Abstract
Background
Primary hyperaldosteronism is most commonly due to a solitary cortical adenoma. Thus, some surgeons have suggested a subtotal adrenalectomy is a reasonable approach when a mass can be identified. On the other hand, adrenal vein sampling (AVS) is being used more frequently to distinguish patients with unilateral disease for adrenalectomy, even if a discrete mass is not identified on axial imaging. In these cases, surgical pathology may reveal a cortical adenoma, a cortical adenoma with hyperplasia, or cortical hyperplasia. The goal of this study was to compare the presentation and outcome among patients undergoing adrenalectomy and found to have different histologic features.
Methods
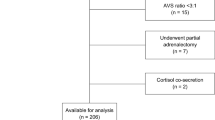
We performed a retrospective analysis of 136 patients with primary hyperaldosteronism. A total of 95 patients had an adrenalectomy for unilateral disease. The preoperative clinical and laboratory, and postoperative outcome of the three aforementioned histologic groups were compared.
Results
A total of 95 patients underwent an adrenalectomy. We found no significant difference in age, gender, body mass index, duration of hypertension, number of antihypertensive medications, serum aldosterone level, serum renin level, or adrenal vein sampling ratios among the three histologic categories. We also found no significant difference among the three categories in postoperative cure rate.
Conclusion
The rate of unilateral hyperplasia in patients with primary hyperaldosteronism (16 %) is likely higher than previously reported, which may be due to the increasing use of AVS. The clinical presentation and outcome of patients regardless of the histologic findings are similar. Our data also suggests that subtotal adrenalectomy would not be appropriate in patients with primary hyperaldosteronism.

Similar content being viewed by others
Reference
Conn JW, Louis LH. Primary aldosteronism: a new clinical entity. Trans Assoc Am Physicians. 1955;68:215–31, discussion, 231–3.
Young WF. Primary aldosteronism: renaissance of a syndrome. Clin Endocrinol (Oxf). 2007;66:607–18.
Schwartz GL, Turner ST. Screening for primary aldosteronism in essential hypertension: diagnostic accuracy of the ratio of plasma aldosterone concentration to plasma renin activity. Clin Chem. 2005;51:386–94.
Stowasser M, Sharman J, Leano R, Gordon RD, Ward G, Cowley D, et al. Evidence for abnormal left ventricular structure and function in normotensive individuals with familial hyperaldosteronism type I. J Clin Endocrinol Metab. 2005;90:5070–6.
Milliez P, Girerd X, Plouin PF, Blacher J, Safar ME, Mourad JJ. Evidence for an increased rate of cardiovascular events in patients with primary aldosteronism. J Am Coll Cardiol. 2005;45:1243–8.
Herrada AA, Campino C, Amador CA, Michea LF, Fardella CE, Kalergis AM. Aldosterone as a modulator of immunity: implications in the organ damage. J Hypertens. 2011;29:1684–92.
Tresallet C, Salepcioglu H, Godiris-Petit G, Hoang C, Girerd X, Menegaux F. Clinical outcome after laparoscopic adrenalectomy for primary hyperaldosteronism: the role of pathology. Surgery. 2010;148:129–34.
Webb R, Mathur A, Chang R, Baid S, Nilubol N, Libutti SK, et al. What is the best criterion for the interpretation of adrenal vein sample results in patients with primary hyperaldosteronism? Ann Surg Oncol. 2012;19:1881–6.
Mathur A, Kemp CD, Dutta U, Baid S, Ayala A, Chang RE, et al. Consequences of adrenal venous sampling in primary hyperaldosteronism and predictors of unilateral adrenal disease. J Am Coll Surg. 2010;211:384–90.
Lonborg J, Mathur M, Grieve SM, Bhindi R, Ward M, Lowe H, et al. Constrictive pericarditis diagnosed by cardiac magnetic resonance. J Am Coll Cardiol. 2010;56:e39.
Young WF, Stanson AW, Thompson GB, Grant CS, Farley DR, van Heerden JA. Role for adrenal venous sampling in primary aldosteronism. Surgery. 2004;136:1227–35.
Magill SB, Raff H, Shaker JL, Brickner RC, Knechtges TE, Kehoe ME, et al. Comparison of adrenal vein sampling and computed tomography in the differentiation of primary aldosteronism. J Clin Endocrinol Metab. 2001;86:1066–71.
