):58–62.
Cullinan S, Raae Hansen C, Byrne S, O’Mahony D, Kearney P, Sahm L. Challenges of deprescribing in the multimorbid patient. Eur J Hosp Pharm. 2017;24(1):43–6.
Sing CW, Woo YC, Lee ACH, Lam JKY, Chu JKP, Wong ICK, et al. Validity of major osteoporotic fracture diagnosis codes in the Clinical Data Analysis and Reporting System in Hong Kong. Pharmacoepidemiol Drug Saf. 2017;26(8):973–6.
Acknowledgements
The authors thank the Korea Research Foundation for supporting this research (nos. 2015R1C1A2A01052768 and 2018R1D1A1B07043416), and the National Health Insurance Service for providing data for this study (Approval number: NHIS-2018-2-022).
Author information
Authors and Affiliations
Contributions
All authors were involved in the conception of the study, and HP and JK directed and executed the research project. HP, SK, and JK designed the statistical analysis, SK and JK executed the analysis, and all authors reviewed the statistical analysis. HP wrote the first draft. All authors contributed to the review, critical analysis, and finalization of this manuscript.
Corresponding author
Ethics declarations
Funding
A National Research Foundation of Korea grant funded by the Korean government (MSIP) provided funding for the study (No. 2015R1C1A2A01052768 and No.2018R1D1A1B07043416), and the funders had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Conflict of interest
Hae-Young Park, Suji Kim, Hyun Soon Sohn, and Jin-Won Kwon declare that they have no conflicts of interest.
Ethical approval
The study protocol was approved by the Institutional Review Board of Kyungpook National University (approval number KNU 2014-0080).
Informed consent
This study was based on a secondary data source and patients were not directly involved in the entire research process, therefore the need for informed consent was waived.
Rights and permissions
About this article
Cite this article
Park, HY., Kim, S., Sohn, H.S. et al. The Association between Polypharmacy and Hip Fracture in Osteoporotic Women: A Nested Case–Control Study in South Korea. Clin Drug Investig 39, 63–71 (2019). https://doi.org/10.1007/s40261-018-0716-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40261-018-0716-3