Abstract
Purpose
To perform a meta-analysis comparing the rates of positive surgical margins (PSM) and biochemical recurrence (BCR) between open radical prostatectomy (ORP) and robot-assisted radical prostatectomy (RARP) in patients with high-risk prostate cancer.
Methods
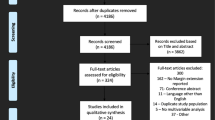
A systematic review was performed on Pubmed, Embase and Scopus databases in August 2016, according to the Preferred Reporting Items for Systematic Review and Meta-analysis (PRISMA) statement. References retrieved were evaluated using the Newcastle–Ottawa scale and the Black and Down’s tool for quality assessment.
Results
Nine retrospective cohorts comparing ORP and RARP were selected and included in the meta-analysis. All studies reported the PSMs. Patients treated with RARP presented less risk of PSMs (risk difference −0.04, p 0.02) than those treated with ORP. Five articles reported hazard ratios for BCR-free survival. Patients treated with RARP had less risk of BCR (HR 0.72, 95% CI 0.58–0.89) than those treated with ORP. Reports for PSM assessment were considered of adequate quality, while the studies retrieved for BCR assessment were considered limited because of the heterogeneity of their results.
Conclusion
Patients with high-risk prostate cancer treated with RARP have less risk of having PSM and BCR when compared to those treated with ORP. A strong conclusion is precluded due to the observational nature of the studies retrieved for our analysis.


Similar content being viewed by others
References
D’Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA et al (1998) Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280(11):969–974
Hernandez DJ, Nielsen ME, Han M, Partin AW (2007) Contemporary evaluation of the D’amico risk classification of prostate cancer. Urology 70(5):931–935
Sooriakumaran P, Nyberg T, Akre O, Haendler L, Heus I, Olsson M et al (2014) Comparative effectiveness of radical prostatectomy and radiotherapy in prostate cancer: observational study of mortality outcomes. BMJ 348:g1502
Boorjian SA, Karnes RJ, Rangel LJ, Bergstralh EJ, Blute ML (2008) Mayo Clinic validation of the D’amico risk group classification for predicting survival following radical prostatectomy. J Urol 179(4):1354–1360
Mottet N, Bellmunt J, Briers E, Bolla M, Cornford P, De Santis M et al European association of urology guidelines (prostate cancer). https://uroweb.org/guideline/prostate-cancer/. Accessed 10 Aug 2016
Cooperberg MR, Vickers AJ, Broering JM, Carroll PR (2010) Comparative risk-adjusted mortality outcomes after primary surgery, radiotherapy, or androgen-deprivation therapy for localized prostate cancer. Cancer 116(22):5226–5234
Petrelli F, Vavassori I, Coinu A, Borgonovo K, Sarti E, Barni S (2014) Radical prostatectomy or radiotherapy in high-risk prostate cancer: a systematic review and meta-analysis. Clin Genitourin Cancer 12(4):215–224
Boorjian SA, Karnes RJ, Viterbo R, Rangel LJ, Bergstralh EJ, Horwitz EM et al (2011) Long-term survival after radical prostatectomy versus external-beam radiotherapy for patients with high-risk prostate cancer. Cancer 117(13):2883–2891
Kohutek ZA, Weg ES, Pei X, Shi W, Zhang Z, Kollmeier MA et al (2016) Long-term impact of androgen-deprivation therapy on cardiovascular morbidity after radiotherapy for clinically localized prostate cancer. Urology 87:146–152
Yamamoto S, Kawakami S, Yonese J, Fujii Y, Urakami S, Masuda H et al (2012) Long-term oncological outcome and risk stratification in men with high-risk prostate cancer treated with radical prostatectomy. Jpn J Clin Oncol 42(6):541–547
Hsu CC, Paciorek AT, Cooperberg MR, Roach M 3rd, Hsu IC, Carroll PR (2015) Postoperative radiation therapy for patients at high-risk of recurrence after radical prostatectomy: does timing matter? BJU Int 116(5):713–720
Meeks JJ, Eastham JA (2012) Robotic prostatectomy: the rise of the machines or judgment day. Eur Urol 62:686–687
Koch MO (2016) Robotic versus open prostatectomy: end of the controversy. J Urol 196(1):9–10
Yaxley JW, Coughlin GD, Chambers SK, Occhipinti S, Samaratunga H, Zajdlewicz L et al (2016) Robot-assisted laparoscopic prostatectomy versus open radical retropubic prostatectomy: early outcomes from a randomised controlled phase 3 study. Lancet 388(10049):1057–1066
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Open Med 3:e123–e130
NCCN Clinical Practice Guidelines in Oncology. (2016) Prostate Cancer—Version 3. https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Accessed 29 Nov 2016
Elm von E, Altman DG, Egger M et al (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370:1453–1457
Wells GA, Shea B, O’Connell D, Robertson J, Peterson J, Welch V et al (2011) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 10 Aug 2016
Downs SH, Black N (1998) The feasibility of creating a checklist for the assessment of the methodological quality both of randomized and nonrandomized studies of health care interventions. J Epidemiol Community Health 52:377–384
Lee EK, Baack J, Duchene DA (2010) Survey of practicing urologists: robotic versus open radical prostatectomy. Can J Urol 17(2):5094–5098