Steichen O, Zinzindohoue F, Plouin PF, Amar L. Outcomes of adrenalectomy in patients with unilateral primary aldosteronism: a review. Horm Metab Res. 2012;44:221–7.
Sawka AM, Young WF, Thompson GB, Grant CS, Farley DR, Leibson C, et al. Primary aldosteronism: factors associated with normalization of blood pressure after surgery. Ann Intern Med. 2001;135:258–61.
Lumachi F, Ermani M, Basso SM, Armanini D, Iacobone M, Favia G. Long-term results of adrenalectomy in patients with aldosterone-producing adenomas: multivariate analysis of factors affecting unresolved hypertension and review of the literature. Am Surg. 2005;71:864–9.
Satoh F, Abe T, Tanemoto M, Nakamura M, Abe M, Uruno A, et al. Localization of aldosterone-producing adrenocortical adenomas: significance of adrenal venous sampling. Hypertens Res. 2007;30:1083–95.
Pang TC, Bambach C, Monaghan JC, Sidhu SB, Bune A, Delbridge LW, et al. Outcomes of laparoscopic adrenalectomy for hyperaldosteronism. ANZ J Surg. 2007;77:768–73.
Zarnegar R, Lee J, Brunaud L, Lindsay S, Kebebew E, Clark OH, et al. Good blood pressure control on antihypertensives, not only response to spironolactone, predicts improved outcome after adrenalectomy for aldosteronoma. Surgery. 2007;142:921–9.
Zarnegar R, Young WF, Jr., Lee J, Sweet MP, Kebebew E, Farley DR, et al. The aldosteronoma resolution score: predicting complete resolution of hypertension after adrenalectomy for aldosteronoma. Ann Surg. 2008;247:511–8.
Quillo AR, Grant CS, Thompson GB, Farley DR, Richards ML, Young WF. Primary aldosteronism: results of adrenalectomy for nonsingle adenoma. J Am Coll Surg. 2011;213:106–12, discussion 112–3.
Dye NV, Litton NJ, Varma M, Isley WL. Unilateral adrenal hyperplasia as a cause of primary aldosteronism. South Med J. 1989;82:82–6.
Ganguly A, Yum MN, Pratt JH, Weinberger MH, Grim CE, Yune HY, et al. Unilateral hypersecretion of aldosterone associated with adrenal hyperplasia as a cause of primary aldosteronism. Clin Exp Hypertens A. 1983;5:1635–58.
Banks WA, Kastin AJ, Biglieri EG, Ruiz AE. Primary adrenal hyperplasia: a new subset of primary hyperaldosteronism. J Clin Endocrinol Metab. 1984;58:783–5.
Ross EJ. Conn’s syndrome due to adrenal hyperplasia with hypertrophy of zona glomerulosa, relieved by unilateral adrenalectomy. Am J Med. 1965;39:994–1002.
Sasagawa I, Nakada T, Hashimoto T, Kato T, Suzuki H, Ishigooka M, et al. Unilateral diffuse adrenal hyperplasia masquerading as aldosterone-producing adenoma in primary hyperaldosteronism. Urol Int. 1993;50:218–22.
Ganguly A, Bergstein J, Grim CE, Yum MN, Weinberger MH. Childhood primary aldosteronism due to an adrenal adenoma: preoperative localization by adrenal vein catheterization. Pediatrics. 1980;65:605–9.
Otsuka F, Otsuka-Misunaga F, Koyama S, Yamanari H, Ogura T, Ohe T, et al. Hormonal characteristics of primary aldosteronism due to unilateral adrenal hyperplasia. J Endocrinol Invest. 1998;21:531–6.
Haenel LCt, Hermayer KL. A case of unilateral adrenal hyperplasia: the diagnostic dilemma of hyperaldosteronism. Endocr Pract. 2000;6:153–8.
Morioka M, Kobayashi T, Sone A, Furukawa Y, Tanaka H. Primary aldosteronism due to unilateral adrenal hyperplasia: report of two cases and review of the literature. Endocr J. 2000;47:443–9.
