Abstract
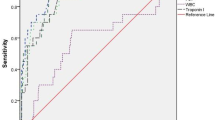
Infants with respiratory distress syndrome (RDS) may suffer from severe hypoxia, asphyxia. In this study, we aimed to evaluate serum ischemia-modified albumin (IMA) level as a diagnostic marker for hypoxia in preterm infants with RDS. Thirty-seven premature newborns with RDS were allocated as the study group and 42 healthy preterm neonates were selected as the control group. IMA was measured as absorbance unit (ABSU) in human serum with colorimetric assay method which is based on reduction in albumin cobalt binding. IMA levels were significantly higher in neonates with RDS as compared to the control group (P < 0.001). Cut-off value of IMA (ABSU) was 0.72, the sensitivity level was 91.9 %, the specificity was 78.6 %, positive predictive value was 79.1 % and negative predictive value was 91.7 % at RDS. Area under curve values was 0.93 (P < 0.001; 95 % CI, 0.88–0.98) in the receiver operating characteristic curve. We concluded that elevated blood IMA levels might be accepted as a useful marker for hypoxia in newborn with RDS.

Similar content being viewed by others
References
Rodrigez RJ, Martin RJ, Fanroff AA. Respiratory dystress syndrome and its manangement. In: Martin RJ, Fanaroff AA, Walsh MC, editors. Fanaroff and Matin’s neonatal perinatal disease of the fetus and infant. 8th ed. Philadelphia: Elsevier-Mosby; 2006. p. 1097–122.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European consensus guidelines on the management of neonatal respiratory distress syndrome in preterm infants–2013 update. Neonatology. 2013;103:353–68.
Dani C, Reali MF, Bertini G, Wiechmann L, Spagnolo A, Tangucci M, et al. Risk factors for the development of respiratory distress syndrome and transient tachypnoea in newborn infants. Italian group of Neonatal Pneumology. Eur Respir J. 1999;14:155–9.
Gitto E, Reiter RJ, Karbownik M, Xian-Tan D, Barberi I. Respiratory distress syndrome in the newborn: role of oxidative stress. Intensive Care Med. 2001;27:1116–23.
Thornberg E, Thiringer K, Odeback A, Milsom I. Birth asphyxia: incidence, clinical course and outcome in a Swedish population. Acta Paediatr. 1995;84:927–32.
Nordstrom L, Arulkumaran S. Intrapartum fetal hypoxia and biochemical markers: a review. Obstet Gynecol Surv. 1998;53:645–57.
Gaze DC. Ischemia modified albumin: a novel biomarker for the detection of cardiac ischemia. Drug Metab Pharmacokinet. 2009;24:333–41.
Shen XL, Lin CJ, Han LL, Lin L, Pan L, Pu XD. Assessment of ischemia-modified albumin levels for emergency room diagnosis of acute coronary syndrome. Int J Cardiol. 2011;149:296–8.
Sadler PJ, Tucker A, Viles JH. Involvement of a lysine residue in the N-terminal Ni2+ and Cu2+ binding site of serum albumins. Comparison with Co2+, Cd2 + and Al3+. Eur J Biochem. 1994;220:193–200.
Caglar GS, Tasci Y, Goktolga U, Oztas E, Pabuccu R, Ozdemir ED, et al. Maternal and umbilical cord ischemia-modified albumin levels in nonreassuring fetal heart rate tracings regarding the mode of delivery. J Matern Fetal Neonatal Med. 2013;26:528–31.
Dursun A, Okumus N, Zenciroglu A. Ischemia-modified albumin (IMA): could it be useful to predict perinatal asphyxia? J Matern Fetal Neonatal Med. 2012;25:2401–5.
Kumral A, Okyay E, Guclu S, Gencpinar P, Islekel GH, Oguz SS, et al. Cord blood ischemia-modified albumin: is it associated with abnormal Doppler findings in complicated pregnancies and predictive of perinatal asphyxia? J Obstet Gynaecol Res. 2013;39:663–71.
Yakut I, Tayman C, Oztekin O, Namuslu M, Karaca F, Kosus A. Ischemia-modified albumin may be a novel marker for the diagnosis and follow-up of necrotizing enterocolitis. J Clin Lab Anal. 2014;28:170–7.
Agrawal V, David RJ, Harris VJ. Classification of acute respiratory disorders of all newborns in a tertiary care center. J Natl Med Assoc. 2003;95:585–95.
Sbarouni E, Georgiadou P, Kremastinos DT, Voudris V. Ischemia modified albumin: is this marker of ischemia ready for prime time use? Hellenic J Cardiol. 2008;49:260–6.
Gunduz A, Turkmen S, Turedi S, Mentese A, Yulug E, Ulusoy H, et al. Time-dependent variations in ischemia-modified albumin levels in mesenteric ischemia. Acad Emerg Med. 2009;16:539–43.
Ustün Y, Engin-Ustün Y, Oztürk O, Alanbay I, Yaman H. Ischemia-modified albumin as an oxidative stress marker in preeclampsia. J Matern Fetal Neonatal Med. 2011;24:418–21.
van Rijn BB, Franx A, Sikkema JM, van Rijn HJ, Bruinse HW, Voorbij HA, et al. Ischemia modified albumin in normal pregnancy and preeclampsia. Hypertens Pregnancy. 2008;27:159–67.
Gugliucci A, Hermo R, Monroy C, Numaguchi M, Kimura S. Ischemia-modified albumin levels in cord blood: a case-control study in uncomplicated and complicated deliveries. Clin Chim Acta. 2005;362:155–60.
Ukinc K, Eminagaoglu S, Ersoz HO, Erem C, Karahan C, Hacihasanoglu AB, et al. A novel indicator of widespread endothelial damage and ischemia in diabetic patients: ischemia-modified albumin. Endocrine. 2009;36:425–32.
Davis JM, Auten RL. Maturation of the antioxidant system and the effects on preterm birth. Semin Fetal Neonatal Med. 2010;15:191–5.
Author information
Authors and Affiliations
Corresponding author
Additional information
Hasan Kahveci and Cuneyt Tayman are the first author.
Rights and permissions
About this article
Cite this article
Kahveci, H., Tayman, C., Laoğlu, F. et al. Serum Ischemia-Modified Albumin in Preterm Babies with Respiratory Distress Syndrome. Ind J Clin Biochem 31, 38–42 (2016). https://doi.org/10.1007/s12291-015-0494-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12291-015-0494-0