Wedmid A, Llukani E, Lee DI (2011) Future perspectives in robotic surgery. BJU Int 108(6 Pt 2):1028–1036
Novara G, Ficarra V, Rosen RC, Artibani W, Costello A, Eastham JA et al (2012) Systematic review and meta-analysis of perioperative outcomes and complications after robot-assisted radical prostatectomy. Eur Urol 62(3):431–452
Novara G, Ficarra V, Mocellin S, Ahlering TE, Carroll PR, Graefen M et al (2012) Systematic review and meta-analysis of studies reporting oncologic outcome after robot-assisted radical prostatectomy. Eur Urol 62(3):382–404
Yuh B, Artibani W, Heidenreich A, Kimm S, Menon M, Novara G et al (2014) The role of robot-assisted radical prostatectomy and pelvic lymph node dissection in the management of high-risk prostate cancer: a systematic review. Eur Urol 65(5):918–927
Pierorazio PM, Mullins JK, Eifler JB, Voth K, Hyams ES, Han M et al (2013) Contemporaneous comparison of open vs minimally-invasive radical prostatectomy for high-risk prostate cancer. BJU Int 112(6):751–757
Punnen S, Meng MV, Cooperberg MR, Greene KL, Cowan JE, Carroll PR (2013) How does robot-assisted radical prostatectomy (RARP) compare with open surgery in men with high-risk prostate cancer? BJU Int 112(4):314–320
Silberstein JL, Su D, Glickman L, Kent M, Keren-Paz G, Vickers AJ et al (2013) A case-mix-adjusted comparison of early oncological outcomes of open and robotic prostatectomy performed by experienced high volume surgeons. BJU Int 111(2):206–212
Busch J, Magheli A, Leva N, Hinz S, Ferrari M, Friedersdorff F et al (2014) Matched comparison of outcomes following open and minimally invasive radical prostatectomy for high-risk patients. World J Urol 32(6):1411–1416
Lee D, Choi SK, Park J, Shim M, Kim A, Lee S et al (2015) Comparative analysis of oncologic outcomes for open vs. robot-assisted radical prostatectomy in high-risk prostate cancer. Korean J Urol 56(8):572–579
Yossepowitch O, Briganti A, Eastham JA, Epstein J, Graefen M, Montironi R et al (2014) Positive surgical margins after radical prostatectomy: a systematic review and contemporary update. Eur Urol 65(2):303–313
Ploussard G, Agamy MA, Alenda O, Allory Y, Mouracade P, Vordos D et al (2011) Impact of positive surgical margins on prostate-specific antigen failure after radical prostatectomy in adjuvant treatment-naïve patients. BJU Int 107(11):1748–1754
Pfitzenmaier J, Pahernik S, Tremmel T, Haferkamp A, Buse S, Hohenfellner M (2008) Positive surgical margins after radical prostatectomy: do they have an impact on biochemical or clinical progression? BJU Int 102(10):1413–1418
Wright JL, Dalkin BL, True LD, Ellis WJ, Stanford JL, Lange PH et al (2010) Positive surgical margins at radical prostatectomy predict prostate cancer specific mortality. J Urol 183(6):2213–2218
Vickers A, Bianco F, Cronin A, Eastham J, Klein E, Kattan M et al (2010) The learning curve for surgical margins after open radical prostatectomy: implications for margin status as an oncological endpoint. J Urol 183(4):1360–1365
Meeks JJ, Eastham JA (2013) Radical prostatectomy: positive surgical margins matter. Urol Oncol 31(7):974–979
Klein EA, Bianco FJ, Serio AM, Eastham JA, Kattan MW, Pontes JE et al (2008) Surgeon experience is strongly associated with biochemical recurrence after radical prostatectomy for all preoperative risk categories. J Urol 179(6):2212–2217
Harty NJ, Kozinn SI, Canes D, Sorcini A, Moinzadeh A (2013) Comparison of positive surgical margin rates in high risk prostate cancer: open versus minimally invasive radical prostatectomy. Int Braz J Urol 39(5):639–646
Hu JC, Gandaglia G, Karakiewicz PI, Nguyen PL, Trinh QD, Shih YC et al (2014) Comparative effectiveness of robot-assisted versus open radical prostatectomy cancer control. Eur Urol 66(4):666–672
Suardi N, Dell’Oglio P, Gallina A, Gandaglia G, Buffi N, Moschini M et al (2016) Evaluation of positive surgical margins in patients undergoing robot-assisted and open radical prostatectomy according to preoperative risk groups. Urol Oncol 34(2):57.e1–e7
Pearce SM, Pariser JJ, Karrison T, Patel SG, Eggener SE (2016) Comparison of perioperative and early oncologic outcomes between open and robotic assisted laparoscopic prostatectomy in a contemporary population based cohort. J Urol 196(1):76–81
Laird A, Fowler S, Good DW, Stewart GD, Srinivasan V, Cahill D, British Association of Urological Surgeons (BAUS) et al (2015) Contemporary practice and technique-related outcomes for radical prostatectomy in the UK: a report of national outcomes. BJU Int 115(5):753–763
Oberlin DT, Flum AS, Lai JD, Meeks JJ (2016) The effect of minimally invasive prostatectomy on practice patterns of American urologists. Urol Oncol 34(6):255.e1–e5
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Srougi, V., Bessa, J., Baghdadi, M. et al. Surgical method influences specimen margins and biochemical recurrence during radical prostatectomy for high-risk prostate cancer: a systematic review and meta-analysis. World J Urol 35, 1481–1488 (2017). https://doi.org/10.1007/s00345-017-2021-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-017-2021-9