Abstract
Purpose
Hepatectomy is feasible for patients with hepatocellular carcinoma (HCC) who are eligible for liver transplantation according to the Milan criteria if they have good hepatic function. This retrospective study investigates the prognostic factors of hepatectomy in HCC patients meeting the Milan criteria.
Methods
Between 1991 and 2005, 175 patients underwent hepatectomy for HCC at our institute; 111 met and 64 exceeded the Milan criteria. The prognostic factors for hepatectomy were investigated using a Cox regression model.
Results
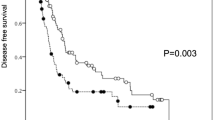
Operative mortality and morbidity were significantly lower in the patients who met the criteria than in those who exceeded the criteria. After a median follow-up of 51.5 months, the 5-year survival rate was significantly better for the patients who met the criteria than for those who exceeded the criteria (77.8% vs 35.7%; P < 0.0001). The factors predictive of poor prognosis were poor differentiation, microscopic vasculobiliary invasion, and a high serum des-gamma-carboxy prothrombin (DCP) level (>100 mAU/ml) for the patients who met the Milan criteria; and only the presence of a microsatellite lesion for the patients who did not meet the Milan criteria.
Conclusions
Hepatectomy is safe and beneficial for HCC patients who meet the Milan criteria, but a high preoperative serum DCP level may be predictive of a poor prognosis.
Similar content being viewed by others
References
El-Serag HB, Mason AC. Rising incidence of hepatocellular carcinoma in the United States. N Engl J Med 1999;340:745–750.
Burroughs A, Hochhauser D, Meyer T. Systemic treatment and liver transplantation for hepatocellular carcinoma: Two ends of the therapeutic spectrum. Lancet Oncol 2004;5:409–418.
Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;334:693–699.
Poon RT. Optimal initial treatment for early hepatocellular carcinoma in patients with preserved liver function: Transplantation or resection? Ann Surg Oncol 2007;14:541–547.
Eguchi S, Takatsuki M, Hidaka M, Tajima Y, Kanematsu T. Evolution of living donor liver transplantation over 10 years: Experience of a single center. Surg Today 2008;38:795–800.
Tanaka S, Noguchi N, Ochiai T, Kudo A, Nakamura N, Ito K, et al. Outcomes and recurrence of initially resectable hepatocellular carcinoma meeting Milan criteria: Rationale for partial hepatectomy as first strategy. J Am Coll Surg 2007;204:1–6.
Imamura H, Sano K, Sugawara Y, Kokudo N, Makuuchi M. Assessment of hepatic reserve for indication of hepatic resection: decision tree incorporating indocyanine green test. J Hepatobiliary Pancreat Surg 2005;12:16–22.
Couinaud C, Foie L. Etudes anatomiques et chirurgicales. Paris: Masson; 1957.
Poon RT, Fan ST, Lo CM, Liu CL, Wong J. Difference in tumor invasiveness in cirrhotic patients with hepatocellular carcinoma fulfilling the Milan criteria treated by resection and transplantation: Impact on long-term survival. Ann Surg 2007;245:51–58.
Margarit C, Escartin A, Castells L, Vargas V, Allende E, Bilbao I. Resection for hepatocellular carcinoma is a good option in Child-Turcotte-Pugh class a patients with cirrhosis who are eligible for liver transplantation. Liver Transpl 2005;11:1242–1251.
Kamiyama T, Nakanishi K, Yokoo H, Kamachi H, Tahara M, Suzuki T, et al. Recurrence patterns after hepatectomy of hepatocellular carcinoma: implication of Milan criteria utilization. Ann Surg Oncol 2009;16:1560–1571.
Yamamoto J, Kosuge T, Saiura A, Sakamoto Y, Shimada K, Sano T, et al. Effectiveness of hepatic resection for early-stage hepatocellular carcinoma in cirrhotic patients: subgroup analysis according to Milan criteria. Jpn J Clin Oncol 2007;37:287–295.
Zavaglia C, De Carlis L, Alberti AB, Minola E, Belli LS, Slim AO, et al. Predictors of long-term survival after liver transplantation for hepatocellular carcinoma. Am J Gastroenterol 2005;100:2708–2716.
Ko S, Kanehiro H, Hisanaga M, Nagao M, Ikeda N, Nakajima Y. Liver fibrosis increases the risk of intrahepatic recurrence after hepatectomy for hepatocellular carcinoma. Br J Surg 2002;89:57–62.
Imamura H, Matsuyama Y, Miyagawa Y, Ishida K, Shimada R, Miyagawa S, et al. Prognostic significance of anatomical resection and des-gamma-carboxy prothrombin in patients with hepatocellular carcinoma. Br J Surg 1999;86:1032–1038.
Fukuda S, Itamoto T, Nakahara H, Kohashi T, Ohdan H, Hino H, et al. Clinicopathologic features and prognostic factors of resected solitary small-sized hepatocellular carcinoma. Hepatogastroenterology 2005;52:1163–1167.
Koike Y, Shiratori Y, Sato S, Obi S, Teratani T, Imamura M, et al. Des-gamma-carboxy prothrombin as a useful predisposing factor for the development of portal venous invasion in patients with hepatocellular carcinoma: a prospective analysis of 227 patients. Cancer 2001;91:561–569.
Okuda H, Nakanishi T, Takatsu K, Saito A, Hayashi N, Takasaki K, et al. Serum levels of des-gamma-carboxy prothrombin measured using the revised enzyme immunoassay kit with increased sensitivity in relation to clinicopathologic features of solitary hepatocellular carcinoma. Cancer 2000;88:544–549.
Sala M, Fuster J, Llovet JM, Navasa M, Sole M, Varela M, et al. High pathological risk of recurrence after surgical resection for hepatocellular carcinoma: an indication for salvage liver transplantation. Liver Transpl 2004;10:1294–1300.
Lee HH, Joh JW, Park JH, Lee KW, Heo JS, Choi SH, et al. Microvascular tumor embolism: independent prognostic factor after liver transplantation in hepatocellular carcinoma. Transplant Proc 2005;37:1251–1253.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Sakaguchi, T., Suzuki, S., Morita, Y. et al. Impact of the preoperative des-gamma-carboxy prothrombin level on prognosis after hepatectomy for hepatocellular carcinoma meeting the Milan criteria. Surg Today 40, 638–645 (2010). https://doi.org/10.1007/s00595-009-4109-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-009-4109-3