Abstract
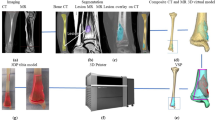
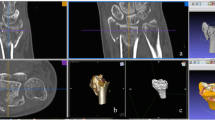
To demonstrate the 3D printed appearance of glenoid morphologies relevant to shoulder replacement surgery and to evaluate the benefits of printed models of the glenoid with regard to surgical planning. A retrospective review of patients referred for shoulder CT was performed, leading to a cohort of nine patients without arthroplasty hardware and exhibiting glenoid changes relevant to shoulder arthroplasty planning. Thin slice CT images were used to create both humerus-subtracted volume renderings of the glenoid, as well as 3D surface models of the glenoid, and 11 printed models were created. Volume renderings, surface models, and printed models were reviewed by a musculoskeletal radiologist for accuracy. Four fellowship-trained orthopaedic surgeons specializing in shoulder surgery reviewed each case individually as follows: First, the source CT images were reviewed, and a score for the clarity of the bony morphologies relevant to shoulder arthroplasty surgery was given. The volume rendering was reviewed, and the clarity was again scored. Finally, the printed model was reviewed, and the clarity again scored. Each printed model was also scored for morphologic complexity, expected usefulness of the printed model, and physical properties of the model. Mann–Whitney–Wilcoxon signed rank tests of the clarity scores were calculated, and the Spearman’s ρ correlation coefficient between complexity and usefulness scores was computed. Printed models demonstrated a range of glenoid bony changes including osteophytes, glenoid bone loss, retroversion, and biconcavity. Surgeons rated the glenoid morphology as more clear after review of humerus-subtracted volume rendering, compared with review of the source CT images (p = 0.00903). Clarity was also better with 3D printed models compared to CT (p = 0.00903) and better with 3D printed models compared to humerus-subtracted volume rendering (p = 0. 00879). The expected usefulness of printed models demonstrated a positive correlation with morphologic complexity, with Spearman’s ρ 0.73 (p = 0.0108). 3D printing of the glenoid based on pre-operative CT provides a physical representation of patient anatomy. Printed models enabled shoulder surgeons to appreciate glenoid bony morphology more clearly compared to review of CT images or humerus-subtracted volume renderings. These models were more useful as glenoid complexity increased.












Similar content being viewed by others
References
Horton K, Fishman E: Pictorial essay: Multidetector CT angiography of pancreatic carcinoma: Part i, evaluation of arterial involvement. Am J Roentgenol. 178:827–831, 2002
Beebe H, Kritpracha B: Computed tomography scanning for endograft planning: Evolving toward three-dimensional, single source imaging. Sem Vasc Surg. 17:126–134, 2004
Radtke A, Sotiropoulos G, Molmenti E et al.: Computer-assisted surgery planning for complex liver resections. When it is helpful? A single-center experience over an 8-year period. Ann Surg. 252:876–883, 2010
Schienfeld M, Dym A, Spektor M, Avery L, Dym R, Amanatullah D: Acetabular fractures: What radiologists should know and how 3D CT can aid classification. RadioGraphics. 35:555–577, 2015
Kim M, Hangsen A, Wink O, Quaife R, Carroll J: Rapid prototyping: A new tool in understanding and treating structural heart disease. Circulation. 117:2388–2394, 2008
Bibb R, Eggbeer D, Evans P: Rapid prototyping technologies in soft tissue facial prosthetics: Current state of the art. Rapid Prototyping Journal. 16:130–137, 2010
Mitsouras D, Liacouras P, Imanzadeh A, Giannopoulos AA, Cai T, Kumamaru KK, George E, Wake N, Caterson EJ, Pomahac B, Ho VB, Grant GT, Rybicki FJ: Medical 3D printing for the radiologist. RadioGraphics. 35:1965–1988, 2015
Wake N, Rude T, Kang S et al.: 3D printed renal cancer models derived from MRI data: Application in pre-surgical planning. Abdom Radiol. 42:1501–1509, 2017
Norris T, Iannotti J: Functional outcome after shoulder arthroplasty for primary osteoarthritis: A multicenter study. J Shoulder Elbow Surg. 11:130–135, 2002
Strauss E, Roche C, Flurin P, Wright T, Zuckerman J: The glenoid in shoulder arthroplasty. J Shoulder Elbow Surg. 18:819–833, 2009
Matsen, III F, Bicknell R, Lippitt S: Shoulder arthroplasty: The socket perspective. J Shoulder Elbow Surg. 16:241S–247S, 2007
Boileau P, Sinnerton R, Chuinard C, Walch G: Arthroplasty of the shoulder. J Bone Joint Surg. 88:562–575, 2006
Matsen, III F: The ream and run: Not for every patient, every surgeon or every problem. International Orthopaedics. 39:255–261, 2015
Edwards T: CORR insights: Can the ream and run procedure improve glenohumeral relationships and function shoulders with the arthritic triad? Clin Orthop Relat Res. 473:2097–2098, 2015
Frankle M, Siegal S, Pupello D, Saleem A, Mighell M, Vasey M: The reverse shoulder prosthesis for glenohumeral arthritis associated with severe rotator cuff deficiency. A minimum two-year follow-up study of sixty patients. J Bone Joint Surg. 87:1697–1705, 2005
Boileau P, Watkinson D, Hatzidakis A, Balg F. Grammont reverse prosthesis: Design, rationale, and biomechanics. J Shoulder Elbow Surg. 2005;14:147S–161S, S147, S161.
