Abstract
Background
The incisional surgical site infection (SSI) is an extremely common complication following open abdominal surgery and imposes a considerable treatment and cost burden.
Method
We conducted a multicenter open-label randomized controlled trial at three Tokyo Metropolitan medical institutions. We enrolled adult patients who underwent either an elective or an emergency open laparotomy. Eligible patients were allocated preoperatively to undergo wound closure with either subcuticular sutures or staples. A central Web-based randomization tool was used to assign participants randomly by a permuted block sequence with a 1:1 allocation ratio and a block size of 4 before mass closure to each group. The primary endpoint was the occurrence of a superficial SSI within 30 days after surgery in accordance with the Centers for Disease Control and Prevention criteria. This trial was registered with UMIN-CTR as UMIN 000004836 (http://www.umin.ac.jp/ctr).
Results
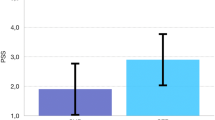
Between September 1, 2010 and August 31, 2015, 401 patients were enrolled and randomly assigned to either group. One hundred and ninety-nine patients were allocated to the subcuticular suture and 202 patients to the staple groups (hereafter the “suture” and “staple” group, respectively). Three hundred and ninety-nine were eligible for the primary endpoint. Superficial SSIs occurred in 25 of 198 suture patients and in 27 of 201 staple patients. Overall, the rate of superficial SSIs did not differ significantly between the suture and staple groups.
Conclusion
Subcuticular sutures did not increase the occurrence of superficial SSIs following open laparotomies mainly consisting of clean-contaminated surgical procedures. The applicability of the wound closure material and method is likely to depend on individual circumstances of the patient and surgical procedure.


Similar content being viewed by others
References
NICE Guidance. Surgical site infection (CG74). http://guidance.nice.org.uk/CG7 (accessed 4 Feb 2016)
Kirkland KB, Briggs JP, Trivette SL, Wilkinson WE, Sexton DJ. The impact of surgical-site infections in the 1990s: attributable mortality, excess length of hospitalization, and extra costs. Infect Control Hosp Epidemiol 1999; 20: 725-30.
Bratzler DW, Houck PM. Antimicrobial prophylaxis for surgery: an advisory statement from the National Surgical Infection Prevention Project. Clin Infect Dis 2004; 38: 1706-15.
Chu CC, Williams DF. Effects of physical configuration and chemical structure of suture materials on bacterial adhesion. A possible link to wound infection. Am J Surg 1984; 147: 197-204..
Cervantes-Sanchez CR, Gutierrez-Vega R, Vazquez-Carpizo JA, Clark P, Athie-Gutierrez C. Syringe pressure irrigation of subdermic tissue after appendectomy to decrease the incidence of postoperative wound infection. World J Surg 2000; 24: 38-41.
Wang ZX, Jiang CP, Cao Y, Ding YT. Systemic review and meta-analysis of triclosan-coated sutures for the prevention of surgical-site infection. Br J Surg 2013; 100: 465-73.
Heyland DK, Novak F, Drover JW, Jain M, Su X, Suchner U. Should immunonutrition become routine in critically ill patients? A systematic review of the evidence. JAMA 2001; 286: 944-53.
Heger U, Voss S, Knebel P, Doerr HC, Neudecker J, Schumacher C, et al. Prevention of abdominal wound infection (PROUD trial, DRKS00000390): study protocol for a randomized controlled trial. Trials 2011; 12: 245.
Diener MK, Knebel P, Kieser M, et al. Effectiveness of triclosan-coated PDS Plus versus uncoated PDS II sutures for prevention of surgical site infection after abdominal wall closure: the randomised controlled PROUD trial. Lancet 2014; 384:142-52.
Basha SL, Rochon ML, Quinones JN, Coassolo KM, Rust OA, Smulian JC. Randomized controlled trial of wound complication rates of subcuticular suture vs staples for skin closure at cesarean delivery. Am J Obstet Gynecol 2010; 203: 285.
Shetty AA, Kumar VS, Morgan-Hough C, Georgeu GA, James KD, Nicholl JE. Comparing wound complication rates following closure of hip wounds with metallic skin staples or subcuticular vicryl suture: a prospective randomised trial. J Orthop Surg (Hong Kong)2004; 12: 191-93.
Sanni A, Dunning J. Staples or sutures for chest and leg wounds following cardiovascular surgery. Interact Cardiovasc Thorac Surg 2007; 6: 243-46.
Johnson RG, Cohn WE, Thurer RL, McCarthy JR, Sirois CA, Weintraub RM. Cutaneous closure after cardiac operations: a controlled, randomized, prospective comparison of intradermal versus staple closures. Ann Surg 1997; 226: 606-12.
Moreno E-O A, Davenport DL, Hundley JC, Daily MF, Gedaly R.Predictors of surgical site infection after liver resection: a multicenter analysis using National Surgical Quality Improvement Program data HPB (Oxford) 2012; 14: 136-41.