Oberfield SE, Levine LS, Firpo A, Lawrence D Sr, Stoner E, Levy DJ, et al. Primary hyperaldosteronism in childhood due to unilateral macronodular hyperplasia. Case report. Hypertension. 1984;6:75–84.
Pignatelli D, Falcao H, Coimbra-Peixoto A, Cruz F. Unilateral adrenal hyperplasia. South Med J. 1994;87:664–7.
Mendlowitz M. A case of predominantly unilateral pseudoprimary hyperaldosteronism. Mt Sinai J Med. 1982;49:76–7.
Goh BK, Tan YH, Chang KT, Eng PH, Yip SK, Cheng CW. Primary hyperaldosteronism secondary to unilateral adrenal hyperplasia: an unusual cause of surgically correctable hypertension. A review of 30 cases. World J Surg. 2007;31:72–9.
Weinberger MH, Grim CE, Hollifield JW, Kem DC, Ganguly A, Kramer NJ, et al. Primary aldosteronism: diagnosis, localization, and treatment. Ann Intern Med. 1979;90:386–95.
Kem DC, Tang K, Hanson CS, Brown RD, Painton R, Weinberger MH, et al. The prediction of anatomical morphology of primary aldosteronism using serum 18-hydroxycorticosterone levels. J Clin Endocrinol Metab. 1985;60:67–73.
Rao A, Melby JC. Idiopathic hyperplasia of the adrenal gland behaving like an aldosterone producing adenoma. J Endocrinol Invest. 1997;20:29–31.
Chen LG, Lee TI, Lin HD, Wang HC, Liu WY, Tang KT. Primary aldosteronism due to unilateral adrenal hyperplasia: a case report. Zhonghua Yi Xue Za Zhi (Taipei). 1997;59:114–20.
Mansoor GA, Malchoff CD, Arici MH, Karimeddini MK, Whalen GF. Unilateral adrenal hyperplasia causing primary aldosteronism: limitations of I-131 norcholesterol scanning. Am J Hypertens. 2002;15:459–64.
Katayama Y, Takata N, Tamura T, Yamamoto A, Hirata F, Yasuda H, et al. A case of primary aldosteronism due to unilateral adrenal hyperplasia. Hypertens Res. 2005;28:379–84.
Omura M, Sasano H, Fujiwara T, Yamaguchi K, Nishikawa T. Unique cases of unilateral hyperaldosteronemia due to multiple adrenocortical micronodules, which can only be detected by selective adrenal venous sampling. Metabolism. 2002;51:350–5.
Hirono Y, Doi M, Yoshimoto T, Kanno K, Himeno Y, Taki K, et al. A case with primary aldosteronism due to unilateral multiple adrenocortical micronodules. Endocr J. 2005;52:435–9.
Omura M, Saito J, Yamaguchi K, Kakuta Y, Nishikawa T. Prospective study on the prevalence of secondary hypertension among hypertensive patients visiting a general outpatient clinic in Japan. Hypertens Res. 2004;27:193–202.
Murashima M, Trerotola SO, Fraker DL, Han D, Townsend RR, Cohen DL. Adrenal venous sampling for primary aldosteronism and clinical outcomes after unilateral adrenalectomy: a single-center experience. J Clin Hypertens (Greenwich). 2009;11:316–23.
Walz MK, Gwosdz R, Levin SL, Alesina PF, Suttorp AC, Metz KA, et al. Retroperitoneoscopic adrenalectomy in Conn’s syndrome caused by adrenal adenomas or nodular hyperplasia. World J Surg. 2008;32:847–53.
Proye CA, Mulliez EA, Carnaille BM, Lecomte-Houcke M, Decoulx M, Wémeau JL, et al. Essential hypertension: first reason for persistent hypertension after unilateral adrenalectomy for primary aldosteronism? Surgery. 1998;124:1128–33.
Celen O, O’Brien MJ, Melby JC, Beazley RM. Factors influencing outcome of surgery for primary aldosteronism. Arch Surg. 1996;131:646–50.
Disclosure
No financial disclosures.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Weisbrod, A.B., Webb, R.C., Mathur, A. et al. Adrenal Histologic Findings Show No Difference in Clinical Presentation and Outcome in Primary Hyperaldosteronism. Ann Surg Oncol 20, 753–758 (2013). https://doi.org/10.1245/s10434-012-2670-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2670-2