Abstract
Background
Primary amoebic meningoencephalitis (PAM) is a rare but fatal infection caused by Naegleria fowleri. The infection is acquired by deep nasal irrigation with infected water. Patients present with signs and symptoms similar to pneumococcal meningitis, leading to delayed diagnosis and treatment and hence high mortality.
Methods
We conducted a case–control study comparing culture proven cases of PAM with pneumococcal meningitis presenting to our center between April 2008 and September 2014. Only patients with blood and/or cerebrospinal fluid cultures positive for Streptococcus pneumoniae during the same time period were included for comparison.
Results
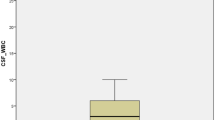
There were 19 cases of PAM and pneumococcal meningitis, each. When comparing PAM with pneumococcal meningitis, patients with PAM were more likely to be male (89.5 vs. 36.8 %), younger (mean age: 30 vs. 59 years), present with seizures (42.1 vs. 5.3 %). Both groups of patients presented with similar vital signs and there were no remarkable differences on physical examinations, Glasgow Coma Scale scores, laboratory and radiological investigations and cerebrospinal fluid parameters. PAM was also more likely to present if the city’s average maximum temperature was higher in the previous week (mean: 34.6 vs. 30 °C). There was history of fresh water contact in only one patient. On multivariate analysis, PAM was more likely if patients presented when the city’s average maximum temperature was high, being young males.
Conclusion
PAM and pneumococcal meningitis remain virtually indistinguishable; however, these predictive features should be validated in a prospective study and may lead to a viable algorithm for early management of these patients.

Similar content being viewed by others
References
Gautam PL, Sharma S, Puri S, Kumar R, Midha V, Bansal R. A rare case of survival from primary amebic meningoencephalitis. Indian J Crit Care Med. 2012;16:34.
Movahedi Z, Shokrollahi MR, Aghaali M, Heydari H. Primary amoebic meningoencephalitis in an Iranian infant. Case Rep Med. 2012;2012.
Yoder JS, Straif-Bourgeois S, Roy SL, Moore TA, Visvesvara GS, Ratard RC, et al. Primary amebic meningoencephalitis deaths associated with sinus irrigation using contaminated tap water. Clin Infect Dis. 2012;55:e79–85.
Capewell LG, Harris AM, Yoder JS, Cope JR, Eddy BA, Roy SL, et al. Diagnosis, clinical course, and treatment of primary amoebic meningoencephalitis in the United States, 1937–2013. J Pediatric Infect Dis Soc. 2015;4(4):e68–75.
Lopez C, Budge P, Chen J, Bilyeu S, Mirza A, Custodio H, et al. Primary amebic meningoencephalitis: a case report and literature review. Pediatr Emerg Care. 2012;28:272–6.
Trabelsi H, Dendana F, Sellami A, Sellami H, Cheikhrouhou F, Neji S, et al. Pathogenic free-living amoebae: epidemiology and clinical review. Pathol Biol. 2012;60:399–405.
Yoder JS, Eddy BA, Visvesvara GS, Capewell L, Beach MJ. The epidemiology of primary amoebic meningoencephalitis in the USA, 1962–2008. Epidemiol Infect. 2010;138:968–75.
Mahmood K. Naegleria fowleri in Pakistan-an emerging catastrophe. J Coll Physicians Surg Pak. 2015;25:159–60.
Shakoor S, Beg MA, Mahmood SF, Bandea R, Sriram R, Noman F, et al. Primary amebic meningoencephalitis caused by Naegleria fowleri, Karachi, Pakistan. Emerg Infect Dis. 2011;17:258.
Durand ML, Calderwood SB, Weber DJ, Miller SI, Southwick FS, Caviness VS Jr, et al. Acute bacterial meningitis in Adults––a review of 493 episodes. N Engl J Med. 1993;328:21–8.
Van de Beek D, de Gans J, Tunkel AR, Wijdicks EFM. Community-acquired bacterial meningitis in adults. N Engl J Med. 2006;354:44–53.
Myint T, Ribes JA, Stadler LP. Primary amebic meningoencephalitis. Clin Infect Dis. 2012;55:1737–8.
Szénási Z, Endo T, Yagita K, Nagy E. Isolation, identification and increasing importance of ‘free-living’ amoebae causing human disease. J Med Microbiol. 1998;47:5–16.
Vargas-Zepeda Js, Gómez-Alcalá AV, Vázquez-Morales JA, Licea-Amaya L, De Jonckheere JF, Lares-Villa F. Successful treatment of Naegleria fowleri meningoencephalitis by using intravenous amphotericin B, fluconazole and rifampicin. Arch Med Res. 2005;36:83–6.
Hara T, Fukuma T. Diagnosis of the primary amoebic meningoencephalitis due to Naegleria fowleri. Parasitol Int. 2005;54:219–21.
Ma P, Visvesvara GS, Martinez AJ, Theodore FH, Daggett PM, Sawyer TK. Naegleria and Acanthamoeba infections: review. Rev Infect Dis. 1990;12:490–513.
Kazi AN, Riaz T. Deaths from rare protozoan encephalitis in Karachi blamed on unchlorinated water. BMJ. 2013;346:f3580.
Siddiqui R, Khan NA. Is ritual cleansing a missing link between fatal infection and brain-eating amoebae? Clin Infect Dis. 2012;54:1817–8.
Goudot S, Herbelin P, Mathieu L, Soreau S, Banas S, Jorand F. Growth dynamic of Naegleria fowleri in a microbial freshwater biofilm. Water Res. 2012;46:3958–66.
Siddiqui R, Khan NA. Primary amoebic meningoencephalitis caused by Naegleria fowleri: an old enemy presenting new challenges. PLoS Negl Trop Dis. 2014;14:e3017.
Blair B, Sarkar P, Bright KR, Marciano-Cabral F, Gerba CP. Naegleria fowleri in well water. Emerg Infect Dis. 2008;14:1499.
Dawn NEWS Internet Edition. ‘Contaminated water’ being supplied to city. http://www.dawn.com/fixed/arch/arch_2009.html. Accessed 22 Jul 2009.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare they have no conflicts of interest.
Sources of funding
The authors did not receive any funding or support for the manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zahid, M.F., Saad Shaukat, M.H., Ahmed, B. et al. Comparison of the clinical presentations of Naegleria fowleri primary amoebic meningoencephalitis with pneumococcal meningitis: a case–control study. Infection 44, 505–511 (2016). https://doi.org/10.1007/s15010-016-0878-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-016-0878-y