Abstract
Objective
To evaluate the impact of accidental surgical incision into the tumour (ASIT) on oncological outcomes in patients undergoing RPN for a malignant tumour.
Materials and methods
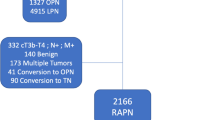
A retrospective review of our prospectively maintained database was performed to identify all patients who underwent RPN for a localized RCC between June 2010 and July 2016. We stratified our cohort into two groups according to the presence of an ASIT. Perioperative data were compared between the two groups. Logistic regression analyses were used to assess the variables associated with ASIT. Recurrence-free survival was estimated using the Kaplan–Meier method and compared between groups with the log-rank test.
Results
A total of 234 patients were identified. 32 (14%) ASIT were observed. Patients’ characteristics were similar in the two groups. Most of intraoperative outcomes were comparable between the two groups, but patients in the ASIT group had greater EBL (475 vs. 300 mL; p = 0.01). In multivariate analysis, tumour size (p = 0.02), RENAL score (p = 0.02), EBL (p = 0.05) and low surgeon experience (p = 0.03) were all predictive factors of ASIT. 15 (6%) of recurrences were observed over a median follow-up of 36 months. There was no difference in recurrence-free survival between the two groups (p = 0.57).
Conclusions
In our experience, accidental surgical incision into the tumour during RPN was a common event that did not appear to compromise oncological outcome.


Similar content being viewed by others
References
Campbell S, Uzzo RG, Allaf ME et al (2017) Renal mass and localized renal cancer: AUA guideline. J Urol [Internet] 198:520–529
Kunath F, Schmidt S, Krabbe L-M et al (2017) Partial nephrectomy versus radical nephrectomy for clinical localised renal masses. In: The Cochrane Collaboration (ed) Cochrane database of systematic reviews [Internet]. Wiley, Chichester. https://doi.org/10.1002/14651858.CD012045.pub2
Schiavina R, Mari A, Antonelli A et al (2015) A snapshot of nephron-sparing surgery in Italy: a prospective, multicenter report on clinical and perioperative outcomes (the RECORd 1 project). Eur J Surg Oncol 41(3):346–352
Peyronnet B, Seisen T, Oger E, Vaessen C et al (2016) Comparison of 1800 robotic and open partial nephrectomies for renal tumors. Ann Surg Oncol 23(13):4277–4283
Ficarra V, Minervini A, Antonelli A et al (2014) A multicentre matched-pair analysis comparing robot-assisted versus open partial nephrectomy: perioperative results of RAPN vs OPN. BJU Int 113(6):936–941
Novara G, La Falce S, Kungulli A et al (2016) Robot-assisted partial nephrectomy. Int J Surg 36:554–559
Ficarra V, Righetti R, Pilloni S et al (2002) Prognostic factors in patients with renal cell carcinoma: retrospective analysis of 675 cases. Eur Urol 41(2):190–198
Tanaka T, Terai Y, Maeda K et al (2017) Intraperitoneal cytology after laparoscopic hysterectomy in patients with endometrial cancer: a retrospective observational study. Medicine 96(27):e7502
Paolucci V, Schaeff B, Schneider M et al (1999) Tumor seeding following laparoscopy: international survey. World J Surg 23(10):989–995
Benway BM, Wang AJ, Cabello JM et al (2009) Robotic partial nephrectomy with sliding-clip renorrhaphy: technique and outcomes. Eur Urol 55(3):592–599
Kutikov A, Uzzo RG (2009) The R.E.N.A.L. nephrometry score: a comprehensive standardized system for quantitating renal tumor size, location and depth. J Urol 182(3):844–853
Davidiuk AJ, Parker AS, Thomas CS et al (2014) Mayo adhesive probability score: an accurate image-based scoring system to predict adherent perinephric fat in partial nephrectomy. Eur Urol 66(6):1165–1171
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Shah PH, Moreira DM, Okhunov Z et al (2016) Positive surgical margins increase risk of recurrence after partial nephrectomy for high risk renal tumors. J Urol 196(2):327–334
Autorino R, Porpiglia F, Dasgupta P et al (2017) Precision surgery and genitourinary cancers. Eur J Surg Oncol 43(5):893–908
Sutherland SE, Resnick MI, Maclennan GT et al (2002) Does the size of the surgical margin in partial nephrectomy for renal cell cancer really matter? J Urol 167(1):61–64
Parker WP, Cheville JC, Frank I et al (2017) Application of the stage, size, grade, and necrosis (SSIGN) score for clear cell renal cell carcinoma in contemporary patients. Eur Urol 71(4):665–673
Bretheau D, Lechevallier E, de Fromont M et al (1995) Prognostic value of nuclear grade of renal cell carcinoma. Cancer 76(12):2543–2549
Maurice MJ, Zhu H, Kim S et al (2016) Survival after partial and radical nephrectomy for high-risk disease: a propensity-matched comparison. Can Urol Assoc J 10(9–10):E282–E289
Becker A, Hickmann D, Hansen J et al (2016) Critical analysis of a simplified Fuhrman grading scheme for prediction of cancer specific mortality in patients with clear cell renal cell carcinoma—impact on prognosis. Eur J Surg Oncol 42(3):419–425
Pahernik S, Ziegler S, Roos F et al (2007) Small renal tumors: correlation of clinical and pathological features with tumor size. J Urol 178(2):414–417 (discussion 416–417)
Frank I, Blute ML, Cheville JC et al (2003) Solid renal tumors: an analysis of pathological features related to tumor size. J Urol 170(6 Pt 1):2217–2220
Bhindi B, Lohse CM, Mason RJ et al (2017) Are we using the best tumor size cut-points for renal cell carcinoma staging? Urology 109:121–126
Kwon EO, Carver BS, Snyder ME et al (2007) Impact of positive surgical margins in patients undergoing partial nephrectomy for renal cortical tumours. BJU Int 99(2):286–289
Bensalah K, Pantuck AJ, Rioux-Leclercq N et al (2010) Positive surgical margin appears to have negligible impact on survival of renal cell carcinomas treated by nephron-sparing surgery. Eur Urol 57(3):466–471
Yossepowitch O, Thompson RH, Leibovich BC et al (2008) Positive surgical margins at partial nephrectomy: predictors and oncological outcomes. J Urol 179(6):2158–2163
Klein EA, Bianco FJ, Serio AM et al (2008) Surgeon experience is strongly associated with biochemical recurrence after radical prostatectomy for all preoperative risk categories. J Urol 179(6):2212–2216 (discussion 2216–2217)
Rolevich A, Minich A, Nabebina T et al (2016) Surgeon has a major impact on long-term recurrence risk in patients with non-muscle invasive bladder cancer. Cent Eur J Urol 69(2):170–177
Khandwala YS, Jeong IG, Kim JH et al (2017) The impact of surgeon volume on perioperative outcomes and cost for patients receiving robotic partial nephrectomy. J Endourol [Internet]. https://doi.org/10.1089/end.2017.0207
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that there is no competing interest.
About this article
Cite this article
Khene, ZE., Peyronnet, B., Pradère, B. et al. Does tumour effraction during robotic partial nephrectomy have any impact on recurrence?. Int J Clin Oncol 24, 87–93 (2019). https://doi.org/10.1007/s10147-018-1331-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-018-1331-2