Abstract
Background
Due to radical resection, endoprosthetic reconstruction (EPR) is more invasive and increases the risk of dislocation. Therefore, the suitability of EPR for elderly patients with metastatic tumor needs further investigation.
Methods
Seventy-one adult patients with isolated proximal femoral bone metastases who underwent EPR were retrospectively analyzed and stratified into two groups: elderly age group (≥60 years, n = 31) and younger age group (<60 years, n = 40). The effect of age on prognosis was analyzed to determine whether EPR is beneficial in elderly patients with proximal femoral metastatic tumor. Cox regression modeling was used to evaluate the effect of different factors on postoperative survival outcomes.
Results
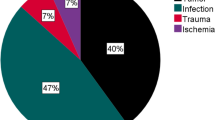
Ten (32.26%) and 9 (22.50%) cases of perioperative complications were recorded in the elderly and younger age groups, respectively, with median survival times of 22.00 ± 4.61 months and 23.00 ± 2.85 months, respectively; a log-rank test showed that the difference was not statistically significant (p = 0.657). A Cox regression model was established with patient age as the covariable to evaluate whether it affected postoperative survival. The risk of death due to age was not significant (p = 0.649), but malignancy and femoral metastasis type were significantly associated with postoperative survival (p = 0.001 and p = 0.019).
Conclusion
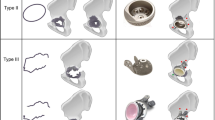
Although older patients have a slightly higher incidence of postoperative complications than younger patients, they do not experience severe adverse consequences. With rigorous selection and careful preparation, EPR is appropriate for the treatment of proximal femoral metastases in older patients, including those with Harrington type I–II acetabular invasion.

Similar content being viewed by others
References
Yang Y, Guo W, Wei R. Analysis of clinical prognostic factor for 99 patients with metastases of proximal femur [in Chinese]. Beijing Da Xue Xue Bao Yi Xue Ban. 2012;44(6):895-900
Xu L, Jin J, Hu A, et al. Soft tissue recurrence of giant cell tumor of the bone: prevalence and radiographic features. J Bone Oncol. 2017;9:10–4. https://doi.org/10.1016/j.jbo.2017.09.002.
Bostel T, Forster R, Schlampp I, et al. Spinal bone metastases in colorectal cancer: a retrospective analysis of stability, prognostic factors and survival after palliative radiotherapy. Radiat Oncol. 2017;12(1):115. https://doi.org/10.1186/s13014-017-0852-6.
Peterson JR, Decilveo AP, O’Connor IT, Golub I, Wittig JC. What are the functional results and complications with long stem hemiarthroplasty in. Clin Orthop Relat Res. 2017;475(3):745–56. https://doi.org/10.1007/s11999-016-4810-7.
Feng H, Wang J, Guo P, Xu J, Chen W, Zhang Y. CT-guided percutaneous femoroplasty (PFP) for the treatment of proximal femoral metastases. Pain Physician. 2016;19(5):E767–73.
Harvey N, Ahlmann ER, Allison DC, Wang L, Menendez LR. Endoprostheses last longer than intramedullary devices in proximal femur metastases. Clin Orthop Relat Res. 2012;470(3):684–91. https://doi.org/10.1007/s11999-011-2038-0.
Steensma M, Boland PJ, Morris CD, Athanasian E, Healey JH. Endoprosthetic treatment is more durable for pathologic proximal femur fractures. Clin Orthop Relat Res. 2012;470(3):920–6. https://doi.org/10.1007/s11999-011-2047-z.
Plancarte R, Guajardo J, Meneses-Garcia A, et al. Clinical benefits of femoroplasty: a nonsurgical alternative for the management of femoral metastases. Pain Physician. 2014;17(3):227–34.
Plancarte-Sanchez R, Guajardo-Rosas J, Cerezo-Camacho O, et al. Femoroplasty: a new option for femur metastasis. Pain Pract. 2013;13(5):409–15. https://doi.org/10.1111/j.1533-2500.2012.00590.x.