Rousseau JA, Girard K, Turcot-Lemay L, Thomas N. A randomized study comparing skin closure in cesarean sections: staples vs subcuticular sutures. Am J Obstet Gynecol 2009; 200: e1-4.
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol 1999; 20: 247-278.
Higgins JP, White IR, Wood AM. Imputation methods for missing outcome data in meta-analysis of clinical trials Clin Trials 2008; 5: 225-39.
Steyerberg EW, Eijkemans MJ, Harrell FE, Habbema JD. Prognostic modelling with logistic regression analysis: a comparison of selection and estimation methods in small data sets. Stat Med 2000; 19: 1059-79.
Kanda Y. Investigation of the freely-available easy-to-use software “EZR” (Easy R) for medical statistics. Bone Marrow Transplant. 2013; 48: 452-458.
American Society of Anesthesiologists Physical Status Classification System. https://www.asahq.org/resources/clinical-information/asa-physical-status-classification-system (accessed 4 Feb 2016)
Singer AJ, Clark RAF. Cutaneous wound healing. N Engl J Med 1999; 341: 738-46.
Mackeen AD, Schuster M, Berghella V. Suture versus staplers for skin closure after cesarean: a metaanalysis. Am J Obstet Gynecol 2015; 212: 621. e1-10.
Tsujinaka T, Yamamoto K, Fujita J, et al. Subcuticular sutures versus staples for skin closure after open gastrointestinal surgery: a phase 3, multicentre, open-label, randomised controlled trial. Lancet 2013; 382: 1105-12.
Kobayashi S, Ito M, Yamamoto S, Kinugasa Y, Kotake M, Saida Y, et al. Randomized clinical trial of skin closure by subcuticular suture or skin stapling after elective colorectal surgery. Br J Surg. 2015; 102: 495-500.
Imamura H, Kurokawa Y, Tsujinaka T, Inoue K, Kimura Y, Iijima S, et al. Intraoperative versus extended antimicrobial prophylaxis after gastric cancer surgery: a phase 3, open-label, randomised controlled, non-inferiority trial. Lancet Infect Dis 2012; 12: 381-87.
Sugiura T, Uesaka K, Ohmagari N, Kanemoto H, Mizuno T. Risk factor of surgical site infection after pancreaticoduodenectomy. World J Surg 2012; 36: 2888-94..
Horton R. Surgical research or comic opera: questions, but few answers. Lancet 1996; 347: 984-85.
Hendriks AA, Vrielink MR, Smets EM, van Es SQ, De Haes JC. Improving the assessment of (in) patients’ satisfaction with hospital care. Med Care 2001; 39: 270-83.
Seiler CM, Bruckner T, Diener MK, Papyan A, Golcher H, Seidlmayer C, et al. Interrupted or continuous slowly absorbable sutures for closure of primary elective midline abdominal incisions: a multicenter randomized trial (INSECT: ISRCTN24023541). Ann Surg 2009; 249: 576-82.
Tanaka A, Sadahiro S, Suzuki T, Okada K, Saito G. Randomized controlled trial comparing subcuticular absorbable suture with conventional interrupted suture for wound closure at elective operation of colon cancer. Surgery; 2014: 155: 486-92.
Delgado-Rodriguez M, Gomez-Ortega A, Sillero-Arenas M, Liorca J. Epidemiology of surgical-site infections diagnosed after hospital discharge: a prospective cohort study. Infect Control Hosp Epidemiol 2001; 22: 24-30.
Acknowledgments
This study was supported by the Clinical Research Fund of Tokyo Metropolitan Government. We thank Ms. Mio Yatsuhashi, Ms. Takako Miyazaki, and Ms. Akemi Masuda of the Data Center at TMTMC for collecting the data. We are also grateful to the kind support of Ms. Masako Tomotsune, coordinator of clinical research at TMCMC.
Authors’ Contributions
KA and KI drafted the paper. SM and KI designed the protocol. MM supervised the design of the trial and assisted with conducting the trial. KI, KA, SS, and YS obtained and analyzed the data. KI, RS, and KA were the main investigators. All other authors participated in study execution and recruitment of patients. YM and TK provided expertise in statistical analysis and interpretation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study protocol was approved by the institutional review boards of all the participating hospitals. All patients provided written informed consent before participation.
Conflicts of Interest
The authors declare that they have no conflicts of interest.
Funding
Research Grant of the Tokyo Metropolitan Government.
Additional information
Kazuhiro Imamura and Kensuke Adachi contributed equally to this work.
Rights and permissions
About this article
Cite this article
Imamura, K., Adachi, K., Sasaki, R. et al. Randomized Comparison of Subcuticular Sutures Versus Staples for Skin Closure After Open Abdominal Surgery: a Multicenter Open-Label Randomized Controlled Trial. J Gastrointest Surg 20, 2083–2092 (2016). https://doi.org/10.1007/s11605-016-3283-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-016-3283-z