Roberts C, Ekelund A, Renfree K, Liu P, Chew F: Radiologic assessment of reverse shoulder arthroplasty. RadioGraphics. 27:223–235, 2007
Farshad M, Gerber C: Reverse total shoulder arthroplasty—From the most to the least common complication. International Orthopaedics. 34:1075–1082, 2010
Thompson T, Greenspoon J, Hanypsiak B, Lederman E: Reverse total shoulder arthroplasty: A comprehensive review of biomechanics, surgical technique, and potential complications. Curr Orthop Pract. 25:580–588, 2014
Simon P, Gupta A, Pappou I, Hussey MM, Santoni BG, Inoue N, Frankle MA: Glenoid subchondral bone density distribution in male total shoulder arthroplasty subjects with eccentric and concentric wear. J Shoulder Elbow Surg. 24:416–424, 2015
Knowles N, Athwal G, Keener J, Ferreira L: Regional bone density variations in osteoarthritic glenoids: A comparison of symmetric to asymmetric (type B2) erosion patterns. J Shoulder Elbow Surg 24:425–432, 2015
Scalise J, Codsi M, Bryan J, Iannotti J: The three-dimensional glenoid vault model can estimate normal glenoid version in osteoarthritis. J Shoulder Elbow Surg. 17:487–491, 2008
Friedman R, Hawthorne K, Genez B: The use of computerized tomography in the measurement of glenoid version. J Bone Joint Surg. 74:1032–1037, 1992
Churchill R, Brems J, Kotschi H: Glenoid size, inclination, and version: An anatomic study. J Shoulder Elbow Surg. 10:327–332, 2001
Inui H, Sugamoto K, Miyamoto T, Machida A, Hashimoto J, Nobuhara K: Evaluation of the three-dimensional glenoid structure using MRI. J Anat. 199:323–328, 2001
Steinmann S, Cofield R: Bone grafting for glenoid deficiency in total shoulder replacement. J Shoulder Elbow Surg. 9:361–367, 2000
https://www.rsna.org/ctp.aspx. Radiological Society of North America: MIRC Clinical Trials Processor (CTP). Accessed 29 August 2017.
Friedman T, Michalski M, Goodman T, Brown J: 3D printing from diagnostic images: A radiologist’s primer with an emphasis on musculoskeletal imaging—Putting the 3D printing of pathology into the hands of every physician. Skeletal Radiol. 45:307–321, 2016
Riesenkampff E, Rietdorf U, Wolf I, Schnackenburg B, Ewert P, Huebler M, Alexi-Meskishvili V, Anderson RH, Engel N, Meinzer HP, Hetzer R, Berger F, Kuehne T: The practical clinical value of three-dimensional models of complex congenitally malformed hearts. J Thoracic Cardiovasc Surg. 138:571–580, 2009
Matsumoto J, Morris J, Foley T et al.: Three-dimensional physical modeling: Application and experience at mayo clinic. RadioGraphics. 35:1989–2006, 2015
Rose A, Webster C, Harryson O, Formeister E, Rawal R, Iseli C: Pre-operative simulation of pediatric mastoid surgery with 3D-printed temporal bone models. Intl J Ped Otorhinolaryngology. 70:740–744, 2015
Gauci M, Boileau P, Baba M, Chaoui J, Walch G: Patient-specific glenoid guides provide accuracy and reproducibility in total shoulder arthroplasty. Bone Joint J. 98-B:1080–1085, 2016
Podolsky D, Martin A, Whyne C, Massicotte E, Hardisty M, Ginsberg H: Exploring the role of 3-dimensional simulation in surgical training: Feedback from a pilot study. J Spinal Disord Tech. 23:e70–e74, 2010
Waran V, Narayanan V, Karuppiah R, Owen S, Aziz T: Utility of multimaterial 3D printers in creating models with pathologica entities to enhance the training experience of neurosurgeons. J Neurosurg. 120:489–492, 2014
Waran V, Narayanan V, Karuppiah R, Pancharatnam D, Chandran H, Raman R, Rahman ZAA, Owen SLF, Aziz TZ: Injecting realism in surgical training—Initial simulation experience with custom 3D models. J Surg Edu. 71:193–197, 2014
Bader C, Kolb D, Weaver JC, Sharma S, Hosny A, Costa J, Oxman N: Making data matter: Voxel printing for the digital fabrication of data across scales and domains. Sci Adv. 4:eaas8652, 2018
Acknowledgments
The authors acknowledge 3D Systems for providing software and 3D printing services used in this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
3D Systems provided access to the DICOM-to-Print software and also printed one model presented in this work. The authors retained full control of all aspects of the study. One author reports grant funding from the Department of Veterans Affairs, and the Orthopaedic Research and Education Foundation, for other work relating to shoulder disorders. Another author reports grant funding from the National Center for Defense Manufacturing and Machining for other work relating to 3D printing.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, K.C., Jones, A., Kambhampati, S. et al. CT-Based 3D Printing of the Glenoid Prior to Shoulder Arthroplasty: Bony Morphology and Model Evaluation. J Digit Imaging 32, 816–826 (2019). https://doi.org/10.1007/s10278-019-00177-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10278-019-00177-4