Vermesan D, Prejbeanu R, Haragus H, et al. Case series of patients with pathological dyaphiseal fractures from metastatic bone disease. Int Orthop. 2017;41(10):2199–203. https://doi.org/10.1007/s00264-017-3582-3.
Yang Y, Guo W, Yang RL, Tang XD, Yan TQ, Wei R. Surgical classification and therapeutic strategy for metastases of proximal femur [in Chinese]. Zhonghua Wai Ke Za Zhi. May 2013;51(5):407-12.
Harrington KD. The management of acetabular insufficiency secondary to metastatic malignant disease. J Bone Joint Surg Am. 1981;63(4):653–64.
Issack PS, Barker J, Baker M, Kotwal SY, Lane JM. Surgical management of metastatic disease of the proximal part of the femur. J Bone Joint Surg Am. 2014;96(24):2091–8. https://doi.org/10.2106/JBJS.N.00083.
Malek F, Somerson JS, Mitchel S, Williams RP. Does limb-salvage surgery offer patients better quality of life and functional capacity than amputation? Clin Orthop Relat Res. 2012;470(7):2000–6. https://doi.org/10.1007/s11999-012-2271-1.
Janssen SJ, Teunis T, Hornicek FJ, van Dijk CN, Bramer JA, Schwab JH. Outcome after fixation of metastatic proximal femoral fractures: A systematic review of 40 studies. J Surg Oncol. 2016;114(4):507–19. https://doi.org/10.1002/jso.24345.
Xing Z, Moon BS, Satcher RL, Lin PP, Lewis VO. A long femoral stem is not always required in hip arthroplasty for patients with proximal femur metastases. Clin Orthop Relat Res. 2013;471(5):1622–7. https://doi.org/10.1007/s11999-013-2790-4.
Johnson JD, Perry KI, Yuan BJ, Rose PS, Houdek MT. Outcomes of endoprosthetic replacement for salvage of failed fixation of malignant pathologic proximal femur fractures. J Arthroplasty. 2019;34(4):700–3. https://doi.org/10.1016/j.arth.2018.12.009.
Langslet E, Frihagen F, Opland V, Madsen JE, Nordsletten L, Figved W. Cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures: 5-year followup of a randomized trial. Clin Orthop Relat Res. 2014;472(4):1291–9. https://doi.org/10.1007/s11999-013-3308-9.
Houdek MT, Wyles CC, Labott JR, Rose PS, Taunton MJ, Sim FH. Durability of hemiarthroplasty for pathologic proximal femur fractures. J Arthroplasty. 2017;32(12):3607–10. https://doi.org/10.1016/j.arth.2017.06.040.
Putnam DS, Philipp TC, Lam PW, Gundle KR. Treatment modalities for pathologic fractures of the proximal femur pertrochanteric region: A systematic review and meta-analysis of reoperation rates. J Arthroplasty. 2018;33(10):3354–61. https://doi.org/10.1016/j.arth.2018.06.012.
Cheng DD, Yang JL, Hu T, Yang QC. Efficacy of limb salvage with primary tumor resection simultaneously for solitary bone metastasis in limbs. World J Surg Oncol. 2016;14(1):31. https://doi.org/10.1186/s12957-016-0786-8.
Pala E, Mavrogenis AF, Angelini A, Henderson ER, Douglas Letson G, Ruggieri P. Cemented versus cementless endoprostheses for lower limb salvage surgery. J BUON. 2013;18(2):496–503.
Ratasvuori M, Wedin R, Hansen BH, et al. Prognostic role of en-bloc resection and late onset of bone metastasis in. J Surg Oncol. 2014;110(4):360–5. https://doi.org/10.1002/jso.23654.
Henrichs MP, Krebs J, Gosheger G, et al. Modular tumor endoprostheses in surgical palliation of long-bone metastases: a reduction in tumor burden and a durable reconstruction. World J Surg Oncol. 2014;12:330. https://doi.org/10.1186/1477-7819-12-330.
Guzik G. Oncological and functional results after surgical treatment of bone metastases at the proximal femur. BMC Surg. 2018;18(1):5. https://doi.org/10.1186/s12893-018-0336-0.
Wedin R, Bauer HC. Surgical treatment of skeletal metastatic lesions of the proximal femur: endoprosthesis or reconstruction nail? J Bone Joint Surg Br. 2005;87(12):1653–7. https://doi.org/10.1302/0301-620X.87B12.16629.
Chandrasekar CR, Grimer RJ, Carter SR, Tillman RM, Abudu A, Buckley L. Modular endoprosthetic replacement for tumours of the proximal femur. J Bone Joint Surg Br. 2009;91(1):108–12. https://doi.org/10.1302/0301-620X.91B1.20448.
Hattori H, Mibe J, Yamamoto K. Modular megaprosthesis in metastatic bone disease of the femur. Orthopedics. 2011;34(12):e871–6. https://doi.org/10.3928/01477447-20111021-13.
Park DH, Jaiswal PK, Al-Hakim W, et al. The use of massive endoprostheses for the treatment of bone metastases. Sarcoma. 2007;2007:62151. https://doi.org/10.1155/2007/62151.
Selek H, Basarir K, Yildiz Y, Saglik Y. Cemented endoprosthetic replacement for metastatic bone disease in the proximal femur. J Arthroplasty. 2008;23(1):112–7. https://doi.org/10.1016/j.arth.2006.11.016.
Sarahrudi K, Greitbauer M, Platzer P, Hausmann JT, Heinz T, Vecsei V. Surgical treatment of metastatic fractures of the femur: a retrospective analysis of 142 patients. J Trauma. 2009;66(4):1158–63. https://doi.org/10.1097/TA.0b013e3181622bca.
Henderson ER, Groundland JS, Pala E, et al. Failure mode classification for tumor endoprostheses: retrospective review of five institutions and a literature review. J Bone Joint Surg Am. 2011;93(5):418–29. https://doi.org/10.2106/JBJS.J.00834.
Sevelda F, Schuh R, Hofstaetter JG, Schinhan M, Windhager R, Funovics PT. Total femur replacement after tumor resection: Limb salvage usually achieved but complications and failures are common. Clin Orthop Relat Res. 2015;473(6):2079–87. https://doi.org/10.1007/s11999-015-4282-1.
Alvi HM, Damron TA. Prophylactic stabilization for bone metastases, myeloma, or lymphoma: do we need to protect the entire bone? Clin Orthop Relat Res. 2013;471(3):706–14. https://doi.org/10.1007/s11999-012-2656-1.
Pala E, Henderson ER, Calabro T, et al. Survival of current production tumor endoprostheses: complications, functional results, and a comparative statistical analysis. J Surg Oncol. 2013;108(6):403–8. https://doi.org/10.1002/jso.23414.
Price SL, Farukhi MA, Jones KB, Aoki SK, Randall RL. Complications of cemented long-stem hip arthroplasty in metastatic bone disease revisited. Clin Orthop Relat Res. 2013;471(10):3303–7. https://doi.org/10.1007/s11999-013-3113-5.
Mirels H. Metastatic disease in long bones. A proposed scoring system for diagnosing impending pathologic fractures. Clin Orthop Relat Res. 1989;249:256–64.
Acknowledgment
The study protocol was approved by the Institutional Review Board at Sichuan Provincial People’s Hospital, and written informed consent was obtained from all patients for publication of this study.
Funding
This article was supported by Chengdu Municipal Science and Technology Project, 2019-YFYF-00093-SN.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Peng Liu, Zhuan Wang, Shiyuan Zhang, Guoqiang Ding, Ke Tan, and Ji Zhou have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, P., Wang, Z., Zhang, S. et al. Application of Endoprosthetic Replacement in Old Patients with Isolated Proximal Femoral Bone Metastases. Ann Surg Oncol 29, 8623–8630 (2022). https://doi.org/10.1245/s10434-022-11912-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-11912-7